|
Abstract:
Failed
fixation of hip fractures typically leads to functional
disability and pain for the individual, technical challenges for
the surgical team, and an increase in the financial burden on
society. Between 1999 and 2005 41 patients (30 women and 11 men)
with a mean age of 70 were treated at our institution with a
total hip arthroplasty for failed dynamic hip screw fixation of
a hip fracture.
This study had three purposes: (1) to determine the reason/s for
failure of internal fixation (2) to record difficulties /
complications encountered in converting to a salvage
arthroplasty and (3) to compare the outcome of patients
who underwent salvage arthroplasty (Group 1) with a
matched group of patients who had a primary hip arthroplasty for
degenerative disease (Group 2).
Failure to achieve a good reduction and optimal screw placement
was evident in 80% of cases of failed fixation. A high incidence
of complications was recorded in the perioperative period during
conversion to a salvage arthroplasty. Functional outcome was
statistically inferior in Group1, this group also had a much
higher incidence of complications. Radiographs at 2 years post
operatively showed evidence of femoral stem loosening in 16% of
the salvage group compared with 3% in the primary hip
arthroplasty group.
Salvage hip arthroplasty is associated with higher complication
rate and poorer outcome than primary hip arthroplasty. We
recorded a high incidence of femoral stem loosening in
patients who had salvage hip arthroplasty, we recommend more
frequent clinical and radiographic follow up of these patients.
J.Orthopaedics 2009;6(1)e4
Keywords:
fracture calcaneum; intraarticular; extraarticular; surgery; outcome
Introduction:
The
incidence of hip fractures worldwide was 1.26 million in 1990
and is estimated to increase to 2.6 million in 2025 and 4.5
million in 20501. The current cost of treating these
injuries is estimated to be 10 billion dollars per year in the
United States alone2. Failed surgical treatment of
hip fractures typically leads to profound functional disability
and pain for the individual, technical challenges for the
surgical team, and an increase in the financial burden on
society.
Epidemiological studies have demonstrated that the anatomical
location of the ‘hip fracture’ is split evenly between the
neck of femur and the intertrochanteric region3.
In both types the fracture pattern, bone quality, accuracy
of reduction and adequacy of fixation are key factors
determining outcome4. There are important differences
however between these two sites ; a fracture of the femoral neck
may cause irreparable damage to the blood supply of the femoral
head leading
to avascular necrosis and femoral head collapse whereas an
intertrochanteric fracture is subject to significant
biomechanical loads which can lead to loss of reduction and/or
fixation failure.
Treatment options for failed internal fixation consist of
non-operative care for the very elderly or medically unfit
patient, revision internal fixation, or hip arthroplasty.
Revision internal fixation has the benefit of retaining the
native joint which may be beneficial in the physiologically
young patient. Frequently, however the patient has poor bone
quality, an unfavourable fracture pattern, damaged femoral head,
damaged articular cartilage and limb shortening. Due to these
issues arthroplasty, with excision of head-neck fragment is an
accepted salvage technique. The technical challenges of
performing a salvage arthroplasty in this situation include the
presence of failed internal fixation devices, difficulties with
dislocation,intra-operative fracture, bone deformity, cement
extravasation, leg length discrepancy, stress risers and poor
bone quality.
This study had three purposes: (1) to determine the reason/s for
failure of internal fixation
in a group of patients treated in our institute for
failed internal fixation of a proximal femoral fracture(2) to
review the conversion in these patients of failed fixation to
total hip arthroplasty and record any difficulties /
complications encountered, and (3) to compare the outcome of
patients who underwent primary hip arthroplasty for degenerative
arthritis with those patients in this study who underwent
conversion of failed fixation to arthroplasty.
Patients
and Methods:
Between
1999 and 2005 41 patients (30 women and 11 men) with a mean age
of 70 were treated at our institution with a total hip
arthroplasty after failed internal fixation of a hip fracture;
24 neck of femur, 17 intertrochanteric fractures. All were
initially fixed
with a dynamic hip screw (DHS) (AO Synthes, Switzerland)
construct and had undergone revision to arthroplasty for a
combination of reasons including pain, stiffness, and decreased
mobility coupled with radiographic evidence of a complication of
the initial fracture treatment.
