|
Abstract:
OBJECTIVES:
Percutaneous vertebral augmentation has improved the quality of
life in patients with osteoporotic vertebral fractures. Our
objective is to review 19 patients with these interventions and
to analyze the obtained improvement.
PATIENTS AND METHODS:
Retrospective study on 10 kyphoplasties, 9 vertebroplasties, 6
men, 13 women, 78.9% in the thoracolumbar junction, Genant grade
I (42.1%), posterior wall involvement (21.1%), cement leakage
(31.6%). We analyzed the Oswestry test, the vertebral and
regional kyphosis, Cobb angle, vertebral collapse, visual
analogue scale of the pain (VAS), among others.
RESULTS:
With kyphoplasty we obtained a correction of the vertebral
kyphosis (p=0.024) and with vertebroplasty a correction of the
collapse (p=0.014), both statistically significant. Significant
differences did not appear in the Oswestry test between both
techniques, although there was a global improvement. The time of
intervention was greater in kyphoplasties (100 +/- 44.53
minutes), as was the time of radiation (5.70 +/- 1.33 minutes)
and the price (4,026.40 +/- 1,016.14 euros). The reduction of
the pain (VAS) was better for kyphoplasties (9.70 +/- 1.76 to
3.50 +/- 1.84 points).
CONCLUSIONS: In
our experience and despite its greater cost and greater
radiation dose kyphoplasty provides a greater correction of the
kyphosis and the pain than vertebroplasty.
Key words:
vertebroplasty, kyphoplasty, Oswestry
J.Orthopaedics 2007;4(4)e13
index.htm
Introduction:
Percutaneous
vertebral augmentation is a procedure that has allowed an
improvement in the quality of life in patients with osteoporotic
vertebral fractures. Solely in the United States 1.5 million
osteoporotic fractures per year were described in 2004, of which
700,000 were seated at the vertebral level1. Due to the elevated
frequency of this pathology and to its growing increase,
techniques were developed to correct these vertebral fractures
in a less invasive or percutaneous way. In the decade of the
80s Galibert2developed the first vertebroplasty to treat a
haemangioma of the C2 vertebra. In 1989, Lapras applied this
technique to the treatment of vertebral fractures, with
encouraging results. On the other hand from the decade of the
90s, authors such as Reiley3, developed a technique that
combined the classic percutaneous augmentation of vertebroplasty
with a previous raising of the vertebral collapse by means of an
expansion balloon, thus arising kyphoplasty giving a greater
correction of the height and the vertebral kyphosis.
Our objective is to review the interventions in 19 patients in
our centre between 2004 and 2005 for vertebral fractures and 1
haemangioma, by means of vertebroplasty and kyphoplasty,
analyzing the clinical, radiological and functional recovery
reached by these patients.
Material and Methods :
A retrospective
descriptive study on a group of 19 patients, of whom 6 were men
(31.6%) and 13 women (68.4%) with an average age of 59.05 years,
and a standard deviation of 12.80 years with a minimum of 33
years and maximum of 81 years, which had undergone 10
kyphoplasties (52.6%) and 9 vertebroplasties (47.4%). We
analyzed:
Personal data: name, history number, sex, technique, life
previous to the intervention.
Characteristic clinical histories prior to the intervention:
Lasegues sign, mobility, sensitivity, reflexes, sphincters
etc., and after the intervention:-
Fracture location, region, cause, osteoporotic, time of
evolution, Genant grade, type, Computerized Axial Tomography
(CAT), Nuclear Magnetic Resonance (NMR), consideration of the
involvement of the posterior wall and/or the medullary canal.
Preoperative and postoperative days, time from the
intervention to walking, time in the operating room, type of
anaesthesia, radiation, costs, and complications.
Vertebral and regional Kyphosis, Cobb angle, vertebral
collapse.
Visual analogue scale of the pain (VAS) before and after.
Need for analgesics and type used.
OPTQoL (Osteoporosis Targeted Quality of Life Questionnaire)4.
Oswestry test.
