|
Abstract:
Introduction: We describe the technique and report the outcome
of 100 arthroscopic subacromial decompressions with excision of
the distal clavicle performed using a new arthroscopy portal.
Methods: We prospectively collected data on all patients who
underwent simultaneous arthroscopic subacromial decompression
and excision of distal clavicle by a single surgeon in one
institution over an 8 month period. All patients had symptoms as
a result of subacromial impingement persisting for at least 6
months despite conservative measures. All patients had MRI scans
confirming subacromial impingement and acromioclavicular joint
degenerative changes except two patients who were claustrophobic
and had ultrasound scans instead. Arthroscopic subacromial
decompression was performed via a postero-lateral viewing portal
and a postero-medial working portal described by Declercq.
Excision of the distal clavicle was performed via a new portal
located posteriorly at the superior edge of the scapular spine
and in-line with the acromioclavicular joint. All operations
were performed under general anaesthesia with instillation of
local anaesthetic into the subacromial bursa at the end of the
operation. Postoperative analgesia consisted of paracetamol,
codeine phosphate and non-steroidal anti-inflammatory drugs
unless contraindicated. Patients were encouraged to start
shoulder movements immediately after surgery. Time to return to
work and driving were recorded. Oxford Shoulder Score (OSS) was
recorded preoperatively and at 2 weeks and 6 months
postoperatively.
Results: 100 patients were included. (58 men and 42 women, mean
age 58 years, range 39-75 years). The mean time to return to
work was 12 days and to driving was 9 days. The mean
pre-operative VAS pain score was 7.2 and 6 weeks post-op was 3.
The mean pre-operative oxford shoulder score (OSS) was 22.4 and
a 6 week follow-up was 36.2. Eleven patients (11) had their
operations done as inpatient due to medical co-morbidities and
were discharged on the first postoperative day. Eighty-Nine
patients (89) had their operations done as day-case procedures;
one of them required overnight admission due to an allergic drug
reaction. No other complications were recorded during the study
period.
Discussion and conclusions: The new arthroscopy portal for
excision of distal clavicle provides direct access to the
acromioclavicular joint and minimises muscle and soft tissue
injury. Simultaneous arthroscopic subacromial decompression and
excision of distal clavicle using this technique can be done as
a day-case procedure, provides good relief of pain and
improvement in functional outcome scores and allows quick return
to work and driving.
J.Orthopaedics 2010;7(4)e10
Keywords:
shoulder; arthroscopy; sub acromial decompression; portal
Introduction:
Neers work in the 1970s/80s (1) first implicated the anterior
acromion as a cause for painful impingement in the subacromial
space. Following Ellmans work in the 1980s (2) arthroscopic
subacromial decompression (ASAD) has become a well recognised
and successful treatment for refractory painful impingement.
In
the study by Fischer et al the authors studied the effect of
violation of the Acromioclavicular joint (ACJ) during
arthroscopic acromioplasty; the authors found that patients that
either had no violation of the AC joint or patients that had
complete distal clavicle resection (DCR) had no postoperative
sequelae in reference to the AC joint, in contrast, 14 / 36
shoulders (39%) with documented AC joint violation and a partial
DCR developed AC joint symptoms at an average of 8.4 months;
this has led to the recommendation that if the AC joint must be
violated to perform an adequate decompression of the subacromial
space, complete resection of the distal clavicle should be
performed, even if the radiographs show no preoperative
degenerative changes.
Most papers describe a posterolateral viewing portal and a
lateral and direct superior working portal for simultaneous
decompression and excision distal clavicle however it is the
primary authors view that this does not afford adequate
visualisation of the ACJ to ensure full resection of the distal
clavicle, thus avoiding the AC joint symptoms described by
Fischer. In 1999 Declercq (4) described the use of a
posteromedial working portal in the same saggital plane as the
ACJ in combination with a direct anterior portal for completion
of the resection.
We describe the use of Declercqs posteromedial portal in
conjunction with a second posteromedial portal located at the
superior edge of the scapula spine directly in line with the
ipsillateral ACJ, thus avoiding the possible damage to the
superior capsular ligaments associated with the use of the
anterior and superior portal.
