|
ABSTRACT
We report outcome of
nine-year follow up of fifty Charnley Cemented Primary
Arthroplasties in forty-seven patients performed between 1996
to 1999.The minimum follow up period was 5 years with a mean
of seven years. All hip joints were thoroughly assessed
preoperatively to document patients functional level and
Harris Hip Score was calculated. All the patients were
disabled because of pain in hip and forty-five (90%) had used
walking aids. At follow up all patients were living. The
radiographs of all patients were available for the entire
follow up period. Of the fifty operated hips, only two
patients (4%) complained of pain while rest all were pain
free. Postoperatively only ten (20%) patients used support for
walking. At follow up none of the hips were revised. Two
patients (4%) had dislocation in postoperative period in which
reduction was done under anesthesia. In one patient (2%)
prosthesis and cement was removed because of deep infection.
In two patients (4%) radiolucent clear zone was seen at bone
cement interface on acetabular side and three (6%) patients
had it on femoral component. None of the patients developed
deep vein thrombosis or heterotopic bone. In post operative
period the Harris Hip Score was calculated in each case and
compared with the preoperative score to evaluate the outcome.
Significant improvement was found in Harris Hip Score after
surgery.
Key
Words:
Charnley Low Friction Arthroplasty, Primary Cemented Hip
Replacement, Harris Hip Score
J.Orthopaedics 2005;2(3)e2
Introduction
Analysis of long-term results of any operative procedure is
important for the establishment of the outcome of the procedure.
This outcome then serves as a basis for comparison of the
results of newer procedures and of non- operative treatment.
Because the rates of survival of the implant and the outcomes
associated with the various designs and procedure for total hip
arthroplasty have changed over time, the long term follow up of
series of patients is important to determine the durability and
the functions of implant over time.
In the
current study, a series of patients in whom Charnley total hip
arthroplasty with cement had been performed were followed up for
a minimum period of 5 years with a mean of seven years. The
purpose of the study was to establish the long term durability
of total hip replacement with cement using mechanically sound
prosthetic design and a hand packing technique for application
of cement. We believe a longer follow up with a large number of
patients is required as a basis for comparison of outcomes of
newer devices
and techniques
of total hip replacement.
Patients and
method
Between years 1996 to
1999, forty-seven patients had fifty total hip replacements at
Sassoon General Hospital, Pune. There were forty men and ten
women in this series. The average age of patients at the time
of index arthroplasty was sixty-five years (range fifty to
eighty years). The pre- operative diagnosis was osteonecrosis
of head of femur in 39 (78%) cases, rheumatoid arthritis in 5
(10%) cases, ankylosing spondylitis in 4 (8%) cases,
post-traumatic arthritis of hip in one (2%) case and
osteoarthritis in one (2%) case. The arthroplasties were
equally distributed between left and right hips. The Harris
Hip Score was calculated in each case preoperatively. It
indicates function of the hip joint. The maximum score is of
100 points. Points are given for pain, functional capacity,
range of movement and absence of deformity.
More the score better the
function of the hip. This score was compared with the
postoperative score to find the improvement after arthroplasty.
The indication for the surgery was pain. All patients
underwent total hip replacement only after conservative line
of management in the form of analgesic drugs, weight
reduction, use of support for walking failed to relieve pain.
The Charnley hip prosthesis was used in all patients. A
stainless steel stem with head diameter of 22 millimeter and
an acetabular cup made of ultrahigh molecular weight
polyethylene with 22 millimeter inner diameter and varying
outer diameter were inserted with polymethyl methacrylate
radio-opaque bone cement. All procedures were performed using
posterolateral approach to the hip in lateral position without
doing osteotomy of greater trochanter. After splitting the
fibres of gluteus maximus the gluteus medius is retracted to
expose short external rotator muscles of the hip. These are
divided close to their insertion and an inverted T shaped
incision is made on the joint capsule. Hip is dislocated and
femoral neck is osteotomised with oscillating power saw.
Retracting the osteotomised neck anteriorly exposes acetabulum.