The statistical methodology applied differed according to 2
aspects. Descriptive analysis. In the first place, a global
exploration of the data was made to identify extreme values and
to characterize differences between sub-groups of cases. The
numerical variables were expressed with means and standard
deviations or, if the distributions were asymmetric with medians
and percentiles (P25-P75), and the qualitative variables with
tables of frequencies and percentages. Inferential analysis. In
order to evaluate the global mean differences between
quantitative variables before and after the intervention, the
Student t-Test for paired samples or the Wilcoxon nonparametric
signed-rank test was used. In order to compare the mean values
of quantitative variables the Student t-Test for independent
samples or the Mann-Whitney nonparametric test was applied. When
significant differences were detected they were quantified by
determining confidence intervals for mean differences to 95%. In
order to study the relationship between qualitative variables,
the Chi-square test with continuity correction or Fishers exact
test (for poorly populated 2x2 tables) was applied. In order to
detect changes in the before and after answers due to the
experimental intervention, the marginal homogeneity test, a
nonparametric test for two related ordinal variables, was used.
This test is an extension of the McNemar test for multivariate
binary responses. Also, the McNemar nonparametric test was
applied with the same objective for two related dichotomizing
variables.
The analysis of the data was made with SPSS 13.5 for Windows
program.
Results :
78.9% of our patients presented an active previous life, whereas
21.1% referred to a sedentary previous life. Mobility,
sensitivity and reflexes were preserved in 100% of the cases. A
sphincter involvement of 5.3% was notable for fractures where an
invasion of the medullary canal took place, in spite of this,
the remaining 94.7% remained within normality in this respect.
The most frequent fractures were those of T12 and L1, with a
31.6% frequency in each one, followed by those of L2 or L3 at
10.5% in each. A fracture of L1 was associated to another
fracture in 2 cases and that of L2 in 1 case.
The thoracolumbar junction T11-L2 was involved in 78.9% of the
cases, followed by the lower lumbar (L3-L5) in 15.8% of the
cases, and with the thoracic (T1-T10) in 5.3% of the cases.
The causal agent was minimal trauma in 73.7% of the cases,
emphasizing osteoporosis as the suspected cause in 68.4% of the
cases.
With regard to the classification according to the type of
fracture, we found a predominance of type I of the Genant
classification, that is, with a collapse between 20-25%, in
42.1% of the cases, nevertheless, in types II or III the
percentage went up to around 36.8% or 21.1% respectively. The
fractures in wedge formation predominated in 52.6% of the cases,
followed by the biconcave in 31.6% and those produced by
crushing in the remaining 15.8%.
NMR was needed in 18 cases (94.7%), with an involvement of the
posterior wall in 21.1%, with repercussion on the rachidian
canal in 10.5%. Nevertheless, tests such as CAT were also needed
in 7 cases, 36.8%, where an involvement of the posterior wall
was also shown in 21.1%, but with this test the involvement of
the rachidian canal was only demonstrable in 5.3%. All this
leads us to consider that a more sensitive diagnosis of invasion
of the rachidian canal would be achieved with NMR rather than
with CAT, at least in our series.
With regard to the date of the intervention, 42.1% were
performed between 2 months and one year (chronic-early mode), as
opposed to the sub-acute ones between 2 weeks and 2 months in
26.3%, the acute ones less than 2 weeks in 21.1% and the
chronic-delayed ones more than a year in the remaining 10.5%.
Regarding the OPTQoL and other data related to the quality of
life prior to the intervention, we observed that 68.4% of our
patients were bed-ridden, 21.1% had a bed-armchair life and
10.5% considered their life as limited by the pain. Basic daily
activities were shown to be disabled in 78.9% because of the
pain and 21.1% were recognized as being able but with severe
pain. Some 47.4% took non-steroidal anti-inflammatory drugs (NSAIDS),
42.1% took NSAIDS and tramadol and 5.3% used morphine patches.
Muscular relaxants were taken by 63.2% of our patients. Some
89.5% referred to a lot of difficulty for their physiological
necessities and 10.5% of our patients noted moderate difficulty.
94.7% indicated that they had enormous difficulty in attempting
to pick up an object. Up to 89.5% of our patients considered
themselves housebound by the pain. 89.5% were very scared of
falling, with 5.3% quite scared. Some 47.4% of our patients
perceived losses of height, including 42.1% who perceived humps.
The psychological repercussion of these deformities led to 15.8%
needing to hide these changes. 15.8% had undergone previous
fractures. In 94.7% of the cases they recognized their quality
of life as bad. 42.15% recognized having members in their family
with osteoporosis. 78.9% never consulted for osteoporosis.
