|
Abstract:
Duncan
and Thurstons seminal research paper written 20 years ago,
demonstrated that the actual number of scaphoid fractures
amongst all cases diagnosed clinically was very small. Three
more research studies over the next 10 years concurred with his
findings. However, specialist clinics still receive a large
number of referrals from the A&E labelled as clinical
scaphoid fractures.
To
improve this situation, this study was undertaken at Ninewells
hospital, Dundee. The objective was to analyze the clinical
value of various tests and thus formulate a new set of
guidelines for the A&E staff to follow.
Patients and Methods:
58
subjects were followed up to assess how many were actually
scaphoid fractures after being referred as clinical fractures.
With this the specificity and sensitivity of various tests could
also be reviewed and compared with literature.
Results:
Only
one of the 58 patients was found to have a scaphoid fracture on
the fourteenth day after initial normal radiographs. Most
examination variables were high in sensitivity, but had poor
specificity.
Conclusions:
More
variables could not be examined due to daily changes in the
A&E staff and no fixed protocol. The value of higher
modalities of imaging was also reviewed only on the basis of
current literature. The level of clinical skills in the
management of scaphoid fractures was fund to be unsatisfactory.
Keywords:
Scaphoid; Clinical fracture.
J.Orthopaedics 2007;4(2)e15
Introduction:
How
many radiologically negative wrist injuries turn out to be true
clinical scaphoid fractures? This is the primary question this
paper addresses. If this number is unacceptably low, what can we
do to improve it? This question will also be tackled
Between
1985 and 1995, four large studies1 showed the percentage of
clinically suspected scaphoid fractures, being actual fractures
to be between 0% and 6.48%. Duncan and Thurstons seminal
paper2 reviewed 108 patients who were immobilised for a
clinically suspected scaphoid fracture. On follow-up it was
discovered that not a single patient had had a scaphoid injury.
This led them to refer to this entity as an illusionary
diagnosis.
Material and Methods :
This
study was conducted at the specialist clinics of Ninewells
hospital, Dundee. All 58 patients who attended the fracture
clinic between September 2005 and February 2006, after being
diagnosed as a suspected scaphoid injury the previous day in the
A&E, were included in the study.
The
patients were followed up clinically and radiologically for a
minimum of three weeks so as to arrive at a definitive
diagnosis. The choice and number of clinical tests and
manoeuvres employed by the A&E staff was also reviewed.
For
the statistical analysis, data was explored for distribution and
extreme values. Descriptive statistical methods were used
including histograms for continuous data and tables for
categorical data. Where appropriate means and standard
deviations were presented otherwise the median was given.
Results :
Of
the 58 study subjects, 13 had scaphoid fractures, but only one
patient was a true clinical scaphoid fracture who was
radiologically negative on days 1 and 2, and then showed
evidence of a scaphoid fracture on day 14.
As
each potential variable was looked at individually, the results
are similarly displayed.
Age
Distribution- The age distribution
in the study subjects ranged from nine to 83 (Figure 1). Amongst
the confirmed fracture patients the ages ranged from 15 years to
61 years with a mean of 31.5 years.
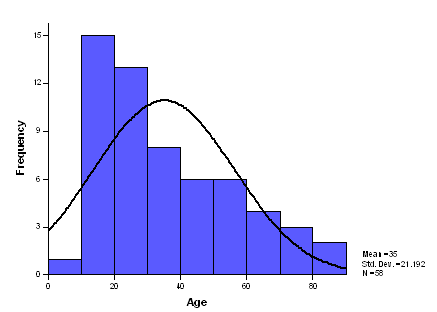
Figure
1- The age distribution of study subjects
Delay
in Presentation- This ranged from
one hour to 336 hours with three exceptionally outlying values
for patients who presented five, ten and fourteen days after the
injury. To get the most statistically accurate picture the
median was calculated which was measured as 10 hours (Figure 2).
