|
Abstract
Sixteen cases of reverse sural artery flap
done in our institution are reviewed. Eleven were done under
combined femoral and sciatic nerve block. All were done for
lower third leg defects. Three flaps underwent necrosis. The
rest achieved their objective with minimum complications and
donor site morbidity. We conclude that this flap is a reliable
alternative to free tissue transfer for lower third defects of
the leg. The anatomical basis and operative technique is also
briefly outlined
J.Orthopaedics 2006;3(1)e3
Introduction:
Soft tissue coverage of the lower third of
the leg is a challenge, especially if microvascular expertise is
not available. Although we have started doing free tissue
transfer, our case load makes it impossible to do it in every
case. We have found the recently introduced sural artery
neurocutaneous flap to be extremely useful for lower third
defects. Here we present a series of 16 cases of sural artery
flap done in the past 2 years.
Material and Methods :
All the case records of patients who
underwent this procedure during the past 2 years were reviewed.
Patients were personally followed up whenever possible. The
patient details, flap size, type of defect, necrosis and other
relevant details were recorded.
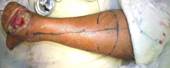 Technique: first, the sural nerve is
marked, from the mid-calf between the two heads of the
gastrocnemius to the midpoint between the Achilles tendon and
the lateral malleolus. The appropriately sized flap is marked
out on this line with the pivot point kept at least 5 cm above Technique: first, the sural nerve is
marked, from the mid-calf between the two heads of the
gastrocnemius to the midpoint between the Achilles tendon and
the lateral malleolus. The appropriately sized flap is marked
out on this line with the pivot point kept at least 5 cm above
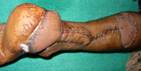
the lateral malleolus. The flap is elevated in the sub-fascial
plane including the sural nerve, the short saphenous vein, and
the vessels accompanying the nerve. We always keep a 2 cm skin
pedicle, which is kept after incising the path to the defect.
Drains are always kept. The donor site is skin grafted.
Results :
Sixteen patients underwent the procedure in
the last 2 years. All of them were referred from the orthopedics
department. All were done electively. Seven
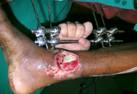
patients underwent the procedure for defects
in the region of the Achilles tendon either immediately for
inadequate soft tissue cover, or for later skin necrosis post
repair. Nine patients underwent the procedure for exposed tibia
in the lower third of the leg.
Out of the 16 patients, 2 were females and
the rest,
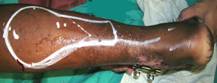
males. The ages ranged from 14 years to 65
years, the average being 36.8. Two people were diabetics and 2
had peripheral vascular disease as demonstrated by color
Doppler.
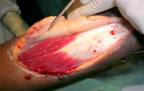
The sizes of the flaps ranged from 4 X 3 cm
to 12 X 10 cm. Three of the flaps underwent complete necrosis.
One flap had minimal rim necrosis. All the rest survived totally
and provided satisfactory cover. One patient complained of
excessive bulk and underwent flap thinning twice. There were no
cases of florid infection, hematoma or total graft loss at the
donor site.
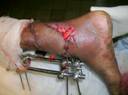
Four of the cases were done under spinal
anesthesia and 1 under general anesthesia. Ten cases were done
under combined sciatic and femoral nerve block, which made the
prone positioning and the position changes needed during graft
harvest and inset of the flap, very simple.
Discussion :
Coverage of wounds of the lower third of the
leg are usually best treated using microvascular free tissue
transfer. These flaps provide for reliable single stage coverage
of these wounds. There are certain disadvantages to free flaps.
These are: the need for a remote donor site, increased operative
time, use of a major vessel to the leg, and the need for
microvascular expertise. The alternative for coverage of these
defects has traditionally been pedicled fasciocutaneous flaps,
as described by Ponten1. but the distalmost portion is often
random in its blood supply and the lower third of the leg is
difficult to cover.
