|
Abstract:
Purpose: To
review clinical and radiological outcome of distal femoral
fractures treated with the Less Invasive Stabilisation System (LISS).
Methods:
Retrospective observational study of all distal femoral
fractures treated with LISS between 2003 and 2007 in three
trauma centres.
Results: A
total of 40 patients were identified. Amongst these, 3 patients
were lost to follow up or died and 37 patients (24 females and
13 males) were included in final analysis. There were 23 acute
femoral fractures and 14 periprosthetic fractures. The commonest
cause of injury was simple mechanical fall. According to the AO
classification, 15 patients with type 33A, 4 patients with type
33C, 13 patients with type 32A and 2 patients with type 32B
and 3 patients with type 32C . Overall, the mean age was 67+/-
23.62 (Mean+/-SD) years. Follow up period was 12+/-6.92 (Mean+/-SD)
months. At the time of follow-up, fractures in 25 patients had
united and the remaining patients were proceeding to union.
Average time to union was 4.0+/-1.48(Mean+/- SD) months. One
patient died 13 months after fixation of fracture. Twenty seven
patients had closed reduction.
Conclusion:
LISS technique can achieve 100% union rate in both acute distal
femoral and periprosthetic fractures. Most fractures proceed to
union without the need for primary bone grafting and there were
no deep infections, thromboembolic events, persistent pain or
malunion. However, the procedure requires careful planning and
experience in the operative technique.
J.Orthopaedics 2008;5(4)e10
Keywords:
Less invasive stabilisation system plates;
distal femur; fractures; periprosthetic fractures.
Introduction:
Fractures of the distal femur are complex
injuries that account for 7% of all femoral fractures [1] and
their surgical treatment has always remained a challenge for the
orthopaedic surgeon. [2]
The goals of surgical treatment are to
restore anatomical congruity and achieve a stable fracture
fixation that will allow early mobilisation.
The results with surgical treatment are now
favourable consequent to the advances in implant technology and
surgical techniques seen in the last 40 years. From 1990
onwards, the decade saw the evolution of minimally invasive
surgical techniques in the fixation of distal femoral fracture.
Studies were undertaken to develop a system
that can combine the principles of a fixed angle construct
(biological plating techniques) that provides angular stability
and the soft tissue preservation that can be achieved with
intramedullary nailing devices. [3] The end result of these
studies was the less invasive stabilisation system (LISS). The
LISS has been shown to provide a stable fracture fixation with
soft tissue preservation and has now gained popularity in
treatment of distal femoral fractures and in fractures around an
implant (periprosthetic fractures).
However, owing to the recent evolution of
this system, there are very few clinical studies undertaken in
UK, so far, which have published the outcome with the LISS
technique.
We therefore undertook a multi centre
retrospective study to assess the outcome with LISS technique in
treatment of distal femoral fractures in three trauma units.
In this paper, we present our results with
respect to the clinical and radiological outcome achieved and
discuss our experience with LISS technique.
Material and Methods :
A retrospective review of all
patients who underwent surgical fixation with the LISS technique
for distal femoral fractures in three trauma units in North East
England (2 district general hospitals and 1 tertiary referral
centre) was undertaken between 2004 and 2007.
A total of 40 cases of distal femoral
fractures underwent LISS procedure during the period of review.
Two patients were lost to follow up and another died at 3 months
due to causes unrelated to surgery and these 3 patients were
excluded from our study.
Therefore, only 37 patients were included in
the final analysis and a review of case notes and radiographs of
these patients were undertaken by the authors.
We noted the patient demographics with
relation to age and gender. Details about the mechanism of
initial injury, type of fracture (open or closed) and presence
of periprosthetic fracture was recorded. Initial plain
radiographs were reviewed and all fractures were classified
according to the AO system.
Intra-operative information about surgical
technique with regards fracture reduction, intra-operative
complications and post operative mobilisation instructions were
obtained from the operative notes.
Clinical and radiological outcome with regard
to bony union, post-operative complications and incidence of
post-operative infection was assessed from the follow up
outpatient clinic notes and radiographs. Simple statistics were
used where possible.
Results :
Between 2003 and 2007, forty patients
underwent LISS plate fixation for treatment of distal femoral
fractures. The case notes and radiographs of 37 patients were
available for final analysis.
There were 23 cases of distal intra and extra
articular acute femoral shaft fractures (AO/OTA Type 32 and 33)
treated with LISS during the period of review.
There were 14 cases of periprosthetic
fractures and the results are discussed separately.
Acute Femoral shaft fractures:
The mean age at time of operation was 62.74
+/- 26.90 years (mean +/- SD). Range (18 102 years).
