|
Abstract:
Objectives:
Subacromial syndrome with cuff involvement can be treated with
the classic, mini-open or arthroscopic methods. Our objective is
to review 71 shoulders interventions in our centre and to study
the results of these techniques.
Materials
and Methods:
We analysed age, sex, NMR lesions, type of repair,
complications, Constant, DASH and UCLA scales, among others.
Results:
Median age: 50 years; standard deviation: 9.97 years; Positive
Yochum (91.5%), partial tear (25.4%), complete tear (33.8%).
Classic repair (70.4%), arthroscopic (4.2%) mini-open (25.4%),
with harpoons (45.1%), transbone suture (15.5%), section of the
coracoacromial ligament (59.2%) and perforations in the zone of
Codman (12.7%). The final DASH results were better for the
arthroscopy (57.33 points). There were statistically significant
results when making before and after comparisons of the surgical
treatment (the open and mini-open techniques): Significant
differences were not found between the Constant and UCLA tests
(p=0.00) in our series, but there were regarding the number of
harpoons (p=0.032), with more being used in the open
techniques.
Conclusions:
In our series we did not find significant differences regarding
the outcomes of the classic and mini-open techniques. We
consider the mini-open technique to be effective, and useful in
the cases where arthroscopic experience is limited.
J.Orthopaedics 2008;5(2)e18
Keywords:
acromioplasty, rotator cuff, Constant, UCLA, DASH
Introduction:
It has been attempted to treat the pathology of the
subacromial syndrome by means of interventions where an
acromioplasty was made with later repair of rotator cuff tears.
Various methods of approaching this intervention have been
described. The classic open methods of Neer1or McLaughlin2;3 are
highlighted and others such as that of Cabot4 (classic open
acromioplasty, but with minimal incision, and without the
support of arthroscopy), Gartsman5, Yukihiko Hata6, McFarland7,
Bateman8, Neviaser9 or Watson10. On the other hand there are the
methods with arthroscopic support, with later mini incision or
mini-open, such as those of Liu11, Paulos and Kody12,
Blevins13, Shinners14, or Fearly15; or those solely with
arthroscopic support as described by Ogilvie-Harris and
Demazière16, Gartsman17or Burkhart18.
Various studies have been made that try to compare the benefits
and damages of the accomplishment of the different techniques,
using the UCLA19;20(University of California-Los Angeles) or
Constant and Murley21 tests. Our objective is to evaluate 71
interventions on subacromial syndromes using traditional
techniques, arthroscopy with the aid of mini-incisions and in
one case arthroscopy alone, evaluating the clinical results
obtained with a minimum follow-up of at least 2 years.
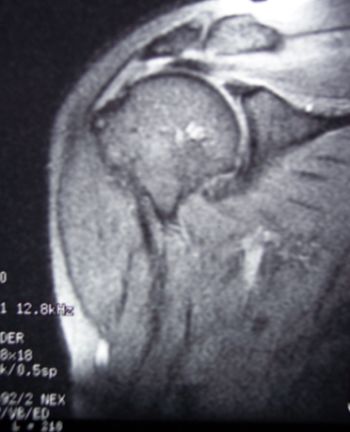
Figure 1. NMR: Observe the reduction of the subacromial
space and the discontinuity in fibres of the rotator cuff.
Zlatkin 3, Tavernier IV and Seeger 3.

Figure 2. Distribution of surgical techniques. The
predominance of the traditional technique (70.4%) is emphasised,
as opposed to the mini-open (25.4%) or arthroscopic (4.2%)
procedures.
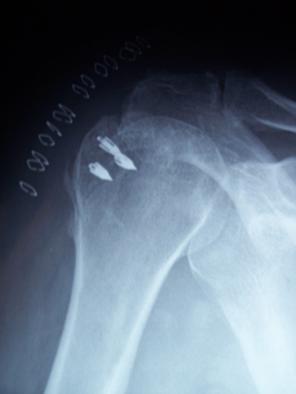
Figure 3. Positioning of harpoons in the insertion zone
of the cuff or footprint.
Table 1. Results of the DASH test. In all the groups an
evident improvement is reached, although the results obtained
with the arthroscopic technique are better than those obtained
with the traditional or mini-open techniques.
|
RESULTADOS
Test
DASH |
Traditional surgery |
Artroscopic surgery |
Miniopen surgery |
|
Preoperatory results |
126.1 |
123.33 |
130 |
|
Postoperatory results |
75.4 |
57.33 |
65.89 |
Material and Methods :
We made a descriptive, retrospective study, where 71 shoulder
interventions were included, of which 54 were men, and 17 were
women (76.1% and 23.9%, respectively). The mean age was 50.87
years, with a median of 50 years and a standard deviation of
9.97 years, with an asymmetry of 0.083 years, a minimum of 28
years and a maximum of 75 years. A right side predominance was
emphasised: 70.4%, against the left, 29.6%.
