|
Abstract:
Internal
fixation has become standard treatment in unstable sacroiliac
injuries. Associated soft tissue trauma increases risk of
complications when attempting open reduction and internal
fixation. Closed reduction and percutaneous screw fixation seems
to minimize this risk. Thirty-six vertically unstable pelvic
fractures were included in a prospective clinical study. Closed
reduction and percutaneous iliosacral screw fixation was done in
all patients. The mean age of patients was 31 years (range 15 to
60 years). The posterior injury was pure sacroiliac dislocation
in seventeen patients, sacroiliac fracture dislocation in seven
and sacral fracture in twelve. The anterior lesion was pure
symphyseal disruption in twelve patients, ipsilateral fracture
of superior and inferior pubic rami in fifteen, bilateral
fracture of pubic rami in two, and combined fracture of pubic
rami and symphyseal disruption in seven. Two pelvic fractures
were open. Perineal tear was associated in two patients.
Anterior fixation was by symphyseal plating in nine patients and
by external fixation in two. Twenty five had no anterior
fixation. Closed reduction was excellent in twenty two patients,
good in ten, and fair in four. Loss of reduction was reported in
three patients during follow up. Screw misplacement occurred in
four patients but without neurological or vascular
complications. Pain free gait was achieved in 54% of patients,
occasional pain in 35% and persistent pain in 11%.
We conclude that closed reduction and iliosacral screw
fixation allows anatomical restoration of stability of
sacroiliac disruptions in the vertically unstable pelvis.
J.Orthopaedics 2007;4(4)e26
Keywords:
Pelvic bone fracture; iliosacral screw; closed reduction; sacral
fracture; sacroiliac injury
Introduction:
Vertically
unstable fractures of the pelvis are uncommon, but it is well
established that extensive disruption of the pelvis is
associated with high rates of mortality and late morbidity (1,
2). According to Tiles classification (3, 4)
the characteristic of completely unstable pelvic ring injury is
complete disruption of the posterior sacroiliac complex
associated with an anterior pelvic ring injury. The posterior
lesion may be a displaced fracture of the sacrum or ilium, a
dislocation through the sacroiliac joint, or a combination of
fracture and dislocation injuries. This lesion renders the
pelvis unstable in all planes. Vertical instability refers to
disruption of the anterior and posterior pelvic ring allowing
potential displacement posteriorly, superiorly, and in the
sagittal plane rotation (flexion), in addition to rotation in
the horizontal plane (internal or external rotation).
In
recent years efforts have been made to improve the results by a
more interventional approach. There is now increased interest in
the use of internal fixation of the posterior disruption (5,
6). There are a variety of methods available, including
iliosacral screws, sacral bars, and anterior and posterior
plating techniques. The benefits of fixation remain to be
clearly established and the optimal methods of fixation,
particularly for sacroiliac dislocations and sacral fractures,
are still a source of controversy. Iliosacral
screw fixation has been popularized by Routt (7, 8).
These screws may be used for both sacroiliac joint dislocations
and sacral fractures and can be placed percutaneously if a
satisfactory closed reduction can be obtained.
The
aim of this study was to evaluate the effectiveness of closed
reduction and percutaneous iliosacral screw fixation in
sacroiliac injuries and to assess the functional outcome of
these patients.
Material and Methods :
Patient
population: Thirty-six pelvic fractures were included in
this study. All patients were treated in the author's
institution, a level I trauma center, over a five-year period
from January 2002 to December 2006. There were nineteen males
and seventeen females with a mean age of thirty-one years (range
15 to 60 years). Motor vehicle accidents accounted for
twenty-four cases. Of the remaining twelve injuries, two were
crushing injuries after train accidents and ten were the result
of a fall from a height.