The commonest mechanism of injury was simple
mechanical fall (n= 13) and other cause of injury was a road
traffic accident [RTA] (n= 10). There were two cases of
compound fracture. According to the AO classification, 11
patients with type 33A, 4 patients with type 33C, 6 patients
with type 32A and 1 patient each with type 32B and 32 C
respectively. (Table 1) There were 2 cases of compound fracture.
|
Fracture Type |
n |
|
32A |
06 |
|
32B |
01 |
|
32C |
01 |
|
33A |
11 |
|
33C |
04 |
TABLE 1. AO/OTA Fracture
classification in acute femoral fractures
Early post operative mobilisation was
encouraged in all patients. Post operative weight bearing status
depended on practice of the operating surgeon. In 11 cases,
patients were initially mobilised non weight bearing for 6 weeks
and in the other 12 cases, patients were allowed to partially
weight bear for 6 weeks immediately after the operation. The
average follow up of patients was 11.77 +/- 8.72 months (mean
+/- SD). All patients were being followed up until bony union
was evident on plain radiographs. At the time of follow-up,
plain radiographs showed that the fractures in 20 patients had
united and the remaining three patients were proceeding to union
with evidence of good callus formation. The average time to
union was 4.0 +/- 1.33 months (mean+/- SD).
Complications: Indirect fracture reduction
with closed technique was achieved in 15 patients but in 6
patients, direct open reduction was necessary to achieve
adequate reduction of fracture (28.5%). Post operative early
failure of fixation was seen in 1 case because of a short plate
being used. This was revised within 6 weeks using a longer holed
plate and satisfactory union was seen at follow up. Another case
of screw pull out was noted on x-ray but overall fracture
fixation was stable. 1 patient died 13 months after fixation of
fracture due to causes unrelated to the fracture fixation.
There was no incidence of deep infections,
thromboembolic events, persistent pain or malunion seen.
Periprosthetic fractures:
Amongst the cases included in our review,
there were 14 cases of periprosthetic fractures. The fractures
occurred in 7 cases around a Total hip replacement and in 6
cases around a Total knee replacement. One patient had both a
hip and knee prosthesis in situ. There was 1 compound fracture.
Mean age of patient was 73.64 +/- 14.22 years. (Mean +/- SD).The
mechanism of injury in 13 patients was a simple fall. Fracture
classification is outlined in Table 2.
|
Fracture Type |
n |
|
32A |
07 |
|
32B |
01 |
|
32C |
02 |
|
33A |
04 |
TABLE 2. AO/OTA Fracture
classification of periprosthetic fractures
In two cases, fractures occurred during
primary total hip replacement and in addition to the LISS,
cables were used to achieve fracture fixation in these 2 cases.
Patients were allowed to commence partial weight bearing
mobilisation for 6 weeks following the operation in all but 4
cases where patients remained non weight bearing for initial 6
weeks. Patients were followed up for 11.5 +/- 5.16 months (mean
+/- SD) and average time to union was 4.54 +/- 1.69 months (mean
+/- SD). All fractures proceeded to bony union.
Complications:
In 4 cases, indirect fracture reduction was
not possible and minimal open incision was required for adequate
reduction (30.7%). No failure of fixation was seen. There was no
incidence of deep infection or thromboembolic events. The
findings are summarised in Table 3.
|
Patients |
Acute femoral
fractures |
Periprosthetic
fractures |
Total |
|
Age (mean+/-SD) |
62.74 +/- 26.90 |
73.61 +/- 14.80 |
67+/- 23.62 |
|
Women |
14 |
10 |
24 |
|
Men |
09 |
04 |
13 |
|
High energy
Low energy |
8
15 |
0
14 |
8
29 |
|
Post op mobilisation
PWB
NWB |
12
11 |
10
04 |
22
15 |
|
Follow up(mean+/-SD) |
11.77+/-8.7 |
11.5+/-5.16 |
12+/-6.92 |
|
Time to union(mean+/-SD) |
4.0+/- 1.33 |
4.54+/-1.69 |
4.0+/-1.48 |
|
Failure of indirect
reduction* |
6
28.5% |
4
30.76% |
10
29.4% |
TABLE 3. Patient characteristics in
distal femoral fractures
*open fractures were excluded
Discussion :
Many treatments for distal femoral fractures
have been advocated in the past years.
In 1960s, clinical studies showed that non
operative treatment was more successful in these fractures but
it remained a serious cause of disability. Invariably the
patients had a stiff knee but the results obtained with surgical
fixation were unfavourable as well. [15] The introduction of the
AO angled blade plate in 1970 however reversed this trend. With
subsequent advances in implant technology and surgical
techniques, it is now accepted that these fractures are best
treated with surgical fixation to achieve a good functional
outcome [2].
