|
Abstract:
Purpose:
To report our early experience with PERI-LOC plate fixation for
Distal Femoral and Proximal Tibial Fractures. The study reports
on (1) the time to callus formation and radiographic union (2)
range of knee motion, (3) the complications and (4) the
comparison with early results of LISS plate fixation.
Methods:
We retrospectively reviewed the results with PERII-LOC plate
(Smith & Nephew Inc) for 11 distal femoral (all closed) and 4
proximal tibial fractures (1 open) between January 2006 and May
2009. The mean follow up was 11 months (Range 6 22 months).
Results:
In Distal Femoral Fractures, the time to callus formation was
6.5 weeks (Range 5 11) and radiographic union 14 weeks (Range
10 22 months). The range of motion (knee) was 110 degrees
(Range 65 135) and the loss of extension 10 degrees (Range 0
15). Two minor complications, one plate irritation, one
superficial wound ooze was observed. In Proximal Tibial
Fractures, the average time to callus formation was 6
weeks ( Range 5 7 ) and to radiographic union 12
weeks( Range 11 -13 ). The average range of motion (knee) was
115degrees (Range 105 - 125) and the average lack of extension
was 10 degrees (Range 5 15). There were 2 complications, both
plate irritations.
Conclusion:
Our study shows that the early results with the PERI-LOC plate
for distal femoral and proximal tibial fractures are comparable
to that of the LISS plate. We feel that further studies are
needed to prove the long term role of the PERI-LOC plates.
J.Orthopaedics 2010;7(2)e12
Keywords:
Distal Femoral Fractures; Proximal Tibial Fractures; Less
invasive stabilisation system (LISS), PERI-Loc plates; Minimal
invasive surgery; internal fixation.
Introduction:
The management of Distal Femoral and Tibial Plateau Fractures
has evolved during the past decade from non-operative treatment
to relatively rigid internal fixation (2,5,9,17,19,24).
The aim is to achieve rapid bony union and allow early
mobilisation of the knee joint minimising the risks of joint
stiffness. Several implants have been developed to achieve these
goals with varying results (34, 35) Early techniques
of Osteosynthesis emphasized anatomic reduction and rigid
fixation. Surgical approaches were often extensive and added to
the soft tissue damage already present (11,16,39,40)
Recently, the optimisation of fracture environment has been the
focus of treatment in order to improve fracture healing and to
minimise complications. The concept of Indirect Reduction and
Minimally Invasive Plate Osteosynthesis (MIPO) has evolved,
illustrating the importance of preservation of bone biology
(12, 22, 24). Modern fracture fixation techniques
encourage the use of implants which can be inserted with minimal
soft tissue dissection, thus preserving bone and soft tissue
vascularity. These implants have been designed with sound
biomechanical properties allowing early mobilisation and
promoting healing before implant failure (15).
This study reviews our initial experience with the PERI-LOC
plate for the treatment of distal femoral and proximal tibial
fractures.
Materials
and Methods:
Between January 2006 and May 2009, 15 consecutive patients with
11 distal femoral and 4 proximal tibial fractures had PERI-LOC
plates inserted. Criteria for inclusion in the study were: all
distal femoral and proximal tibial fractures treated with PERI-LOC
plate. All notes and radiographs were retrospectively reviewed
independently. Patients were followed up at 1, 2, 6 weeks, 3
months, 6 months and thereafter depending on the clinical and
radiological progress. Union was defined as full weight bearing
without pain and radiological callus in two planes at right
angles to each other. The mean follow up was for 11 months,
Tibial Fractures 8 14 months, Femoral Fractures 6---22 months.
Surgical technique:
Tibia /Femur
All closed fractures had a closed technique using the PERI-LOC
Jig. A limited surgical approach through a curved incision was
performed. The Deep Fascia was opened and sub muscular plane
developed with a cobb elevator .The articular portion of the was
reduced, temporary stabilised with k wires and Cannulated Screws
inserted. The plates were inserted sub muscularly and checked
with using biplanar Image Intensification. All the patients
routinely received 3 doses of IV antibiotics (Cefuroxime) at
induction followed by 2 doses postoperatively. CPM was commenced
immediately. They were non weight bearing for 2 weeks, Toe-touch
bearing for 4 to 6 weeks and full weight bearing depending on
the progress of the fracture healing.