Patients
were identified from our institutions computerised database.
The
radiographs and medical charts of all patients were obtained
following institutional approval.
Intracapsular
femoral neck fractures were classified according to the Garden
system5 and intertrochanteric fractures were
classified as stable or unstable as per Kyle et al6.
The
time lag from fracture to definitive reduction and fixation for
intracapsular fractures was recorded from the medical notes.
The
quality of the reduction of the fracture achieved was assessed
on the basis of displacement and alignment of the fracture. The
reduction was categorized as good, acceptable, or poor. For a
reduction to be considered good, there had to be normal or
slight valgus alignment on the anteroposterior (AP) radiograph,
less than 20 degrees’ angulation on the lateral radiograph,
and no more than 4mm of displacement of any fragment. To be
considered acceptable, a reduction had to meet the criterion of
a good reduction with respect to either alignment or
displacement or both. A poor reduction met neither criterion7.
The
technical quality of the radiographs available and the patient
positioning were too inconsistent
to allow for quantification of osteoporosis with the use
of the method of Singh et al.
The
tip-apex distance (TAD), the sum of the distance from the tip of
the lag screw to the apex of the femoral head as described by
Baumgaertner et al.was used to describe the position of the
screw in the femoral head. They demonstrated that a TAD of 25
millimeters (mm) or less resulted in no cut-outs, a TAD of 35
– 45mm resulted in a cut-out rate of 36% and a TAD of over
45mm a cut-out rate of 60%7.
The
time to revision was recorded as the length of time in months
between initial fracture fixation and salvage arthroplasty.
Each
patient who had undergone salvage arthroplasty (Group 1) was
matched with a patient who had undergone total hip arthroplasty
for degenerative disease in our unit (Group 2). Patients were
matched for age, sex, implant and time since insertion of the
implant. The vast
majority (>95%)of
patients in both groups had a cemented total hip
with either an Exeter or a Charnley stem in combination
with a polyethelene cemented cup. The patients in Group
2 were selected without any knowledge of their outcome to
eliminate selection bias.
All
surviving patients form both groups were followed up for a
minimum of two years (mean 5 years). Three main outcome measures
were compared between the two groups; surgical complications,
the Oxford hip score( interpreted as per Murray et al.
with a continuous score ranging from 0 (most severe symptoms) to
48 (least symptoms / best outcome))8, and radiographic analysis
of the femoral component for signs of loosening. Criteria of
loosening were defined (Table 1), and the standard 2 year
post-operative radiographs were compared with those obtained in
the early (1-3days) postoperative period.
Statistical
Methods
Statistical
analysis were performed with SPSS 13 (SPSS, Chicago, Illinois).
Between group comparisons were made using Mann-Whitney U
tests. A P- value of
less than 0.05 was considered to be significant.
|
Progressive
lucent zone at bone-cement interface >2mm
Subsidence
>5mm
Varus
displacement
Fracture
of the cement
Appearance
of a lucent zone between metal and cement/bone
|
| Table
1. Radiographic signs of loosening of the femoral stem |
Results:
Details
of the patients are summarised in Table 2. Mean follow up was 5
years (range 9 – 2.5 yrs).In the 11 unstable intertrochanteric
fractures, failure of fixation was due to a combination of both
inadequate reduction (acceptable reduction in 6, poor reduction
in 5) and screw placement (<35 in 8, <45 in 3). The
combination of these factors lead to a non-union in 5, cut-out
in 3 and implant breakage in 3 (Figure 1).
