|
Abstract:
Giant cell
tumors have been extensively studied but the debate still
continues on the ideal management. Treatment modalities range
from simple curettage followed by packing of cavity with bone
cement or grafts to more radical surgeries like enbloc resection
with reconstruction. More radical procedures are associated with
much higher patient morbidity. All the procedures are associated
with recurrence and there is no consensus on the treatment of
local recurrence.
We present the case report of a 21 year male with Giant cell
tumor distal radius treated initially by wide excision and
reconstruction using autologous non vascularized fibula who had
recurrence 2 years after the initial surgery
J.Orthopaedics 2008;5(2)e3
Keywords:
Giant cell tumor, Radius, Recurrence
Introduction:
Giant cell tumor
(GCT) of bone is a benign but locally aggressive tumor involving
the ends of long bones. It constitutes about 20% of all benign
bone tumors and 5% of all bone tumors 1. It is
usually seen in young adults (females more than males) between
20 to 40 years of age 1,5,10. Its location is
typically metaphysio epiphyseal; often extending up to the sub-chondral
plate or even lies alongside the cartilage. Its most frequent
locations are, in the distal femur, the proximal tibia, the
distal radius and the sacrum, occurring in that order
1,5,10. Other less frequent sites include the fibular
head, the proximal femur, the proximal humerus and the spine. In
the long bones it is more frequently eccentric, but in several
cases it may be central. Various treatment protocols have been
advocated in the management of recurrent GCT. Traditionally,
wide en bloc resection 2,3,6 and reconstruction done
using fibular transfer (for distal radius), allograft, and
endoprosthesis. No guidelines are described if recurrence of
tumour occurs after reconstruction.
Case Report :
The patient, a
21 year male presented initially with complaints of pain and
swelling left wrist and distal forearm which was progressively
increasing. Patient was initially treated by a local
practitioner without relief and presented to us 6 months after
onset of initial symptoms. Local examination revealed fusiform
swelling on distal forearm and wrist predominantly on dorsal and
lateral aspects. Wrist range of movements restricted only at
extremes.
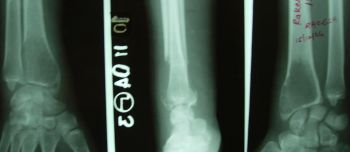
Investigations - X ray of the wrist and forearm showed an
osteolytic, expansile, lesion with ballooning of the walls over
the lower end of radius (metaphysioepiphyseal region). It
appeared geographic with well-defined borders and without
sclerosis or new bone formation or calcification, commensurate
with features of Giant cell tumor. An incisional biopsy was done
which confirmed the diagnosis of Giant cell tumor. (Fig-1).
Initial
treatment - Considering the size and extent of the tumor, a
wide excision with a 3cm healthy margin of distal radius was
performed using Henrys volar approach. Intraoperatively the
tumor capsule was found breached on the dorsal side with the
tumor tissue protruding out. The excised distal radius was
reconstructed using ipsilateral proximal fibula. The fibula was
fixed to radial stump using Dynamic compression plate and fixed
to the carpus and distal ulna using K wires. The extremity was
protected in a plaster splint for about 4 months till
radiological signs of union at radio fibular junction were seen.
The K wires were removed at 6 weeks. Patient was put on
physiotherapy regimen and gained full elbow movements. At the
wrist he had 20 deg dorsiflexion, 30 deg palmarflexion and about
10 deg side to side movements. Grip strength was about 70 % of
opposite side. Patient was not given any chemotherapy
postoperatively. (Fig 2,3 shows immediate post-op and follow-up
x-rays).
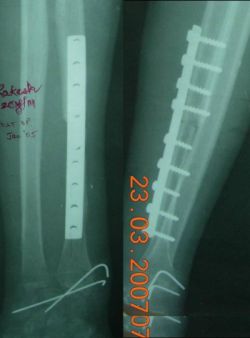

Management
after recurrence- 2 years later he returned with increasing
pain and swelling near the same wrist. X ray showed osteolytic
lesions in the transplanted fibula although the radiofibular
junction was well consolidated. A repeat biopsy was done and
came out as Giant cell tumor proving it to be a recurrence.
After proper workup and finding no obvious secondaries, patient
was operated. A wide excision was performed. The distal ulna
dissected free and centralized into a notch prepared in the
carpus after denuding the distal articular surface of ulna.
