|
Abstract:
Recurrent elbow dislocation is rare in the absence of associated
fracture. Treatment for chronic elbow instability is usually
ligamental reconstruction. We present a previously unreported
indication of total elbow arthroplasty in a case of recurrent
elbow dislocation in an elderly lady. She had excellent results
at two year follow up. The rationale for this new indication is
discussed.
J.Orthopaedics 2009;6(3)e8
Keywords:
elbow dislocation; total elbow
Case history:
A 69 year-old female with history of rheumatoid arthritis,
epilepsy, and Parkinson’s disease presented with a posterior
dislocation of her right elbow after a fall (figure I). No
associated fractures were detected on orthogonal radiographs of
the elbow. Clinically, there was no evidence of neurovascular
compromise before and after reduction. Post reduction
radiographs showed a well-reduced joint with no associated
fractures. As such, her elbow was immobilized at 90 degrees.
One week after injury, the range of motion at the elbow was
limited by her apprehension. Her arc of movement was between 10
to 90 degrees after three weeks of immobilization. She
underwent physiotherapist supervised elbow mobilization, and
managed to achieve full range of motion, two months later.
Subsequently, she sustained two further dislocations as a result
of falls, both required manipulative reduction. Her main
complaints were severe pain, instability, crepitus and
limitation in performing her activities of daily living.
Clinically, her elbow was grossly unstable, and was easily
dislocated. There were no manifestations of rheumatoid
arthritis in her elbow, although she did have a mild degree of
metacarpophalangeal subluxation, and ulnar deviation of her
fingers. The calculated Mayo Elbow Performance Score1
was 15. In view of her symptoms and medical problems, she was
offered total elbow arthroplasty.
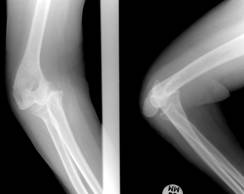
Fig. 1 Initial radiographs showing dislocation
The procedure was performed under general anaesthesia via
Bryan’s approach by the senior author (CHL). There was marked
attenuation of the medial and lateral collateral ligament
complexes and a moderate amount of chronic synovitis was
present. A Coonrad-Morrey semi-constrained total elbow
prosthesis (Zimmer, Warsaw, IN, USA) was inserted and cemented
(Simplex, Howmedica, Limerick, Ireland) with a third generation
cementing system. Gentle physiotherapy was commenced on the
third postoperative day and continued for the next few weeks.
She recovered uneventfully from the surgery and at three months
post op, she was able to resume her activities of daily living
independently (Figure 2 post operative radiograph). Her Mayo
Elbow Performance Score was 95. Two years on, she had 10 to 140
degrees of flexion, and prono-supination of 70/70.
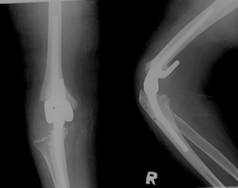
Fig. 2 Post operative radiograph
Discussion :
Recurrent elbow dislocation is rare in the absence of associated
fracture2. Following reduction and early range of
motion exercises, the majority of elbow dislocations remain
stable3. Most cases of chronic elbow instability is
attributed to injury of the lateral collateral ligament complex.
Medial elbow instability is usually associated with throwing
athletes4. Chronic elbow instability does not
improve over time. In the symptomatic patient, surgery is
justified. Surgical treatment for chronic elbow instability
without associated fractures is reconstruction of the lateral
collateral ligament complex with tendon grafts5, 6, 7.
Authors have reported using palmaris longus, semitendinosus,
plantaris, triceps fascia, and strips of tendo Achilles as
tendon autografts. The remaining attenuated soft tissue may be
imbricated to increase the lateral capsular tightness and
strengthen the repair. Complications of
reconstruction include delayed laxity, redislocation, and donor
site morbidity. Thus far, we are not aware of total elbow
arthroplasty being indicated in recurrent dislocations, or as a
salvage procedure for failed soft tissue reconstruction
procedure in elbow instability. The demographics of patients,
being younger, would account for this. However, there might be
a role for total elbow arthroplasty in the elderly patient with
lower functional demand who suffers from chronic elbow
instability or dislocations.