Inclusion
criteria: According to Tile's classification, (3, 4)
thirty six patients with vertically unstable type-C pelvic
disruptions (Figure 1) were included in this study, when the
posterior lesion was either sacroiliac dislocation (C1.2) or
sacral fracture (C1.3). Pelvic fractures with posterior
disruption through the iliac bone (C1.1) were excluded.
Pre-operative
Assessment: Prior to operative treatment, all patients were
evaluated clinically and radiographically with standard
anteroposterior, inlet, and outlet views of the pelvis. This was
augmented with a computed tomography scan of the pelvis in all
patients.
Fracture
classifications: The posterior injury was pure sacroiliac
dislocation in seventeen patients, sacroiliac fracture
dislocation in seven and sacral fracture in twelve. According to
the classification proposed by Denis et al. (9),
there were seven Zone I trans-alar sacral fractures and five
Zone II trans-foraminal fractures. The anterior lesion was pure
symphyseal disruption in twelve patients, ipsilateral fracture
of superior and inferior pubic rami in fifteen patients,
bilateral fracture of pubic rami in two patients, and combined
fracture of pubic rami and symphyseal disruption in seven
patients. Two of the pelvic fractures were open.
Perineal tear was associated in two patients.
Neurological
assessment: Six patients (17%) had a preoperative sacral
nerve root or lumbosacral plexus lesion. All were reported in
patients with sacral fractures. Thus, the incidence of nerve
injury was (50%) in this group of twelve patients with sacral
fractures. In four patients the lesion consisted of pain in an
S1 to S3 distribution and impairment of sensation with no
significant motor loss. In one patient there was motor weakness
of plantar flexion and knee flexion. The final patient had a
complete lumbosacral plexus injury of the injured side.
Associated
injuries: In thirteen patients the pelvis was the only
injury; the remaining twenty three patients had multiple
injuries. The median injury severity score was 25 (range 16 to
54). Four of these patients had a laparotomy to
deal with intraperitoneal sources of blood loss before
definitive orthopaedic fixation. One of them was associated with
traumatic intrauterine foetal death that needed hysterotomy. Six
patients had urological injuries in the form of ruptured bladder
in two patients and urethral injury in four. Two patients
suffered chest injuries with multiple rib fractures and
pulmonary contusion. Ten patients had associated skeletal
injuries in the form of long bone fractures in six, crushed hand
in one, contralateral pelvic ring fracture in two and
ipsilateral acetabular fracture in one. Head injury was reported
in one patient.
Time
of surgery: Fixation of the pelvic fracture was performed
within the first week after injury in all patients.
Surgical
technique: Closed reduction and percutaneous iliosacral
screw fixation of the posterior element of the injury was
performed with the patient positioned prone on the radiolucent
operating table. Single C-arm fluoroscopic
guidance for check of reduction and placement of cannulated
screws was used in all patients. The operative procedure
included the following steps:
1.
Closed reduction of the fracture: Under fluoroscopy control
in alternating anteroposterior, inlet and outlet projections to
correct the three dimensional displacement of the hemipelvis. It
included 3 steps: 1) Longitudinal traction to correct the
vertical migration, 2) Forward push of the hemiplevis to correct
the posterior displacement, and 3) Internal or external rotation
to correct external or internal rotation of the hemipelvis.
2.
Insertion of guide wires: Location of the starting point was
first done under fluoroscopic guidance targeting S1 segment,
followed by insertion of the guide wires under sequential
anteroposterior, inlet, and outlet fluoroscopic views to pass
perpendicular to the sacroiliac joint following S1 mass into the
body of S1 (Figure 2). The sequential fluoroscopic guidance in
the three views is mandatory during insertion of guide wires to
avoid mal-placement and surgical risks such as neurological or
vascular injury. The anatomical landmarks or S1 boundaries
should be identified under fluoroscopy. These are S1 foramen
inferiorly and L5-S1 intervertebral disc superiorly that are
best identified in outlet view. Neural canal posteriorly and
anterior cortex of S1 segment anteriorly are best viewed in the
inlet projection.