In this study the following aspects were considered at the time
of data collection:
n
PERSONAL DATA: Name, age, history number, sex, telephone number,
profession, associated pathologies. Exploration: Gerber, Yochum,
Yegarson, Neer, Hawkins, Jobe.
n
DIAGNOSTIC TESTS: Echography, Rx, NMR: tendinitis, tendinosis,
calcifications, partial or complete tears etc. Staging of the
cuff lesions according to Zlatkin, Tavernier and Seeger.
n
SURGICAL INTERVENTION: Pre-operative days, post-operative days,
open/traditional acromioplasty, mini-open or arthroscopic.
Repair of the rotator cuff with transbone sutures or harpoons.
Type of anaesthesia used. Codman perforations. Section of the
coracoacromial ligament.
n
COMPLICATIONS AND SEQUELAE: Re-tears, infection, persistent
pain, harpoon movement.
n
REHABILITATION: Time, type of rehabilitation.
n
Constants Test.
n
U.C.L.A. Test
n
D.A.S.H. Test
n
Iconographic study.
The data from the field study were analysed statistically by
means of the SPSS program, with the intention of making a
descriptive study and to state the distribution of the patients
by confidence intervals to describe the statistically
significant results that arose.
Results :
At the time of asking for the working or daily habits of the
patients, we found a predominance of mechanical activities with
trades such as bricklayer in 11.3% of men, or housewife, in
11.3% of women. Other trades such as agriculturist, plasterer,
waiter, truck driver, warehouse worker, painter or mechanic were
emphasised.
At the time of investigating for possible concomitant
pathologies, we discovered rheumatoid arthritis alone in 1.4%,
arthrosis alone in 42.3%, rheumatoid arthritis and arthrosis in
4.2% and others such as the associations of arthrosis,
rheumatoid arthritis and diabetes in 1.4%, arthrosis and
diabetes in 1.4%, arthrosis and psoriasis in 1.4%, arthrosis and
consolidated fracture in bad position in 1.4%, arthrosis and
subacromial syndrome after glenohumeral arthroplasty in 1.4%,
sequelae of greater tubercle fracture treated with cerclage in
1.4%, sequelae of greater tubercle fracture treated by means of
osteosynthesis with screw and acromioplasty in 1.4% and sequelae
of open acromioplasty 3 years before in another 1.4%.
Exploration gave the following signs, Gerber: 49.3% positive and
50.7% negative, Yegarson: 8.5% positive and 91.5% negative,
Yochum: 91.5% positive and 8.5% negative, Jobe: 83.1% positive
and 16.9% negative and finally, Neer: 45.1% positive and 54.9%
negative.
Magnetic resonance found tendinitis of the supraspinatus in
53.5%, tendinosis in 19.7% (although for many tendinitis is
synonymous with tendinosis), osteophytes in 38.0%, partial tear
in 25.4%, complete tear in 33.8%, bursitis in 23.9%,
tenosynovitis in 23.9%, old fractures of the greater tubercle in
7%, decrease in the subacromial space in 100% and bony cysts in
11.3%.
In the NMR different stages were described according to Zlatkin,
with types 0 in 1%, 1 in 12.70%, 2A in 22.50%, 2B in 9.90% and 3
in 50.70%. With the staging of Tavernier we obtained the
following distribution: I in 1%, IIA in 8.50%, IIB in 16.90%,
III in 21.10%, IV in 16.90% and V in 32.40%. The staging of
Seeger, gave: type 1 in 4%, 2A in 43.70%, 2B in 16.90% and 3 in
32.40%. (See Figure 1.)
The distribution of acromioplasties was the following:
traditional or open method in 70.4%, arthroscopic in 4.2% and
mini-open in 25.4%. Subacromial syndrome without tear: 39.4%.
There were cases of subacromial syndrome with rotator cuff tear
in 60.6%, the repair of the rotator cuff was made in 60.6%,
using transbone suture in 15.5% and the positioning of harpoons
in 45.1%. We made the exeresis of osteophytes in 16.9% and
perforations in the zone of Codman in 12.7%. (See Figures 2 and
3).
The number of pre-operative days had a median of 1 day, with a
standard deviation of 0.563 days, the number of post-operative
days had a median of 2 days, with standard deviation of 2.131
days. On the other hand, the number of harpoons used had a
median of 1 harpoon and a standard deviation of 1.2 harpoons,
with a minimum of 0 harpoons and a maximum of 4 harpoons. The
time of the intervention had a median of 105 minutes with a
standard deviation of 31.81 minutes, with minimums of 45 minutes
and maximums of 180 minutes. Lastly, the time of rehabilitation
had a median of 4 months, with a standard deviation of 1.8
months, with a minimum of 0 months and a maximum of 9 months.
Other surgical acts were the Bristow procedure in 1.4%,
bursectomy in 14.1%, bursectomy and screw extraction in 1.4%,
extraction of harpoon in 1.4%, exeresis of the supra-external
tubercle in 1.4%, fistulectomy in 1.4%, interposition of the
biceps in 1.4% and reinsertion of the rotator cuff on the
prosthesis in 1.4%.
The distribution of the intraoperative risk was ASA I: 32.4%,
II: 53.5% and III: 14.1%. The type of anaesthesia used was
balanced general: 5.6%, general with intubation: 62%, general
without intubation: 2.8%, interscalenic locoregional: 11.3%,
brachial locoregional: 5.6% and intersternocleidomastoid
locoregional: 12.7%.