Of note all three cases of implant breakage were
associated with a short screw; tip-apex distance (TAD) <45
mm).
| Patients
Fracture
Reduction
TAD
Cause of failure Time
to revision |
| No. Age. Sex |
|
1 79
M
Intertroch. – stable
Acceptable
<35mm
Cut-out 16months
2 85
M
Intertroch – unstable
Acceptable
<35mm
Cut-out 2months
3 55
M
Intertroch – unstable
Poor
<35mm
Non-union 6 months
4 88
M
Neck of femur- G1
Good
<25mm
AVN 15months
5 76
F
Neck of femur- G2
Good
<45mm
Cut-out 14months
6 76
F
Intertroch - unstable
Acceptable
< 35mm Non –union
14months
7 73
F
Neck of femur – G1
Good
<45mm
Cut-out 36months
8 85
F
Neck of femur – G2
Good <25mm
AVN
36months
9 84
F
Neck of femur – G3
Good
<35mm
AVN
12months
10 65
F
Neck of femur – G2
Good
<25mm
AVN
10months
11 51
F
Neck of femur – G1
Good
< 35mm
AVN
18months
12 84
F
Intertroch – unstable
Acceptable
<45mm
Implant breakage13months
13 78
F
Intertroch – stable
Poor
< 35mm
Cut-out 29months
14 66
F
Intertroch – unstable
Acceptable
<45mm
Implant breakage37months
15 70
F
Intertroch – stable
Good
<45mm
Cut-out 10months
16 56
M
Neck of femur – G3
Acceptable
<25mm
AVN 31months
17 80
F
Intertroch – unstable
Poor
<35mm Cut-out 4months
18 75
F
Neck of femur – G2
Good
<45mm
Cut-out 1month
19 79
F
Neck of femur – G2
Good
<35mm
Cut-out 3months
20 70
F
Neck of femur – G2
Good
<25mm
AVN 38months
21 73
F
Neck of femur – G3
Acceptable
<35mm
Non-union 37months
22 54
M
Intertroch – unstable
Acceptable
<35mm
Non-union 19months
23 62
M
Neck of femur – G4
Acceptable
<25mm
AVN 18months
24 53
F
Neck of femur – G3
Acceptable
<35mm Non-union
12months
25 80
M
Neck of femur – G1
Good
<25mm
AVN 18months
26 58
F
Neck of femur – G3
Acceptable
< 35mm
AVN 9months
27 67
M
Neck of femur – G3
Good
< 25mm
AVN
18months
28 80
F
Neck of femur – G1
Good
<45mm
Cut-out 1month
29 80
F
Intertroch – unstable
Acceptable
<35mm
Non-union 11months
30 81
F
Intertroch – stable
Acceptable
<45mm
Cut-out 2months
31 84
F
Intertroch – unstable
Poor
<45mm
Implant breakage
21months
32 56
F
Neck of femur – G3
Acceptable
<35mm
AVN 16months
33 90
F
Neck of femur – G1
Good
<25mm
Cut-out 15months
34 70
F
Neck of femur – G1
Good
<35mm
AVN 12months
35 82
F
Intertroch – stable
Acceptable
<35mm
Cut-out 3months
36 89
F
Neck of femur – G1
Good
<25mm
AVN
5months
37 64
M
Neck of femur – G3
Acceptable
<35mm
Cut-out 1month
38 66
F
Intertroch – unstable
Poor
<35mm
Non-union
12months
39 68
M
Intertroch – stable
Acceptable
<35mm
Cut-out 16months
40 66
F
Intertroch – unstable
Poor
<35mm
Cut-out 16months
41
57
F
Neck of femur – G3
Acceptable <25mm
AVN
24months |
| Intertroch =
Intertrochanteric, G1
= Garden 1(incomplete valgus impacted intracapsular
fracture neck of femur), G2 = Garden 2 (complete fracture,
no displacement), G3 = Garden 3 (Complete fracture,
partial displacement), G4 = Garden 4 (complete
displacement) TAD
= Tip-Apex Distance, AVN = Avascular Necrosis |
Table
2. Summary of patients’data
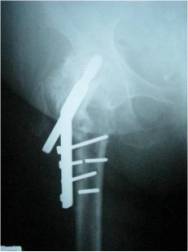 |
| Figure
1: Failed
fixation of an intertrochanteric fracture with implant
breakage |
In
the 6 stable intertrochanteric fractures , an acceptable
reduction was obtained in 4, with 1 good and 1 poor reduction.
