|
Abstract:
Acute
Neuropathic Arthropathy of the Ankle resulting from acute
trauma, even though rare, is reported in diabetic patients.
If detected late, it can cause permanent deformity and
disability. It can
also cause flap damage and can lead to amputation.
The aim of this article is to report a patient with
history of diabetis mellitus with acute neuropathic arthropathy
of left ankle joint which evolved over a short period of 6
weeks, following acute trauma.
A 38 years old diabetic male presented with history of
trivial fall and sustained a minimally displaced fracture of
left medial malleolus extending to the tibial plofound.
Since the episode was painless because of diabetic
peripheral neuropathy, patient came walking on the second day
with swelling of left ankle joint.
Below knee POP cast was given as a primary treatment. But since the ankle was totally painless, patient walked with
the cast and removed the POP on seventh day on his own. He returned after 6 weeks with gross swelling and deformity
of left ankle joint. But
it was totally painless. Radiograph
at 6 weeks showed non union of fracture medial malleolus with
gross disorganization of the ankle joint along with bony
fragmentations. The
patient was treated with ankle foot orthosis.
Follow up radiograph showed non union of medial malleolus,
but consolidation of other fragments.
This article stresses to be aware of this particular
condition; and even though rare, it should be suspected in
diabetic patients with acute injuries.
Late diagnosis will result in disability and deformity. Awareness about the existence of this condition will avoid
chances of missed diagnosis.
Keywords: acute neuropathic arthropathy; ankle joint; diabetis mellitus;
neuropathy; acute injury.
J.Orthopaedics 2007;4(2)e23
Introduction:
Acute
neuropathic arthropathy is a rare complication of acute trauma
to ankle and foot. It is reported in diabetic patients1. Many surgeons fail to
diagnose it in the initial stage, untill full grown neuropathic
arthropathy sets in. Delay
in diagnosis will result in gross deformity and disability2.
The real incidence of acute neuropathic arthropathy has
not been estimated because of the diagnostic difficulties3.
The recommended treatment of acute neuropathic
arthropathy is non weight bearing immobilization for at least 3
months 4, 2, . Diabetic patients do have higher incidence of
incordination in the lower limbs due to neuropathy and are
likely to have frequent falls5. Due to greater weight
transmission, acute neuropathic arthropathy of foot and
ankle is likely to take longer time to heal 1.
Body weight, body mass index and duration of diabetis are
likely to affect the outcome of acute neuropathic arthropathy1.
The current article describes a 38 years old diabetic
patient with acute neuropathic arthropathy of left ankle which
followed a trivial fall. Follow
up radiograph at 6 weeks showed well established acute
neuropathic arthropathy. This
article intends to discuss the pathophysiology of acute
neuropathic arthropathy. It
is important to note that 25000 cases of neuropathic arthropathy
are undiagnosed every year 6.
It is also important to be aware of this condition so
that such missed diagnosis can be avoided.
Case Report:
A 38 years old male patient with a history of diabetes mellitus
for the last 5 years, presented following a trivial fall, which
was followed by swelling of left ankle but without pain.
Patient initially thought it as a sprain, and did not
request for medical help. He
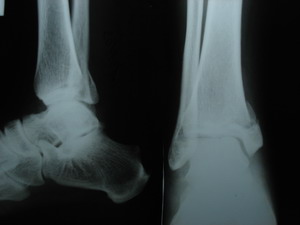
presented after two days to the Orthopaedic OPD and the X
rays at that time showed minimally displaced fracture of the
medial malleolus extending to tibial plafound (Figure 1).
It was totally painless.
He was immobilized with below knee POP cast and was
directed not to bear weight.
Since it was totally painless, he did not follow the
instructions and started weight bearing on the next day.
And on seventh day, the patient removed the POP on his
own and walked full weight bearing.
As there was no pain, he did not request for the medical
help for 6 weeks. At
6 weeks he presented to the OPD again because of persistent
swelling and deformity of the left ankle joint.
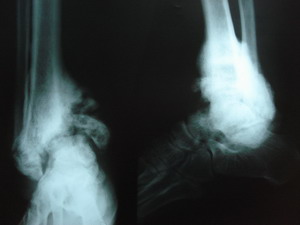
X- rays at that time showed full blown neuropathic
arthropathy with non union of medial malleolus and fragmentation
(Figure 2). He was
treated with Ankle-Foot-Orthosis.
