|
Abstract:
Legg-Calvé Perthes disease and Slipped Capital Femoral
Epiphysis (SCFE) in the same child occur very rarely. Only eight
such cases have been reported in the literature. We report a
case of SCFE occurring in a patient with Perthes disease who
also had proximal femoral osteotomy for the correction of
rotational mal-alignment.
Also, going through the literature it seems likely that slippage
of proximal femoral epiphysis after previous Perthes disease in
the contra lateral hip is most likely a coincidental
occurrence. We believe this case highlights a rare but
important clinical scenario which can have serious consequences
for the patient if not identified and treated appropriately.
J.Orthopaedics 2009;6(3)e9
Keywords:
Legg-Calvé Perthes; Disease, Slipped Capital Femoral Epiphysis;
Osteotomy; Retroversion; Rotational mal-alignment.
Introduction:
Legg-Calvé Perthes disease is the name given to idiopathic
osteonecrosis of the capital femoral epiphysis of the femoral
head. It is caused by an interruption to the blood supply of the
head of the femur and is typically found in young children aged
between three to 12 years. They present with hip, knee or groin
pain exacerbated by movements which can easily be dismissed as
growing pains. Its treatment varies between careful monitoring
to surgical intervention when necessary.
Slipped Capital Femoral Epiphysis (SCFE) is another condition
where there is posterior and inferior slippage of the proximal
femoral epiphysis on the metaphysic which occurs during the
adolescent growth spurt and is most frequent in obese children.
They too present with hip, knee or groin pain exacerbated by
movements. Its management involves either pinning in situ or
corrective osteotomy.
Although Perthes disease and SCFE are completely different
entities they both can present with similar symptoms in a
relatively similar age group. Diagnosing these diseases is often
enigmatic and unfortunately in many instances it is initially
missed. It is therefore important to have a clear understanding
of their manifestations and management as delay in their
treatment results in a less favourable long term prognosis.
Both of these are relatively unusual conditions in Children. The
reported incidence in Caucasians is about one in 6500 for
Perthes disease and only about one in 10000 for SCFE [1,2]. We
report a case where both these conditions were diagnosed and
treated effectively in the same child.
Case Report:
A six years old Caucasian male child presented with spontaneous
onset of a painful right hip of a few days duration. Radiographs
revealed changes consistent with Perthes disease with whole
head involvement but without any head at risk signs (Fig-1). He
was treated with analgesia and short periods of bed rest.
Subsequent follow up radiographs showed re ossification of
epiphysis.
Approximately two years later at the age of eight he was seen
with an abnormal gait. On examination, he had an external
rotation of 90° in extension at both hips with no internal
rotation possible. He also had increased external torsion in
both tibias. The child was mildly obese but did not have any
clinical evidence of neuromuscular disease or hyper laxity of
joints. There was no evidence of any other coexisting
abnormality, which could explain the rotational deformity of
both hips. He underwent bilateral femoral rotational osteotomies
with 45° of internal rotation at the level of lesser trochanter
(Fig-2). He was allowed full weight bearing after radiological
evidence of callus formation.
At the age of 10, he presented with a limp and painful left hip.
On examination, he had flexion 100° abduction 35° internal
rotation 20° and external rotation 35°. Radiographs suggested
mild slipping of proximal femoral epiphysis (Fig-3). Bone scan
showed increased uptake in the left hip. He underwent in situ
pinning with one 6.5mm AO screw after the removal of blade plate
(Fig-4). On subsequent follow up there was no evidence of
further slipping or avascular necrosis of the femoral head.
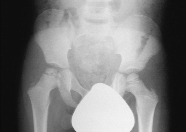
Fig1:
Initial anteroposterior radiograph of the pelvis showing the
evidence of Perthes disease of right hip.
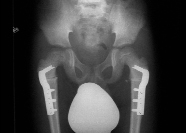
Fig2:Anteroposterior
radiograph of the pelvis after the corrective osteotomy of the
proximal femur showing re-ossification of the right femoral
head.
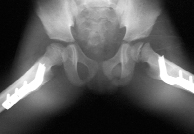
Fig3:Frog
leg lateral radiograph of the pelvis showing mild slip of the
left proximal femoral physis.
