|
Abstract:
Although
rare, pediatric spinal injuries are associated to the highest
mortality rate of all orthopedic injuries in children. We
present a retrospective study of 15 children operated for
unstable spinal fractures between October 2002 and November
2005. The mean age ranged from 7 to 14 years old with an average
of 10.3 years old and the male/female ratio was 2. The causative
etiologies were falls in 12 cases and motor vehicle accidents in
3 cases. 40% of the children sustained one or more associated
injuries and 73.3% of patients had neurological deficits. The
lumbar spine and the thoracolumbar
junction were the predominant levels of trauma. For the surgical
treatment, posterior approach was employed in 13 cases and a
transpleural thoracotomy in 2 cases. Except patients with
Frankel grade A, all others won at least 1 grade according to
the grading of Frankel. There was no case of death.
Consolidation, maintenance of alignment, and stable fixation
after one year recessions were seen in all documented
radiography of patients. Length of follow-up for these patients
ranged from 1 to 4 years.
Keywords:
child, unstable fractures, spine, surgery.
J.Orthopaedics 2007;4(2)e27
Introduction:
Fractures
and severe injuries of the spine in children are relatively
rare; it represents 1 to 10% of spinal injuries reported by
various authors (1-8). Anatomic and biomechanical
characteristics of the spine in the developing child explain the
different patterns of injury occurring in the childhood
comparatively to the adult population. Therefore,
the purpose of this paper is to describe the clinical and therapeutical particularities of
spinal trauma in children and to compare our results to other
series reported in the literature.
Material and Methods :
This
is a retrospective series of fifteen infants
hospitalized at the neurosurgery department of the
university hospital of Fez for injuries
of the vertebral column or the spinal cord between
October 2002 and November 2005.
Only the unstable lesions were included in this study.
Hospital
and clinic records for each patient were reviewed, noting
demographic data, mechanism of injury, level involved, type of
bony injury, presence of spinal cord injury, any associated
injuries, treatment received, length of hospital stay, and
outcome.
Results :
There
were 123 cases of spinal traumatism admitted into our department
during the same period (October 2002- November 2005). Eighteen
Childs with spinal injuries were identified from the trauma
registry, and fifteen medical records were available for review.
There were ten boys and five girls; the male/female ratio was 2.
The age of our patients was situated between 7 and 14 years; the
mean age was 10.3 years.
Falls
were the most common cause in this series (12 cases); Motor
vehicular accidents were seen in 3 cases only. However, there
were no documented cases of child abuse. The duration of
admission varied from 2 hours to Three weeks.
Preoperatively,
the neurological examination was normal in four patients. In
contrast, 11 patients had spinal cord injury. The neurological
deficit was classified according to the Frankel grading: seven
patients had paraplegia (three of grade A and four of grade B),
four patients had paraparesia (three of grade C and one of grade
D).
All
patients have systematically benefited of x-ray at the level of
lesion and CT scan of the spinal cord. Injuries localized to the
thoraco-lumbar junction (T11-L1) were predominant (6 cases). The
cervical spine was affected in 4 cases and the lumbar spine in 3
cases. Only two patients had thoracic involvement. There
wasnt any patient with multiple spine level involvement.
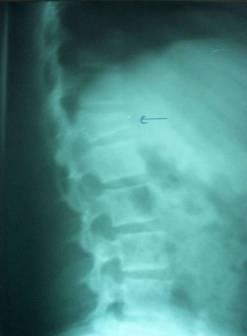
Patterns of vertebral column injury were divided into three
types: Vertebral fracture without disco-ligamentous injuries
(Figure 1) was seen in 11 cases (73.3%); subluxation or
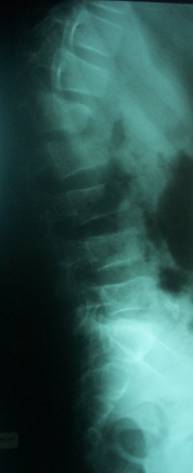
dislocation only was seen in one case (6.7%); and fracture with
disco-ligamentous injuries or mixed injuries (Figure 2) were
seen in 3 cases (20%). Excluding abrasions and minor
lacerations, associated injuries were seen in six patients, five
of them had associated lower limbs.
In addition, two patients had closed head injury and one
patient had hemothorax.
|
 |
 |
| Fig 1 |
Fig 2 |
No
neurological deterioration was noted during any patients
hospital stay. All patients underwent spinal surgery during
their hospitalization. The posterior approach was employed in 13
cases. The remaining two patients underwent anterior
decompression through a transpleural thoracotomy. For patients
operated using posterior approach, a laminectomy in frontal of
the involved level was practiced in 6 cases. Three patients
underwent posterior stabilization alone; they had complete
spinal cord injuries, with no signs of neurological improvement
in the postoperative course. However, the remaining patients won
at least 1 grade according to the Frankel grading. In our
series, the mean length of hospitalization was 9 days ranging
from 6 to 23 days.
The
overall complication rate was 20% (3 patients).
Two
of them developed ulceration at the supporting point; one of
them was treated also for urinary tract infection with a
favorable outcome. The osteosynthesis infection was deplored in
one case by the tenth day after surgery; this required the
removal of the osteosynthesis materiel and antibiotherapy
according the favorable clinical evolution; considering the
paraplegia, this patient benefited also of orthopedic treatment
(Grade A de Frankel). No death was recorded in the studied
series.
Consolidation,
maintenance of alignment, and stable fixation as documented on
radiographs at 1 year were seen in all patients. Length of
follow-up for these patients ranged from 1 to 4 years.