Results :
|
|
Femoral Fractures
11 |
Tibial Fractures
4 |
|
Males Females |
4 :7 |
4 : 0 |
|
Age
yrs |
72 (55-92) |
49 (3860) |
|
Mechanism of injury |
9 Fall 2 R.T.A. |
4 Fall |
|
Injury to Operation
days |
2.5 |
2.5 |
|
Classification
AO / Number |
33A 5 3 Per Prosthetic
33B 2
33C 4 |
41B1 2
41C3 2 1 open |
|
Surgeon Grade
SPR : Con |
5 : 6 |
1 : 3 |
|
Operation Time
mins |
72 (50110) |
75 (55-100) |
|
Plate Size
cms |
4.5 |
4.5 |
|
Hospital Stay
days |
22.5 (1055) |
22.5 (555) |
Fig 1.
Demographic Details
|
|
Femoral |
Tibial |
|
Mobility |
Pre op |
Post Op |
Pre op |
Post op |
|
Independently Mobile |
7 |
5 |
4 |
3 |
|
Walking Stick |
2 |
4 |
|
1 |
|
Zimmer Frame |
1 |
1 |
|
|
|
Wheelchair |
1 |
1 |
|
|
Fig 2 Mobility Pre and Post Surgery
|
|
Femoral Plating |
Tibial Plating |
|
Callus Formation
Weeks |
6.5 (511) |
6 (6-7) |
|
Radiological Union
Months |
3.5 (2.55.5) |
3 (2.753.25) |
|
Range of motion Knee
Degrees |
110 (65135) |
115 (105-125) |
|
Lack of Extension
Degrees |
10( 015) |
10 (5-15) |
|
Complications |
1 Plate Irritation
1 Superficial Wound Problem |
2 Plate Irritation |
Fig 3 Results of Healing
Distal Femoral Fractures 11 cases
The time to callus formation was 6.5 weeks (Range 5 11). The
time to radiographic union was 3.5 months ( Range 2.5 5.5
months ). The range of motion at last clinic review was 110
degrees ( Range 65 135) and the lack of extension was 10
degrees ( Range 0 15). There were 2 minor complications in
this group. One patient developed Plate Irritation One patient
developed a wound discharge. Both settled with time. No plate
was removed.
Proximal Tibial Fractue 4 Cases
Time to callus formation was 6 weeks (Range 5 7). Time to
radiographic union was 12 weeks (Range 11 -13). The range of
motion at last clinic review was 115 degrees (Range 105 - 125)
and the lack of extension was 10 degrees (Range 5 15). 2
patients complained Plate Irritation and one plate was removed
after 6.5 months. The other case has not had the plate removed
yet.
Discussion :
Treatment Methods for Distal Femoral and Proximal Tibial
fracture have undergone
a major change in the last few years
(1,2,5,6,9,10,11,13,17,19,30,31,38).
External fixation with limited joint line internal fixation is
the norm. With the recent development of locking plates more
internal fixation has been advocated with a minimal invasive
approach (MIPPO). Kruttek et al took this concept further by
emphasising the need to obtain relative rather than absolute
stability of the fracture. He also suggested minimal
interference with the zone of the injury which was achieved by
sliding plates in the sub-muscular plane on the lateral side of
the femur (minimally invasive percutaneous plate osteosynthesis
MIPPO). (4,8,12,18,22,25) Mast et al first reported
the importance of reduced surgical dissection of the fracture
site and utilised the surrounding soft tissues for fracture
reduction (24). He termed this indirect reduction of
the fracture. This helps to maintain blood supply to the bone
ends and reduces non union rates (4,24).
The LISS plate was developed to complement the concept of the
MIPPO technique(3,7,14,15,20,21,23,26-29,32,33,36,37,41).
It consists of a precontoured plate to the bone block utilising
multiple fixed angle screws. Utilising the cantilever principle,
the bone plate interface closely resembles an external fixator.
It is not surprising that it has been called an Internal Fixator.
Its other main advantage is preservation of bone biology,
eliminating the need for bone grafting in most cases.