However in no case was the ideal TAD achievied, 4 had a TAD of
<35 and 2 a TAD of <45, all failed due to cut-out of the
screw.
Of
the 14 intracapsular undisplaced (Garden 1 + 2) neck of femur
fractures all were classified as having a good reduction.
Failure occurred due to cut-out in 6 cases (Figure 2), 5 of
which had inadequate screw length ( TAD <45mm in 4 and
<35mm in 1). The remainder failed due to the development of
avascular necrosis (AVN).
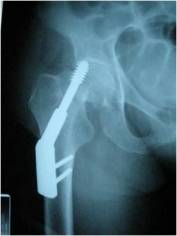 |
| Figure
2: Superior cut
out of screw in an intracapsular fracture |
In
the displaced neck of femur fractures (Garden 3+ 4) a good
reduction was obtained in 2 and an acceptable reduction in the
remaining 8. There were no open reductions. Screw placement was
also satisfactory in this group; TAD <25mm in 4 and <35mm
in 6. Failure occurred due to the development of AVN in 7,
non-union in 2 and cut-out in 1.
The
mean time from fracture to fixation for the patients who
developed AVN was 21.1 hours (hrs) compared to 16.2 hrs in the
non AVN group, however this was not significant (p =0.164).
The
mean time between fracture fixation and subsequent revision to
arthroplasty was 16 months (range 1 – 38 months).
On
review of the operative notes of the 41 cases, the mean surgical
time was 2 hours and 55 minutes. Mean blood loss was
923millilitres. Difficulty with dislocation was documented on 11
occasions, difficulty with removal of metal was documented on 10
occasions. Cement extrusion through previous screw holes was
noted on 11 post-operative radiographs. One patient had two
episodes of hip dislocation while still an in-patient, these
were treated successfully with closed reduction (Figure 3). Two
patients required re-operation, one for debridement of a sterile
wound haematoma, and another for rewiring of a trochanteric
nonunion. On one occasion only was the surgeon forced to change
the operative plan from a cemented to a uncemented long stemmed
implant with cables due to both a fractured greater trochanter
and difficulty with removal of the previous metal work.
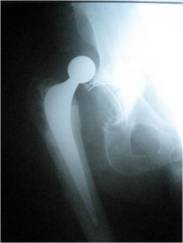 |
| Figure
3: Dislocated salvage total hip replacement 2 days
post-operativley |
Before
the follow-up date 10 of the 41 patients had died. All were over
80 years of age at the time of their death. Two died within 1
year of revision of their fixation. One patient died within 1
month due to a deterioration in her extensive medical
co-morbidities, although radiographs were satisfactory, she had
never ambulated post-operativley. Another patient died within 6
months of surgery, again from a combination of medical problems,
she had been progressing on a walking frame prior to his
deterioration. The remaining 8 patients died of illnesses
unrelated to their surgery at a later stage.
All
of the 41 patients who had undergone revision of their fixation
to total hip arthroplasty (Group1) were matched with a group who
had undergone primary hip arthroplasty for degenerative disease
(Group2) as described in the methods section. At the follow up
date 4 of the patients in Group 2 had died, none within 1 year
of their surgery. No deaths in this group were attributable to
their hip surgery.
Of
the remaining 31 patients in Group 1 we were unable to contact 7
leaving 24
patients available for follow up in Group 1. Of the remaining 37
patients in Group 2 we were unable to contact 4 patients and 4
did not wish to participate in the study, leaving 29 patients
for follow-up in Group 2.
All
of the patients in Group 1 were initially asked if conversion to
a total hip replacement had (a) provided pain relief and (b)
improved their ability to ambulate; 23 out of the 24 patients
felt that the surgery had been successfully in achieving these
aims.
