|
Abstract:
J.Orthopaedics 2008;5(4)e12
Keywords:
Lateral release; Female TKA; Modified femoral design.
Introduction:
The history of total knee arthroplasty (TKA)
is one of constant innovation with progress towards components
that more closely reproduce normal human knee dimensions and
kinematics. Early components began with one, or few sizes. As
the success rate and application of the procedure grew, multiple
sizes were introduced to address the range of knees undergoing
surgery [1].
Femoral components were initially designed to
be non-side specific. High rates of patellar complications,
patellar clunk, and lateral release occurred. Further research
resulted in side specific components with attention to the
patellofemoral anatomy. This resulted in a decrease in failures,
and an almost complete elimination of patellar clunk problems
[8, 14]. Modified surgical techniques and prosthesis design,
particularly with respect to component rotation and position
[23, 25], have resulted in improved patellar tracking, reduced
need for lateral release, and decreased patellofemoral specific
modes of failure.
Despite these changes, rates of lateral
release continue to run as high as to 56.9 percent in combined
studies of male and female patients [20], though in most series
values range from 3-30 percent [2, 17-20, 26].
This procedure is not without risk, as previous authors have
noted increased rates of avascular necrosis (AVN) and patella
related failures following release [4]. In contrast, failure to
address patellar tracking appropriately can result in increased
rates of patellar and extensor mechanism complications [5, 6].
Modified trochlear dimensions and sizing
options are a natural next step in femoral component design, as
it has long been known that gender differences exist in native
knee geometry and biomechanics [7, 12, 15, 16, 23, 27]. Clinical
outcomes in females have also been inferior to those seen in men
in some studies [3, 13]. This study was designed to look at the
impact of this introduction on two related aspects of the
surgical procedure: the rate of lateral patellar release needed
for neutral patellar tracking and the size of the femoral
component used.
Material and Methods :
Standard
The senior author performed 79 consecutive
primary TKAs using the Zimmer LPS flex system (Zimmer Inc.,
Warsaw, IN) in 51 females (14 bilateral) between September 2003
and June 2004. The average age was 64.9 years (range 45-84) and
there were 46 left, and 33 right knees. BMI averaged 30.9 with a
range from 18.6 to 53.3.
Modified
The senior author performed 80 consecutive
primary TKAs using a modified design (Zimmer LPS flex gender
Zimmer Inc., Warsaw, IN) in 69 females (9 simultaneous
bilateral, 2 staged bilateral) between May 2006 and April 2007.
The average age was 66.7 years (47-89) and there were 41 left
and 39 right knees. BMI averaged 31.1 with a range from 19.5 to
52.1.
Statistical
analysis
Chi-squared test was used, with a p value
0.05 to determine significance.
Technique
The senior author performed all TKAs. In all
cases an incision only long enough to safely and accurately
insert the components was used, and has previously been
described at length [10, 11]. Femurs were placed using
posterior rotational referencing, and tibial components using
the medial 1/3 of the tubercle and crest of the tibia.
With respect to the patella, a mini-medial
parapatellar arthrotomy was performed in all cases. The patella
was laterally subluxed, but not everted. The patellar
preparation was performed following the femoral and tibial cuts,
to allow more space for application of the patellar clamp.
Patellar reaming was then performed to an appropriate depth to
recreate the pre-patellar height with the addition of the
button. Onlay circular patellar component size was chosen to
provide maximum coverage without overhang. Following
application of the button, any lateral bone, and osteophyte were
bevelled using a saw.
Trial components were then inserted and the
patellar tracking was observed using a no thumbs technique
[24]. The tourniquet was not released for this step. If lateral
tracking was observed a towel clip was used to provide
longitudinal tension to the extensor mechanism [10, 11], and
tracking was reassessed as the no thumbs technique has been
shown to over represent the need for lateral release [2]. In
cases where lateral tracking or tilt persisted, a lateral
release was performed. A soft tissue sleeve of a minimum 1
centimetre was left lateral to the patella, and the
superolateral vascular structures were identified and
preserved. In all cases, a lateral release provided central
tracking. After cementing all components, a trial tibial insert
was placed, and patellar tracking was once again assessed.
Results :
Standard Femoral Component
Standing anteroposterior x-rays were used in
all cases for measurements of alignment. Pre-operative tibio-femoral
alignment was a mean 0.5 degrees of varus (range 25 degrees of
valgus to 14 degrees of varus). There were 5 patients with 15 or
more degrees of valgus and 5 with 10 or more degrees of varus.
Post-operative tibio-femoral alignment averaged 4.1 degrees of
valgus (range 1 to 8 degrees of valgus).