3.
Insertion of screws: Cannulated 7mm lag screws are inserted
after drilling over the guide wires under fluoroscopy to check
the final screw position and length (Figure 3).
A
total of eighty-two screws were used. Two screws were used in
twenty-six cases, and three screws in the remaining ten cases.
Fixation
of the anterior lesion: In
all cases the anterior lesion was usually addressed first. The
patients can be sorted into three groups according to fixation
of the anterior lesion.
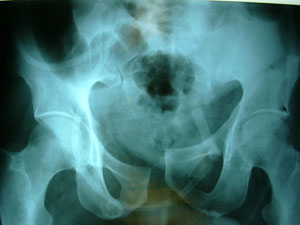
Figure
1. shows disruption of the pelvic ring in vertically
unstable Tile's type-C fracture pelvis.
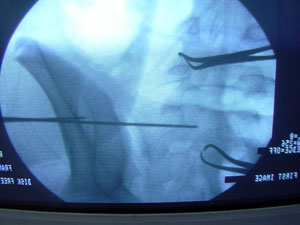
Figure
2. shows insertion of guide wires under fluoroscopic
guidance perpendicular to the sacroiliac joint into S1 body
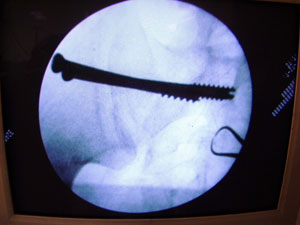
Figure
3. shows final check of position and length of inserted
iliosacral lag screws.
Group
A: Internal fixation group
Anterior
plate fixation was done in cases with pure symphyseal
disruption. Anterior plating was done before iliosacral screw
fixation because this facilitates closed reduction of the
posterior lesion. It was performed through a Pfannenstiel
incision, using narrow four-hole DCP plates. Internal fixation
with plating was done in nine cases. Single plate fixation was
used in seven patients and double plates in two (Figure 4 A-C).
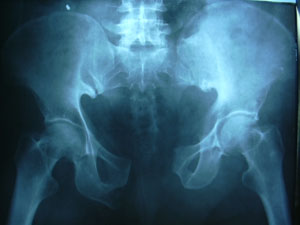
Preoperative
Radiograph
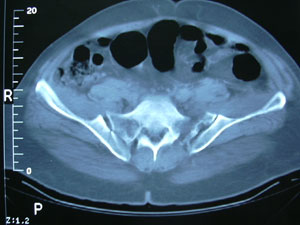
CT
scan of the posterior pelvis which reveals sacroiliac disruption
bilaterally
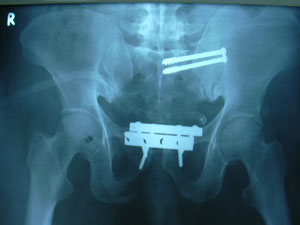
Postoperative
radiograph showing anatomic restoration of the pelvic ring with
anterior symphyseal plate fixation and posterior percutaneous
iliosacral lag screws.
Group
B: External fixation group
In
the present series, external fixation was used in two cases, one
with open pelvic fracture and extensive soft tissue injury, and
the second had disruption of the contralateral pelvic ring
through pubic rami anteriorly and the iliac bone posteriorly.
The general condition of the patient did not allow extensive
surgery using an extended ilioinguinal approach to fix the
anterior lesion bilaterally. In the two cases where external
fixation was used, the iliosacral screws were placed first
because the external fixation frame makes patient's positioning
and imaging of the sacroiliac region more difficult. The
external fixation consisted of a simple anterior trapezoidal
frame taking purchase from the strong supra-acetabular bone by
introducing the pins through the anterior inferior iliac spine.
Group
C: No fixation group
Twenty
five patients had no fixation of the anterior lesion, as the
anterior lesion consisted of minimally displaced pubic rami
fractures after reduction and fixation of the posterior lesion
in twenty four patients, and a minimally displaced symphyseal
disruption with a leaking supra-pubic tube preventing anterior
fixation in one patient.