Details
of the follow-up of patients in Group1 and 2 are summarised in
Table 3. The overall incidence of complications was much higher
in Group 1 (16) compared with Group 2 (5). The mean oxford hip
score for Group 1 was 30 compared with 43 for Group 2.
Comparative analysis showed this to be significant
(p=0.03).
|
Group Group2 |
|
No.
of Patients
24
29
Median Age
75
76
M:F ratio
7:17
10:19
Surgical
Complications
Haematoma
3
1
Superficial Infection
6
2
Dislocation
3
0
DVT
2
2
Re-operation for any
2
0
cause
Mean
Oxford hip score
at mean follow up of 5 years
30
43 |
Table 3. Surgical Complications and Oxford Hip Score (OHS) in
the two groups
A
2year postoperative radiograph was available for comparison with
the early postoperative radiograph in 31 of the patients in
Group1 and 33 of the patients in Group 2. As defined by the
criteria in Table 1 there was evidence of loosening of the
femoral stem in 16% (5/31) of the patients in Group 1; 3 with
progressive lucent zones at the cement bone interface, and 2
with varus displacement and subsidence. Only 1 patient in Group
2 showed evidence of loosening with a progressive lucent zone at
the cement bone interface.
Discussion:
A number
of factors may impact negatively on the outcome of internal
fixation of hip fractures. The two factors which are under the
surgeons direct control however are; the quality of the
reduction, and the accuracy of insertion of the fixation device.
Of
the 17 cases of failed fixation of intertrochanteric fractures
treated in this study none had the ideal combination of good
reduction and optimal location of the screw in the femoral head.
Union rates of up to 100% have been reported in well-reduced,
intertrochanteric
fractures treated with ideal implant placement9, however
failure rates of up to 56% have also been reported when this
optimal situation is not achievied4. This problem has led to the
design of several types of fixation devices including
intramedullary devices, however none have shown a clear clinical
advantage over the dynamic hip screw (DHS), which has a definite
cost-benefit advantage. To date no single implant is universally
accepted for the treatment of these fractures.
The
optimal surgical treatment of intracapsular femoral neck
fractures in adults and eldery patients remains controversial.
The two options are prosthetic replacement or internal fixation.
Proponents of prosthetic replacement argue that replacement of
the femoral head eliminates the necessity for revision surgery
due to avascular necrosis (AVN) and non-union10.
Those in favour of internal fixation report decreased operative
time, blood loss, and mortality rates11. Of the 24
femoral neck fractures in this study failure due to screw
cut-out with a suboptimal placement occurred in 6 patients.
Failure due to AVN occurred in 15 cases in spite of all having
had a satisfactory reduction and fixation. The literature would
suggest that the development of AVN in such cases is primarily
due to the degree of initial displacement, and the length of
time between fracture and fixation10, 11.
When
converting failed internal fixation of a hip to an arthroplasty,
a number of technical challenges must be overcome. Difficulties
with dislocation and intraoperative fracture have been reported12.The
internal fixation device which has failed, often has broken
screws which must be removed, also the ununited head-and neck
fragment or fragments are usually in a deformed position and
must be mobilised before being excised. This requires additional
dissection placing nearby neurovascular structures and muscles
at risk and leading to increased blood loss12.
It
has been suggested that the results of salvage total hip
arthroplasty following failed internal fixation
are comparable with those of primary joint replacement12,13.
The patients in our study who required a salvage arthroplasty
had a greater prevalence of complications and poorer functional
results than did patients who underwent primary hip arthroplasty
despite the use of similar techniques and implants. The reasons
for these differences are probably multifactorial. Patients with
failed internal fixation often have a prolonged period of hip
pain and immobility leading to muscle wasting and disuse
osteoporosis prior to revision surgery. The increased technical
challenges described earlier, prolonged operating time,
increased exposure, altered anatomy and greater blood loss all
are likely to play a role in poorer outcome. However conversion
to hip arthroplasty alleviated pain and improved function in the
vast majority of these patients, which is the hallmark of an
effective salvage procedure.