The average pre-cut patellar thickness was
22.0 mm and the average post-cut thickness, following
cementation of the button, was 21.6 mm. In no cases was the
difference greater than two millimetres for this measured value.
In two cases (bilateral same patient) a patelloplasty was
performed and the patella was not resurfaced due a very thin 15
mm preoperative thickness. In one other case a 24mm patella was
left unresurfaced at the surgeons discretion in a young,
non-obese patient with central tracking and minimal patellar
chondral changes. None of the unresurfaced patellae required a
lateral release.
Table 1: Lateral
release rate with standard femoral components in women
Femoral component size
|
C |
D |
E |
F |
Totals |
|
no lateral release |
2 |
23 |
33 |
8 |
66 |
|
lateral release |
1 |
1 |
5 |
6 |
13 |
|
Totals |
3 |
24 |
38 |
14 |
79 |
Table 2:
Lateral release rate with modified femoral components in women
Femoral component size
|
C |
D |
E |
F |
Totals |
|
no lateral release |
0 |
23 |
35 |
19 |
77 |
|
lateral release |
0 |
0 |
2 |
1 |
3 |
|
totals |
0 |
23 |
37 |
20 |
80 |
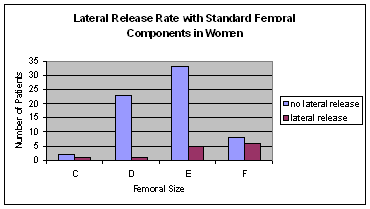
Figure 1: Cases of lateral release and
corresponding femoral size with the standard femoral component
In 13 (16.5 percent) cases a lateral release
was required for central tracking of the patella (Table 1). The
pre-operative alignment in these cases averaged 4.5 degrees of
tibio-femoral valgus with 2 cases in 15 or more degrees of
valgus. The rate of lateral release was higher in larger femoral
components (Figure 1). In cases where an F (the largest size
implanted) femoral component was used, six of fourteen knees
required a lateral release.
There was one complication in the lateral
release group during the post-operative course. A postoperative
lateral dislocation occurred in one case following a
hyperflexion injury which resulted in a dehiscence of the medial
arthrotomy. This necessitated repeat surgery at three months and
again at 19 months post-operatively. Ongoing problems with
patellar tracking have occurred, and a revision was performed.
The patient is doing well with no recurrent patellar problems at
early follow-up.
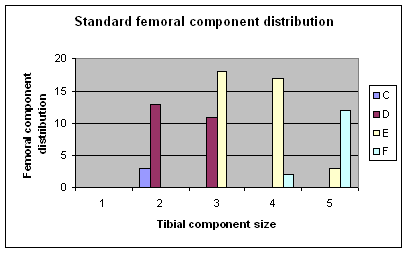
Figure 2: Standard femoral component
sizes used
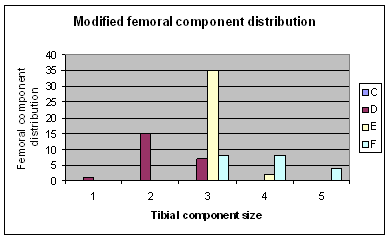
Figure 3: Modified femoral component
sizes used
Modified Femoral Component
Pre-operative standing tibio-femoral
alignment was a mean 0.6 degrees of valgus (range 25 degrees of
valgus to 18 degrees of varus). There were 11 patients with 15
or more degrees of valgus and 16 patients with 10 or more
degrees of varus. Post-operative tibio-femoral alignment
averaged 5.6 degrees of valgus (range 3 to 9 degrees of valgus).
Alignment values were not statistically significantly different
from the standard to the modified group.
The patella was resurfaced in all cases in
this group. The average pre-cut patellar thickness was 22.1 mm
and the average post-cut thickness, following cementation of the
button, was 22.3 mm. In no cases was the difference greater than
two millimetres for this measured value.
In three cases (4.3%) a lateral patellar
release was required for central patellar tracking (Table 2).
Two of these were in one patient undergoing bilateral TKAs with
preoperative anatomic alignments of 10 and 15 degrees of valgus.
The only other case requiring a lateral release was in a patient
with 18 degrees of valgus. Femoral components (requiring lateral
release) used included two E and one F component.
Lateral Release Rate
In the 79 standard cases 13 (16.5%) required
a lateral patellar release, versus 3 (4.3%) of modified femoral
component cases. This difference was statistically significant
(p< 0.01).
Component Sizing
Femoral component size, when plotted versus
tibial component size, shows a trend towards the use of larger
femoral components with the modified design, than with the
standard femoral component (Figures 2 and 3). This trend was not
statistically significant.