Fixation was done using an intramedullary nail passed into the
carpus. Limb was protected in plaster splint. Post operative
period was uneventful. At 2 months the ulna-carpal arthrodesis
was progressing satisfactorily. The appearance of forearm was
good. Patient had no wrist movements. At 3 months patient gained
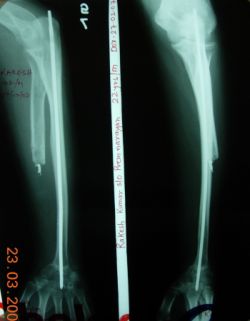
full elbow movements and was satisfied with outcome. Follow-up
at 2 years shows no local problems, good elbow movements and
satisfactory ulno-carpal union (Fig 4,5).
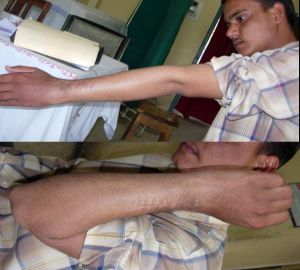
Functional
Outcome- Elbow and wrist range of movement in both flexion
and extension were assessed. Elbow flexion was 0-140 deg while
extension is 140-0 degree. No wrist movement was present. Scar
on both volar and dorsal side is also acceptable.
Discussion :
Giant cell tumor
distal radius is a common entity and wide excision followed by
reconstruction using ipsilateral fibula is a standard procedure
that has been giving satisfactory results but as mentioned
earlier there is no consensus on the management of local
recurrences after such reconstruction. Various authors have used
procedures like repeat curettage and cementing 4,
wide excision with reconstruction using the second fibula (vascularized
/ non vascularized) 7,8,11, reconstruction using
artificial prosthesis, translocation of distal ulna into the
radial gap. F.Vult von Steyern et al studied 19 patients of
local recurrence after primary curettage and cementing of which
13 had satisfactory results with repeat curettage and cementing.
We have used
centralization of ulna into the carpus as a salvage procedure
for recurrence after reconstruction using ipsilateral fibula
with satisfactory results. The disadvantage of the procedure is
a loss of pronation and supination movements at the elbow. The
procedure has got several advantages like being much simpler to
perform, no donor site morbidity, good union rate at the
ulnocarpal junction site. Translocation of distal ulna into
radius does preserve the pronation and supination at elbow but
involves lot of mobilization of the translocated ulnar fragment
with a risk of jeopardizing the vascularity and also the fact
that union has to be attained at two sites between the
tanslocated ulna to radius and between translocated ulna to
carpus 9.
We conclude that
centralization of ulna is a simple and effective salvage
procedure for recurrence of Giant cell tumor distal radius.
Reference :
-
Bridge JA, Neff JR, Mouron BJ. Giant cell tumour of bone:
chromosomal analysis of 48 specimens and review of literature.
Cancer Genet Cytogenet 1992; 58:2-13.
-
Campanacci M, Giunti A, Olmi R.Giant cell tumours of bone. A
study of 209 cases with long term follows up in 130. Ital J
Orthop Trauma 1975; 1:53-80.
-
Campanacci M, Baldini N, Boriani S,et al. Giant cell tumour
of bone. J Bone Joint Surg Am 1987; 69:105-44.
-
F.Vult von Steyern, H.C.F. Bauer, C. Trovik, A. Kivioja, P.
Bergh, P. Holmberg Jorgensen, G. Folleras, A. Rydholm. Treatment
of local recurrences of giant cell tumor in long bones after
curettage and cementing. JBJS (British) Vol 88-B, Issue 4; 2006;
531-535.
-
Huvos AG. Bone tumours: Diagnosis, treatment and prognosis.
2nd edition Philadelphia: saunders Co.; 1991
-
Liu HS, Wang JW. Treatment of giant cell tumour of bone: A
comparison of local Curettage and wide resection. Chang Keng I
Hsuey 1998; 21: 37-43.
-
Minider S. Kocher, Mark C. Gebhardt, Henry J. Mankin.
Reconstruction of the Distal Aspect of the Radius with Use of an
Osteoarticular allograft after excision of a Skeletal Tumor.
JBJS 80; 1998: 407-19.
-
Murray J A, Schalfy B. Giant cell tumors in the distal end of
the radius. Treatment by resection and fibular autograft
interpositional arthrodesis. JBJS Vol. 68-A, No. 5; June 1986;
687 694
-
Serdage H. Distal ulnar translocation in the treatment of
giant cell tumors of the distal end of radius. JBJS; Vol. 64-A,
No.1; Jan 1982; 67-73
-
Unni KK. Dahlins bone tumors: General aspect and data on
11087 cases. 5th edition. Philadelphia: Lippincott- Raven: 1998.
-
Vander Griend R.A, Funderburk C.H. The treatment of Giant
Cell Tumors of the distal part of the Radius. JBJS Vol.75-A;
No.6; June 1993; 899-908
|