Finally, up to 94.7% had never had any bone densitometry (BDM),
nor received preventive treatment before their fracture, a
finding which illustrates the need to initiate a preventive
treatment of osteoporosis in postmenopausal patients.
However, after the intervention 0% were bed-ridden and 10.5%
referred to a bed-armchair life, which suggests a great
improvement in the quality of life. 26.3% recognized a life
limited by the pain and finally, in 47.4% and 15.8% they
described a normal life with/without pain. 0% were disabled by
the pain after the intervention for their basic daily
activities, whereas 15.8% were able, but with severe pain.
Postoperatively 21.1% continued taking NSAIDS, 10.5% NSAIDS and
tramadol, 5.3% morphine patches and pregabalin or gabapentin was
prescribed in 10.5%. Often these pains had a neuropathic
component associated with spondyloarthrosis and lumbar sciatica
present at the moment of the fracture. The cases in which there
were cement leakages (31.6%), and especially in the cases which
were symptomatic (5.3% of the cases), also required
postoperative sedatives. 31.6% took muscular relaxants after the
intervention. Only 10.5% referred to great difficulty performing
their physiological necessities, 31.6% referred to moderate
difficulty and up to 47.4% denied having problems on the matter.
21.1% described having enormous difficulty trying to pick up
object, as opposed to 15.8% who did not refer to any difficulty.
After the intervention only 5.3% recognized that they were
housebound due to the pain. Finally the quality of life after
the intervention was bad in 5.3% of the cases, fair in 52.6% and
good in 42.1% of the cases. All this leads to the consideration
of how the techniques of percutaneous vertebral augmentation in
our centre have been able to improve the quality of life of our
patients.
The mean pre-intervention VAS changed from 9.79 points with a
standard deviation of 1.273 points, to a mean post-intervention
VAS of 4.68 points with a standard deviation of 2.286 points. It
entailed a statistically significant difference, with p=0.0,
with concrete lower and upper limits (3.90;6.30). Nevertheless,
we did not find statistically significant differences between
kyphoplasty and vertebroplasty with regard to the reduction of
VAS. What is worthy of mention was the change of the mean
pre-intervention VAS of 9.70 points with a standard deviation of
1.76, to a mean post-intervention VAS of 3.50 points with
standard deviation of 1.84 points for the kyphoplasty in our
series, which showed a better improvement of the VAS with this
technique than with vertebroplasty which gave a change of the
mean pre-intervention VAS from 9.89 points with a standard
deviation of 0.33 points, to a mean post-intervention VAS of 6
points with a standard deviation of 2.06 points. This smaller
reduction of the VAS after vertebroplasty with respect to
kyphoplasty in our series may explain that 100% of the patients
submitted to kyphoplasty would recommend this procedure to other
patients, as opposed to only 66.7% that would recommend
vertebroplasty after having this intervention.
At the global level, 84.2% acknowledged that they would have the
operation again, as opposed to 15.8% that would not have it
again. Also the quality of life referred to by the patients was
better after the kyphoplasty interventions: being good in 60%,
as opposed to vertebroplasties where the final quality of life
was good in 22.2%, and bad in 11.1%. There is the possibility of
an error factor in that the age of the patients submitted to
kyphoplasty was less (mean of 52.80 years with a standard
deviation of 11.16 years) than that of those submitted to
vertebroplasty, (mean of 68 years with a standard deviation of
11.20 years), as a conditioner of these last results.
As far as the surgical procedure the degree of anaesthetic risk
conditioned a predominance of ASA II in 52.6%. The most used
anaesthetic procedure was local anaesthesia with sedation in
89.5%, although general anaesthesia was required in 10.6%.
We evaluated the vertebral kyphosis, the Cobb angle, the
regional kyphosis and the percentage of vertebral collapse5
prior to, and after, the operation.
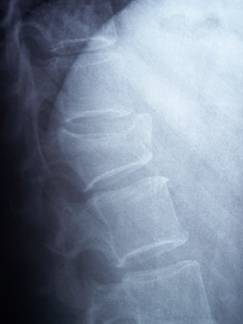
Fig. 1. Vertebral
fracture with involvement of the anterior wall.
