| ORIGINAL
ARTICLE |
|
The use of locking plates in
proximal humeral fractures: comparison of outcome by patient age
and fracture pattern |
|
Michael Leonard, Leibo Mokotedi, Uthman Alao,
Aaron Glynn, Mark Dolan, Pat Fleming.
Department of Trauma and Orthopaedic Surgery,Cork University
Hospital, Cork, Ireland
Address for Correspondence:
Michael
Leonard
Department of Trauma and Orthopaedic Surgery, Cork University
Hospital, Wilton, Cork, Ireland.
Phone: (00353)879163747
E-mail:
mikeleonard77@gmail.com
|
|
Abstract:
This study was undertaken to evaluate the efficacy of a proximal
humeral locking plate, and to specifically study the effect of
patient age and fracture type on outcome.
Thirty-one cases of proximal humeral fractures fixed using the
proximal humeral interlocking (PHILOS) plate were reviewed.
Average functional scores ( minimum 18 months post-op) per AO/ASIF
fracture type were 25.3 for type A, 21.4 for type B and 22.7 for
type C. There was no statistically significant difference
between groups. Functional score for patients over 65 years of
age were significantly inferior (p=0.03).
At final radiologic review (mean 12 months post-op) 30 (96%) of
the patients had united. Seven patients (22.5%) required a
second surgical procedure.
We obtained both good functional results and bone healing with
the PHILOS plate irrespective of fracture type, older patients
had a poorer outcome. We caution surgeons on the high potential
for re-operations with its use.
J.Orthopaedics 2009;6(3)e2
Keywords:
Proximal humeral fractures; Locking plates; PHILOS
Introduction:
Proximal humeral fractures are common, accounting for 5 to 9% of
all fractures 1. In patients over 65 years of age
they are the third most common fracture after fractures of the
hip and distal radius 2. Most proximal humeral
fractures are stable, minimally displaced and can be managed
conservatively 3.
The surgical treatment of displaced unstable fractures however
remains a challenge. Non-operative management of these more
severe fractures is associated with poor results 3.
The large range of operative techniques described (e.g., K
wiring, tension band wiring, plating, nailing, arthroplasty) for
managing the more complex fractures is a testament to the lack
of clear superiority of any one method. Most of these techniques
have been associated with complications related to hardware
failure, osteonecrosis, non-union, malunion, rotator cuff
impairment, and impingement 4.
Proximal humeral locking plates such as the proximal humeral
interlocking (PHILOS) plate (Synthes, Switzerland) offer several
potential advantages in the treatment of these injuries. They
are site specific, low profile plates. The plate is precontoured
for the proximal humerus and the insertion of locking screws
obviates the need of plate to bone compression, preserving the
bones blood supply. The insertion of multiple polyaxial locking
screws through the specific targeting device into the humeral
head fragment provides fixed-angle support in multiple planes
which should in theory maintain the reduction achieved 1,
while allowing for early mobilisation. However, in spite of all
the potential benefits significant levels of construct failure
and revision surgery with the use of proximal humeral locking
plates have been reported, particularly in patients over 65
years of age 5.
This study was undertaken to evaluate the use of the PHILOS
plate system for the treatment of proximal humeral fractures. We
specifically wanted to examine the effectiveness of the PHILOS
plate on different fracture patterns, the impact of patient age,
and of the humeral neck-shaft angle attained following fixation
on outcome.
Materials
and Methods:
From May 2003 to May 2007 31 patients with displaced fractures
of the proximal humerus had open reduction and internal fixation
with a PHILOS plate (Synthes, Switzerland). Patients were
identified from the trauma database of a single university based
level 1 trauma centre.
There were 23 women and 9 men with a mean age of 61.6 years (19
to 86). Twenty- five of the patients sustained their injury
following a fall, 5 from a road traffic accident and 1 from
direct assault.
Fractures were classified with the AO/ASIF system (8),
there were 8 type A (extra-articular unifocal), 15 type B
(extra-articular bifocal) and 8 type C (articular) fractures.
All fractures met the indications for operative treatment
outlined by Neer et al 7, i.e. an angulation of the
articular surface of more than 45 degrees or displacement
between the major fracture fragments of more than 1cm. It is
our policy to treat some fracture-dislocations (particularly in
the physiologically elderly), head-splitting fractures, and
impression fractures that involve over 40% of the articular
surface with a hemiarthroplasty.
Operative Technique:
All cases were performed by a senior orthopaedic surgeon.
