|
Chikahisa Higuchi, Akio
Nakura, and Hideki Yoshikawa
Department of Orthopaedic Surgery,
Osaka University Graduate School of Medicine,
2-2 Yamadaoka, Suita, Osaka 565-0871, Japan
Address for Correspondence:
Chikahisa Higuchi
Osaka University Graduate School of Medicine,
2-2 Yamadaoka, Suita, Osaka City, 565-0871, Japan
Phone :
81-6-6879-3552
Fax :
81-6-6879-3559
E-mail :
c-higuchi@umin.ac.jp |
|
Abstract:
Background: Pyomyositis is a rare disorder in children without
underlying diseases. It primarily caused by Staphylococcus
aureus. Especially, pyomyositis due to Streptococcus
pneumoniae is much rarer. We report a case of pneumococcal
pyomyositis in hip adductors of a child.
Case presentation: A 14-month-old girl without previous history
of disease developed infection of the adductor longus due to
Streptococcus pneumoniae. Pneumococcal pyomyositis in this
case was misdiagnosed as suppurative arthritis of the hip on the
affected side. Diagnosis of pyomyositis was determined by
clinical features including inflammatory signs around the medial
thigh and magnetic resonance imaging. Drainage of pyogenic
discharge and administration of antibiotics completely resolved
symptoms without complications.
Conclusions: Pnuemococcal pyomyositis in hip adductors is a very
rare condition in respect of pathogenic bacteria and lesion
site. A proper diagnosis and treatment is necessary when
encountered with this disease.
J.Orthopaedics 2010;7(2)e7
Keywords:
Pyomyositis; Streptococcus pneumoniae; hip adductor
Introduction:
Pyomyositis can occur in patients with underlying diseases such
as immunodeficiency. The disease is primarily caused by
Staphylococcus aureus. Pneumococcal pyomyositis (pyomyositis
due to Streptococcus pneumoniae) is a very rare
condition, and only a few cases in children < 15 years old have
been reported [1-5]. We report herein the case of an infant with
pneumococcal pyomyositis who was successfully diagnosed and
treated.
Case Presentation:
A 14-month-old girl was transferred to our hospital for
treatment of general fever and pain in the left lower limb. She
had suffered from severe cough and fever for 2 days before pain
around the left hip was identified. The first orthopedic surgeon
at a nearby hospital diagnosed septic arthritis of the hip. On
our first medical examination, she could move the affected lower
limb despite her bad humor. The left crotch was swollen and
reddish (Figure. 1).
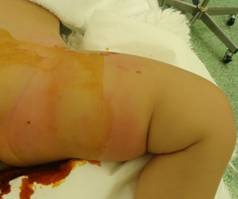
Figure-1:
Swelling and reddening thigh in the affected limb
Radiography of bilateral hip joints revealed lateral shift of
the left femoral head without osteolytic changes (Figure. 2).
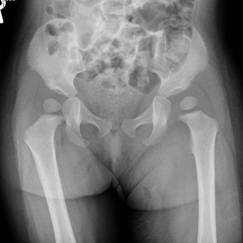
Figure-2:
Radiography revealed lateralization of the left femoral head
without osteolysis
Magnetic resonance imaging (MRI) disclosed the existence of a
lesion in the left thigh. Compared with muscle, that lesion was
isointense on T1-weighted imaging and hyperintense on
T2-weighted imaging (Figure 3).
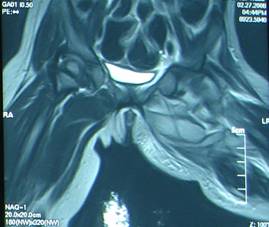
Figure-3: T2 MR image showed high-signal mass in left hip
adductor
This physiological and radiographic information led us to diagnose
pyomyositis in the adductor muscles. The abscess was emergently
removed by surgical intervention and drainage under general
anesthesia. Postoperatively, the patient was treated with
intravenous antibiotics until C-reactive protein levels reduced
to within normal range. No deformities of the hip joint or femur
were evident on the last examination (Figure 4).
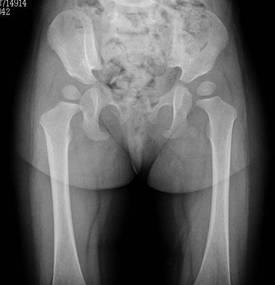
Figure-4: No deformity of left hip after treatment
Discussion :
Pyomyositis is a suppurative infection of skeletal muscles caused
by bacteria, and predominantly affects muscles around the hip
joint such as the quadriceps, gluteal muscles and obturator
internus [1-3, 6-10]. Misdiagnosis is common because the
uncommon nature of this entity. In particular, orthopedic
surgeons tend to misdiagnose this condition as septic arthritis
of the hip [4,11,12]. In the present case, septic arthritis of
the hip was initially diagnosed by a pediatrician and an
orthopedic surgeon. Laterality of the femoral head in hip
radiography seemed to be septic arthritis. However, we
identified two clinical features suggesting that septic
arthritis was the wrong diagnosis on our first examination. One
of these features was her active motion of the affected hip,
which is typically limited in cases of septic arthritis. The
other was the inflammatory skin lesion on the thigh. This
symptom was regarded as a sign of strong inflammation
immediately beneath the skin. These features led us to consider
other diagnoses. As most previous reports have suggested
[8,13,14], MRI was helpful in reaching the definitive diagnosis
in this case. As a result, the laterality of the femoral head
in the affected limb was judged to be caused by mass effect.