Postoperative
care: Patients were allowed to mobilize and start
weight-bearing on the unaffected side with touch weight-bearing
on the affected side. Patients with bilateral lesions were kept
non-weight-bearing for a period of at least six weeks. External
fixators were removed six weeks post-injury. Initial data
regarding clinical results and complications were recorded for
all patients. Reduction was graded
according to the method of Tornetta and Matta (10)
(excellent: </= 4 mm of residual
displacement; good: 4-10 mm; fair: 10-20 mm; poor: > 20 mm).
Follow-up:
After discharge, the patients were reviewed clinically and
radiologically. These patients were asked to report persistent
pelvic pain. Clinically a neurological assessment was made of
lower limb motor and sensory function. Any apparent leg length
discrepancy was measured. Inlet-outlet and anteroposterior
pelvic views were taken. Reductions
with residual displacement in excess of one centimeter in any
plane were taken to represent a malunion.
Results :
The
mean period of follow-up was twenty one months (range 6 to 48
months). One multiply injured patient died during follow up.
Reduction
of the posterior injury: According
to Tornetta and Matta reduction was excellent in
twenty-two patients (61%), good in ten (28%) and fair in four
(11%) at the initial operative procedure. The posterior lesion
in the four patients with fair reduction was two sacroiliac
dislocations, one fracture dislocation sacroiliac joint and one
Denis type-II fracture sacrum. The anterior lesion in these
patients was associated symphyseal disruption and pubic rami
fractures in two, pure symphyseal disruption in one and pubic
rami fracture in one.
Re-displacement
of the posterior injury: Over the course of the following
two months, a gradual loss of reduction was noted in three
patients (8%), two with sacral fractures and one with sacroiliac
joint dislocation.
Therefore,
radiographs following fracture union showed malunion (more than
one centimeter displacement) in seven patients (19%). All
patients of malunion group were treated without anterior
internal fixation. In one patient, external fixator was used
anteriorly and the deformity recurred while the frame was still
in situ. The other six patients were left without any anterior
fixation. None of patients in whom the anterior lesion was
plated sustained a malunion.
Malunion
was noted in three out of twelve (25%) sacral fractures, three
out of seventeen (18%) sacroiliac dislocations, and one of seven
(14%) fracture dislocations of the sacroiliac joint. The extent
of final malunion varied from 1.5 to 2.5 centimeters (mean 1.8
centimeters).
Screw
placement: Screw misplacement occurred in four patients
(11%). Three patients had screws violating the anterior cortex
and protruding through the anterior aspect of the sacrum. One
patient had a screw with protruded threads into S1 foramen. This
was not detected during fluoroscopic placement and was only
apparent on postoperative radiographs. No new neurological or
vascular injuries were observed in spite of these errors.
Infection:
Infection occurred once after percutaneous iliosacral screw
fixation in an immune compromised multiply injured patient with
intra-peritoneal haemorrhage and traumatic intrauterine foetal
death. Pin tract infection of external fixator pins complicated
the two cases where frames were used.
Infection subsided after hardware removal.
Functional
outcome: The functional
outcome of one patient, who died during follow up, was excluded
from the results. All other patients regained full weight
bearing during follow up. Time to full weight bearing varied
according to associated other skeletal injuries with average 12
weeks. The patient with associated complete lumbosacral plexus
injury became brace user.
Four
patients reported erectile dysfunction that remained till last
follow up.
Nineteen
(54%) patients regained pain free gait. Twelve (35%) patients
reported occasional pain that did not affect the patient's daily
activity. Four (11%) patients reported persistent pain. The
first patient was multiply injured patient who had associated
sacral roots injury with ipsilateral fracture acetabulum and
contralateral pelvic ring disruption. The second had associated
ipsilateral complete lumbosacral plexus injury. The third was a
female patient who had open fracture of the pelvis with
extensive perineal tear and severe soft tissue injury that
needed several surgeries for repair and reconstruction of her
soft tissue trauma. The last patient had persistent pain that
was explained by an associated spondylolysis of the fifth lumbar
vertebra.