Patients received prophylactic intravenous antibiotics. All
patients were placed in the beach-chair position and the C-arm
was positioned parallel to the patient at the head of the bed.
Satisfactory imaging was ensured before prepping the patient. A
delto-pectoral approach was used with minimal soft tissue
dissection. The biceps tendon was identified and retracted, and
the fracture exposed. On occasion the biceps tendon was found to
be interposed in the fracture fragments requiring mobilisation.
Traction sutures were then placed around the tendon-bone
interfaces of the rotator cuff and tuberosity fragments. The
head fragment, when involved, was then reduced from its typical
varus position through manipulation and flexing of the arm. Once
in position the traction sutures were used to bring the
fragments beneath the head to buttress the articular fragment.
The facture was then held temporarily with K wires and the
reduction checked fluoroscopically. The traction sutures were
then passed through the proximal eyelets on the plate without
any tension. The PHILOS plate was then applied lateral to the
bicipital groove, 1-2cm distal to the upper end of the greater
tuberosity. A conventional non-locking screw was then inserted
into the slotted gliding hole on the plate this both brings the
plate to the bone and allows for minor adjustments in plate
height and position when checked on fluoroscopy. The proximal
targeting device was then used to insert the polyaxial locking
screws into the head, locking screws were also inserted into the
shaft. In one patient with poor bone stock Allomatrix bone
substitute (Wright Medical, USA) was used. The traction sutures
were then tied down to the plate and final images taken.
The arm was placed in a sling after wound closure. Pendular
exercises only were permitted for the first 4 weeks
post-operatively, with elbow and wrist range of motion also
encouraged. Passive progressing to active range of motion was
then commenced under the guidance of a physiotherapist at 4-6
weeks post-op. Resistive strengthening was begun when fracture
union was ensured.
Using the immediate anteroposterior post-operative radiograph
the humeral neck-shaft angle was determined. The anatomic
neck-shaft angle of the humerus varies from 130 to 140 degrees.
Postoperative outcome was measured with the Quick Disabilities
of the Arm, Shoulder, and Hand Outcome Measure (QuickDASH) at a
minimum of 18 months postoperatively (range 18-60 months). The
QuickDASH is an eleven-item questionnaire that has been
validated for either proximal or distal disorders of the upper
limb 8.The total score ranges from 0 to 100 points,
with 100 indicating the most disability. Functional outcome
using DASH has been rated as excellent (<20 points), good (20-39
points), fair (40-60 points) or poor > 60 points.
Radiologic outcome measurements recorded at a mean of 12 months
(range, 10-15 months) post-operatively included bone-union,
defined as the continuity of cortex visible on at least two
radiographic views, avascular necrosis, loss of fixation and/or
hardware failure.
Statistical Analysis:
Statistical analyses were performed with SPSS 13 (SPSS, Chicago,
Illinois). Comparisons were made using Mann-Whitney U
tests. A P- value of less than 0.05 was considered to be
significant.
Results :
The mean operative time was 81 minutes (range, 60-123) and the
mean blood loss was 222 millilitres (range, 150-600). Two
patients developed superficial wound infections, both responded
to intravenous antibiotics. No neurovascular injuries occurred.
Average clinical follow-up period was 14 months (range, 12-18).
Twenty seven patients (87%) responded to the DASH questionnaire.
Post-operative Quick DASH scores ranged from 0 to 93.2 (mean =
22.7). The 4 patients who did not respond had undergone an
uneventful recovery, had united their fractures radiologically
and had been discharged from the clinic.
Average DASH scores per AO/ASIF fracture type were 25.3 for type
A, 21.4 for type B and 22.7 for type C. There was no
statistically significant difference between these groups.
The mean DASH score for patients under 65 years of age (n=14)
was 21.5, and 27.5 for patients over 65 years of age (n=13). The
difference was statistically significant (p=0.03).
There was a trend for patients with intra-operative restoration
of the humeral head-neck angle to greater than 90 degrees (n=15)
to have better outcome (mean DASH score = 20.4) than those who
were fixed with an angle of under 90 degrees (n=12, mean DASH
score 24.3). However this was not statistically significant.
At final radiologic review (mean 12 months post-op) 30 of the
patients had united clinically and radiologically (96%) (Figure
1 a + b). The mean time to union was 12 weeks (9 to 20).
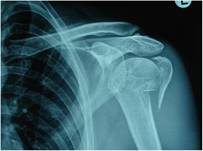
Figure 1 a:
Pre - operative anteroposterior radiograph of a 54 year old
female with a four-part fracture of her left proximal humerus.