Discussion :
Spine
injury in the pediatric population remains uncommon, with
reported frequencies of 1 to 10% (1-8). Comparing to the adult,
the pediatric patient is anatomically and biomechanically
different with more flexible and mobile spine (9). In fact,
ligaments, discs, and surrounding soft tissue structures are
more elastic and the musculature is less developed in children
than in adults. These explain the relative resilience of the
pediatric spine to injury as well as the different features of
spinal injuries occurring in the childhood comparatively to the
adult population.
In
our series, the most common cause of injury was falls. This
contrasts with the majority of previous reports in that the
motor vehicle accidents were the principle causes (1, 4, 5,
10-12). Generally, 50% of children with spinal injuries have
associated injuries. The most common extra spinal injury was in
head (4, 13). This is in difference from our results where 33.3%
of patients had associated orthopedic injuries.
Furthermore,
the incidence of pediatric spinal injury increased with age
(1-4, 14). This may be
reflective of the protective effect of a flexible spine in the
younger child. In previous reports, most of spinal injuries in
children were located at the cervical spine (1-3, 5, 10, 11). In
contrast, the lumbar spine and the thoracolumbar junction were
the most involved levels in our series. This could be explained
by the mechanism of the traumatism, where falls were
predominant. The choc wave transmission during axial trauma is
mainly achieved at the lumbar spine and the thoracolumbar
charnel. Previous published works reported 11 to 16% incidence
of multilevel spine involvement in children (5, 14). We
havent recorded any multimodal lesion.
Generally,
spinal cord involvement is observed in 19% of spine injury in
children (10). Indeed, patients with a dislocation or
fracturedislocation had a higher incidence of neurologic
injury than did patients with fracture alone. This is to be
expected as dislocation causes larger degrees of displacement
than pure fracture types, and the force required to produce such
a displacement must be greater (10). In our series, a total of
11 patients had neurologic deficit; seven of them were
paraplegic.
Ideally,
the surgical treatment should be done in emergency. This permit
neural decompression as well as good alignment of the spinal
column and a satisfactory stabilization of the spine. As in
previous studies, the majority of patients with partial injuries
showed neurologic improvement in the postoperative course (9).
This is attributable to plasticity and greater capacity for
recovery of the immature spinal cord (10).
In
our series, the overall complication
rate was 20% and there wasnt any case of death recorded.
Previous reports in the literature showed a much high rate of
mortality and complications (12, 15). We can explain
these results by higher average age of our patients and the
dominance of the thoracolumbar spinal lesions.
In
fact, previous studies have shown that the more serious and
fatal injuries occurred in children younger than 8 years (13,
16) and from cervical spine injuries (17).
Conclusion:
Spinal
injuries in children are relatively uncommon compared with
adults. The spinal cord involvement is the greater risk. Optimal
treatment requires a well understanding of the medical and
spinal characteristic of this population. The prognosis depends
on the rapidity of care, the spinal level of the lesion and the
clinical profile of the associated lesions
Reference :
-
Anderson JM, Schutt AH. Spinal injury in children: a review of 156
cases seen from 1950 through 1978. Mayo Clin Proc. 1980; 55:
499-504.
-
Burke DC. Spinal cord injuries, 1976. Aust NZ J Surg. 1977; 47:
166-170.
-
Dickman CA, Zabramski JM, Hadley MN, Rekate HL, Sonntag VK.
Pediatric spinal cord injury without radiographic abnormalities:
Report of 26 cases and review of the literature. J Spinal Disord
1991; 4: 296-305.
-
Eleraky MA, Theodore N, Adams M, et al. Pediatric cervical spine
injuries: report of 102 cases and review of the literature. J
Neurosurg. 2000; 92: 12-17.
-
Hamilton MG, Myles ST. Pediatric spinal injury: review of 174
hospital admissions. J Neurosurg. 1992; 77: 700-704.
-
McPhee IB. Spinal fractures and dislocations in children and
adolescents. Spine. 1981; 6: 533-537.
-
Rekate HL, Theodore N, Sonntag VK, Dickman CA: Pediatric spine
and spinal cord trauma: State of the art for the third
millennium. Childs Nerv Syst 1999; 15: 743-750.
-
Ruge JR, Sinson GP, McLone DG, Cerullo LJ. Pediatric spinal
injury: The very young. J Neurosurg 1988; 68: 25-30.
-
Osenbach RK, Menezes AH. Pediatric spinal cord and vertebral
column injury. Neurosurgery 1992; 30: 385-390.
-
Carreon LY., Glassman SD., Campbell MJ. Pediatric
Spine Fractures A Review of 137 Hospital Admissions. J Spinal
Disord Tech 2004; 17: 477-482
-
Cirak BB, Ziegfeld S, Knight VM et al. Spinal Injuries in
Children. Journal of Pediatric Surgery 2004; 39 (4): 607-612.
-
Kewalramani LS, Kraus JF, Sterling HM. Acute spinal-cord lesions
in a pediatric population: epidemiological and clinical
features. Paraplegia. 1980; 18: 206-219.
-
Orenstein JB, Klein BL, Gotschall CS, et al. Age and outcome in
pediatric cervical spine injury: 11-year experience. Pediatr
Emerg Care. 1994; 10: 132-137.
-
Hadley MN, Zabramski JM, Browner CM, et al. Pediatric spinal
trauma: review of 122 cases of spinal cord and vertebral column
injuries. J Neurosurg. 1988; 68: 18-24.
-
Hamilton MG, Myles ST. Pediatric spinal injury: review of 61
deaths. J Neurosurg. 1992; 77: 705-708.
-
Orenstein JB, Klein BL, Oschenschlager DW. Delayed diagnosis of
pediatric cervical spine injury. Pediatrics 1992; 89(6):
1185-1188.
-
Nitecki S, Moir CR. Predictive factors of the outcome of
traumatic cervical spine fracture in children. J Pediatr Surg
1994; 29(11): 1409-1411.
|