Discussion :
Introduction of a modified femoral design was
associated with a statistically significant reduction in the
rate of lateral patellar release. There was a trend towards
using larger femoral components with the modified design when
standardized for corresponding tibial component used. The
theoretical basis for design modifications in femoral components
has been reviewed at length [9, 15], but this is the first study
that we are aware of, that demonstrates a benefit to introducing
a modified femoral design in females.
The advantage to avoiding lateral patellar
release is well known. Complications involve increased rates of
AVN and patella related failures following release [4]. In
contrast, failure to address patellar tracking appropriately can
result in increased rates of patellar and extensor mechanism
complications [5, 6].
There are three alterations that have been
made in this new femoral design, all of which better approximate
native female anatomy: the thickness of the anterior flange of
the femoral component is reduced; the angle of the trochlear
groove is increased by ten degrees, to better approximate the
higher Q-angle in females; the M-L to A-P aspect ratios are
reduced, thus decreasing overhang, allowing a more lateralized
position for the femoral component, and maintaining posterior
condylar offset. These modifications are consistent with
anatomic gender differences [9, 15], and would also be presumed
to decrease the lateral release rate based on a large outcome
study by Pierson et al. showing that the odds ratio for lateral
release increased 2.2 times for every centimetre increase in
anterior femoral offset [22].
It is interesting to note that the need for a
narrower femoral component is not a new concept. The
Insall-Burnstein component had a special mid-size with a reduced
ML to AP size ratio. Poilvache et al. in their 1996 study on
measured bone parameters about knees at the time of TKA
concluded that some narrow femora
could require narrower implants to avoid medial-lateral overhang
of the femoral component [23]. Other investigators have made
similar observations with respect to ML to AP ratios in women
versus men [6, 15], indicating the possible benefit to modified
femoral designs.
The rate of lateral patellar release was
higher when a larger femoral component was used, particularly
with the standard design (Table 1 and Figure 1). This is
consistent with previously published anthropometric
measurements, which showed that the discrepancy in aspect ratio
between the native female anatomy and standard component sizes
increased as femoral component size increased [15]. It is also
consistent with a recently published large study of lateral
release rates in total knee arthroplasty [22]. Overhang of
larger components leads to stretching of the lateral tissues,
likely leading to the higher rate of lateral patellar tracking
and need for lateral release. If a smaller size is chosen to
decrease overhang, a flexion extension mismatch is created.
Though the trend towards more lateral releases with larger
components also existed with the modified femoral component, it
was not nearly as strong (Table 2).
A second important benefit to a modified
design is a more balanced flexion-extension gap. The ability to
insert a larger femoral size decreases the risk of flexion
instability as posterior condylar offset is maintained, and
provides a more balanced tibio-femoral articulation. Clinical
follow-up will be important to assess whether this results in a
decrease in mid flexion, and flexion instability in this group.
Conclusion:
This study demonstrates a statistically
significant decrease in the rate of lateral patellar release
with the use of a modified femoral component in females. Despite
this decrease, a small number of cases continued to require a
lateral release, particularly in cases with significant
pre-operative tibio-femoral valgus combined with a larger
femoral component. A trend toward the use of larger modified
femoral component sizes, when standardising for tibial size was
also observed. Further follow-up studies will be important in
determining the significance of these operative changes on the
long-term outcome of this new prosthetic design.
Reference :
1. Allardyce TJ, Scuderi GR, Insall JN. The Insall Burstein
Posterior Stabilized Condylar Knee Prosthesis. In: Scuderi GR
and Tria AJ Jr., ed: Surgical Techniques in Total Knee
Arthroplasty. New York: Springer-Verlag, 67-74, 2002.
2. Archibeck MJ, Camarata D, Trauger J, Allman J, White Jr RE.
Indications for lateral retinacular release in total knee
replacement. Clin Orthop Relat Res. 2003 Sep;(414):157-61.
3. Baker PN, van der Meulen JH, Lewsey J, Gregg PJ; National
Joint Registry for England and Wales. The role of pain and
function in determining patient satisfaction after total knee
replacement. Data from the National Joint Registry for England
and Wales. J Bone Joint Surg Br. 2007 Jul;89(7):893-900.
4. Berend ME, Ritter MA, Keating EM, Faris PM, Crites BM. The
failure of all-polyethylene patellar components in total knee
replacement. Clin Orthop Relat Res. 2001 Jul;(388):105-11.
5. Berger RA, Crossett LS, Jacobs JJ, Rubash HE. Malrotation
causing patellofemoral complications after total knee
arthroplasty. Clin Orthop Relat Res. 1998 Nov;(356):144-53.
6. Chin KR, Bae DS, Lonner JH, Scott RD. Revision surgery for
patellar dislocation after primary total knee arthroplasty. J
Arthroplasty. 2004 Dec;19(8):956-61.