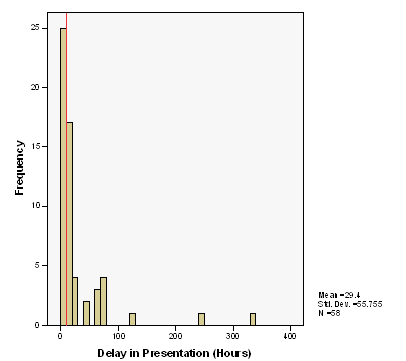
Figure
2- The median delay in presentation shown as a red line
Mechanism
of Injury- The commonest mechanism
described by the patients was a fall on an outstretched hand
with a dorsiflexion strain on the wrist. 45 of the 58 study
subjects described this mechanism. Of the 13 fracture patients,
all described this mechanism.
Also
noteworthy is that over 30% of the scaphoid fracture group were
indulging in a sporting activity at the time of injury.
Site
of Pain- The anatomical snuff box
(ASB) was the commonest site of pain described by patients
(Table 1). Sites such as the lower end of the radius, the radial
styloid and the base of the thumb have been labelled as
other
| Site
of pain |
Anat.
Snuff box only |
Anat.
Snuff box & other |
Other |
| In
study subjects (58) |
22
(37.9 %) |
31 (53.4 %) |
5 (8.7 %) |
| In
scaphoid fracturepatients (13) |
7 (53.8%) |
5 (38.4%) |
1(7.8%)
(No pain) |
Table
1-
Incidence of pain in the anatomical snuff box
History
of Previous Injury- Three (23%) of
the thirteen fracture patients had a history of previous
scaphoid fractures or fractures adjacent to the scaphoid.
Presence
of Swelling- This is displayed in
Table 2.
| Presence
of swelling |
Anat.
Snuff box |
Diffuse
over wrist |
Nil |
| In
study subjects (58) |
8
(13.7%) |
24
(41.3) |
26
(45%) |
| In
scaphoid fracture patients (13) |
3 (23%) |
5 (38.5%) |
5 (38.5%) |
Table 2- Incidence of
swelling
Presence
of Local Redness- The appearance
of signs of inflammation over the wrist and ASB are shown in
Table 3
| Presence
of local redness |
Yes |
No |
| In
study subjects (58) |
18
(31%) |
40
(69%) |
| In
scaphoid fractureIn scaphoid fracture patients (13) |
3 (23%) |
10 (77%) |
Table 3- Incidence of local
redness
Radiographs
at Presentation- 41 (70.6%) of the
study subjects were X-rayed on presentation. Amongst those
X-rayed, the primary diagnoses made by the A&E staff are
displayed in Table 4.
| Suspected scaphoid
fracture |
4
(9.7%) |
| Obvious
scaphoid fracture |
6
(14.6%) |
| No
abnormality detected (NAD) |
30
(73.2%) |
| Other
injuries |
1
(2.5%) |
Table
4-
Primary radiographic diagnoses in the A&E
Follow-up
Radiographs- 51 patients were
deemed warranting a follow-up radiograph to attain a definitive
diagnosis.
Additional
Information-Three cases of
scaphoid fractures were missed by A&E staff and reported as
NAD on radiographs.
Four cases of scaphoid fractures were not X-rayed in the
A&E.
Seven
(54%) scaphoid fractures were diagnosed in follow-up clinics.
Three
cases of scaphoid fractures were not X-rayed in the A&E, and
were diagnosed by X-rays on day-2.
One
case of scaphoid fracture was not X-rayed in the A&E, and
was diagnosed by X-rays on day-14.
Two
cases were interpreted as NAD by A&E staff on radiographs
and then diagnosed as fractures by the fracture clinic staff on
day-2.
One
case was diagnosed as NAD on days 1 and 2 and then diagnosed as
a scaphoid fracture on day-14.
Four
cases of fresh scaphoid fractures were diagnosed by the A&E
staff.
Discussion :
This
study demonstrates that no one piece of history or clinical test
will conclusively prove or disprove a scaphoid fracture, hence
the examiner must be careful that he asks all the relevant
questions and performs all the tests with an acceptably high
level of sensitivity and specificity.
The
age of the patient guides us as scaphoid fractures are rarely
seen in extremes of ages. These age groups usually suffer a
distal radial injury.
The
mean delay in presentation even in the fracture group was 26.15
hours hence the junior doctor should not assume lesser
importance in these patients.