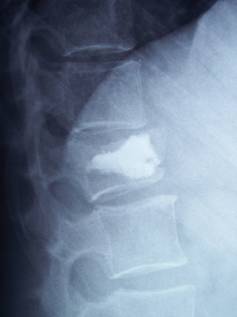
Fig. 2. Kyphoplasty.
Correction of vertebral collapse and kyphosis.
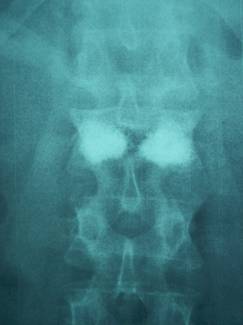
Fig. 3. Transpedicular
introduction of PMMA. Kyphoplasty.
We found a statistically
significant difference in the correction of the vertebral
kyphosis for kyphoplasties with a p=0.024 (1.35;11.54) and there
was also a statistically significant difference for the
correction of the vertebral collapse for vertebroplasties with a
p=0.014 (3.50;21.87). (See tables 1 and 2). (See figures 5 and
6.) Although both techniques corrected both values, in our
series the statistically significant differences were centred in
the results given above.
We found differences in
the time of radiation, the time of intervention and the price,
all these parameters being greater for kyphoplasties.
|
Comparative table |
Kyphoplasty |
Vertebroplasty |
|
Vertebral kyphosis correction |
15º |
7,87º |
|
Cobbs angle correction |
11º |
5,12º |
|
Regional kyphosis correction |
15,2º |
7,62º |
|
Preoperatory days |
3,4 days |
1,56 days |
|
Postoperatory days |
1,20 days |
1,33 days |
|
Time to walk (days) |
1,20 days |
1 days |
|
Radiation time |
5,70 minutes |
4,55 minutes |
|
Surgical time |
100 minutes |
80.56 minutes |
|
Costs |
4026,40 Euros |
1436,67 Euros |
Table. 1. Comparative
table between both techniques. We can observe differences on
costs, radiation time and surgical time.
With regard to the
Oswestry test, differences were found in the results before and
after the application of the surgical technique. In fact mean
pre-intervention values changed from 92.27 points with a
standard deviation of 6.16 points to mean post-intervention
values of 43.08 points with a standard deviation of 22.19
points. Which would determine that a statistically significant
difference existed, p= (0.00), (33.75-60.62), after the
application of both techniques in the quality of life
information gathered in the Oswestry test. Nevertheless,
significant differences were not found in the results of this
test when comparing both techniques, within our series.
Finally, we found some
complications such as, persistent kyphotic attitude with
continued pain after the treatment in 5.3%, cement leakage in
31.6% (6 cases), symptomatic in 5.3% (persistent pain) and
persistence of the pain without cement leakage in 31.7%. We did
not find serious complications such as the pulmonary embolisms
described in the bibliography. We considered that a cement
leakage had taken place when it was indicated in the clinical
history by the surgeon who had made the intervention previously.
Discussion:
When injected at the vertebral level
polymethylmethacrylate, PMMA, allows a reinforcement of the
vertebral body to develop, avoiding the forces of micromovement,
compression and deformation, conferring a greater strength for
the support of loads and greater resistance to deformation by
compression, and causes an exothermic reaction that causes
damage in sensory endings, producing analgesia of the zone. Also
the curing process of PMMA causes the formation of toxic
monomers that damage the nociceptive endings. These thermal
and/or toxic effects cause anti tumour like cytotoxic effects.
In our series we evaluated its use both as a vertebral
reinforcement, and as an agent which can entail analgesia of the
zone by the said mechanisms. In our patients we did not
incorporate antibiotics to the PMMA, in fact, the administration
of gentamicin or tobramycin is known to be capable of reducing
the strength of the cement up to 24%5. Nevertheless, it has been
observed that it does have some clinical significance, which is
why some authors continue applying these techniques with these
antibiotics. Recently, the use of a new cement preparation for
the treatment of osteoporotic vertebral fractures has been
described, called SrHA (Strontium hydroxyapatite) it is a
bioactive bone cement containing strontium, taking 15-18 minutes
to cure, and reaching a polymerization temperature of up to 58º,
with a capacity to support compression stresses of up to 40.9
MPa and allowing stabilization, mineralization, the induction of
bone formation, as well as osteointegration6.