The percentage of repair of the rotator cuff differed according
to the type of surgical procedure, thus in the open
acromioplasties 70% of the cases were repaired, in the
arthroscopic the rotator cuff was not repaired and in the
mini-open 44.4% of the cases were repaired. The type of repair
also differed according to the procedure used: thus, in the
open/traditional methods transbone suture was made in 16% of the
cases and harpoons were placed in 54%, of a total of 70% of
repaired cuffs, whereas in the mini-open, transbone suture was
made in 16.7% and harpoons were placed in 27.8%, of a total of
44% of repaired cuffs. The partial section of the coracoacromial
ligament differed according to the procedure used, thus, in
open/traditional acromioplasties it was made in 64%, in
arthroscopic in 0% and in the mini-open in 55.6%. The exeresis
of osteophytes was also different, in the open/traditional
procedures it was 20%, in the arthroscopic it was 0% and in the
mini-open it was 11.1%. Lastly, the perforations in the zone of
Codman were more frequent in traditional or open acromioplasties
at 16%, the arthroscopic at 0% and in the mini-open at 5.6%.
Different sequelae arose such as persistent pain in 19.7% of the
cases, crepitation in 8.5%, pain on hyperabduction in 21.1%,
keloid scar in 4.2%, limitation on attempted movement in 21.1%,
movement of harpoon in 2 cases, 2.8% of the total, in the group
of traditional acromioplasties. Re-intervention for infection in
1 case, another case with fistula from a previous intervention
for fracture of the greater tubercle, deltoid atrophy and
molestations in the deltoid region in 2.8% and 1 case of
retractable capsulitis in one open acromioplasty that prolonged
the rehabilitation to more than 1 year. It is significant that
among the sequelae, in our series, persistent pain was greater
in the open/traditional group and in the arthroscopic than in
the mini-open group, crepitation was greater in the open group,
painful hyperabduction was more frequent in the arthroscopic
group (33.3% as opposed to 22.2% in the traditional group and
16.70% in the mini-open group), keloid scars did not arise in
the arthroscopic group, nevertheless, they did appear in 4% of
the open/traditional group and in 5.6% of the mini-open group.
The limitation of mobility was greater in our series for the
arthroscopic group with values of 33.3%, as opposed to 24% of
the open/traditional group or 11.10% of the mini-open group.
Rehabilitation was centred on kinestherapy in 95% of all the
patients, although pulley-mechanotherapy in 45.10% and pendular
exercises in 39.40%, are also highlighted.
We did not find statistically significant differences regarding
pre-operative days between the different techniques, p=0.586.
There were no statistically significant differences regarding
post-operative days between the different techniques, p=0.232.
Statistically significant differences were found regarding the
number of harpoons used between the different techniques,
p=0.032. Statistically significant differences were not found
regarding the time of operation, p=0.42, nor for the time of
rehabilitation, p=0.924.
The U.C.L.A. scores ran from intolerable pain: 91.5%, one
function: Disabled 95.8%, only for light activities 1.4%. A
prior active flexion: <30º: 31%; 30-45º: 57.7%; 45-90º: 8.5%;
90-120º: 2.8% and a muscular strength for the flexion: 0:33.8%;
1:60.6%; 2:4.2%; 3:1.4%; to the post-operative tolerable pain
values: 13%, pain at rest: 18.30%, pain with heavy activities:
19.7%, occasional pain: 19.7% and no pain: 29.60%. Function:
Light activities: 7%; little: 11.3%; more: 26.8%; slight
restriction: 29.6%, normal activity: 25.4%. Prior active
flexion: Less than 30º = 0º; 30-45º: 2.8%; 45-90º: 7%; 90-120º:
11.3%; 120-150º: 26.8%; More than 150º: 52.1%. A progression
took place from a pre-operative average of 3.49 points, with a
standard deviation of 1.34 points, to an post-operative average
of 25.01 points, with a standard deviation of 8.106 points,
passing from bad pre-operative results in 100% to the integrated
post-operative distribution for bad results in 19.70%, regular
in 39.40%, good in 22.50% and excellent in 18.30%. A
statistically significant global improvement took place
regarding the difference produced between the pre-operative and
the post-operative values in all the groups: p= 0.001, with
margins in - 19.596; - 23.446. Statistically significant partial
improvement in the open/traditional group: p= 0.000,
statistically significant partial improvement in the mini-open
group: p=0.000 and partial improvement, although not
statistically significant in the arthroscopy group: p=0.102.
The Constant test showed a global improvement, in that bad
pre-operative scores in 100% changed to post-operative scores
after open/traditional acromioplasties of bad in 26%, regular in
28%, good in 20% and excellent in 26%; in the arthroscopic, bad
in 33%, regular in 33% and good in 33%, without excellent
results, and finally, with post-operative results in the
mini-open techniques that were bad in 17%, regular in 33%, good
in 16.70% and excellent in 33%. This global improvement in the
Constant scores was statistically significant, with p=0.000, a
95% confidence interval for the difference between the
pre-operative and post-operative results, with reductions in the
scores of between 57.793 and 48.038, with a mean reduction of
52.915 points. Statistically significant differences were
obtained in each individual technique, however, there were no
statistically significant differences when comparing the results
of one technique with those of another.