Less Invasive Stabilization System (LISS) has
been designed to provide a stable biomechanical fixation while
preserving the blood supply to the bone with minimal soft tissue
disruption. The locked screw plate construct has greater angular
stability than compression plating devices with lesser incidence
of implant failure and has thus gained popularity in the
treatment of supracondylar femoral fractures in the last decade
[4-6].
The widely accepted indications for use of
this technique are periprosthetic fractures, intra and extra
articular diaphyseal fractures [8].
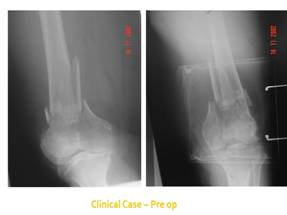
Figure1: Clinical Case pre-operative
radiographs distal femur AP and Lateral
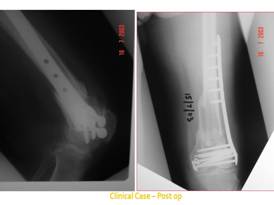
Figure 2: Post-operative radiographs
showing fracture union
The LISS acts as a splint and its function as
an internal fixator offers relative stability and results in
indirect bone healing with callus formation. Therefore, in
contrast to compression plating, the LISS plate does not have to
be in direct contact with the bone. This reduces soft tissue
dissection and preserves the blood supply to the periosteum.
This not only reduces the incidence of infection but also helps
with early post operative mobilisation. A low infection rate is
reported with LISS technique (0-8%) [4-8] and in our study there
are no cases of superficial or deep infections reported.
The biomechanical principle used during the
evolution of the LISS technique was to develop an implant which
would resist failure until after fracture healing [3,9] and a
biomechanical comparison of 4 different constructs used in
treatment of distal femoral fractures has shown that LISS has
improved distal fixation especially in osteoporotic bone [9].
Early clinical studies evaluating the
efficacy and outcome of the LISS technique have reported union
rates of 93% - 100%. [4,5,7] The average time to bony union is
between 3.5 to 4.5 months [4-6]. As evidenced in our study, we
were able to achieve 100 % union rate with LISS technique. The
average time to union noted in our study was 4 months and this
is similar to the average time reported in other studies.
Giving particular attention to the management
of periprosthetic fractures, the incidence is 0.3% to 2.5 %
[10]. The trend in management of periprosthetic fractures has
been surgical fixation with either intramedullary nailing
devices such as a retrograde nail, rush or enders nail and the
angled blade plate. The outcome has been reasonable with a
complication rate of 30%. [11]
However, in recent years, LISS technique has
emerged as an ideal technique of fixation in the treatment of
periprosthetic fractures around the knee. When compared to other
fixation methods such as compression plate and intramedullary
nailing, there were fewer instances of failure of fixation and
resultant varus angulation in fractures treated with LISS
technique. It offers better return of function and early
mobilisation. The other advantages are that there is no need for
acute bone grafting, a low risk for infection and is associated
with minimal blood loss. A recent review of the management of
periprosthetic fractures has shown that modern treatment options
in surgical fixation are better than conventional techniques of
open reduction and compression plating or non operative
management [12].
In our case series, we have treated 14 cases
of periprosthetic fractures. All cases proceeded to union (100%
union rate) with no need for primary bone grafting. We were able
to achieve early postoperative mobilisation and patients were
allowed to partially weight bear in all but 4 cases. No cases
of deep infection or failure were seen.
One of the challenges we encountered with
LISS technique was achieving adequate fracture reduction using a
closed/indirect technique. In our study, 10 cases required open
reduction (4 periprosthetic, 6 distal shaft fractures 29.41%).
Of these 10 cases, 5 cases were Type C
fractures and open reduction was probably required to visualise
the articular surface to help anatomical reduction and restore
joint congruity. The other possible explanations are complex
fracture pattern, inexperience of the surgeon and inadequate
closed reduction. These difficulties can be overcome by careful
surgical planning.
Early studies comparing the outcome of LISS
plating have highlighted its limitations in less experienced
hands and that inadequate operative experience and inappropriate
technique can result in suboptimal fixation [1]. However one
study found this system user-friendly with no major technical
difficulties [5].
Technical tips suggested in helping fracture
reduction include use of femoral distracters or Schanz screws
(joy stick).
Additional aids described to achieve an appropriate reduction
include percutaneous clamps and a bone hook. [4]
The surgical assistant can also aid fracture
reduction with posterior support of the distal fragment to
overcome the resistance of the gastrocnemius muscle. Fixation
with a k-wire will help maintain the fracture reduction.