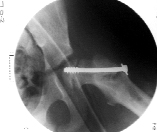
Fig4:Anteroposterior
radiograph of the left hip after insitu pinning of the left
proximal femoral epiphysis.
Discussion :
Slipped Capital Femoral Epiphysis and Legg-Calvé Perthes
disease in the same child occur very rarely. Only eight such
cases have been reported in the literature. Individual cases
were reported by Crawford and Markheim [3,4]. Graziano et al in
1987 reported a series of three cases [5]. Sutro in 1935 in his
series on the SCFE reported a patient whose radiograph showed
previous contra lateral Perthes disease [6]. Crawford
calculated the incidence of both occurring in the same child as
0.71-3.41/12000000. In all except one of the described cases in
the literature SCFE occurred in the contra lateral hip of
Perthes disease [3]. In 1992 Ruoff et al described one case of
SCFE which occurred in the ipsilateral hip after cheilectomy for
Perthes disease [7].
In all these cases no common risk factors were found. Also the
treatment options for Perthes disease were diverse and could
not be attributed as etiological factors for subsequent SCFE
(Table-1). Catterall et al in 1982 described the histological
changes in the physis of hip affected by Perthes disease. They
included a thinner physeal plate with irregular columns of
cartilage cells and tongues of unossified cartilage extending
into the metaphyseal region [8]. If these changes were to weaken
the physis and contribute to slipping of proximal femoral
epiphysis, the incidence of SCFE following Perthes disease
would be expected to be much higher both in clinical practice as
well as in the literature reported so far.
|
NUMBER |
AUTHOR |
AGE AT LCPD |
MANAGEMENT OF LCPD |
AGE AT SFCE |
MANAGEMENT OF SFCE |
|
1 |
Markhiem 1949 |
11 |
Skin traction
Ischial Calliper
Shoe Rise |
13 |
Skin Traction |
|
2 |
Crawford 1975 |
5 |
Split Russell Traction
Patten bottom brace |
6 |
Split Russell Traction |
|
3 |
Graziano 1987 |
9 |
Traction
Chielectomy |
14 |
In situ Knowles pin fixation |
|
4 |
Graziano 1987 |
4 |
Perthes sling |
12 |
Closed Reduction
Knowles pin fixation |
|
5 |
Graziano 1987 |
9 |
Contralateral hip showed old LCPD |
9 |
Insitu Knowles pin fixation |
|
6 |
Ruoff 1992 |
14 |
Chielectomy & greater trochanteric advancement |
16 |
Insitu percutaneous pin fixation |
|
7 |
Ruoff 1992 |
13 |
Toronto brace
Chielectomy |
14 |
Percutaneous pin fixation |
Table 1:
Data On Patients With Perthes Disease And Slipped Capital
Femoral Epiphysis
After three dimensional tomography in 22 hips with Perthes
disease and epiphyseal dysplasia Kim et al in 1997 proposed
functional retroversion and functional coxa vara [9]. In Perthes
disease deformed femoral head consists of two portions, an
antero-infero-lateral false head blocking the internal rotation
and a postero-medial-superior portion representing the true
articulating femoral head. The true head is retroverted in
relation to the antero-lateral segment resulting in functional
retroversion which causes an externally rotated gait [10].
Functional retroversion and functional coxa vara explain the
paradox of supposed increased antiversion on radiograph in a
child who walks with the externally rotated limb.
Retroversion of the proximal femoral epiphysis was supposed to
predispose to SCFE by altering the biomechanics across the
proximal femur. However if the functional retroversion in healed
Perthes disease is a contributing factor to SCFE their
coexistence should be a lot higher.
To determine the rotational profile of the lower limb a CT scan
was performed and it showed a 25º retroverted femoral head. A
45º de rotation osteotomy corrected the rotational profile of
the proximal femur from 25º retroversion to 25º anteversion.
Several ultra structural alterations of the physis were
documented in both Perthes disease and SCFE [10]. These include
reduction in the number of chondrocytes, chondrocyte
degeneration and haphazardly arranged collagen. The significance
of these changes in the physis is unknown and they may have a
causative role. Obesity predisposes to SCFE by two different
mechanisms, increased stresses across the physis and decreased
anteversion of femur.