Materials
and Methods:
Patients were followed up prospectively over a period of 1 year;
all of them had clinical impingement refractory to conservative
management (mean symptoms 14 months) and an MRI scan confirming
subacromial impingement and a degenerative ACJ. They were all
scored preoperatively on the day of surgery using the oxford
shoulder score (OSS) and the visual analogue (VAS) pain scoring
system. Other demographic details were also collected. All
operations were carried out or supervised by a single surgeon
(senior author MP) using a standard technique described below.
After induction of general anaesthesia the patient is placed in
the lateral decubitus position and tilted 30° posteriorly.
Between 4 and 5 kg of skin traction is applied to the arm, which
is placed in 20° of abduction and slight forward flexion. The
arthroscope is placed through a posterolateral portal just
lateral to the soft spot to inspect the glenohumeral joint and
the under surface of the cuff (Fig 1). Through the same skin
incision, we place the arthroscope into the subacromial space.
After inspection of the subacromial space, we make the
posteromedial working portal. This portal is 2.5 to 3 cm more
medial to the posterolateral portal and 3 to 4 cm inferior to
the spine of the scapula (Fig 1). Normally, the portal will lie
in the same sagittal plane as the ipsilateral AC joint. The
acromion is planned flat through this portal and the prominent
CA ligament removed, initial resection of the ACJ is then
performed to the extent allowable by the constraints of the
portal. A third posteromedial portal is then made on the
superior edge of the spine of the scapula in line with a
posteriorly projected extension of the ACJ (Fig 2), the exact
location of the skin incision is variable and may need to be
more posterior to prevent skin and fat being compressed on the
spine of the scapula depending on patient habitus. A pencil
point trochar is then inserted directed towards the front of the
ACJ parallel to the floor to check the alignment of the portal
which should come out directly underneath the ACJ. A shaver is
then introduced in place of the trochar (Fig 3) and a full 1cm
resection of the distal clavicle is performed from posterior to
anterior under direct vision.
The subacromial space is the infiltrated with 20mls of
chirocaine following removal of the skin traction and closure of
the 2 posteromedial portals with 4.0 vicryl and steristrips. The
postero-lateral portal is then closed in a similar fashion and
spirit gauze and mepore dressings applied.
Postoperatively the patient is advised to fully mobilise the
shoulder and no sling is required. The patients were then
followed up by the surgical team at 2 weeks and 6 months and
again scored using the VAS and OSS questionnaires.
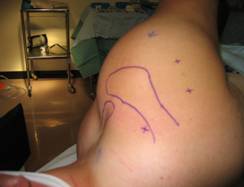
Figure 1: Location of 3 arthroscopy
portals
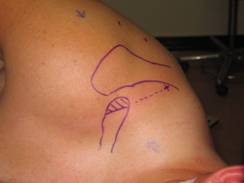
Figure 2:
Illustrates the
position of the second posteromedial working portal superior to
the spine of the scapula in line with a posterior projection of
the ACJ.
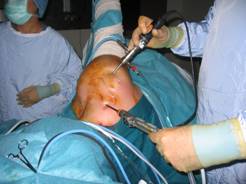
Figure 3:
Insertion of shaver to perform complete
resection of ACJ
Results :
100 consecutive patients (100 shoulders) were followed
prospectively. There were 58 men and 42 women with a mean age of
58 (39-75). The dominant arm was operated on in 64 patients. The
mean follow-up was 7 months (6-14). 35 patients had a full
thickness rotator cuff tear confirmed at arthroscopy and 19 had
evidence of Grade 2 or above osteoarthritis on either the
humeral head or glenoid surface. The mean preoperative VAS was
7.2 decreasing to 3.8 at 2 weeks and 3.0 at 6 months, no
patients reported an increase in their VAS score. The mean
pre-operative oxford score was 22.4, 30.8 at 2 weeks and 34.2 at
6 months. The average time to return to driving was 9 days
(2-36) and to work was 12 days (1-42) 21 patients did manual
work.
In the cohort who had a full thickness rotator cuff tears the
mean pre-operative VAS was 6.9 and at 6 months post op was 3.2.
The mean increase in Oxford shoulder score from pre-operative to
6 month follow up was 13 (average 18 pre-op, 31 at 6 months).
All of these patients were offered a second procedure to repair
their cuff tears but none accepted as they were all satisfied
with their pain and function post decompression. In the group of
patients with co-existing Glenohumeral osteoarthritis the mean
vas improved from 8.1 to 3.2 and the mean OSS from 20.7 to 33.4
at 6 weeks.