In our series we tried to follow criteria to indicate or to
contraindicate a technique of percutaneous vertebral
augmentation, in fact, and in relation to that found in the
bibliography7, we indicated it in the cases of pain associated
to osteoporotic vertebral fractures, benign tumour, such as
aggressive and/or painful haemangioma, even in malignant, and
Kümmels disease. Nevertheless, we did not indicate it in those
cases where risks of active infection at the vertebral level
existed, osteomyelitis type, diskitis, epidural abscess,
intracanalicular tumoural extension, disorders of coagulation
and/or compression fractures with deformity greater than 70%.
In general, it has been considered in the bibliography that
vertebroplasty has been able to reduce the morbidity, the time
of hospitalization and the care required after an osteoporotic
vertebral fracture 8;9. Also, kyphoplasty would have the
advantage over vertebroplasty in correcting the deformity of the
fractured vertebral body in a controlled manner10. In our
experience we have tried to compare both techniques and have
seen that our results correspond with these affirmations.
In our series we found that vertebroplasty as much as
kyphoplasty provided an improvement in the mean pre-intervention
VAS of 9.79 points with a standard deviation of 1.27 points, to
a mean post-intervention VAS of 4.68 points with a standard
deviation of 2.28 points. Nevertheless, the improvement reached
in VAS was better in kyphoplasties than in vertebroplasties when
obtaining a change from a mean pre-intervention VAS of 9.70
points with a standard deviation of 1.76 points, to a mean
post-intervention VAS of 3.50 points with a standard deviation
of 1.84 points, which would be over the post-intervention VAS
reached by vertebroplasty with a mean of 6 points. These results
are reinforced in the consulted bibliography, since Rhyne11, for
example, speaks of a change of a mean pre-intervention VAS of
9.16 points to a mean post-intervention VAS of 2.91 points after
the performance of kyphoplasties on 52 patients, whereas
McKiernan12 obtains a mean pre-intervention VAS of 7.7 points,
with a mean post-intervention VAS of 2.8 points after the
performance of 49 vertebroplasties; thus giving improvements of
6.25 points for kyphoplasties and 4.9 points for
vertebroplasties. In our series we did not find statistically
significant differences between both techniques regarding the
VAS results, in fact other authors like Pflugmacher13, recognize
that they have not found differences in VAS between 20 patients
with vertebroplasty and 22 with kyphoplasty.
Neither is a large amount of PMMA needed to obtain the desired
effect, thus, Guglielmi14 emphasizes a good functional recovery
after the injection of between 2 and 5 ml of intravertebral
cement, which would agree with our surgical technique. It must
be remembered that an excess of cement or pressure, could entail
the appearance of later leakages.
In our series we reached a statistically significant correction
of the vertebral kyphosis (p=0.024) (1.35;11.04), with the
kyphoplasties, from a mean of 15º with a standard deviation of
5º, to a post-intervention mean of 8.80º with a standard
deviation of 2.77º. All this agrees with that shown by Rhyne11,
with a correction of 3.4º with kyphoplasties (p<0.05). Also
other authors13note a greater correction of the vertebral
kyphosis with kyphoplasties with a p<0.05.
In our series we found a statistically significant correction of
the vertebral collapse, changing from a mean pre-intervention
vertebral collapse of 25.4% to a mean post-intervention 12.76%,
p=0.014, (3.50,21.87). This supposes a correction of 12.64º. In
the bibliography, we found restitutions of the prior vertebral
collapse of 30% and 50% at the mean vertebral level10, with
kyphoplasties correcting the vertebral collapse in 60% of the
acute fractures and in 26% of the chronic fractures15. Which is
in favour of kyphoplasty as it would be useful also for its
correction of the collapse, although better in the acute
fractures that in the chronic, in which cases it is more
difficult to correct this deformity. We shared this idea and
reserved this technique for acute cases rather than chronic. The
correction of the vertebral collapse was for us more
statistically significant in vertebroplasties than in
kyphoplasties. In a self-critical mode, our sample, of about 19
cases, is not very great and possibly with a greater sample a
statistically significant correction in the cases with
kyphoplasty would also be reached. We also emphasize the
measurement problems of these radiological parameters where
several observers are used, which may cause possible bias in
inter-observer individual variability. In our series the review
of the images was the responsibility of 3 different observers.
With regard to the collected data of the Oswestry scale, we
obtained an evolution from the pre-intervention mean of 92.27
points with a standard deviation of 6.16 points to a
post-intervention mean of 43.08 points with a standard deviation
of 22.19 points, which supposes an improvement of 49.19 points.