In our patient, we used one 6.5 mm cannulated screw as that is
the standard practice and we did not have any further
complications. However, there have been concerns expressed in
the past about using this technique in this age group due to
growth disturbance of the proximal femur and premature physeal
closure which has led to the consideration of alternative
methods.
Segal et al in 1991 presented a series of 21 patients (33 hips)
where pinning for SCFE resulted into growth disturbances
including greater trochanteric overgrowth, coxa vara, and coxa
breva in 64% of the hips [11]. In 1988 Huggland et al presented
six boys with SCFE who were successfully treated using a hook
pin. The advantages of this technique are that it causes minimal
trauma, cannot slide back therefore does not loose epiphyseal
grip resulting into normal hip growth [12]. Guzzanti et al in
2004 presented 10 skeletally immature patients with SCFE who
were treated by using a modified cannulated screw. The threaded
portion of the screw was placed entirely within the epiphysis
and the screw head was allowed to remain two to three cm lateral
to the lateral femoral cortex. The screw used by them allowed
continued growth of the femoral neck, epiphyseal/physeal complex
and remodelling of the epiphysis and metaphysic [13].
Altered biomechanics following the de-roatation osteotomy and
obesity are two possible mechanisms which might have a
contributory role in the SCFE in our patient.
We agree with the other authors who have reported similar cases
that there is no common aetiological factor for the causation of
the Perthes disease and SCFE in the same child. It seems likely
that slippage of proximal femoral epiphysis after previous
Perthes disease in the contra lateral hip is most likely a
coincidental occurrence.
Reference :
-
Pillai A, Atiya S, Costigan PS (2005) The Incidence of Parthes
Disease in Southwest Scotland. J Bone Joint Surgery.Br.
87-B(11):1531-1535.
-
Murray AW, Wilson NIL (2008) Changing Incidence of Slipped
Capital Femoral Epiphysis. J Bone Joint Surgery.Br.
90-B(1):92-94.
-
Crawford A H (1975) Legg-Calve-Perthes Disease Coexistent
with Slipped Capital Femoral Epiphysis. J Bone Joint
Surgery.Am. 57-A(2):280-281.
-
Markheim HH (1949) LeggPerthes Disease and Slipped Epiphysis
in the Same Patient: A Case Report. J Bone Joint Surgery. Am.
31-A(3):666-668.
-
Graziano GP, Kernek CB, Derosa GP (1987) Coexistant
Legg-Calve-Perthes Disease and Slipped Femoral Epiphysis in
the Same Child. J Pediatr Orthop. 7(1):61-62.
-
Sutro CJ (1935) Slipping of the Capital Epiphysis of the Femur
in Adolescence. Arch Surg 31(3):345-360.
-
Ruoff MJ, Schwentker EP (1992) Legg-Calve-Perthes Disease and
Slipping of the Capital Femoral Epiphysis in the Same Child.
Orthopaedics. 15(9):1070-1072.
-
Catterall.A, Pringle J, Byers PD, Fulford GE, Kemp HB (1982)
Is the Epiphyseal Infarction Complete? J Bone Joint Surgery.
Br. 64(3):276-281.
-
Kim HT, Wegner DR (1997) Functional Retroversion of the
Femoral head in Legg-Calve-Perthes Disease and Epiphyseal
Dysplasia: Analysis of head neck deformity and its effects on
limb position using three dimensional computed tomography. J
of Pediatr Orthop. 17(2):240-246.
-
Aronsson DD, Loder RT, Breur GJ, Weinstein SL (2006) Slipped
Capital Femoral Epiphysis: Current Concepts. J Am Acad Orthop
Surg. 14(12):666-679.
-
Segal LS, Davidson RS, Robertson WW, Drummond DS (1991) Growth
Disturbances of the Proximal Femur after Pinning of Juvenile
Slipped Capital Femoral Epiphysis. J Pediatr Orthop.
11(5):631-637.
-
Huggland G, Bylander B, Hansson L I, Selvik G (1988) Bone
Growth After Fixing Slipped Femoral Epiphysis : Brief Report
. J Bone Joint Surgery.Br. 70-B(5):845-846
-
Guzzanti V, Falciglia F, Stanitski CL (2004) Slipped Capital
Femoral Epiphysis in Skeletally Immature Patients. J Bone
Joint Surgery.Br. 86-B(5):731-736
|






