|
J.Orthopaedics 2007;4(4)e1
Introduction:
Clavicle fractures are common in young active
adults. They constitute 2.6% of all adult fractures [1] of
which 80% occur in the midshaft of the clavicle [2]. Fractures
of the middle third of the clavicle show a rotatory
posterosuperior angular displacement of the medial fragment
whereby the trapezuis muscle is penetrated and soft tissue
interposition prevents fragments from contaction each other.
Also, overlap in multiple fragment fractures results in a
shortening of the shoulder girdle at the fracture site which
leads to poor cosmetic and functional results [3]. In an Allman
I [4] fracture, the distal fragment is pulled distally and
medially due to the influence of the weight of the upper
extremity and the pectorals major muscle, while the proximal
fragment is elevated due to the force of the sternocleidomastoid.
The incidence of non-union in midclavicular
fractures is usually quoted as being 0.1-0.8% [5] with
non-operative treatment. More recent data, based on detailed
classification of fractures, suggest that the incidence of non
union in displaced midshaft clavicular fractures is between
10-15% especially in those with an initial shortening of >20 mm
[6]. This resulted in unsatisfactory patient outcome in 31% of
the study group treated with non operative treatment [7]. There
have been many papers published on treatment of established
malunion of clavicular fractures and their complications [8].
Previously this was described only as a cosmetic deformity.
Malunion with shortening and rotational deformity does not
remodel in adults. This can be debilitating for the patient and
challenging for the surgeon. Emphasis in literature has been
more on non union until Eskola [3] reported that patients with a
shortening of greater than 15 mm had statistically significantly
more pain. Recent papers have analysed the results of plating of
fresh clavicle fractures [9, 10].
The purpose of this
study was to compare the results of anterior versus superior
plating of freshly displaced clavicular fractures with an
initial shortening of >20mm
Material and Methods :
This is a non randomised retrospective study
from 2000-2004. Patients with an acute non-pathological fracture
of the midshaft of the clavicle treated surgically at Southend
District General Hospital were considered. Inclusion criteria
were (i) closed midshaft fracture (ii) Age between 16 to 65
years (iii) Shortening of more than 20 mm measured on initial
radiographs. Exclusion criteria were (i) floating shoulder (ii)
pathological fracture (iii) Unfit for general anaesthesia (iv)
Associated neurovascular injuries.
The choice of surface for plating the
clavicle was based on the surgeon operating. One of the authors
(GJP) preferred to place the reconstruction plates anteriorly.
The other consultants plated the clavicle superiorly.
The timing of the operation was 3.6 days post
injury on an average. It was performed under general anaesthesia
with patient in beach chair position. A longitudinal incision
along the superior border of the clavicle was made. Large
branches of the supraclavicular nerves were protected. The
fracture was plated with the aim of restoring the clavicular
length. Lag screw was used to fix large butterfly fragments.
Reconstruction plate was used to fix the fracture with the
intention of getting altleast 6 cortices on either side of
fracture. They were contoured to the three dimensional anatomy
of the clavicle. Post operatively, the limb was kept in a sling
and mobilised within pain limits. Patients were discharged by
the next day and were followed up at two weeks for wound check,
six weeks, three months and six months.
Continuous normally distributed data was
analysed using Chi-square test, T-test, Fishers exact test
using SPSS 10.0 software (SPSS Inc.Chicago Illinois, USA). P
value <0.05 was considered significant for the purpose of this
study.
Results :
Forty nine patients were included in the
study. There were 22 patients in the anterior group (Fig 1) and
27 in the superior group (Fig 2). The mean age in the anterior
group was 36.3 years (Range 17-64) and in the superior group was
37.6 years (Range 16-65). There were no demographic differences
in the two groups (Table 1). The follow up varied between six
months to 24 months. The outcomes were assessed based on
complications, Constant score and patient satisfaction
questionnaire.