(20,21,23) The PERI-LOC plate incorporates all the
advantages and principles of the LISS plate with better
contouring.
Our Results are comparable to previous LISS studies. To our
knowledge, there have been no published results using the PERI-LOC
plate for Distal Femoral Fractures. The PERI-LOC plate has
specific design features. This plate has a bevelled tip
proximally to allow easy sub muscular insertion of the plate.
There are scallops distally to allow for the easy placement of
independent articular lag screws close to the joint surface.
Each hole in the plate can accept 4 different screws 4.5mm non
locking screw, 4.5mm locking screw, 5.7mm cannulated locking
screw and 6.5mm partially threaded cancellous screw unlike the
LISS plate. The contouring in the plate design is more
anatomical hence less plate irritation. Our results show
comparable time to callus formation and union as the LISS
series. The better plate design has lead to fewer complications
particularly plate irritation.
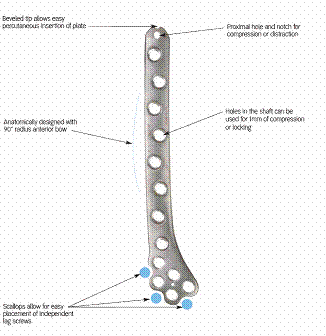
Femoral PERI-LOC plate
|
|
Femoral # Numbers |
Callus time Weeks |
Union time
weeks |
R.O.M. knee |
Complications |
|
Fankhauser |
30 |
5 |
12 |
106 (4) |
7
Plates Irritation
Removed |
|
Wong
|
16 |
|
30 |
|
2
Plates Loose
Removed |
|
Warrington
|
11 |
6.5 |
14 |
110 |
2
Plate Irritation
Settled
|
Fig 4 Distal Femoral LISS studies
|
Tibial Fractures No. |
Callus time Weeks |
Union time
weeks |
R.O.M. knee |
Complications |
|
Bolin 26 |
5.7 |
11 |
|
2 early knee arthritis |
|
Cole 77 |
|
12.6 |
122 |
2 loss of fixation
2 non union
2 infection
1 Peroneal palsy |
|
Stannard 35
(36) |
6.6 |
16.9 |
116 |
2 infections |
|
Warrington 4 |
6 |
12 |
115 |
2 Plate Irritation |
FIG 5 Proximal Tibia / LISS Studies
There have been no published results using the PERI-LOC plate
for Proximal Tibial Fractures. PERI-LOC Tibial plates come in
two sizes 3.5cm and 4.5cm. The plates have a scalloped edge
which allows for easy placement of independent lag screws for
reduction of articular surface. The plate head has a 5 degree
posterior tilt and is contoured to match the lateral proximal
tibia. There are also 3 additional small holes proximally for
meniscal repair. The plate shaft has a 3 degree bend to match
the diaphysis of tibia. There is a bevelled tip distally which
allows for the easy percutaneous insertion of the plate. Each of
the holes can accept 4 different screws 4.5mm non locking screw,
4.5mm locking screw, 5.7mm cannulated locking screw and 6.5mm
partially threaded cancellous screws.
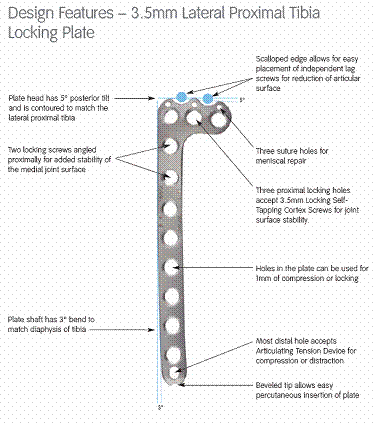
Tibial PERI-LOC Plate
Our hypothesis that the results of the distal femoral and
proximal tibial fractures fixed with the PERI-LOC plate are
comparable to that of the LISS plate have been affirmed
considering the time to callus formation, time to union, range
of motion and the incidence of complications. The PERI-LOC plate
system is user friendly and no specific technical difficulties
were encountered. This plate incorporates the advantages of
minimally invasive surgical techniques with a fixed angle
device. We believe the better anatomical contouring; bevelling
and wider choice of screws gives it an advantage over other
similar systems.