In the D.A.S.H test the following outcome measures were
obtained: in the open/traditional group a pre-operative mean of
126.10 points was obtained, with a standard deviation of 10.181
points, and a post-operative mean of 75.24 points, with a
standard deviation of 32.131 points. In the arthroscopic group
the pre-operative mean was 123.33 points, with a standard
deviation of 8.145 points, and a post-operative mean of 57.33
points, with a standard deviation of 14.189 points.
Finally, in the mini-open interventions, the pre-operative mean
was 130 points, with a standard deviation of 7.404 points, and a
post-operative mean of 65.89 points, with a standard deviation
of 28.130 points.
Statistically significant improvements in D.A.S.H outcome
measures took place, with p=0.000 and a 95% confidence interval
for the difference, with a lower limit of 47.812 points and an
upper of 61.906 points, a statistically significant improvement
in the open group with p=0.031, with lower and upper limits of
14.668 and 117.332 points respectively, with a statistically
significant improvement in the mini-open group with p=0.000,
with lower and upper limits of 49.242 and 78.980 points
respectively and, in general, with a statistically significant
improvement in all the items when making pre- and post-operative
comparisons. (See Table 4).
Discussion :
In our series we have tried to compare
different surgical procedures at the time of approaching
subacromial syndrome, as well as the repair of the rotator cuff.
We found a general improvement after the interventions,
nevertheless, we did not find statistically significant
differences between the different techniques. Throughout recent
history multiple studies have been published where these
possible differences are expressed. Open techniques have been
proposed, such as that described by Gartsman5 in 1997, who made
a revision of massive tears in the rotator cuff with a series of
33 patients, who underwent debridement of adhesions and
subacromial decompression by means of open acromioplasty. His
study was based on the tests of Constant and Murley21and that of
the University of California in Los Angeles (UCLA)19;20,
verifying a functional improvement in the shoulder with a
significant reduction of pain with p= 0.001 and an increase in
the range of movement with p= 0.016. Post-operatively there were
no cases of dehiscence in the transdeltoid suture, the pain
decreased and the abduction improved p=0.0022. The UCLA scale
went from 11.5 points to 21.0 points finally. The Constant and
Murley test results went from 31.2 points to 52.4 points
finally. Nevertheless, although the function of the shoulder
improves after the intervention, a diminution occurs in the
range of movement and remaining strength in comparison with the
non affected opposite shoulder. This is one of the conclusions
reached by Kronberg22 in his 1997 work, where 37 patients with
traditional repairs to cuff tears were studied. Comparing both
shoulders, those with intervention reached a mean score of 77
points in the Constant test as opposed to a mean score of 92
points in the shoulders without intervention.
Nevertheless, other authors prefer traditional surgery without
arthroscopy, but with different approaches. Thus, Yukihiko Hata6
applied a less invasive approach in a group of 22, by means of a
trans-acromial incision of about 3 cm in length and making a
prior acromioplasty with liberation of the coracoacromial
ligament. Prior arthroscopy had been made. This group was
compared with another of 36 patients to whom the classic
technique was applied. There were no significant differences
between the groups where the UCLA test gave 33.2 and 32.8 points
in both groups respectively at follow-up one year after the
surgery. However, the active mobility in forward flexion in the
group with the mini approach was greater (157.1º +/- 9.5º) than
in the group with the classic open technique (149.2 +/- 13.7º)
at 3-6 months after the surgery. With the mini approach the
patients returned to their sports or daily activities earlier
than the traditional group.
McFarland7 described lateral acromioplasty that would be
indicated fundamentally in patients with massive tears of the
rotator cuff, where the acromion in its anterior segment and the
coracoacromial ligament have to be preserved.
Other authors have preferred to use the techniques with
mini-approaches and arthroscopic support, in this way, Levy23,
described the arthroscopic decompression and suture of the tear
by means of a small route of approach or mini-open, obtaining
an improvement in pain, functionality, movement and strength,
with a satisfaction of 96%. Paulos and Kody12 also proposed the
technique of repair by lateral transdeltoid mini-approach with
arthroscopic decompression, in a study of 18 patients of whom
88% reached a favourable result in the UCLA test. Blevins13 made
revisions in 64 patients with interventions for repair of the
rotator cuff by means of arthroscopy and assistance with a
mini-approach, obtaining a reduction in subacromial compression
or impingement from 96% to 16%. Shinners14 developed a study
on 67 patients using arthroscopic repair assisted with a
mini-approach, obtaining a mean of 32.3 points in the UCLA test.
There were no significant differences in the UCLA test results
with respect to the size of the tear (p<0.4286) or the age of
the patient (p< 0.1131). Stephen Fearly15 later applied prior
visualisation with arthroscopy and a mini-approach in various
tears, with 83% of the patients returning to their prior
activities after the intervention.