One of the identified causes of failure of
fixation in LISS plating is an incorrectly placed plate. The
plate has a tendency to externally rotate against the lateral
femoral condoyle [1] and this can be overcome by taking
precautions to fix the plate parallel to the femur. A cadaveric
study has shown that plates fixed in external rotation are more
prone to failure [14]. In our case series, only 1 case was
noted to have a less than satisfactory fixation due to shorter
plate being used. This was revised within 6 weeks and a longer
15 hole plate was used to achieve satisfactory reduction. At
time of final follow up the fracture was united with no further
complications.
Other complications noted with LISS technique
have been delayed union (11%) and malreduction (6%) and plate
breakage (2%) [4,13] but in our study we have not encountered
any of these complications.
Conclusion :
We were able to achieve a 100% union rate
with LISS technique in both acute distal femoral and
periprosthetic fractures. There was no primary bone grafting
required and no incidence of infection was noted.
The LISS technique offers the advantages of a
stable construct with minimal soft tissue disruption.
However the procedure requires careful
surgical planning and experience in the operative technique is
paramount.
Reference :
-
OBrien P J, Meek RN,
Blachut PA, Broekhuyse H. Fractures of distal femur in Rookwood
and Green 6th ed; Vol 2; Chapter 48; Pg 1915- 1938.
-
J. H. Newman .Fractures of the femur,
Injury (1990) 21, 280-282
-
Frigg R, Appenzeller
A, Christensen R, Frenk A, Gilbert S, Schavan R. The development
of the distal femur less invasive stabilization system (LISS).
Injury 2001; 32:2431.
-
Kregor PJ, Stannard
JA, Zlowodzki M, Cole PA. Treatment of distal femur fractures
using the less invasive stabilization system: surgical
experience and early clinical results in 103 fractures. J Orthop
Trauma 2004;18:50920
-
Syed AA, Agarwal M,
Giannoudis PV, Matthews SJE, Smith RM. Distal femoral fractures:
long-term outcome following stabilization with the LISS. Injury
2004;53:599607
-
Wong MK,
Leung F,
Chow SP.
Treatment of distal femoral fractures in the elderly using a
less-invasive plating technique.
Int
Orthop. 2005 Apr; 29(2):117-20.
-
Ricci AR, Yue JJ,
Taffet R, Catalano JB, Defalco RA, Wilkens KJ. Less invasive
stabilization system for treatment of distal femur fractures. Am
J Orthop 2004;33:2505
-
Less Invasive
Stabilization System (LISS) © 2000 SYNTHES (USA)
TECHNIQUE GUIDE. Original Instruments and Implants of the
Association for the Study of Internal Fixation AO ASIF
-
Zlowodzki
M,
Williamson S,
Cole PA,
Zardiackas LD,
Kregor PJ.
Biomechanical evaluation of the less invasive stabilization
system, angled blade plate, and retrograde intramedullary nail
for the internal fixation of distal femur fractures.
J Orthop
Trauma. 2004 Sep; 18(8):494-502.
-
Althausen PL, Lee MA, Finkemeier CG, Meehan JP, Rodrigo
JJ. Operative stabilization of supracondylar femur fractures
above total knee arthroplasty: a comparison of four treatment
methods. J Arthr 2003; 18:8349.
-
Chen F,
Mont MA,
Bachner
RS.Management of ipsilateral supracondylar femur
fractures following total knee arthroplasty.
J
Arthroplasty. 1994 9(5):521-6.
-
Herrera
DA,
Kregor PJ,
Cole PA,
Levy BA,
Jönsson A,
Zlowodzki M. Treatment of acute distal femur fractures above a
total knee arthroplasty: systematic review of 415 cases
(1981-2006).
Acta
Orthop. 2008 Feb; 79(1):22-7.
-
Schultz M, Muller M,
Krettek C, Hontzsch D, Regazzoni P, Ganz R, et al. Minimally
invasive fracture stabilization of distal femoral fractures with
the LISS: a prospective multicenter study. Results of a clinical
study with special emphasis on difficult cases.Injury 2001;32:
4854.
-
Khalafi A,
Curtiss S,
Hazelwood
S,
Wolinsky
P.The effect of plate rotation on the stiffness of
femoral LISS: a mechanical study.
J Orthop
Trauma. 2006 Sep; 20(8):542-6.
-
A P Whittle.
Fractures of the Lower extremity in
Campbells Operative Orthopaedics Eleventh ed; Vol III; Chapter
51; Pg 3085.(Book Chapters)
|