The limitation of our study is the relatively small number of
patients included Also it is a retrospective study and there is
no control group. This is a preliminary report of results of a
new system of osteosynthesis. Longer term follow up may add
findings that lead to additional conclusions. The strengths of
conclusions would certainly be enhanced with a randomised
prospective study to prove the long term role of PERI-LOC in the
management of distal femoral and proximal tibial fractures.
Conclusion:
Our study shows that the early results with the PERI-LOC plate
for Distal Femoral and Proximal Tibial fractures are comparable
to that of the LISS plate. We feel that further studies are
needed to prove the long term role of the PERI-LOC plate.
Reference :
-
Benirschke SK, Agnew SG, Mayo KA, Santoro VM, Henley MB.
Immediate internal fixation of open complex tibial plateau
fractures: treatment by a standard protocol. J Orthop Trauma
1992; 6:78-86.
-
Blokker CP, Rorabeck CH, Bourne RB. Tibial plateau fractures.
An analysis of the results of treatment in 60 patients. Clin
Orthop Rel Res 1984; 182:193.
-
Boldin C, Fankhauser F, Hofer HP, Szyszkowitz R. Three year
results of proximal tibia fractures treated with the LISS.
Clin Orthop Rel Res 2006; 445:222-29.
-
Bolhofner B, Carmen B, Clifford P. The results of open
reduction and internal fixation of distal femur fractures
using the a biologic reduction technique. J Orthop Trauma
1996; 10:372-7.
-
Burri C, Gartzke G, Coldewey J, Muggler E. Fractures of the
tibial plateau. Clin Orthop Rel Res 1979; 138:84.
-
Butt M, Krikler S, Ali M. Displaced fractures of the distal
femur in elderlypatients.Operative versus non operative
treatment. J Bone Joint Surg 1996;78B:110-4.
-
Cole PA, Zlowodski M, Kregor PJ. Treatment of proximal tibia
fractures using the Less invasive stabilisation system. J
Orthop Trauma 2004; 18:528-34.
-
Collinge C, Sanders R, DiPasquale T. Treatment of complex
tibial periarticular fractures using percutaneous techniques.
Clin Orthop Rel Res 2000;375:69.
-
Connolly J, Dehne E, Lafollette B. Closed reduction and early
cast brace ambulation in treatment of femoral fractures.
Results in one hundered and forty three fractures. J Bone
Joint Surg 1973; 55A:1581-99.
-
Dendrinos GK, Kontos S, Katsenis D, Dalas A. Treatment of high
energy tibial plateau fractures by the Ilizarov circular
fixator. J Bone Joint Surg 1996; 78:710.
-
Duwelius PJ, Rangitsch MR, Colville MR, Woll TS. Treatment of
tibial plateau fractures by limited internal fixation. Clin
Orthop Rel Res 1997;339-47.
-
Farouk O, Krettek C, Miclau T, Schandelmaier P, Guy P,
Tscherne H. Minimally invasive plate osteosynthesis: does
percutaneous plating disrupt femoral blood supply less than
the traditional technique? J Orthop Trauma 1999; 13:401-6.
-
Firoozbaksh K, Behzadi K, Decoster TA, Moneim M, Naragi F.
mechanics of retrograde nail versus plate fixation for
supracondylar femur fractures. J Orthop Trauma 1995; 9:152-7.
-
Frankhauser F, Gruber G, Schippinger G, Boldin C, Hofer HP,
Greechenig W, Szyszkowitz R. Minimal invasive treatment of
distal femoral fractures with the LISS. Acta Orthop Scand
2004; 75:56-60.
-
Frigg R, Appenzeller A, Christensen R, Frenk A, Gilbert S,
Schavan R. The Development of the distal femoral LISS. Injury
2001; 32(3):24-31.
-
Gaudinez RF, Mallik AR, Szporn M. Hybrid external fixation of
comminuted tibial plateau fractures. Clin Orthop 1996;
328:203-210.
-
Giles JB, DeLee JC, Heckman JD, Keever JE. Supracondylar
intercondylar fractures of femur treated with a supracondylar
plate and lag screw. J Bone Joint Surg 1982; 64A:864-870.