This difference is significant, not only statistically speaking,
with a p= (0.00), (33.75-60.62), but because according to
Fairbank16, the American Food and Drug Administration has chosen
a minimum difference of 15 points between the preoperative and
postoperative evaluations of the Oswestry questionnaire as an
indication of clinical change in patients undergoing spinal
fusion. Therefore, in our series the significant improvement of
these patients is stated, although we do not establish important
differences between both techniques with regard to the Oswestry
test. Pflugmacher13 finds significant differences between both
techniques with regards to the Oswestry test results.
Finally, as in all the series, we have also had complications.
Thus persistent kyphotic attitude with pain continuing after
treatment appeared in 5.3%, cement leakage (6 cases) in 31.6%
being symptomatic in 5.3% (with persistent pain) and the
persistence of pain without cement leakage in another 31.7%. For
authors like Evans17, who described a series of 488 patients
submitted to vertebroplasties, the rate of complications rose to
around 4.9% and it was considered that vertebroplasty is a safe
and effective technique. However, there are complication rates
in the bibliography, especially relating to the cement leakage,
that lead to the consideration of the risks of the intervention.
Thus, McKiernan12 notes a risk of leakage around 7.7%, Majd10,
locates it between 20 and 65% for vertebroplasties.
Nevertheless, Majd10 notes a risk of cement leakage of 10.6% for
kyphoplasties and Rhyne11 places it at 9.8%. All this would lead
to thinking that there is a greater leakage risk with
vertebroplasties than with kyphoplasties. In fact, in our series
we found 2 cases of cement leakage in the patients with
kyphoplasty and 4 cases in the patients with vertebroplasty.
Equally, a greater percentage of contiguous fractures have been
described in vertebroplasties than in kyphoplasties, thus
McKiernan12 notes a 6.5% risk after vertebroplasties, whereas
Gaitanis18 considers that this risk oscillates between 10-39%
for kyphoplasties and 12.4-52% for vertebroplasties. Other risks
described are hypotension, costal fractures, damage in the dura
mater, pulmonary embolisms, respiratory distress (ARDS),
cerebral cement embolisms, radicular compression after
intraforaminal cement leakage, paraplegia, cauda equine
syndrome, intracanal compression, toxicity, allergy or thermal
damage. Many of these effects could be explained by the multiple
vascular connections established in the vertebral column,
highlighting especially the internal and external vertebral
venous plexuses, and the basivertebral veins 1919. Venography
prior to vertebroplasty has been proposed with the intention of
reducing the risks of embolisms, but in our series it was not
necessary. In fact there are authors like Vasconcelos20, who
recognize that the performance of venography prior to
vertebroplasty is not necessary, since after 205
vertebroplasties only 3 (1.5%) complications appeared, such as
hypotension, hypoestesia in the puncture zone and proximal
radiculopathy, concluding that in none of the cases could it be
said that it had been caused by cement leakage. Vasconcelos
recommends vertebroplasty with a precise fluoroscopic control as
a better preventive measure.
Conclusion:
In our experience and despite its greater
cost, greater radiation dose and greater operating time,
kyphoplasty produces a greater, statistically significant
(p=0.024), correction of kyphosis, and of the pain than
vertebroplasty. With vertebroplasty we reached a statistically
significant correction of vertebral collapse (p=0.014). We
reached a global improvement in the Oswestry test with both
techniques, p=(0.00) (33.75-60.62), although without
statistically significant differences between them.
Reference :
1. Riggs BL, Melton LJ 3rd. The
worldwide problem of osteoporosis: insights afforded by
epidemiology. Bone.1995 Nov;17(5 Suppl):505S-511S.
2. Galibert P, Deramond H, Rosat P,
Le Gars D. [Preliminary note on the treatment of vertebral
angioma by percutaneous acrylic vertebroplasty].
Neurochirurgie.1987;33(2):166-8.
3. Garfin SR, Yuan HA, Reiley MA. New
technologies in spine: kyphoplasty and vertebroplasty for the
treatment of painful osteoporotic compression fractures.
Spine.2001 Jul 15;26(14):1511-5.