At the time of writing this report the fracture did not
unite, but other fragments consolidated and the swelling
decreased in severity. There was no skin breakdown.
He had loss of all modalities of sensation including
proprioception in the foot distal to the ankle.
Random blood sugar at the time of first presentation was
240 mg% and subsequently it was well under control with Insulin.
He was on oral hypoglyceamic drugs for 5 years.
The opposite limb had features of peripheral neuropathy.
But there was no evidence of neuropathic arthropathy.
His body weight was 80 Kg.
|
|
|
| Figure 1: Xray on first presentation
showing minimally displaced fracture of the medial
malleolus extending to Tibial plafond |
Figure 2: X ray at 6
weeks after the initial injury showing established
neuropathic arthropathy of the ankle joint |
Discussion :
Neuropathic
Arthropathy was first described by Jordan in 1936 6.
It was originally described in tabes dorsalis by Jean
Mary Charcot. With
the effective control of syphilis, now the majority of
neuropathic arthropathic joints are due to diabetis mellitus.
Colhisty and Thomson 4 reported 18 adult patients with
juvenile onset diabetis mellitus and neuropathic fractures of
ankle. They
advocated strict immobilization as a mode of treatment.
Arrmstrong et al 7 reported that longer periods of
immobilization is needed for a better outcome.
It is possible that a patients after a fall presenting
with swelling and a normal X- ray, the surgeon diagnoses the
injury as minor, as it is usually painless and sends the patient
home, without immobilization or restriction of weight bearing1. This could aggravate the condition. It is also possible that the patient may present late, since
the condition is totally painless.
It will be too late when the patient presents for medical
help1 as in this case.
So
it is important that this condition should be diagnosed early.
Surgical outcome of acute neuropathic arthropathy is
usually is very poor 8, 2. In this case patient had marginal
improvement with ankle-foot-orthosis.
He had symptomatic relief, even though the fracture of
medial malleolus did not unite.
Early immobilization is an effective treatment and helps
in limiting the destructive phase of acute neuropathic
arthropathy1. Each
year 40000 new cases of neuropathic arthropathy are diagnosed11.
Majority of them are usually chronic.
Less than 10% of neuropathic arthropathy affects the
ankle joint 9
Usual
presentation of neuropathic arthropathy is in the sixth and
seventh decade of life with a long history of diabetes mellitus
(15 years) 10. This
patient presented in his fourth decade of life with a history of
diabetes mellitus for the last 5 years.
The usual features of diabetic peripheral neuropathy are
loss of all modalities of sensation including proprioception 11.
Neuropathy is a pre-requisite for neuropathic arthropathy. Majority are diabetic patients on either oral hypoglyceamic
drugs or insulin 12. Edema,
erythema, crepitus and increase in foot temperature are the
usual signs of neuropathic arthropathy 6.
The
radiographic appearance of neuropathic arthropathy is classified
as hypertrophic, atrophic and atrophic evolving on hypertrophic
13. The
pathophysiology of acute neuropathic arthropathy is unknown.
There are certain theories, which describe the
pathophysiology of neuropathic arthropathy.13
Nuerovascular
theory: There is
loss of sympathetic tone to the blood vessels which results in
hyperemia of bone and ligaments.
The hyperemia leads to bone resorption and ligament
weakning resulting in fractures and dislocations during normal
weight bearing. The
patient will have no pain; hence the fracture is not
immobilized. This
results in hypertrophic non union.
Nuerotraumatic
theory: It states that repeated microtrauma due to the
peripheral neuropathy, results in exaggerated healing as the
fracture is not protected, 13.
Microangiopathy and increased atherosclerosis could also
contribute to the pathogenesis of neuropathic arthropathy 11.
Even
though diabetis mellitus is a commonest cause of neuropathic
arthropathy, other causes 13 should be kept in mind to avoid
missed diagnosis. They include Syphilis, Multiple sclerosis,
Hansens disease, Syringomyelia, Alcoholism, Myelopathy, Steroid
injection and congenital insensitivity to pain.
There
are 3 stages in the development of neuropathic arthropathy 13.