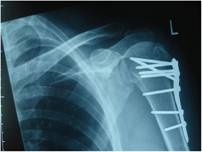
Figure 1 b:
Note the multiple angled screw fixation and solid bony union
evident on the post-operative radiograph at 8 months, with no
signs of avascular necrosis.
Seven patients (22.5%) required a second surgical procedure.
Three patients failed to unite after initial fixation, one a 19
year old female had autologous bone grafting alone performed
(Figure 2 a +b), the other two (both over 65 years of age)
underwent plate removal, bone grafting and intramedullary
nailing. Both the young female patient and one of the patients
over 65yrs of age went on to unite, the other patient did not
and subsequently had a hemiarthroplasty performed 7 months after
PHILOS plate fixation. Two patients required removal of the
plate which in both cases had been placed in an excessively
superior position causing symptomatic impingement. One patient
required removal of a prominent screw and one patient required a
manipulation under anaesthesia for a frozen shoulder following
fracture healing.
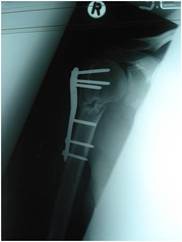
Figure 2 a:
A completely displaced proximal humeral fracture in a 19 year
old girl. The fracture was treated with a PHILOS plate but had
not united at 4 months post-operativley.
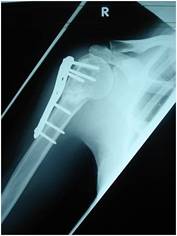
Figure 2 b:Autogenous
iliac crest cancellous graft was subsequently inserted and the
fracture united at 6 months post-operativley.
Avascular necrosis (AVN) was observed in 2 patients both of whom
had AO/ASIF type C fractures. In both cases only a small
percentage of the humeral head was involved, the fracture healed
and there was no perforation of the humeral head by any of the
screws.
Discussion :
Proximal humeral fractures are challenging to treat. Despite
being common injuries there are no clear-cut indications for any
of the various surgical options described 4. Defining
correct treatment guidelines through analysis of current
treatment options is becoming increasingly important as the
prevalence of osteoporotic fractures of the proximal humerus is
expected to rise in the next three decades and the functional
outcome achieved after treatment may determine a patients level
of independence 9.
The PHILOS plate was designed to improve screw fixation and
minimise soft tissue dissection. It attempts to achieve these
aims through a combination of multidirectional locking screws
for the head, precontouring of the plate and locking screws in
the shaft 10. The clinical results to date have been
mixed 1,5,10.
This study evaluated the clinical and radiological results of
the PHILOS plate used in 31 patients over a 4 year period in a
University based Level 1 trauma centre.
We found no significant difference in functional outcome using
DASH scoring after PHILOS plate fixation between fracture types
using the AO/ASIF classification system at a minimum of 18months
post-operatively. We could find only one other paper which
compared fracture type before PHILOS fixation with clinical
outcome. Bjorkenheim et al., in their study reported a reducing
trend in clinical outcome related to severity of fracture at a
minimum follow-up of 1 year, but they did not report any
statistical analysis of their results. However the 3 cases of
non-union and the 2 cases of AVN we report all occurred in the
more severe fracture types B and C.
The impact of age on outcome after PHILOS plate fixation is of
interest, particularly as there is a general belief that these
plates provide more secure fixation in osteoporotic bone 8.
We found a significantly inferior clinical outcome in patients
over 65 years of age. Fracture type distribution was similar
between the under and over 65s. Moonot et al., demonstrated no
significant difference in functional outcome between under and
over 65 year olds at a mean follow up of 11 months post PHILOS
plate fixation 10. We recorded 2 cases of non-union
and 1 case of AVN in the over 65 group. The inferior functional
outcome and complications in the elderly population is probably
multifactorial, combining both lower strength and reduced range
of motion, with a more tenous blood supply and healing capacity.
We encountered no mechanical failure of the plate and screws.
The use of local adjuvants, such as bone graft or bone graft
substitutes at the time of surgery, particularly when poor bone
stock is encountered, may well improve the rate of union and has
been advocated by others 3,10.
There was no statistically significant difference in clinical
outcome between those who had restoration of their humeral
head-neck angle to greater than 90 degrees at the time of
surgery and those that did not. As with all locking plates,
fracture reduction must be achieved prior to plate application,
this can be technically demanding. We achieved this in only 17
of our cases (54%). It has been shown that unstable proximal
humeral fractures have a tendency towards varus collapse even in
the presence of locking plate fixation. This can lead to varus
deformity with impingement and potential screw cut-out. While we
have not encountered this problem to date, we advocate optimal
restoration of the head-neck angle to guard against this
potential complication.