In general, arthroscopic surgery of the rotator cuff involves a
series of advantages, as reported by Yamaguchi24, who indicated
that the greatest advantage of the mini-open and arthroscopic
techniques over the traditional approach is based on the small
incisions, the preservation of the deltoid musculature, with
less damage, less tissue dissection, less post-operative pain,
shorter stays in hospital14, easier rehabilitation, better
visualisation and access to the glenohumeral joint, facilitating
the diagnosis and the treatment of associated intra-articular
diseases such as synovitis, bicipital tendinitis, capsular-labral
diseases and glenohumeral arthritis. For Burkhart18, arthroscopy
allows treating rotator cuff tears irrespective of the size of
the tear or the number of tendons involved, allowing the better
appreciation of the configuration of the tear that is obtained
with the arthroscope and by the development of the repair
technique called margin convergence.
Similarly, there are various studies, like the one of Liu11,
that establish that the mini-open approach allows results
similar to the traditional open technique to be obtained, but
involving a shorter hospital stay, faster rehabilitation, better
cosmetic result, better evaluation and treatment of glenohumeral
diseases and preservation of the deltoid insertions. A value of
32.7 points in the UCLA test was reached in his series of 44
patients. The mini-open technique combines the benefits of the
open technique with the advantages of making a small and
cosmetic scar in the deltoid, that does not violate the
insertion of the musculature in the acromion, nevertheless
Fearly15, for example, does not recommend its use in cases of
subscapularis tears, since in these cases the open or
traditional technique would be preferred. Paulos and Kody12 also
found a 94% satisfaction among their patients treated by means
of arthroscopy assisted mini-open approach. Also Blevins13 , was
able to achieve a reduction in impingement from 96% of the
pre-operative cases to 16% post-operatively with the mini-open
technique. The active elevation increased significantly, from
129º to 166º. Baker and Liu25 compared the open technique with
the mini-open assisted arthroscopically. In a retrospective
study on 37 patients they obtained good results in 80% of the
traditional or open group, nevertheless, in the group with the
mini-open approach good results were obtained in 85% of the
cases, with a shorter hospital stay and an earlier return to
their labour activities. Yukihiko Hata26 studied the atrophy of
the deltoid after rotator cuff surgery. For this he grouped 43
cases treated in the traditional open way and 45 with an
arthroscopic manner assisted with a mini-approach or
mini-open. It was observed that the weakness of the anterior
segment of the deltoid was not manifest in the mini-open group,
however, in the traditional group an atrophy occurred that was
measurable in NMR up to approximately 60%. The period required
to return to work in the mini-open group was 2.4 months, which
was shorter than the time required for the return to work with
the traditional approach, which was 3.4 months. Vives27 studied
subacromial syndrome in golf players, for which he grouped 15
patients who had the traditional open technique and 16 who had
the arthroscopic technique with mini-open. There were no
significant differences regarding the driving distances when
comparing the pre- and post-intervention data. Yukihito Hata6
made a comparative study of a group of 36 patients who had the
traditional intervention with another group of 22 patients where
a mini-approach of 3cm was used, emphasising that there were no
significant differences between groups in the UCLA test,
referring to post-operative values of the UCLA test of 33.2 and
32.8 in both groups respectively at follow-up one year after the
surgery. With the mini technique the patients returned earlier
to their previous activities.
Also, other studies have been developed where arthroscopy was
evaluated as an exclusive technique. In fact, the exclusively
arthroscopic repair has produced better results than even the
traditional open forms. A proof of this is the review of Tauro28
on 53 patients modifying the values of the UCLA scale from 16 to
45 points post-operatively, with less postsurgical pain and
easier rehabilitation, compared with those that had a classic
traditional or open approach. Ogilvie-Harris and Demazière16,
published a study in 1992 where they compared 2 types of
treatments, a group of 22 patients where arthroscopic
subacromial decompression was used, against 23 patients where
the traditional open technique was applied. Similar results were
obtained regarding the improvement of pain and the active range
of flexion. In 1998 Gartsman17 made another review of 73 purely
arthroscopic repairs, with a minimum follow-up of 2 years. Good
to excellent post-operative results were obtained in 84% of the
patients in the UCLA test. In 2001 Burkhart18, made a study
where he evaluated the arthroscopic repair of the cuff on 59
cases with the UCLA test. For Burkhart the results were
independent of the size of the tear with a p>0.05 and the
results obtained by means of suture of the tendon to the bone or
margin convergence were similar, emphasising the functional
improvement presented in the UCLA test with a p<0.0001. These
results were not influenced by the size of the tear or by the
number of tendons involved. The results that Burkhart obtained
led him to state that the arthroscopic technique gives superior
results than the open procedures in the cases of large or
massive tears. Severud29 compared 35 patients who had the purely
arthroscopic technique with 29 patients who had the mini-open
technique, with a follow-up of 44.6 months. The mean final score
obtained with the UCLA scale was 32.6 points for the
arthroscopic group and 31.4 points for the mini-open group. In
general the results are similar, but the low rate of fibrosis in
the arthroscopic group leads the author to prefer the
exclusively arthroscopic form. Weber30 made a study where he