The co-existing rheumatoid arthritis in our patient strengthens
the case for arthroplasty. Long-term corticosteroid therapy
impairs tissue and wound healing. Disease activity in the elbow
may erode and destroy the soft tissue reconstruction, rendering
the elbow unstable, and subsequently requiring a revision
surgery. A semi-constrained total elbow arthroplasty is able to
provide elbow stability without the potential complications
associated with ligamental reconstruction. General consensus8
for cut-off age is 60, although in rheumatoid patients who
suffer from debilitating arthritis, the age limit is reduced to
30. The semi-constrained Coonrad-Morrey prosthesis has
favorable long-term results9, 10, 11, 12. Alridge et
al reports functional success in 50% of cases 10-14 years post
op, and 25% at 15-19 and 20-31 years. The complications of
total elbow arthroplasty include aseptic loosening, septic
arthritis, peri-prosthetic fractures, and polyethylene bushing
wear. Early implant failure is associated with lifting objects
more than 10lb or repetitive lifting greater than 2lb8.
Conclusion:
In elderly patients who suffer from recurrent dislocations and
chronic instability, total elbow arthroplasty provides stability
and symptomatic relief. The co-existence of arthritis – RA, OA,
etc. with instability makes a patient a suitable candidate for
arthroplasty. The caveat: patient must accept the limitation of
the implant.
Reference :
-
Morrey BF, An KN, Chao EYS. Functional evaluation of the
elbow. In The Elbow and Its Disorders, edited by B. F. Morrey.
Ed. 2, Philadelphia, W. B. Saunders, 1993
-
Duckworth AD, Ring D, Kulijdian A, et al. Unstable elbow
dislocations. J Shoulder Elbow Surg 2008; 17(2): 281-286
-
Mehlhoff TL, Noble PC, Bennett JB, Tullos HS. Simple
dislocation of the elbow in the adult. Results after closed
treatment. J Bone Joint Surg Am 1988; 70A: 244-249
-
Grace SP, Field LD. Chronic Medial Elbow Instability. Orthop
Clin N Am 2008; 39: 213-219
-
Nestor BJ, O'Driscoll SW, Morrey BF. Ligamentous
reconstruction for posterolateral instability of the elbow. J
Bone Joint Surg 1992:74A:1235-1241
-
Sanchez-Sotelo J, Morrey BF, O’Driscoll SW. Ligamentous
repair and reconstruction for posterolateral rotatory
instability of the elbow. J Bone Joint Surg Br 2005; 87-B:
54-61
-
Lee BPH, Teo LHY. Surgical reconstruction for posterolateral
rotatory instability of the elbow. J Shoulder Elbow Surg
2003; 12: 476-479
-
Gallo RA, Payatakes A, Sotereanos DG. Surgical options for
the arthritic elbow. J Hand Surg 2008; 33A: 746-759
-
BF Morrey, Adams RA. Semiconstrained arthroplasty for the
treatment of rheumatoid arthritis of the elbow. J Bone Joint
Surg Am 1992; 74: 479-490
-
Gill DRJ, Morrey BF. The Coonrad-Morrey total elbow
arthroplasty in patients who have rheumatoid arthritis. A ten
to fifteen year follow-up study. J Bone Joint Surg Am 1998;
80: 1327-1335
-
Little CP, Graham AJ, Karatzas G, et al. Outcomes of total
elbow arthroplasty for rheumatoic arthritis: comparative study
of three implants. J Bone Joint Surg Am 2005; 87: 2439-2448
-
Aldridge JM III, Lightdale NR, Mallon WJ, et al. Total elbow
arthroplasty with the Coonrad/Coonrad-Morrey prosthesis. A 10
to 31 year survival analysis. J Bone Joint Surg Br 2006; 88:
509-514.
|