The fact that 7 (22.5%) of our patients required a second
procedure following PHILOS plate fixation is a cause of concern.
Three of these re-operations were as a result of technical
error. In one case a screw was left too long, and in the two
other cases the plate was placed in an excessively superior
position causing symptomatic impingement. The reported rate of
complications following PHILOS plate fixation is high, Owlesy et
al., reported a radiographic complication rate in 36% of their
patients, with a 43% rate of cut-out in patients over 60 years
of age 5. Moonot et al reported significant
complications in 21% of their cases 10. Of the 3
patients in this study who developed a symptomatic non-union 2
were over 65years of age and had sustained a complex fracture
type. A hemiarthroplasty in this situation is an option, the
possible benefits of which include; a single operation,
excellent pain relief, reasonably good function and no potential
for non-union or avascular necrosis 3. However the
results obtained in recent studies of hemiarthroplasties for
trauma have been mixed 11,12,13. Problems with
strength, function, range of motion, neurological deficits,
reoperations and displacement of both the prosthetic head and
tuberosities have all been reported 11,13.
Although the number of patients in our study was relatively
small and it was not a randomised controlled study the results
demonstrate both the potential benefits and problems with the
PHILOS plate. We obtained both good functional results and bone
healing in the vast majority of our patients. There was no
statistical difference in functional outcome between the
fracture types at a minimum of 18 months post-operatively.
Patients under 65 years of age had a significantly better
outcome. The PHILOS plate is a useful addition to the
armamentarium of the trauma surgeon, however we caution all
surgeons on the high potential for complications and
re-operations with its use.
Reference :
-
Badman BL, Mighell M. Fixed-angle locked plating of two-,
three-, and four-part proximal humerus fractures. J Am Acad
Orthop Surg 2008; 16:294-302
-
Baron JA, Barrett JA, Karagas MR. The epidemiology of
peripheral fractures. Bone 1996;18-3:209-213
-
Nho SJ, Brophy RH, Barker JU et al. Management of
proximal humeral fractures based on current literature. J
Bone Joint Surg Am 2007; 89-3:44-58
-
Robinson CM, Page RS, Hill RM et al. Primary
hemiarthroplasty for treatment of proximal humeral fractures.
J Bone Joint Surg Am 2003;85:1215-23
-
Owsley K, Gorczya JT. Displacement/Screw cutout after open
reduction and locked plate fixation of humeral fractures. J
Bone Joint Surg Am 2008;90:233-40
-
Muller ME, Nazarian S, Koch P et al. The comprehensive
classification of fractures of long bones. Springer Verlang
Berlin 1990
-
Neer CS. Displaced proximal humeral fractures. Part 1.
Classification and evaluation. J Bone Joint Surg Am
1970;52:1077-89
-
Beaton DE, Wright JG, Katz Jn. Development of the QuickDASH:
comparison of the three item-reduction approaches. J Bone
Joint Surg Am 2005;87:1038-46
-
Kannus P, Palvanen M, Niemi S et al. Increasing number
and incidence of osteoporotic fractures of the proximal
humerus in elderly people. BMJ 1996;313:1051-2
-
Moonot P, Ashwood N, Hamlet M. Early results for treatment of
three- and four-part fractures of the proximal humerus using
the PHILOS plate system. J Bone Joint Surg Br
2007;89-B:1206-9
-
Boileau P, Krishnan SG, Tinsi L et al. Tuberosity
malposition and migration: reasons for poor outcomes after
hemiarthroplasty for displaced fractures of the proximal
humerus. J Shoulder Elbow Surg 2002; 11:401-412
-
Christoforakis JJ, Kontakis GM, Katonis PG et al.
Shoulder hemiarthroplasty in the management of humeral head
fractures. Acta Orthop Belg 2004; 70:214-8
-
Phillips NJ, Ali A, Stanley D. Treatment of primary arthritis
of the elbow by ulnohumeral arthroplasty. J Bone Joint Surg
Br 2003;85-B:347-50
|
|
This is a peer reviewed paper Please cite as:
Michael
Leonard:
The use of locking plates in proximal humeral fractures:
comparison of outcome by patient age and fracture pattern.
J.Orthopaedics
2009;6(3)e2
URL:
http://www.jortho.org/2009/6/3/e2 |
|
|