analysed 126 shoulders operated on with the exclusively
arthroscopic technique and 154 by means of the mini-open
techniques. No significant differences between the 2 groups were
found at the end of the follow-up in the ASES, UCLA or SST
assessments. In 1999 Weber31 made a comparative study between
the arthroscopic and mini-open procedures, with it being
remarkable that only 6 of the 33 patients with the traditional
or open procedure did not require narcotics in the recovery
room, whereas 31 of the 32 patients with the arthroscopic
procedure did not require these drugs, a finding which supports
the view that the arthroscopic procedure causes less
post-operative pain. Warner32 made a study where he included 9
patients operated on in an exclusively arthroscopic manner and
12 with a repair with a mini-open procedure. The SST or Simple
Shoulder Test was used which revealed a significant reduction in
the pain levels, whilst there were no large differences between
the groups regarding the pre- or post-operative flexions or the
external rotation. The group with the arthroscopic intervention
showed an increase in the strength of the intervened member
(p<0.01), something not so evident in the group with the
mini-open intervention (p=0.26). Seung-Ho Kim33 tried to
evaluate the differences existing between 42 patients where the
technique applied was exclusively arthroscopic and another 34
patients where the mini approach was used after having tried a
previous arthroscopy without success. Using the UCLA test and
the ASES (American Shoulder and Elbow Surgeons shoulder rating
scale) he observed improvements regarding the pain, mobility of
the shoulder and the return to daily activity, without seeing
clear differences between both techniques, however, the larger
the tear the lower were the test results.
Fearly15 considered that the accomplishment of an arthroscopic
subacromial decompression with mini-open can be an effective
alternative to the exclusively arthroscopic repair of the
rotator cuff, because it allows an intense mobilisation of the
retracted tendons and a medial liberation of the adhesions.
Herrera34 considers that the arthroscopic procedures are the
best, semi-sterile, with a continuous washing of the surgical
field. The conversion from an arthroscopic method to an open or
a mini-open method supposes an increase in the risk of
developing an infection by the saprophytic flora of the skin, by
agents such as Propionibacterium acnes, Staphylococcus
epidermidis, aureus or Pseudomonas aeruginosa. Although the rate
of deep infection after the repair of the rotator cuff with an
open or standard technique can be determined at 0.27-1.7%35;36,
the rate of infection after the approach with mini-incision
would be determined at 1.9%.
The strange method of the study made in 1994 by Grana37 is
highlighted, where it is explained that the arthroscopic
evaluation did not in itself affect the functional result, but
which increased the cost by 2000 dollars for each patient. The
arthroscopy can help to define the size of the tear, which can
condition the type of approach used, but for Grana the
arthroscopic treatment of glenohumeral problems would not alter
the functional result, it would be expensive, non-effective and
in addition he would not recommend it. We do not share this
idea.
In our series we have not had excessive complications, in fact,
there were specific cases, nevertheless, the surgery of the
rotator cuff is not free of complications, as in the series of
Gartsman with the appearance of 2 seromas and a case of
infection. Vives27 in his series describes 2 cases of infection,
with positive cultures for Staphylococcus epidermidis. Herrera34
describes a rate of infections of 1.9% after the 360
acromioplasties performed with the mini-open procedure. The
treatment consisted of the debridement and irrigation of the
articular cavity and revision of the rotator cuff repair
together with intravenous antibiotherapy during an average of
4.2 weeks, observing sensitivity to ciprofloxacin, vancomycin,
clindamycin and kefzol. After the intravenous treatment it was
possible to continue with oral treatment with amoxicillin-clavulanic
acid and/or ciprofloxacin for 2 weeks. The agent most involved,
in up to 86% of the cases, was Propionibacterium acnes. The
conversion from an arthroscopic method to an open, supposes an
increase in the risk of developing an infection by the
saprophytic flora of the skin, as has been commented previously.
Settecerri36 also observed 16 cases of infection after the
repair of the rotator cuff between 1975 and 1994, where the most
frequent agent was Propionibacterium acne in 6 cases, coagulase
negative Staphylococcus in 4 cases, Peptostreptococcus magnus in
1 case and the association of Propionibacterium and coagulase
negatives in another case. Mirzayan38 studied deep infection
after rotator cuff repair and found agents in the following
order of frequency, Staphylococcus epidermidis, Staphylococcus
aureus and Propionibacterium species. Also, cutaneous
hypersensitivity in the lateral portal has been described by
Kim33, transitory paresthesias in the hand of the intervened
side described by Burkhart18, keloid scars33, reactions to the
suture material used, as Severud29 explains, persistence of the
clinical picture of subacromial compression, with
re-interventions (Blevins13), reappearance of osteophytes and
subacromial clinical picture (Shinners14), reduction in strength
when trying to elevate objects in some series with p=0.0007, or
difficulties for working overhead can be caused by the resection
of the coracoacromial ligament as reported by Rockwood39,
Nirschl40and Flatow41. The atrophy of deltoids26, reviewed by
Groh42, that would take place in the classic intervention by the
involvement of the insertion point of the deltoid or by damage
in the axillary nerve. The preservation of deltoid function is
essential, as has been described by authors such as Adamson43,
Bigliani44, Neviaser45 or Iannotti46, since it provides 50%42 of
the strength for the elevation of the arm in the scapular plane.