Pneumococcal pyomyositis is a pyogenic myositis caused by S.
pneumoniae, which has rarely been demonstrated to invade
muscles. Common pyomyositis is caused by S. aureus.
Streptococcus pyogenes is the second-most common etiological
agent. Pneumococcal pyomyositis is very uncommon, particularly
among children < 15 years old, and only 5 cases have been
reported [1-5]. Some cases showed a preceding upper respiratory
tract infection. None of the children with pneumococcal
pyomyositis had an underlying illness such as diabetes mellitus,
human immunodeficiency virus
infection, or connective tissue diseases. Conversely, younger
infants are known to have little ability to mount an immune
response to streptococcal infection [15]. Our patient also
displayed no underlying diseases and the first symptom was
cold-like. Skeletal symptoms appeared after several days. A
speculative route of infection in this case was hematogenous
spread and infection from the respiratory system to the hip
adductors.
Administration of antibiotics represents the first-choice therapy.
Some groups have reported that surgical drainage is not always
needed. However, this procedure should be performed if
antibiotics show a lack of effect. In the case of pyomyositis
with large abscess as in our patient (MRI revealed large abscess
in the thigh), an orthopedic surgeon should select the surgical
intervention. MRI is thus regarded as an indispensable
examination to determine the need for surgical drainage.
In summary, we have reported a case with pyomyositis caused by
S. pneumoniae in a 14-month-old girl. Successful diagnosis
and treatment depend on familiarity with the disease.
Reference :
-
Tuerlinckx D, Bodart E,
de Bilderling G, Nisolle J-F. Pneumococcal psoas pyomyositis
associated with complement deficiency. Pediatr Infect Dis J
2004, 23: 371-373.
-
Breton JR, Pi G, Lacruz
L, Calvo I, Rodriguez I, Sanchez A, Camarena JJ, Hernandez R.
Pneumococcal pyomyositis. Pediatr Infect Dis J 2001,
20: 85-87.
-
Steiner J, Septimus E,
Vartian C. Infection of the psoas muscle secondary to
Streptococcus pneumoniae infection. Clin Infect Dis
1992, 15: 1047-1048.
-
Renwick S, Ritterbusch
J. Pyomyositis in children. J Pediatr Orthop 1993, 13:
769-772.
-
Oliff M, Chuang V.
Retroperitoneal iliac fossa pyogenic abscess. Radiology
1978, 126: 647-652.
-
Chacha PB. Muscle abscesses in children.
Clin Orthop
1970, 70: 174-180.
-
Chiedozi LC. Pyomyositis: review of 205 cases in 112 patients.
Am J Surg
1979, 137: 255-259.
-
Peckett W, Butler-Manuel
A, Apthorp LA. Pyomyositis of the iliacus muscle in a child.
J Bone Joint Surg Br 2001, 83: 103-105.
-
John W-C, Mohammed B,
Sangam K. Physical signs in pyomyositis presenting as a
painful hip in children: a case report and review of the
literature. J Pediatr Orthop B 2004, .13: 211-213.
-
Dror O, Eli E, Liat B-S,
Ada K, Jacob B, David K, Moshe Y, Shlomo W, Franklin L.
Primary pyomyositis in children: a retrospective analysis of
11 cases. J Pediatr Orthop B 2007, 16: 153-159.
-
Andrew JG, Czyz WM. Pyomyositis presenting as septic
arthritis: a report of 2 cases.
Acta Orthop Scand
1998, 59: 587-588.
-
De Boeck H, Noppen L, Desprechins B: Pyomyositis of the
adductor muscles mimicking an infection of the hip: diagnosis
by magnetic resonance imaging: a case report.
J Bone Joint Surg Am
1994, 76-A: 747-750.
-
Karmazyn B, Loder RT,
Kleiman MB, Buckwalter KA, Siddiqui A, Yig J, Applegate KE.
The Role of Pelvic Magnetic Resonance in Evaluating Nonhip
Sources of Infection in Children With Acute Nontraumatic Hip
Pain. J Pediatr Orthop 2007, 27: 158-164.
-
Omar AG, Lawson AB C, S
Tyler H, Richard HB, Lori AT, Shellye EC. The Impact of the
Current Epidemiology of Pediatric Musculoskeletal Infection on
Evaluation and Treatment Guidelines. J Pediatr Orthop
2008, 28: 777-785.
-
Bruyn GAW,
Zegers BJM, van Furth R. Mechanisms of host defense against
infection with Streptococcus
pneumoniae. Clin Infect Dis 1992, 14: 251-262.
|






