|
Abstract:
Staphylococcal
toxic shock syndrome is a multi systemic illness that occurs
infrequently, with an incidence less than 0.05 cases per 100,000
populations. A missed diagnosis of staphylococcal toxic shock
syndrome can have potentially long-lasting squeal. This report
stresses the need to employ a high index of suspicion when
treating unwell children with febrile illness and cutaneous
signs.
J.Orthopaedics 2008;5(1)e11
Case
Report:
A
ten months old Chinese girl with normal developmental
milestones, presented in casualty with a two weeks history of
illness and cough. She had been spiking temperature for two days
and had experienced two episodes of diarrhoea and vomiting. On
admission, she was febrile and irritable with a grunting
respiration. She was tachycardiac and hypotensive with a
capillary refill time of 5 seconds. The conjunctivae and
oropharynx looked inflamed.
Urgent
blood tests showed raised CRP (215 mg/l), leukopenia (WCC
3x109/l), reduced platelets (94x109/l), and a deranged
coagulation profile (D-dimer 16166 ng/ml, INR 1.7). Arterial
blood gas analysis revealed metabolic acidosis. A chest x ray
revealed right-sided lower lobe consolidation. The Cerebrospinal
Fluid analysis was normal.
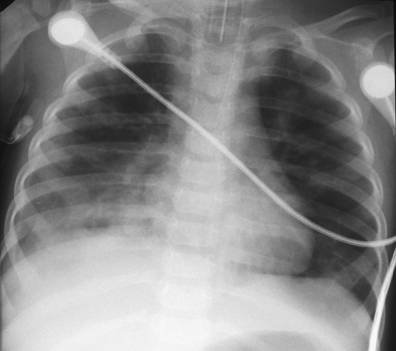 Figure
1. Chest radiograph showing pneumonic consolidation in the
right lung base
She
was intubated, ventilated and resuscitated with intravenous
fluids and inotropic support. Intravenous Ceftriaxone and
Benzylpenicillin were commenced immediately. She received fresh
frozen plasma, cryoprecipitate and Vitamin K to correct her
coagulation profile. Within hours of admission, three petechial
spots developed on her back, followed by a purpuric rash on her
legs that became rapidly progessive. She also developed poor
perfusion in both lower extremities. She had established global
purpura fulminans by the time she was transferred to the
paediatric intensive care unit.
The
patient had a protracted ICU admission. Initially she developed
a picture consistent with ARDS, which improved with high
frequency oscillation, nitric oxide and steroids. By this time,
a virulent Staphylococcus Aureus had been grown from blood
cultures, skin scrapings from her purpuric rash, throat swab,
and endotracheal secretions. The microbiologist recommended
starting her on a poly-antimicrobial regime, consisting of
Flucloxacillin, Clindamycin and Imipinem. She also received
electrolyte infusions, blood and platelet transfusions. By the
second week, her cardiovascular system had stablilised.
Investigations revealed essentially normal immunoglobins and T
cell subsets, normal coagulation profile and Proteins C and S.
By
now, the perfusion in her lower extremities had deteriorated
further. These became gangrenous and developed two clear
demarcation lines. This necessitated bilateral below-knee
amputations, followed by split-skin grafting to both stumps. The
right stump healed well, such that it was fitted with a
tuber-bearing prosthesis two months later. However, the left
lower limb stump developed
an infection and assumed a fixed flexion deformity at the knee.
A sinus developed on the anteromedial aspect of the stump, and a
swab taken from it returned positive for staphylococcus aureus.
MRSA was also isolated from nose, throat, axillary and groin
swabs.
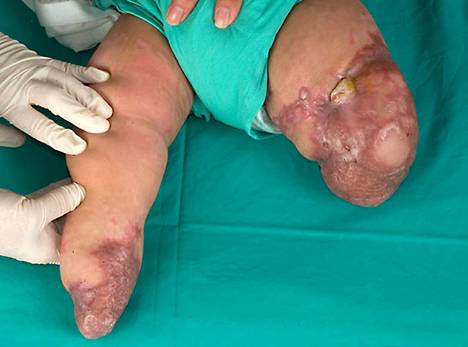
Figure
2. A healed low trans-tibial amputation on the right, and an
infected stump on the left, with the knee in fixed flexion, and
a sinus anteromedially.