Also tears of the long portion of the biceps29 have been
described, re-tears of the cuff29 as described by Cabot4 or
Blevins13, which in some cases required revision surgery, this
time open27. Also adhesions and frozen shoulder have been
described after rotator cuff surgery, as described by Mormino47.
Ankylosis or fibrosis, defined as a failure to reach a flexion
greater than 120º has been described in patients in whom the
mini-open has been used.
Postsurgical pain can be corrected with the accomplishment of
interscalenic blockades, which also determines a reduction in
the anaesthetic requirements during the intervention.
Conclusion:
With acromioplasty and the repair of the rotator cuff we were
able to improve the clinical picture of subacromial syndrome.
The progression of the surgery has brought about the boom in
arthroscopic procedures. We consider that the mini-open
technique with prior arthroscopic support is an alternative that
will allow the progressive step to an exclusively arthroscopic
system, that can be used without requiring large learning
curves, especially in those shoulder cases which are not yet
controlled with arthroscopic procedures.
Reference :
-
Neer CS 2nd. Anterior acromioplasty for the chronic
impingement syndrome in the shoulder: a preliminary report. J
Bone Joint Surg Am.1972 Jan;54(1):41-50.
-
McLaughlin HL. Lesions of the musculotendinous cuff
of the shoulder. The exposure and treatment of tears with
retraction. 1944. Clin Orthop Relat Res.1994 Jul;(304):3-9.
-
McLaughlin HL. Repair of major cuff ruptures. Surg
Clin North Am.1963 Dec;43:1535-40.
-
Cabot A, Cabot JC. Minimal incision acromioplasty.
Orthopedics.2002 Dec;25(12):1347-50.
-
Gartsman GM. Massive, irreparable tears of the
rotator cuff. Results of operative debridement and subacromial
decompression. J Bone Joint Surg Am.1997 May;79(5):715-21.
-
Hata Y, Saitoh S, Murakami N, et al. A less invasive
surgery for rotator cuff tear: mini-open repair. J Shoulder
Elbow Surg.2001 Jan-Feb;10(1):11-6.
-
McFarland EG, Park HB, Kim TK, et al. Limited lateral
acromioplasty for rotator cuff surgery. Orthopedics.2005
Mar;28(3):256-9.
-
Bateman JE. The diagnosis and treatment of ruptures
of the rotator cuff. Surg Clin North Am.1963 Dec;43:1523-30.
-
Neviaser JS. Surgical approaches to the shoulder.
Clin Orthop Relat Res.1973 Mar-Apr;(91):34-40.
-
Watson M. Major ruptures of the rotator cuff. The
results of surgical repair in 89 patients. J Bone Joint Surg
Br.1985 Aug;67(4):618-24.
-
Liu SH. Arthroscopically-assisted rotator-cuff
repair.
J
Bone Joint Surg Br.1994 Jul;76(4):592-5.
-
Paulos LE, Kody MH.
Arthroscopically enhanced "miniapproach" to rotator cuff repair.
Am J Sports Med.1994 Jan-Feb;22(1):19-25.
-
Blevins FT, Warren RF, Cavo C, et al. Arthroscopic
assisted rotator cuff repair: results using a mini-open deltoid
splitting approach. Arthroscopy.1996 Feb;12(1):50-9.
-
Shinners TJ, Noordsij PG, Orwin JF. Arthroscopically
assisted mini-open rotator cuff repair. Arthroscopy.2002
Jan;18(1):21-6.
-
Fealy S, Kingham TP, Altchek DW. Mini-open rotator
cuff repair using a two-row fixation technique: outcomes
analysis in patients with small, moderate, and large rotator
cuff tears. Arthroscopy.2002 Jul-Aug;18(6):665-70.
-
Ogilvie-Harris DJ, Demaziere A. Arthroscopic
debridement versus open repair for rotator cuff tears. A
prospective cohort study. J Bone Joint Surg Br.1993
May;75(3):416-20.
-
Gartsman GM, Khan M, Hammerman SM. Arthroscopic
repair of full-thickness tears of the rotator cuff. J Bone Joint
Surg Am.1998 Jun;80(6):832-40.
-
Burkhart SS, Danaceau SM, Pearce CE Jr. Arthroscopic
rotator cuff repair: Analysis of results by tear size and by
repair technique-margin convergence versus direct tendon-to-bone
repair. Arthroscopy.2001 Nov-Dec;17(9):905-12.
-
Burkhart SS. Arthroscopic debridement and
decompression for selected rotator cuff tears. Clinical results,
pathomechanics, and patient selection based on biomechanical
parameters. Orthop Clin North Am.1993 Jan;24(1):111-23.
-
Ellman H, Hanker G, Bayer M. Repair of the rotator
cuff. End-result study of factors influencing reconstruction. J
Bone Joint Surg Am.1986 Oct;68(8):1136-44.
