|
Abstract:
A forty four year old gentleman presents to
the Emergency Department following an injection of paint thinner
bilaterally into his antecubital fossa in an attempted suicide.
The injections resulted in erythematous, tense, and painful
swellings over the volar aspects of his forearms. The patient
underwent extensive surgical debridement and washout for toxic
fat necrosis.
He consequently developed a local abscess in his left
antecubital fossa requiring incision and drainage. Subsequently,
the patient was transferred to a regional specialist plastics
centre for secondary closure of the wounds with split skin
grafting.
Reports of subcutaneous injection of hydrocarbons in the medical
literature are few and far between. There are no clear
guidelines for management with some articles describing an
initial conservative approach, while others advocating immediate
surgical exploration of the affected area. We believe that early
surgical intervention was critical in preventing
limb-threatening complications and that individual case
reporting should be encouraged to provide evidence-based
guidelines.
J.Orthopaedics 2010;7(3)e4
Keywords:
hydrocarbon toxicity; subcutaneous injection;surgical
debridement
Introduction:
Hydrocarbons are a heterogeneous group of organic substances
that are primarily composed of carbon and hydrogen molecules. It
is abundant in modern society such as in paint, gasoline,
lighter fluid, and cleaning products.
Hydrocarbon intoxication has been commonly seen in domestic
accidents and attempted suicide (1). Inhalation and ingestion of
hydrocarbons have been well documented and can affect many
different organs causing pulmonary, cardiovascular and central
nervous system toxicity. However there have been very few
documented reports on subcutaneous injection of hydrocarbons.
Subcutaneous injection of petroleum distillate was originally
documented in World War I when soldiers injected themselves with
naphtha to escape military training (3).
The affects of hydrocarbon injection locally can range from mild
cutaneous irritation to myonecrosis and compartment syndrome.
Systemic effects can be profound causing severe pneumonitis,
neurological impairment coma and even death.
Case Report
A forty four year old gentleman presented to the Emergency
Department after injecting paint thinner into both his the
antecubital fossa in an attempted suicide. He used a
subcutaneous insulin injection pen to inject 3ml of paint
thinner into his arms. He attempted to inject the substance into
his veins, but was unable to penetrate the vein. He consequently
gave himself multiple subcutaneous injuries localised to his
arms.
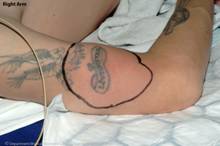
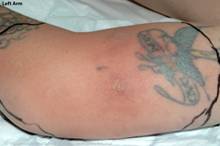
On presentation to the Emergency Department 11 hours after
injecting, the patient had erythematous, tense swellings, with
the left arm much more extensive than the than right (Figure a,b).
He displayed no signs of systemic toxicity with normal blood
haematology, biochemistry and liver function tests.
The patient was taken direct to theatre where we found extensive
fat necrosis, which was debrided. His wounds were washed out,
packed with gauze and left open. A prophylactic regimen of
intravenous benzylpenicillin and flucloxacillin were initiated.
The wounds were monitored on the ward for signs of local
complications, such compartment syndrome.
Postoperatively the patient developed pyrexia and two days later
he was taken back to theatre for further washout and debridement
of necrotic tissue. A small amount of pus was noted at the
operation and swabs were sent for microscopy and culture. Again
the wounds were left open and packed with gauze with a plan to
return to theatre for further inspection and debridement.
On return to theatre three days later the lesion on his left arm
was debrided back to bleeding tissue with a vacuum dressing
applied over a large defect. Liquefied fat necrosis was removed
from a smaller defect from his right arm, and a vacuum dressing
applied.
Following his third operation he improved clinically with
reduced pain and improved range of movement. However five days
later he developed tense collection in the left antecubital
fossa accompanied with a spike in his temperature and raised
inflammatory markers. He was subsequently taken to theatre for a
fourth time where 50-75ml of frank pus was drained from a large
abscess. Microbiology swabs taken during the procedure showed no
growth confirming a sterile abscess.
The plastic surgical team were consulted from the initial
presentation and he was later transferred to a tertiary centre
for split skin grafting. From early on in his admission the
psychiatric team were involved in the care of the patient, and
he will receive ongoing care in the community.
Discussion :
Hydrocarbons are an abundant substance in modern society and are
accessible
in products
such as gasoline, turpentine, furniture polish and household
cleansers. The physical property of hydrocarbons causes toxicity
by solubilizing membrane lipids and disrupting their integrity
(1,5). It is postulated that the hydrogen and carbon molecules
dissolve in the lipid rich membranes of the microvasculature
causing a defatting process and tissue necrosis (7). They
distribute along tissue planes causing release of tissue
mediators and inflammation through the soft tissues (1,5).