7. Chin KR, Dalury DF, Zurakowski D, Scott RD. Intraoperative
measurements of male and female distal femurs during primary
total knee arthroplasty. J Knee Surg. 2002 Fall;15(4):213-7.
8. Clarke HD, Fuchs R, Scuderi GR, Mills EL, Scott WN, Insall JN.
The influence of femoral component design in the elimination of
patellar clunk in posterior-stabilized total knee arthroplasty.
J Arthroplasty. 2006 Feb;21(2):167-71.
9. Conley S, Rosenberg A, Crowninshield R. The female knee:
anatomic variations. J Am Acad Orthop Surg. 2007;15 Suppl
1:S31-6.
10. Cook JL, Cushner FD, Scuderi GR. Minimal-incision total knee
arthroplasty. J Knee Surg. 2006 Jan;19(1):46-51.
11. Cook JL, Scuderi GR, Tenholder M. Incidence of lateral
release in total knee arthroplasty in standard and mini-incision
approaches. Clin Orthop Relat Res. 2006 Nov;452:123-6.
12. Csintalan RP, Schulz MM, Woo J, McMahon PJ, Lee TQ. Gender
differences in patellofemoral joint biomechanics. Clin Orthop
Relat Res. 2002 Sep;(402):260-9.
13. Fisher DA, Dierckman B, Watts MR, Davis K. Looks good but
feels bad: factors that contribute to poor results after total
knee arthroplasty. J Arthroplasty. 2007 Sep;22(6 Suppl 2):39-42.
14. Fuchs R, Mills EL, Clarke HD, Scuderi GR, Scott WN, Insall
JN. A third-generation, posterior-stabilized knee prosthesis:
early results after follow-up of 2 to 6 years. J Arthroplasty.
2006 Sep;21(6):821-5.
15. Hitt K, Shurman JR 2nd, Greene K, McCarthy J, Moskal J,
Hoeman T, Mont MA. Anthropometric measurements of the human
knee: correlation to the sizing of current knee arthroplasty
systems. J Bone Joint Surg Am. 2003;85-A Suppl 4:115-22.
16. Hsu RW, Himeno S, Coventry MB, Chao EY. Normal axial
alignment of the lower extremity and load-bearing distribution
at the knee. Clin Orthop Relat Res. 1990 Jun;(255):215-27.
17. Husted H, Toftgaard Jensen T. Influence of the pneumatic
tourniquet on patella tracking in total knee arthroplasty: a
prospective randomized study in 100 patients. J Arthroplasty.
2005 Sep;20(6):694-7.
18. Lachiewicz PF, Soileau ES. Patella maltracking in
posterior-stabilized total knee arthroplasty. Clin Orthop Relat
Res. 2006 Nov;452:155-8.
19. Laskin RS. Lateral release rates after total knee
arthroplasty. Clin Orthop Relat Res. 2001 Nov;(392):88-93.
20. Lee GC, Cushner FD, Scuderi GR, Insall JN. Optimizing
patellofemoral tracking during total knee arthroplasty. J Knee
Surg. 2004 Jul;17(3):144-9
21. Newbern DG, Faris PM, Ritter MA, Keating EM, Meding JB,
Berend ME. A clinical comparison of patellar tracking using the
transepicondylar axis and the posterior condylar axis. J
Arthroplasty. 2006 Dec;21(8):1141-6.
22. Pierson JL, Ritter MA, Keating EM, Faris PM, Meding JB,
Berend ME, Davis KE. The effect of stuffing the patellofemoral
compartment on the outcome of total knee arthroplasty. J Bone
Joint Surg Am. 2007 Oct;89(10):2195-203.
23. Poilvache PL, Insall JN, Scuderi GR, Font-Rodriguez DE.
Rotational landmarks and sizing of the distal femur in total
knee arthroplasty. Clin Orthop Relat Res. 1996 Oct;(331):35-46.
24. Scott RD. Prosthetic replacement of the patellofemoral
joint. Orthop Clin North Am. 1979 Jan;10(1):129-37.
25. Scuderi GR, Insall JN. Rotational positioning of the femoral
component in total knee arthroplasty. Am J Knee Surg. 2000
Summer;13(3):159-61.
26. Sodha S, Kim J, McGuire KJ, Lonner JH, Lotke PA. Lateral
retinacular release as a function of femoral component rotation
in total knee arthroplasty. J Arthroplasty. 2004
Jun;19(4):459-63.
27. Woodland LH, Francis RS. Parameters and comparisons of the
quadriceps angle of college-aged men and women in the supine and
standing positions. Am J Sports Med. 1992 Mar-Apr;20(2):208-11.
|