Exposed acetabulum is reamed using reamers of increasing size.
Cement fixation holes are drilled in the acetabulum followed
by saline irrigation and roller gauze packing. Femoral canal
is gradually reamed with the rasps. Trial prosthesis is used
to ensure fit. Trial reduction gives idea about the stability
and range of movement. Acetabulum followed by femur is
prepared for insertion of components using manual cementing
technique. After reduction range of motion and stability are
checked. Short external rotators are reattached to femur with
drill holes. Closure is carried out over the drain.
Postoperatively
intravenous antibiotics were given for one day and drain was
removed after fortyeight hours. Aspirin was used as
prophylaxis for deep vein thrombosis. Average duration of the
surgery was two hours and average blood loss was 400 ml.
Postoperative protocol was carried out as per the
recommendations of Internal Publication No.27, Nov.1970 (John
Charnley Writhington Hospital). The limb is kept in abduction
over a pilow. The breathing exercises and static exercises of
calves, quadriceps and gluteal muscles are taught to patients
preoperatively and carried out from the first day. Patient
stands out of bed twice daily from the second postoperative
day. Patients walk with the help of walker from third
postoperative day. Range of motion exercises adduction,
adduction, flexion are taught after 3 days.
The patient is discharged
after complete rehabilitation. At the time of discharge
radiograph of the hip anteroposterior and lateral views are
taken. Patient is followed monthly for three months, three
monthly for a year and six monthly thereafter. At each
follow-up visit patient is examined clinically to calculate
Harris Hip Score and radio logically to find out aseptic
loosening.
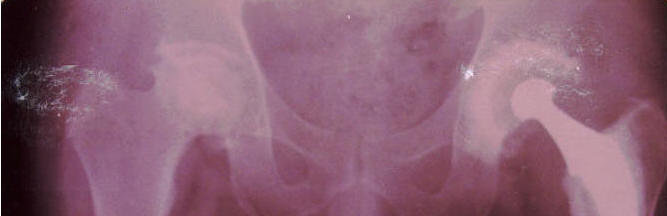
Radiographic Evaluation :
Observations were based on anterioposterior radiographs of
pelvis that had been made early postoperatively and at the
latest follow up evaluation for all patients. In addition
interval radiographs were used to determine the time that
various radiographic changes had occurred. Loosening of the
femoral component was defined according to criteria of Harris
et al. It included subseidence of femoral component, fracture
of cement or stem and presence of radioleucent line of greater
than two millimeter that had not been seen on the
immediate postoperative radiograph at the interface of
prosthesis and cement. Subsidence of femoral component was
determined using the Loudon and Charnley method. The distance
between tip of the trochanter and the tip of the stem was
measured and compared with earlier radiographs to find out
subsidence. Any bone loss in the periacetabular region that
appeared cystic was recorded, as was any localized loss of
endosteal cortex of femur. The position of the stem (varus,
valgus or neutral) was recorded on each radiograph.
Heterotopic bone when present was graded according to
classification of Brooker et al. Radioleucent lines between
cement and bone, as seen on anterioposterior radiograph were
recorded on the basis of the three acetebular zones described
by Delee and Charnley and the seven femoral zones described by
Gruen et al.
Results
At the follow up
evaluation, the average age of the patient was seventy years
(range fifty-seven to eighty-eight years). All patients were
alive till latest follow up. The minimum follow up period was
5 years and the mean follow up was 7 years. A deep infection
had developed in one (2%) of the fifty hips and two (4%) hips
had dislocated at the time of latest follow up. None of the
patients had undergone revision surgery. Before the index
arthroplasty all patients had pain. All patients had excellent
relief of pain after the total hip replacement and this was
well maintained during the course of the follow up. Only two
(4%) patients have moderate pain at the follow up.