The
mechanism of injury in this study was always a fall on an
outstretched hand with a forced dorsiflexion at the wrist.
However studies by Leslie and Dickson and Clay et al both showed
a 3% incidence of a hyper-flexion being the mechanism of
injury3. The present study had two (3.4 %) patients give a
similar mechanism history with clinical features of a possible
scaphoid injury.
The
site of pain located at the ASB in 93% of the cases. However
apart from ASB tenderness, other commonly employed tests such as
scaphoid tubercle tenderness (Freeland, 1989) and scaphoid
compression tenderness(Chen, 1989) could not be evaluated in
this study due to the inconsistency in their usage. R.Grover4 in
1996 published his results on the reliability of these three
signs (Table 5). This shows us that even though these tests are
very sensitive, their specificity is low.
| |
Sensitivity
% (95%
confidence limits) |
Specificity
% (95% confidence limits) |
| ASB
tenderness |
100% |
29%
(23-35%) |
| ST
tenderness |
83%
(70-96%) |
51%
(44-58%) |
| SC
tenderness |
100% |
80%
(74-86%) |
Table
5 Sensitivities and
specificities of ASB, ST and SC tenderness as indicators of
fracture in patients with suspected scaphoid injury (R.Grover,
1996)
The
presence of swelling was found to be an equivocal finding. This
concurs with the findings of Waizenegger et al5 who stated that
swelling and discolouration around the anatomical snuff box is
more common in cases with scaphoid fractures than without, but
not enough to be statistically or clinically significant.
The
presence of local redness and raised local temperature were both
found to be of no practical information.
The
importance of taking radiographs in the A&E is demonstrated
by the fact that scaphoid fracture cases were not X-rayed in the
A&E. Most cases of scaphoid fractures are diagnosed on
presentation radiographs, very few required follow-up
radiographs for their diagnosis (Dias J.J. et al,)6
Follow-up
radiographs were only required in one patient in this study.
The
usefulness of higher modalities of imaging was beyond the scope
of this study. However literature does seem to support their
role in indicated patients
In
conclusion, the findings of Tai C.C. et al.7paint a current
picture-
In
2005, they studied the management of suspected scaphoid
fractures in A&E departments in the U.K. They conducted a
survey on 146 A&E senior house officers (SHO) in 50
different hospitals. Their findings were -
55.8%
SHOs performed only one clinical test to diagnose suspected
scaphoid fractures
41%
were unable to cite the number of the radiographic views taken
Only
10% of departments have direct access to further radiological
investigation
Wide
variation in early treatment with 46% receiving scaphoid casts
54%
SHOs were not aware of any local guidelines for management of
suspected scaphoid fractures in their departments
92%
were not aware of the existence of the 1992 British association
for accident and emergency medicine (BAEM) guidelines.
They
concluded that the clinical knowledge and the management of
suspected scaphoid fractures in A&E are unsatisfactory.
This
paper therefore demonstrates the need for a new set of
guidelines to be laid down for the management of suspected
scaphoid fractures in the A&E department.
Reference :
-
Gow
K.: Immobilisation of suspected scaphoid fractures. BestBET:
2000.
-
Duncan
DS and Thurston AJ: Clinical fracture of the carpal scaphoid -
an illusionary diagnosis. Journal of Hand Surgery (Br) : 10:
375-6. 1985
-
Barton
N.J.: Twenty questions about scaphoid fractures. Journal of Hand
Surgery (Br): 17: 289-310. 1992
-
Grover
R: Clinical assessment of scaphoid injuriesand the detection of
fractures. Journal of Hand Surgery (Br): 21B: 3: 341-343. 1996
-
Waizenegger M, Barton N.J., Davis T.R.C. et al.: Clinical signs
in scaphoid fractures. Journal of Hand Surgery (Br): 19:
743-747. 1994.
-
Dias
JJ, Thompson J, Barton NJ et al.: Suspected scaphoid fractures.
The value of radiographs. Journal of Bone and Joint Surgery
(Br); 72: 98-101. 1990
-
Tai
C.C. et al.: Management of suspected scaphoid fractures in
accident and emergency departments - time for new guidelines.
Annals of the Royal College of Surgeons of England: 87 (5):
353-357. 2005
|