Table 1- Demographic data
|
TABLE 1 |
|
|
|
Parameter |
Anterior group(N=22) |
Superior group(N=27) |
|
Male |
16 |
20 |
|
Female |
6 |
7 |
|
Mean age (yrs) |
36.3 |
37.6 |
|
Dominant Arm |
17/22 (77.3%) |
21/27 (77.7%) |
|
Mech of Injury |
|
|
|
RTA |
14 (63.6%) |
21 (77.7%) |
|
Fall |
4 (18.2%) |
2 (7.1%) |
|
Assault |
3 (13.6%) |
2 (9.1%) |
|
Sports |
1 (4.5%) |
2 (7.4%) |
|
Employment |
|
|
|
Light |
12 (54.5%) |
15 (55.5%) |
|
Heavy manual |
9 (40.9%) |
11 (40.7%) |
|
Unemployed |
1 (4.5%) |
1 (3.7%) |
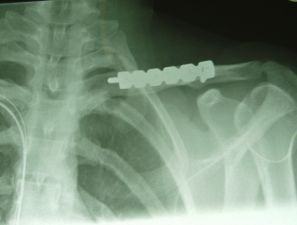
Fig.1
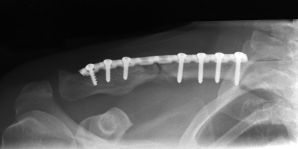
Fig.2
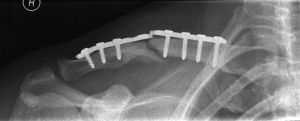
Fig.3
Any adverse event or complication was defined
as any event necessitating another operative procedure or
medical treatment (Table 2). Out of the six patients in whom the
plates were removed, five were superiorly placed plates (P value
0.032) and one was anterior. Two patients (P value 0.041) in the
superior group had a broken implant (Fig 3) which was replated
anteriorly. Two wounds-one in each group, had superficial
infection (P value 0.693). The wounds were dressed regularly and
healed in two weeks. One patient in the superior group developed
deep infection, for which the metal work had to be removed (P
value 0.869). The clavicle was replated anteriorly once the
infection settled. There were no non-unions/delayed unions/
neurovascular complications/ pulmonary injury /shoulder droop in
either group.
Table 2- Complications
|
TABLE 2 |
Anterior
group(N=22) |
Superior group
(N=27) |
P value |
|
Hardware
removal |
5 |
1 |
0.032 |
|
Hardware
failure |
0 |
2 |
0.041 |
|
Superficial
infection |
1 |
1 |
0.693 |
|
Deep infection
|
0 |
1 |
0.869 |
Table 3- Patient satisfaction
|
TABLE 3 |
Anterior
group(N=22) |
Superior group
(N=27) |
|
Patient
questionnaire |
|
|
|
Scar |
|
|
|
Excellent |
17 |
20 |
|
Good |
2 |
3 |
|
Fair |
1 |
3 |
|
Poor |
2 |
1 |
|
Return to work |
22 |
25 |
|
Patient
satisfaction |
21 |
26 |
The results were analysed by a
Physiotherapist as a neutral observer with a Biodex machine.
Constant score, shoulder range of movements and patient
satisfaction with function and scar were assessed. Constant
score was used to assess outcome in 37 patients. Since it was
impossible to allocate a preinjury score, the injured side was
compared to the uninjured side. Among them, 19 patients in the
superior group had mean Constant score of 87. The remaining 18
patients in the anterior group had a mean score of 89 (P value
0.784). Rest of the patients were assessed for outcome based on
clinical case notes and telephonic questionnaire as they were
unable to come for the appointment.
Patients were asked specific questions about
the scar, satisfaction with the operation, level of activity and
return to work (Table 3). Three patients (6%) considered the
scar as poor out of which one had a scar hypertrophy. Forty
seven patients (96%) thought that the operation helped them get
back to their work and activities of daily living while two
thought the contrary( one from each group) of which one of them
had a claim going through. Forty seven patients (Anterior
group-21, Superior group-26) felt that they would have the
operation on the opposite side if their clavicle fractured.
Discussion :
In this retrospective assessment, we have
compared the results of anterior versus superior placement of
the plate on the clavicle. Fractures of the clavicle account for
35-45% of shoulder girdle injuries [11]. According to Allman,
midshaft fractures are the commonest type of clavicle fractures
accounting for 80%. They occur at the site of lowest resistance
of the bone, when it passes from a prismatic cross-section to a
flattened one.
The clavicle does have several important
functions, each of which can be expected to alter in non-union
and malunion. In treating fractures of middle third of clavicle,
several factors should be considered: the patients age and
general condition, sex, fracture comminution, occupation,
personality of the patient and other concomitant injuries [12].
Neers[5] non-union rate of 1% is misleading in that the patient
population was mixed with regard to age, clavicular fracture
site and severity of fracture. In Robinsons series [12] the
non-union rate was between 4.5-9.5% for type 2B1/2 fractures
while in Hills series [6] 15% developed non-union.
Shortening of clavicle exceeding 17mm can
result in abduction weakness due to a restriction of the scapula
in the adducted position by the shortened clavicle [3, 13].
Potential drawbacks of conservative management can be overcome
by surgical treatment with the recovery of a normal anatomic
profile.
Displaced fractures of clavicle with
shortening of 20mm or more should not be treated the same way as
undisplaced or minimally displaced fractures. It is very rare to
achieve success with conservative treatment of such fractures.
The deforming force of sternocleidomastiod is very strong [14]
and cannot be overcome by external supports.