-
Goesling T, Frenk A, Appenzeller A, Garapati R, Marti A,
Krettek C. LISS plate: design, mechanical and biomechanical
characteristics. Injury 2003; 34:11-15.
-
Henry SL. Supracondylar femur fractures treated percutaneously.
Clin Orthop 2000; 375:51-9.
-
Kregor PJ, Hughes JL, Cole PA. Fixation of distal femoral
fractures above total knee arthroplasty utilising LISS. Injury
2001; 32:64-75.
-
Kregor PJ, Stannard J, Zlowodski M, Cole PA, Alonso J. Distal
femoral fracture fixation utilising the less invasive
stabilisation system: the technique and early results. Injury
2001; 32:32-47.
-
Krettek C, Muller M, Miclau T. Evolution of minimally invasive
plate osteosynthesis in the femur. Injury 2001; 32:14-23.
-
Marti A, Frankhauser C, Frenk A, Cordey J, Gasser B.
Biomechanical evaluation of the less invasive stabilisation
system for the internal fixation of distal femoral fractures.
J Orthop Trauma 2001; 15:482-7.
-
Mast J, Jakob R, Ganz R. Planning and reduction techniques in
fracture surgery. New York: Springer-Verlag; 1989.
-
Miclau T, Holmes W, Martin RE, Krettek C, Schandelmaier P.
Plate osteosynthesis of the distal femur: surgical technique
and results. J South Orthop Assoc 1998; 7:161-70.
-
Panasiuk M, Kmieciak M. Treatment of periprsthetic fractures
of the distal femur with the LISS system. Chir Narzadow Ruchu
Orthop Pol 2004; 69:369-71.
-
Ricci WM, Rudzki JR, Borrelli J. Treatment of complex proximal
tibia fractures with the less invasive stabilisation system. J
Orthop Trauma 2004; 18:521-27.
-
Schandelmaier P, Krettek C, Miclau T. Stabilisation of distal
femoral fractures using the LISS. Tech Orthop 1999; 14:230-46.
-
Schandelmaier P, Partenheimer A, Koenemann B, Grun OA, Krettek
C. Distal femoral fractures and LISS stabilisation. Injury
2001; 32:55-63.
-
Schatzker J. Fractures of the distal femur revisited. Clin
Orthop 1998; 347:43-56.
-
Schatzker J, Lambert DC. Supracondylar fractures of the femur.
Clin Orthop1979; 138:77-83.
-
Schutz M, Muller M, Kaab M, Haas N. LISS in the treatment of
distal femoral fractures. Acta Chir Orthop Traumatol Cech
2003; 70:74-82.
-
Schutz M, Muller M, Krettek C, Hontzsch D, Regazzoni P, Ganz
R, Haas N. Minimally invasive fracture stabilisation of distal
femoral fractures with the LISS: a prospective multicenter
study. Injury 2001; 32:48-54.
-
Siliski JM, Mahring M, Hofer HP. Supracondylar intercondylar
fractures of the femur. Treatment by internal fixation. J Bone
Joint Surg Am 1989; 71A:95-104.
-
Slatis P, Ryoppy S, Huittinen VM. AO osteosynthesis of
fractures of the distal third of the femur. Acta Orthop Scand
1971; 42:162-72.
-
Stannard JP, Wilson TC, Volgas DA, Alonso JE. Fracture
stabilisation of proximal tibial fractures with the proximal
tibial LISS: Early experience. Injury 2003; 34:36-42.
-
Syed AA, Agarwal M, Giannoudis PV, Matthews SJ, Smith RM.
Distal femoral fractures: long term outcome following
stabilisation with the LISS. Injury 2004; 35:599-607.
-
Tees JD. Fracture of the lower end of the femur. Am J Surg
1937; 38:656-9.Waddell JP, Johnston DW, Neidre A. Fractures of
the tibial plateau: a review of ninety five patients and
comparison of treatment methods. J Trauma 1981; 21:376-381.
-
Watson JT. High energy fractures of the tibial plateau. Orthop
Clin North Am. 1994; 25:723-52.
-
Wong MK, Leung F, Chow SP. Treatment of distal femoral
fractures in the elderly using a less invasive plating
technique. Int Orthop 2005; 29:117-20.
|