Radiographs
showed evidence of chronic osteomyelitis, with an involucrum
overlying nearly all of the femoral diaphysis. She was continued
on a long-term course of oral clindamycin. A radiograph taken a
couple of weeks later revealed a pathological fracture at the
junction of the middle and lower thirds of the diaphysis. A
wait-and-see policy was followed with continued antibiotics,
weekly inflammatory markers and monthly x-rays. The fracture
eventually healed, with only some residual infection in the
region of the distal diaphysis. This was addressed with a
limited incision and curettage, from which she recovered well.
She is doing well developmentally and is now awaiting a
left-sided prosthesis, nearly 14 months after initial
presentation.
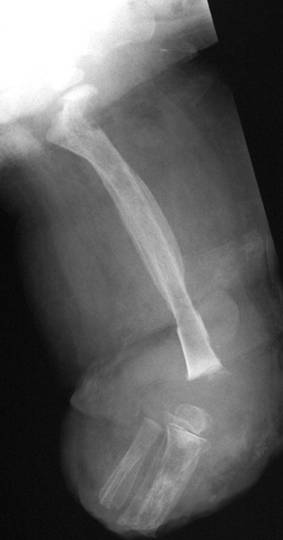
Figure
3. Radiograph showing large involucrum and sequestrum
involving femoral shaft, with a fracture line visible in the
lower femoral shaft.
Discussion:
Staphylococcal
toxic shock syndrome is a multisystemic1 illness that
occurs infrequently, with an incidence less than 0.05 cases per
100,000 population2,3. It is caused by
Exotoxin-producing strains of Staphylococcus aureus. The Centre
for disease control has established major, minor, and
exclusionary criteria to aid diagnosis4.
Major
Criteria:
Fever
> 38.9
Rash
(diffuse macular erythroderma)
Desquamation
Hypotension
/ orthostatic syncope
Minor
Criteria: Multisystem involvement (3 or more criteria must be
met)
Gastrointestinal:
vomiting or diarrhea at onset of illness
Muscular:
severe myalgia or creatine kinase level twice upper limit of
normal for laboratory
Mucous
membrane: vaginal, oropharyngeal, or conjunctival hyperemia
Renal:
blood urea nitrogen or creatinine level at least twice upper
limit of normal for laboratory, or >5 white blood cells per
high-power field in absence of urinary tract infection
Hepatic:
total bilirubin, aspartate aminotransferase, or alanine
aminotransferase at least twice upper limit of normal for
laboratory
Hematologic:
platelets <100,000/mm3
Central
nervous system: disorientation or alterations in consciousness
without focal neurologic signs when fever and hypotension are
absent.
Exclusionary
Criteria: Normal results on the following tests (if performed):
Blood,
throat, or cerebrospinal fluid cultures (blood culture may be
positive for Staph aureus)
Absence
of other explanation for the clinical presentation.
This
patients initial presentation satisfied three major (fever,
rash, hypotension) and three minor criteria (vomiting/diarrhoea,
conjunctival hyperaemia, thrombocytopaenia), and both the
exclusionary criteria for case definition. Treatment in such
cases is mainly supportive. It is aimed at correcting the
multiorgan dysfunction with circulatory and inotropic support,
maintaining respiratory and renal function, parenteral
antibiotics, and correction of disturbed haematological indices
and electrolytes.
We
need to employ a high index of suspicion when treating unwell
children with febrile illness and cutaneous signs. The
differential diagnosis includes Kawasaki syndrome, streptococcal
toxic shock syndrome, leptospirosis and measles. A missed
diagnosis of staphylococcal toxic shock syndrome can have
potentially long-lasting sequelae, as experienced by this
patient.
References:
- Behrman RE, Kleigman RM, Jenson HB eds
(2004). Nelsons
Textbook of Paediatrics. 17th ed. Saunders Ltd, Pennsylvania:
865-866.
- Centers
for disease control. Follow-up on Toxic Shock Syndrome - United
States. MMWR Morb Mortal Wkly Rep 1980; 29(25); 297-9.
- Hajjeh
RA, Reingold A, Weil A et al (1999) Toxic shock syndrome in the
United States: Surveillance Update, 1979-1996. Emerg Infect Dis
5:807-10.
- Centers
for disease control and prevention. Case Definitions for Public
Health Surveillance. MMWR Morb Mortal Wkly Rep October 19, 1990;
39; 38-9.
|