The design of these fasciocutaneous flaps has
undergone a revolution on the basis of the discovery of
neurocutaneous territories2. The cutaneous nerves of the body
are frequently accompanied by small arteries and veins that
supply the nerve and send small perforators to the overlying
skin. Experience subsequently demonstrated that the skin
overlying these territories could be elevated based on this
blood supply, even in a retrograde fashion, to cover defects as
distal as the forefoot. These kinds of flaps were first
described in the foreaem3. The best described of these flaps is
the sural artery flap.
The medial sural nerve descends in close
association with the lesser saphenous vein, passing posterior to
the lateral malleolus to supply the lateral side of the foot and
the great toe. It is also accompanied by the median sural
artery, a branch of the poplitial artery. This artery
communicates with perforators from the peroneal artery 5-10 cm
above the lateral malleolus. The blood supply courses in a
retrograde fashion from these perforators when the nerve and
artery are cut proximally. The exact technique of elevation is
described in materials and methods.
Mustafa Y et al in 1998 described 17 cases of
sural artery flap done for various defects of the ankle,
malleolus and the heel4. The largest flap used was 12 X 15 cm in
length. He observed partial necrosis of the flap in 2 patients.
He also noted the reliability of the flap and the importance of
taking a skin extension along with the pedicle of the flap.
Hollier L et al in 2002 studied the same flap
done in 11 patients5. He described partial necrosis in one
patient. He also emphasized a broad inferolateral pedicle and
the importance of including the short saphenous vein. Our series
of 16 patients, notes 3 total necrosis and 1 minimal rim
necrosis. But all these cases occurred early in our series and 2
of the patients were complicated by long standing diabetes and
peripheral vascular disease. Our largest flap measured 12 X
10cm. We were also maintaining a 2 cm skin paddle over the
pedicle instead of totally islanding it. We also note the ease
of doing the flap under combined sciatic and femoral nerve
block, which makes the positioning of the patient very easy6.
Intra-operative change of position especially for anterior
defects is made very simple. We also used tumescent solution
(dilute lignocaine and adrenaline) for infiltrating the margins
of the flap, which made a pneumatic tourniquet unnecessary7.
The disadvantages of the flap include ugly
donor site in the calf, and loss of sensation in the lateral
foot and leg5.
Conclusion:
To conclude, the distally based sural artery
flap is our flap of choice for reconstruction of the lower third
of the leg, when the lower lateral aspect of the leg is
relatively uninjured. It is a reliable one-stage procedure when
properly done. It can be safely done under combined femoral and
sciatic nerve block.
Reference :
- Ponten B. The fasciocutaneous flap. Its use in soft tissue
defects of the lower leg. Br. J. Plast surg. 34: 215.1981.
- Masquelet A C, Ramana M C, Wolf G. Skin island flaps
supplied by the vascular axis of the sensitive superficial
nerves: Anatomic study and clinical experience in the leg.
Plast.Reconstr.surg. 89: 1115, 1992.
- Beretelli JA and Khoury Z. Neurocutaneous island flaps in
the hand: Anatomical basis and preliminary results. Br. J.
Plast.surg. 45: 586, 1992.
- Yilmaz M, Karatas O, Baruteu A. The distally based
superficial sural artery island flap: clinical experiences and
modifications. Plast.Recostr.Surg. 102: 2358, 1998.
- Hollier L, Sharma S, Babigumira E, Klebuc M. Versatility
of the sural fascocutaneous flap in the coverage of lower
extremity wounds. Plast.Reconstr.Surg. 110: 1673, 2002.
- Khoo ST and Brown STK. Femoral nerve block- The anatomical
basis of a single injection technique. Anesthesia and critical
care. 11: 40, 1983.
- Klein JA. Tumescent technique for regional anesthesia
permits lidocaine doses of 35 mg/ kg for liposuction. Dermatol
Surg oncol. 16: 248, 1990.
|