Preoperatively 45 (90%) patients used support for walking. Of
these thirty (60%) patients used stick and fifteen (30%) used
crutches. After surgery only ten (20%) patients use stick for
walking. Deep vein thrombosis, heterotopic bone formation
occurred in none of the cases. Radiolucent lines were seen at
the bone cement interface on acetabular side in two (4%) cases
and on femoral side in three (6%) cases. These were of less
than two-millimeter width. But none of these patients
complained of pain. Subsidence of cement prosthesis or
Table 1 (Sex distribution)
|
Sex |
Number |
Percentage |
|
Male |
40 |
80 |
|
Female |
10 |
20 |
Table 2 (Indications )
|
Indication |
Cases |
|
Osteonecrosis |
39 |
|
RA |
5 |
|
AS |
4 |
|
OA |
2 |
|
Total |
50 |
Table 3 (Harris Hip Score )
|
Preoperative score |
Postoperative score |
|
Osteonecrosis |
43 |
88 |
|
RA |
45 |
82 |
|
AS |
49 |
83 |
|
OA |
47 |
87 |
| |
|
|
|
Table 4 (Complications )
|
Complication |
% |
|
Infection |
2 |
|
Dislocation |
4 |
|
Acetabular radiolucency |
4 |
|
Femoral radiolucency |
6 |
|
DVT |
0 |
|
Heterotopic ossification |
0 |
fracture of cement or stem did not occur in any of the hips. The
average preoperative Harris Hip Score in patients having
osteonecrosis of head of femur was 43 and it went up to 88
postoperatively. In rheumatoid hips the score improved to 82
from a preoperative average value of 45. In cases of ankylosing
spondylitis the average preoperative score was 49 and the
postoperative score was 83. In cases of osteoarthrosis the
average
preoperative score was 47 and it improved to 87 after total hip
replacement.
Discussion
The
present study was undertaken to know the vital role of
cemented total hip replacement in cases of osteonecrosis of
head of femur and arthritic hip joints. Osteonecrosis of head
of femur (39 cases) was the major indication in this series
followed by rheumatoid arthritis (5 cases) and ankylosing
spondylitis (4 cases). The results obtained in this series are
comparable to those obtained worldwide. In 1971,Eftekhar
followed up 205 case for 8 years (1962-1970). The sepsis rate
was 3.6% and 1.4% had loose sockets. In present study the
sepsis rate is 2% and none of the patients have clinically
significant loosening. In 1972, Charnley published the results
in 338 cases (1962-1965) followed up for 5 years.
Postoperative hip scores improved over the preoperative ones.
The sepsis rate was 3.8% and 1% had loose sockets. In 1973,
Cupic published follow up of 185 cases for 10 years
(1962-1972).The scores improved and the sepsis rate was 5% and
2% had loosening. Wroblewski studied 15 21 year follow up of
Charnley Low Friction Arthroplasty in 93 patients. 85% were
painfree. 29% showed subsidence of stem cement complex. 78%
had full range of movement. 36 hips showed socket demarcation.
It may be inferred that the results are similar to other
studies and are highly encouraging. All the patients are very
well adjusted to the changed life style required after total
hip replacement. The patients were crippled because of the
pain, loss of movements and inability to carry out day to day
activities. All the patients have shown significant
improvement in relief of pain, range of movement and
deformities. Most of the patients have resumed their jobs and
satisfied. Total hip arthroplasty is boon to the patients
crippled because of arthritis of hip, as life is movement.
References
1.Charnley J: Internal publication No.27,
November 1970, Centre for Hip Surgery.Wrightington Hospital
2.Charnley J : The long term results of low
friction arthroplasty of the hip performed as a primary intervention.
Journal of Bone and Joint Surgery, 54B: 61, 1972
3.Eftekhar NS, Stinchfielf FE: Experience
with low friction arthroplasty a statistical review of early results and
complications. Clinical Orthopaedics, 95: 60, 1973.
4.Harris WH: Traumatic arthritis of hip
after dislocation and acetabular fractures treatment by mold arthroplasty
An end result study using a new method of result evaluation. Journal
of Bone and Joint Surgery, 51A: 4, 1969
5.Wroblewski BM, Siney PD: Charnley low
friction arthroplasty of hip:
long term results. Clinical Orthopaedics, 292: 191, 1993.
|