The use of open reduction in the treatment of
fresh fractures remains controversial; with wide geographical
and institutional variation in the choice of treatment. There is
still a reluctance to treat fresh clavicle fractures with
primary internal fixation in significant number of institutions
due to problems with operative treatment like operative scar,
infection, implant failure and implant removal [15].
A recent meta-analysis showed that operative
fixation compared to conservative treatment reduces the relative
risk of non-union by 86% [9]. Operative fixation allows earlier
rehabilitation with a high level of patient satisfaction with
respect to shoulder function. Pain relief is faster and there is
no problem of immobilisation with shoulder straps. Rigid
internal fixation may also allow patients to return to certain
occupations and driving earlier.
The choice of surface for plating of clavicle
fractures is not clearly defined. Conventionally the clavicles
are plated on its superior surface. Anterior plating of the
clavicle makes the metal work less prominent due to better soft
tissue cover. As a result, the need for removal of prominent
hardware becomes less. Also the risk of injuring the important
neurovascular structures is less while drilling the screw holes
from anterior to posterior compared to superior to inferior
direction.
We accept that this is a retrospective study
and a relatively small series. Further studies to compare
surface of choice for clavicular plating in a prospective
randomised manner would be useful to substantiate these
results.
In our study, the union rate was 100%. The p
values did not reach significance with respect to Constant
scores and infection. Majority of patients in both groups were
satisfied with the scar as the location of the scar was the same
in both groups irrespective of whether the clavicle was plated
anteriorly or superiorly.
The superior group had significantly higher
number of hardware failures and hardware removal compared to the
anterior group. Placement of the plate anteriorly rather than
superiorly on the clavicle yielded better results with regards
to these two factors. Hence we recommend anterior plating as a
better method of fixation of midshaft clavicular fractures.
Reference :
1. Neer C. Fractures of
the clavicle. In: Rockwood CA Jr, Green DP, editors. Fractures
in adults. 2nd ed. Philadelphia: Lippincott; 1984.
p707-13.
2. Crenshaw AH.
Fractures of the shoulder girdle arm and forearm. In: Crenshaw
AH, editor. Campbells operative orthopaedics. 8th
ed. St.Louis: Mosby Year book; 1992.p 989-1053.
3. Eskola A, Vaininpaa
S. Surgery of ununited clavicle fracture. Acta Orthop Scand
1986; 57:300-70.
4. Allman Jr FL.
Fractures and ligamentous injuries of the clavicle and its
articulation. J Bone Joint Surg [Am] 1967; 49-A: 774-84.
5. Neer CS. Nonunion of
the clavicle. JAMA 1960:172:1006-11.
6. Hill JM, Mcguire MH,
Crosby LA. Closed treatment of displaced middle-third fractures
of the clavicle gives poor results. J Bone Joint Surg [Br] 1997;
79-B: 537-9.
7. McKee MD, Schemitsch
EH, Stephen DJ, Kreder HJ, Yoo D, Harrington J. Functional
outcome following clavicle fractures in polytrauma patients. J
Trauma. 1999; 47:616.
8. Chan KY, Jupiter JB,
Leffert RD, Marti R. Clavicle malunion. J Shoulder Elbow Surg.
1999; 8:287-90.
9.Zlowodzki M, Zelle BA,
Cole PA, Jeray K, Mckee MD; Evidence-Based Orthopaedic Trauma
Working group. Treatment of midshaft clavicle fractures:
systematic review of 2144 fractures: on behalf of Evidence-Based
Orthopaedic Trauma Working group. J Orthop Trauma. 2005;
19:504-7
10. Nonoperative
Treatment Compared with Plate Fixation of Displaced Midshaft
Clavicular Fractures. A Multicenter Randomised Clinical Trial By
the Canadian Orthopaedic Trauma Society. J Bone Joint Surg Am.
2007; 89:1-10.
11. Robinson CM.
Fractures of the clavicle in the adult. Epidemiology and
classification. J Bone Joint Surg [Br] 1998; 80-B: 476-84.
12. Robinson CM,
Court-Brown CM, Mcqueen MM, Wakefield AE. Estimating the risk of
non-union following nonoperative treatment of clavicular
fracture. J Bone Joint Surg AM. 2004; 86:1359-65.
13. Mckee MD, Pedersen
EM, Jones C, Stephen DJ, Kreder HJ, Schemitsch EH, Wild LM,
Potter J. Deficits following non-operative treatment of
displaced clavicular fractures. J Bone Joint Surg Am. 2006;
88:35-40.
14. Poigenfurst J,
Rappold G, Fischer W. Plating of fresh clavicular fractures:
results of 122 operations. Injury 1992; 23(4):237-41.
15. Bostman O, Manninen
M, Pihlajamaki H. Complications of plate fixation in fresh
displaced midclavicular fractures. J Trauma. 1997; 43:778-783.
|