In stage one, there is swelling, erythema, warmth and
hyperemia. In stage
II, also known as coalescence stage, there will be fractures,
subluxations or dislocations.
Stage III is the healing stage. There will be no
inflammation, but with residual deformity.
It is always important to rule out osteomyelitis in
neuropathic arthropathy 10.
Osteomyelities is quiet distinct clinically and
radiologically.
The
traditional method of treatment of neuropathic arthropathy is
conservative, even though surgical fusion and amputation are
described 14. Bisposphanates
may help in reducing bone loss 13.
Sincare 1 achieved 100% healing with total contact
casting and partial weight bearing.
After healing rocker bottom heel is given to prevent
future damage1. This
case was treated with ankle-foot-ortosis.
The other devices which can be used are
Charcot restrained orthotic walker, Patellar Tendon
bearing caliper, or extra depth shoes.
Combined magnetic field therapy may be beneficial in
neuropathic arthropathy. Electrostimulation
is reported to be useful in the treatment of neuropathic
arthropathy 15
The
traditional methods are the gold standards in the treatment of
neuropathic arthropathy. But
complimentary techniques may help in better healing.
Conclusion:
This
article describes a case of acute neuropathic arthropathy, which
evolved over a short period of 6 weeks.
Patient had history of diabetes mellitus.
It is very important not to miss the diagnosis in the
acute stage so that the delay in starting the treatment can be
avoided. This
article signifies the need to be aware of acute neuropathic
arthropathy even though the X-ray may look normal.
An early diagnosis will help in a long way to prevent
deformity and disability.
Reference :
-
Sincare R D.
Acute Charcot arthropathy in Patients with Diabetes
Mellitus:Healing Times by foot location.J diabetic
complications 1998;12:77-82.
-
Johnson JTH.
Neuropathic fractures and joint injuries: Pathogenesis and
rationale of prevention and treatment. J Bone Joint
Surg1967; 49A:130,
-
Armstrong DG,
Lavery LA. Acute Charcot arthropathy of the foot and ankle.
Phys Ther 1998;78:74-80.
-
D.R. Clohisy
and R.C. Thompson. Fractures associated with neuropathic
arthropathy in adults who have juvenile-onset diabetes. J
Bone Joint Surg 1988;70-A: 11921200
-
P.R. Cavanagh,
J.A. Derr, J.S. Ulbrecht, R.E. Maser and T.J. Orchard.
Problems with gait and posture in neuropathic patients with
insulin-dependent diabetes mellitus. Diabetic Med 1992;9:
469474.
-
Grady JF.
Oconnoor KJ, Axe TM,Zager EJ, Dennis LM, Brenner LA.Use
of electro stimulation in the treatment of diabetic neuro
arthropathy. Jam PodiatrMed Assoc 2000;90:287-94.
-
D.G.
Armstrong, W.F. Todd, L.A. Lavery, L.B. Harkless and T.R.
Bushman, The natural history of acute Charcots
arthropathy in a diabetic foot specialty clinic. Diabetic
Med 1997:14;357363.
-
Sinha S,
Munichoodappa CS, Kozak GP. Neuro-arthrop-athy (Charcot
joints) in diabetes mellitus: Clinical study Manageof 101
cases. Medicine 1972;51:191210.
-
Gupta R .A
short history of Neuropathic Arthropathy.Clin
Orthop1993;296:43-49.
-
Pinzur MS
Charcots foot . Foot and Ankle Clin 2000;5:897-912
-
Shaw JE. The
Pathogensis of Diabetic Foot Problems: an overview.
Diabetes1997: 46(suppl 2):S 58-61.
-
Smith DG,
Barnes BC, Sands AK, Boyko EJ, Ahroni JH. Prevalence of
radiographic foot abnormalities in patients with Diabetes.
Foot ankle. int 1997;18:342-6.
-
Melanie D,
Osterhouse DC, Norman W, Kettner DC. Neuropathic Osteo
arthropathy in Diabetic foot. J Manipul and Physiol Ther
26;6:416-22.
-
Harrelson JM.
Management of of diabetic foot . Orthp clin North Am
1989;20:605-19.
-
Evans RD, Foltz
D, Foltz K. Electrical stimulation with bone and wound
healing. Clin Podiatr Med Surg 2001;18:79-95.
|