All
cases in this study were performed by experienced hip surgeons
using modern techniques and implants, in spite of this however
we still recorded radiographic evidence of femoral stem loosing
at 2 years in
16% of the patients who had undergone conversion to arthroplasty.
It has been suggested that cortical holes left by previous
screws may lead to cement extravasation with suboptimal
pressurisation, and poor remodelling of the cortical bone,
leading to an inferior cement mantle and potential stress risers
at areas of cement extrusion14. Is it intuitive that
every effort should be made to obtain the best mantle possible
but we would also recommend that these patients be followed up
for longer periods with more frequent radiographs than the
standard hip replacement patient.
In
summary when undertaking surgical stabilisation any hip fracture
one should make every effort to achieve the best reduction and
most accurate fixation possible, failure to achieve these goals
was evident in 80% (33/41) of our cases. Factors such as
osteoporosis, compliance with post-operative mobilisation and
delay in fracture fixation are to some extent ‘out of the
surgeons hands’. Conversion to arthroplasty is technically
challenging, and is associated with higher complication rate and
poorer outcome than primary hip arthroplasty. We recorded a high
incidence of femoral stem loosening in patients who had
undergone conversion to hip arthroplasty for failed fixation, as
a result we recommend more frequent clinical and radiographic
follow up of these patients.
Reference :
-
Lorich
DG, Geller DS, Nielson JH Osteoporotic Pertrochanteric Hip
Fractures: Management and Current Controversies. J Bone
Joint Surg Am 2004; 86 2:398-410
-
Sattin
RW Falls among older persons: a public health perspective.
Annu Rev Public Health 1992;13:489-508
-
Apple
DF, Hayes WC. Prevention of falls and hip fractures in the
elderly. Rosemont, IL: American Academy of Orthopaedic
Surgeons 1993
-
Haidukewych
GJ, Israel TA, Berry DJ
Reverse obliquity fractures of the intertrochanteric
region of the femur. J Bone Joint Surg Am 2001; 83:643-50
-
Garden
RS Low-angle
fixation in fractures of the femoral neck.J Bone Joint Surg
Br 1961;43-B:647-63
-
Kyle
RF, Gustilo RB, Premer RF Analysis of six hundred and
twenty-two intertrochanteric hip fractures. A retrospective
and prospective study. J Bone Joint Surg Am 1979;61:216-221
-
Baumgaertner
MR, Curtin SL, Lindskog DM
The value of the tip-apex distance in predicting
failure of fixation of peritrochanteric fractures of the
hip. J Bone Joint Surg Am 1995; 77:1058-1064
-
Murray
DW, Fitzpatrick R, Rogers K.
The use of the Oxford hip and knee scores. J Bone
Joint Surg Br 2007;8:1010-14
-
Baumgaertner
MR, Solberg BD
Awareness of the tip-apex distance reduces failure of
fixation of trochanteric fractures of the hip. J Bone Joint
Surg Br 1997;79:969-71
-
Chua
D, Jagial SB, Schatzker J.
An orthopaedic surgeon survey on the treatment of
displaced femoral neck fracture: opposing views. Can J Surg
1997;40:271-7
-
Parker
MJ, Pryor GA. Internal fixation or arthroplasty for
displaced cervical hip fractures in the elderly: a
randomised controlled trial of 208 patients. Acta Orthop
Scand 2000;71:440-6
-
Tabsh
I, Waddell JP, Morton J. Total hip arthroplasty following
failed internal fixation of hip fractures. Clin Orthop
1997;11:166
-
Mehlhoff
T, Landon GC, Tullos HS. Total hip arthroplasty following
failed internal fixation of hip fractures. Clin Orthop
1991;269:32-7
-
Patterson
BM, Salvati E, Huo MH.
Total hip arthroplasty for complications of
intertrochanteric fracture. J Bone Joint Surg Am 1990;72:
776-77
|