Discussion :
Unstable
pelvic injuries have been associated with high rates of
morbidity and mortality (11).
There has been increasing interest in the role of
internal fixation in the management of these injuries (12).
A number of reports have suggested that mortality and long-term
functional results can be improved by a more interventional
operative protocol (13, 14). In many cases the
anterior fracture can be stabilized by plating, which is the
method of choice in cases where it is technically feasible. The
selection of fixation method for the posterior lesion is more
controversial. Sacral bars have the advantage
of simplicity and relative safety. They are also versatile and
can be used for sacroiliac joint dislocations, for sacral
fractures, and in patients with bilateral posterior lesions.
However, judging the quality of the reduction is difficult and
there is a risk of over-compression with nerve injury when a
sacral fracture is present. In addition, the ends of the bars
are often prominent and a source of discomfort to the patient (15).
More direct methods of reduction and fixation include techniques
of anterior and posterior plating. Anterior plate fixation of a
sacroiliac dislocation is a useful technique. Simultaneous
exposure of the anterior lesion is possible and the quality of
reduction is therefore easier to assess. However, access to the
sacral side is limited and injury to the L5 nerve root is a
definite risk. Anterior plating is not feasible for sacral
fractures because the medial access is too limited. Posterior
approaches have been advocated, particularly for sacral
fractures. Pohlemann et al. (2) have shown
biomechanically that local osteosynthesis with specially
designed plates is comparable to the fixation achieved with
sacral bars. Mears et al. (1) have suggested the use
of a double cobra plate to deal with complex bilateral posterior
lesions. Iliosacral screw fixation is a
well-recognized technique for treating the posterior lesion (7).
Iliosacral screws may be used for both sacral fractures and
sacroiliac joint dislocations. Fixation has most commonly been
carried out using an open posterior approach. Some authors have
noted a high complication rate in association with posterior
pelvic wounds. The major disadvantage
of the posterior approach is the risk of impaired wound healing
and subsequent infection with a combined incidence reported as
high as 25% in one series (15). More recently
the use of percutaneous placement has been described (7).
This method has particular advantages in the multiply
traumatized patient and in patients with hemodynamic instability
where it is desired to minimize blood loss (7).
However, an adequate closed reduction must be obtained prior to
screw placement.
Closed
reduction and percutaneous fixation
Routt
et al. (8) reported on the use of percutaneous
iliosacral screws in sixty-eight pelvic fractures, of which
forty-three were Type C injuries. Closed reduction of the
posterior lesion was possible in fifty-one cases. Mal-reduction
occurred in twelve (18%) and failure of fixation in a further
three cases.
In
this study, excellent and good reduction of fracture was
achieved in 89%. Loss of reduction occurred in three patients
(8%). The overall
malunion rate was 19%.
Screw
misplacement
Some
concern has been expressed about the safety of the technique,
and with screw misplacement there are undoubtedly significant
risks to the cauda equina and the L5 and S1 nerve roots in
particular. The need for high-quality fluoroscopic imaging and
technical expertise has been emphasized if the technique is to
be used safely (7, 8). Bony anatomical variations are
common in this region, and the importance of the lateral view of
the sacrum to show the alar slope is now well recognized (3).
The
potential for screw misplacement is demonstrated in the present
study. Fortunately, the degree of error was small, only in four
occasions (11%), and no vascular or neurological complications
occurred.
Functional
outcome
As
might be expected, the functional outcome following these severe
injuries may be poor in a high percentage of patients. Late pain
in the region of the sacroiliac joint is a well-recognized
problem, even in cases where the reduction is satisfactory (6).