-
Constant CR, Murley AH. A clinical method of
functional assessment of the shoulder. Clin Orthop Relat
Res.1987 Jan;(214):160-4.
-
Kronberg M, Wahlstrom P, Brostrom LA. Shoulder
function after surgical repair of rotator cuff tears. J Shoulder
Elbow Surg.1997 Mar-Apr;6(2):125-30.
-
Levy HJ, Uribe JW, Delaney LG. Arthroscopic assisted
rotator cuff repair: preliminary results.
Arthroscopy.1990;6(1):55-60.
-
Yamaguchi K, Ball CM, Galatz LM. Arthroscopic rotator
cuff repair: transition from mini-open to all-arthroscopic. Clin
Orthop Relat Res.2001 Sep;(390):83-94.
-
Baker CL, Liu SH. Comparison of open and
arthroscopically assisted rotator cuff repairs. Am J Sports
Med.1995 Jan-Feb;23(1):99-104.
-
Hata Y, Saitoh S, Murakami N, et al. Atrophy of the
deltoid muscle following rotator cuff surgery.
J
Bone Joint Surg Am.2004 Jul;86-A(7):1414-9.
-
Vives MJ, Miller LS, Rubenstein DL, et al.
Repair of rotator cuff tears in golfers. Arthroscopy.2001
Feb;17(2):165-72.
-
Tauro JC. Arthroscopic rotator cuff repair: analysis
of technique and results at 2- and 3-year follow-up.
Arthroscopy.1998 Jan-Feb;14(1):45-51.
-
Severud EL, Ruotolo C, Abbott DD, et al.
All-arthroscopic versus mini-open rotator cuff repair: A
long-term retrospective outcome comparison. Arthroscopy.2003
Mar;19(3):234-8.
-
Weber S.C. All-arthroscopic versus mini-open repair in the
management of tears of the rotator cuff: A prospective
evaluation (abstract). Arthroscopy.2001.17(suppl 1).
-
Weber SC. Arthroscopic debridement and acromioplasty
versus mini-open repair in the treatment of significant
partial-thickness rotator cuff tears. Arthroscopy.1999
Mar;15(2):126-31.
-
Warner JJ, Tetreault P, Lehtinen J, et al.
Arthroscopic versus mini-open rotator cuff repair: a cohort
comparison study. Arthroscopy.2005 Mar;21(3):328-32.
-
Kim SH, Ha KI, Park JH, et al. Arthroscopic versus
mini-open salvage repair of the rotator cuff tear: outcome
analysis at 2 to 6 years' follow-up. Arthroscopy.2003
Sep;19(7):746-54.
-
Herrera MF, Bauer G, Reynolds F, et al. Infection after
mini-open rotator cuff repair. J Shoulder Elbow Surg.2002
Nov-Dec;11(6):605-8.
-
Post M. Complications of rotator cuff surgery. Clin
Orthop Relat Res.1990 May;(254):97-104.
-
Settecerri JJ, Pitner MA, Rock MG, et al. Infection
after rotator cuff repair. J Shoulder Elbow Surg.1999
Jan-Feb;8(1):1-5.
-
Grana WA, Teague B, King M, et al. An analysis of
rotator cuff repair. Am J Sports Med.1994 Sep-Oct;22(5):585-8.
-
Mirzayan R, Itamura JM, Vangsness CT Jr, et al.
Management of chronic deep infection following rotator cuff
repair. J Bone Joint Surg Am.2000 Aug;82-A(8):1115-21.
-
Rockwood CA Jr, Williams GR Jr, Burkhead WZ Jr.
Debridement of degenerative, irreparable lesions of the rotator
cuff. J Bone Joint Surg Am.1995 Jun;77(6):857-66.
-
Nirschl RP. Rotator cuff surgery. Instr Course
Lect.1989;38:447-62.
-
Flatow, E. L. Coracoacromial ligament preservation in
rotator cuff surgery. J.Shoulder and Elbow Surg.1994.3:573 .
-
Groh G.I, Simoni M, Rolla P, et al. Loss of the
deldoid after shoulder operations: an operative disaster. J
Shoulder Elbow Surg.1994.3:243-53.
-
Adamson G.J, Tibone J. E. Ten-year assessment of
primary rotator cuff repairs. J Shoulder Elbow Surg.1993.2:57-63
.
-
Bigliani L.U, McIlveen S. J Cordasco F. A, et al.
Operative management of failed rotator cuff repairs. Orthop
Trans.1998.12:674.
-
Neviaser R.J, Neviaser T. Reoperation for failed
rotator cuff reapir: Analysis of fifty cases. J Shoulder Elbow
Surg.1992.1:283-286.
-
Iannotti JP. Full-Thickness Rotator Cuff Tears:
Factors Affecting Surgical Outcome. J Am Acad Orthop Surg.1994
Mar;2(2):87-95.
-
Mormino MA, Gross RM, McCarthy JA. Captured shoulder:
a complication of rotator cuff surgery. Arthroscopy.1996
Aug;12(4):457-61.
|