4. Lydick E, Zimmerman SI, Yawn B,
Love B, Kleerekoper M, Ross P, et al. Development and validation
of a discriminative quality of life questionnaire for
osteoporosis (the OPTQoL). J Bone Miner Res.1997
Mar;12(3):456-63.
5. Amar AP, Larsen DW, Esnaashari N,
Albuquerque FC, Lavine SD, Teitelbaum GP. Percutaneous
transpedicular polymethylmethacrylate vertebroplasty for the
treatment of spinal compression fractures. Neurosurgery.2001
Nov;49(5):1105-14; discussion 1114-5.
6. Cheung KM, Lu WW, Luk KD, Wong CT,
Chan D, Shen JX, et al. Vertebroplasty by use of a
strontium-containing bioactive bone cement. Spine.2005 Sep
1;30(17 Suppl):S84-91.
7. Dixon RG, Mathis JM.
Vertebroplasty and kyphoplasty: rapid pain relief for vertebral
compression fractures. Curr Osteoporos Rep.2004 Dec;2(4):111-5.
8. Diamond TH, Champion B, Clark WA.
Management of acute osteoporotic vertebral fractures: a
nonrandomized trial comparing percutaneous vertebroplasty with
conservative therapy. Am J Med.2003 Mar;114(4):257-65.
9. Papaioannou A, Adachi JD,
Parkinson W, Stephenson G, Bedard M. Lengthy hospitalization
associated with vertebral fractures despite control for comorbid
conditions. Osteoporos Int.2001;12(10):870-4.
10. Majd ME, Farley S, Holt RT.
Preliminary outcomes and efficacy of the first 360 consecutive
kyphoplasties for the treatment of painful osteoporotic
vertebral compression fractures. Spine J.2005
May-Jun;5(3):244-55.
11. Rhyne A 3rd, Banit D, Laxer E, Odum
S, Nussman D. Kyphoplasty: report of eighty-two thoracolumbar
osteoporotic vertebral fractures. J Orthop Trauma.2004
May-Jun;18(5):294-9.
12. McKiernan F, Faciszewski T, Jensen
R. Quality of life following vertebroplasty. J Bone Joint Surg
Am.2004 Dec;86-A(12):2600-6.
13. Pflugmacher R, Kandziora F,
Schroder R, Schleicher P, Scholz M, Schnake K, et al. [Vertebroplasty
and kyphoplasty in osteoporotic fractures of vertebral bodies --
a prospective 1-year follow-up analysis]. Rofo.2005
Dec;177(12):1670-6.
14. Guglielmi G,
Andreula C, Muto M, Gilula LA.
Percutaneous vertebroplasty: indications, contraindications,
technique, and complications. Acta Radiol.2005
May;46(3):256-68.
15. Crandall D, Slaughter D, Hankins PJ,
Moore C, Jerman J. Acute versus chronic vertebral compression
fractures treated with kyphoplasty: early results. Spine J.2004
Jul-Aug;4(4):418-24.
16. Fairbank JC, Pynsent PB. The
Oswestry Disability Index. Spine.2000 Nov 15;25(22):2940-52;
discussion 2952.
17. Evans AJ, Jensen ME, Kip KE, DeNardo
AJ, Lawler GJ, Negin GA, et al. Vertebral compression fractures:
pain reduction and improvement in functional mobility after
percutaneous polymethylmethacrylate vertebroplasty retrospective
report of 245 cases. Radiology.2003 Feb;226(2):366-72.
18. Gaitanis IN, Hadjipavlou AG, Katonis
PG, Tzermiadianos MN, Pasku DS, Patwardhan AG. Balloon
kyphoplasty for the treatment of pathological vertebral
compressive fractures. Eur Spine J.2005 Apr;14(3):250-60.Epub
2004 Oct 8.
19. Groen RJ, du Toit DF, Phillips FM,
Hoogland PV, Kuizenga K Coppes MH, et al. Anatomical and
pathological considerations in percutaneous vertebroplasty and
kyphoplasty: a reappraisal of the vertebral venous system.
Spine.2004 Jul 1;29(13):1465-71.
20. Vasconcelos C, Gailloud P,
Beauchamp NJ, Heck DV, Murphy KJ. Is percutaneous
vertebroplasty without pretreatment venography safe? Evaluation
of 205 consecutives procedures. AJNR Am J Neuroradiol.2002
Jun-Jul;23(6):913-7.
|