In
the present series many patients had pain at the time of
follow-up but it was severe in only four patients (11%). These
four patients have associated injuries or other reasons that
account for this persistent pain.
The
present series includes a comparatively large number of
vertically unstable injuries. When they are subdivided with
respect to the posterior and anterior lesions, this makes firm
conclusions difficult to draw. It seems clear, however, that
these injuries have a marked tendency to re-displace. It is a
trend that was most notable in fractures where no anterior
fixation was applied. In retrospect, anterior plate fixation
would have been advisable in these cases. The use of external
fixation may reduce the malunion rate, but the lowest rate was
found in patients with plate fixation of the anterior pelvis.
Although the numbers studied were not large enough to achieve
statistical significance, the trend suggests that more rigid
anterior fixation yields superior anatomical results.
Conclusion:
We believe that
early stabilization of the vertically unstable pelvis is
valuable in terms of reducing morbidity and improving long-term
functional outcome. Closed reduction and percutaneous iliosacral
screws are very useful for dealing with the posterior lesion
with minimum morbidity. However, our results suggest that for
optimum anatomic results, rigid internal fixation of the
anterior lesion is required.
Reference :
1.
Mears DC, Capita CP, Deleeuw H. Posterior pelvic disruptions
managed by the use of the double cobra plate. AAOS Instruct
Course Lect 1988; 37: 143-150.
2.
Pohlemann T, Angst M, Schneider E, Ganz R, Tscherne H. Fixation
of transforaminal sacrum fractures: a biomechanical study. J
Orthop Trauma 1993; 7: 107-117.
3.
Tile M. Classification. In: Tile M, ed. Fractures of the Pelvis
and Acetabulum. Media, PA: Williams & Wilkins, 1995. p.
66101.
4. Tile M. Acute pelvic
fractures: I. causation and classification. J Am Acad Orthop
Surg. 1996; 4: 143151.
5.
Leighton R, Waddell J. Open reduction and internal fixation of
vertical fractures of the pelvis using the sacroiliac joint
plate. J Orthop Trauma 1991; 5: 255-258.
6.
Matta JM, Saucedo T. Internal fixation of pelvic ring fractures.
Clin Orthop 1989; 242: 83-97.
7.
Routt ML Jr, Meir MC, Kregor PK, Mayo KM. Percutaneous
iliosacral screws with the patient supine technique. Operat Tech
Orthop 1993; 3: 35-45.
8.
Routt MLC, Kregor PJ, Simonian PT, Mayo KA. Early results of
percutaneous iliosacral screws placed with the patient in the
supine position. J Orthop Trauma 1995; 9: 207-214.
9.
Denis F, Davis S, Comfort T. Sacral fractures: an important
problem. Retrospective analysis of 236 cases. Clin Orthop 1988;
227: 67-81.
10. Tornetta III P, Matta JM: Long term follow-up of operatively treated
unstable posterior pelvic ring disruptions. Orthop Trans 1995;
19: 161.
11.
McMurtry R, Walton D, Dickinson D, et al. Pelvic disruption in
the polytraumatised patient: a management protocol. Clin Orthop
1980; 151: 22-30.
12.
Burgess AR, Eastridge BJ, Young JWR, et al. Pelvic ring
disruptions: effective classification system and treatment
protocols. J Trauma 1990; 30: 848-856.
13.
Gruen GS, Leit ME, Gruen RJ, Peitzman AB. The acute management
of haemodynamically unstable multiple trauma patients with
pelvic ring fractures. J Trauma 1994; 36: 706-711.
14.
Leenen LPH, van der Werken C, Schoots F, Goris RJA. Internal
fixation of open unstable pelvic fractures. J Trauma 1993; 35:
220-225.
15.
Kellam JF, McMurtry RY, Paley D, Tile M. The unstable pelvic
fracture. Operative treatment. Orthop Clin North Am 1987; 18:
25-41.
|