We reviewed the documented cases in the literature of
subcutaneous injection of hydrocarbons, and there is some debate
in the management of these patients, in particular relating to
operative or conservative management, and also in the use of
antibiotics.
The timing of surgical intervention is controversial (1-5).
Shusterman et al have described their management to be similar
as for a chemical cellulitis. They adopt and initial
conservative approach with elevation and immobilisation,
monitoring closely for limb threatening complications. They do
not feel immediate wide surgical exploration of the affected
area is necessary but that surgical debridement may well
eventually be required. (1,2).
On the contrary, Kjossev and Losanoff from Sofia Bulgaria report
seeing patients with soft tissue petroleum distillate injection
once or twice a year in their emergency department. They comment
that subcutaneous injection of less than 2cc of petroleum
distillate results in fever, leukocytosis, and local abscess or
extensive cellulitis. Their policy in the management of these
patients is immediate, wide surgical exploration of the affected
area followed by daily dressings for monitoring of the spread of
necrosis (3).
Another report by Farahvash et al from Iran published a case
series of twenty-one patients presenting with hydrocarbon
injection between 2001-2005 (5). They believe that from their
experience early surgical intervention is important, and that a
delay in surgical intervention would allow the noxious agent to
cause irreversible necrosis and possible suppuration (5,6).
However, having argued the above, they conclude by stating that
they feel surgical intervention is necessary when conservative
management fails and/or local complications occur.
The use of antibiotic therapy is another area of controversy.
There are no clear controlled studies available to determine if
prophylactic antibiotics are beneficial in the management of
these cases (1). Shusterman et al argue that antibiotic
treatment should be considered on an individual basis, but is
probably not helpful in the absence of sepsis or suprainfection
of the wound (1). Kjossev and Losanoff agree that abscess
content is usually sterile and even argue that early surgical
debridement renders systemic antibiotic therapy unnecessary (3).
However since the injection of hydrocarbons invariably occurs
with non-sterile injection technique, they stress that Tetanus
toxoid is mandatory (3). Farahvash et al recommends that
intravenous antibiotics along with elevation of affected limbs
are the main part of the treatment in these patients (5).
Conclusions:
What remains clear is that the initial management of these
patients, following the initial resuscitation, stabilisation and
adequate analgesia, should be the prevention or supportive
treatments of systemic complications (5,6). The patient should
have affected extremities elevated and immobilised. Injection
sites need close monitoring for local complications such as
compartment syndrome.
We believe that early aggressive surgical intervention was
critical in preventing further limb-threatening complications.
The initial clinical findings may not be consistent with the
amount of potential damage to the skin and underlying
structures, and therefore early surgical exploration and
debridement is essential. We believe prophylactic antibiotics do
have an important role in the prevention of secondary bacterial
infection and that early discussion with a microbiologist can
help guide treatment. Finally, a multidisciplinary team approach
with early involvement of plastic surgeons, microbiologists,
psychiatric team, and other allied professionals are important
in the overall care of these patients.
a:
b:
c:

d:
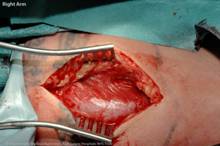
(a,b) Dolor rubor and tumor of antecubital fossa around the
injection sites. (c,d) Pictures taken at the initial operation-
Fat necrosis seen extensively on the left side.
Reference:
-
Shusterman EM, Williams SR, Childers BJ. Soft tissue injection
of hydrocarbons: a case report and review of the literature. J
Emerg Med 1999;17:63-5
-
Rush MD, Schoenfield CN, Watson WA. Skin necrosis and venous
thrombosis from subcutaneous injection of charcoal lighter
fluid (naptha). Am J Emerg Med 1998;16: 508-11
-
Krastanov P et al J Emerg Med. 1999 Nov-Dec;17(6):1073-4
-
Krastanov P, Kjossev K, Losanoff, Iliev I, Mitev P,
Mutafehijski V. Subcutaneous naptha injection: a review of 48
cases. Br J Surg 1996;83(S2):65
-
Mohammad
Reza Farahvash, Rooh-Allah Yegane, Mohammad Bashashati, Mina Ahmadi,
Nasim Tabrizi.
Surgical
approach to hydrocarbon injection in upper extremities: Case
series. International Journal of Surgery 2009;7:382-386
-
Terzi C,
Bacakoglu A, Unek T, Ozkan MH. Chemical necrotizing fascitis
due to household insecticide injection: is immediate radical
surgical debridement necessary? Hum Exp Toxicol 2002
Dec;21(12):687-90
-
Machle W.
Gasoline intoxication JAMA 1941;117:1965-71
|