89 patients were done as day case procedures with 1 requiring
admission overnight for management of an allergic drug reaction
and 11 patients had their surgery on an in-patient list as a
result of medical co-morbidities. There were no early or late
complications from surgery and 100% of patients declared they
were satisfied with their surgery at 6 months, no patients went
on to have further shoulder surgery.
Discussion :
Our results show ASAD with EDC carried out through 3 posterior
portals as described above is an effective way of treating
coexistent impingement and ACJ degenerative change and in
particular has as much beneficial effect in patients with full
thickness rotator cuff tears and or GHJ arthritis as in those
with otherwise normal shoulders. The senior author (MP) started
using this portal in 1995 and has since performed over 1500
cases he has found it to be both simple and effective.
In 1999 Declercq (3) described the posteromedial working portal
used here for the acromioplasty and demonstrated that in
conjunction with a direct anterior portal it is effective for
performing concomitant decompression and resection of the AC
joint, our second posteromedial portal was developed as an
alternative to the addition of an anterior portal. We feel it
allows easier triangulation and more effective resection of the
distal clavicle, in particular the posterior portion, therefore
preventing the most common cause of failure of the procedure
incomplete resection of bone. The second posteromedial working
portal at the superior edge of the scapula spine allows direct
access to the ACJ in line with it, affording easy resection of
the distal clavicle whilst avoiding trauma to the soft tissues
posteriorly as a result of compression against the spine of the
scapula. Its approach through the muscle bulk of supraspinatus
greater than 5cm medial to the suprascapular notch means there
is no risk of damaging either the axillary or suprascapular
nerve. Levine et al (6) compared the bursal and direct
approaches to the distal clavicle in 2006 and found both to be
effective at treating AC joint arthrosis, however he found the
direct approach using posterosuperior and anteriosuperior
portals led to possible disruption of the superior capsular
ligaments which on occasions caused post operative ACJ
instability. This approach enters inferior to the ACJ and
prevents any risk of damage to the key stabilising structures.
It is the senior authors feeling that decompressive surgery
carried out in this way often provides satisfactory pain relief
and functional improvement in patients with degenerative rotator
cuff tears as to negate the need for further cuff repair surgery
and the morbidity associated with it. This is supported by our
results which indicate patients with full thickness cuff tears
or osteoarthritis of the glenohumeral joint have had equally as
much improvement in both their pain and functional scores as
those with otherwise normal shoulders, also no patients in our
series elected to have further surgery (either cuff repair or
arthroplasty).
Conclusions:
Arthroscopic subacromial decompression carried out using a third
posterior working portal located posteriorly at the superior
edge of the scapular spine and in-line with the
acromioclavicular joint is a safe and effective way of treating
sub-acromial impingement with coexisting degenerative change in
the ACJ.
Reference:
-
Neer CS. Anterior acromioplasty for the chronic impingement
syndrome in the shoulder. J Bone Joint Surg Am 1972;54:
41-50.
-
Ellman H. Arthroscopic subacromial decompression: Analysis of
one- to three-year results. Arthroscopy 1987;3:173-181.
-
Fischer, BW, MD Arthroscopic subacromial decompression.
Arthroscopy, Vol 15, No 3 (April), 1999: (pp 241-248)
-
Declercq G, M.D., Petre´D, M.D., and De Mulder K, M.D.
A
posteromedial working portal for arthroscopic subacromial
decompression and acromioclavicular joint arthroplasty.
Arthroscopy: The Journal of Arthroscopic and
Related Surgery, Vol 15, No 4 (May-June), 1999: pp 456458
-
Neviaser TJ.
Arthroscopy of the shoulder.
Orthop Clin North Am.
1987;18:361372
-
Levine W, M.D., Soong M, M.D., Ahmad S, M.D., Blaine T, M.D.,
and Bigliani L, M.D. Arthroscopic Distal Clavicle Resection: A
Comparison of Bursal and Direct Approaches.
Arthroscopy: The Journal of Arthroscopic and Related Surgery,
Vol 22, No 5 (May), 2006: pp 516-520
-
Woolf S, M.D.,Guttmann D, M.D., Karch M, M.D., Lubowitz J, M.D.
The Superior-Medial Shoulder Arthroscopy Portal Is Safe.
Arthroscopy: The Journal of Arthroscopic and Related Surgery,
Vol 23, No 3 (March), 2007: pp 247-250
|





