|
ABSTRACT
Background: The
primary concern of LSI is radicular pain and pain due to
instability. The reduction in the disk height results in
narrowing of the intervertebral foramen and there by produces
compression of the emerging root. This can be relieved to a
little extent by foraminotomy, but total correction of the real
pathological processes could be achieved by increasing the disk
height by the method of jacking of the spine so that the size of
the intervertebral foramen increases and there is indirect
decompression of root. Purpose of the study to understand the
clinical outcome regarding the radicular pain by the technique
of PLIF with distraction, instrumentation and fusion
posterolaterally.
Patients And Methods: 21 patients between 2001 and 2004
who had discectemy, PLIF with posterior distraction
instrumentation and posterolateral fusion were followed up for
an average of 16 months. There were 12 females and 9 males.
The clinical and radiological criteria of Lumbar Segmental
Instability were defined for inclusion in to the study group.
Clinical outcome was assessed VAS and Oswestry score.
Radiological assessment of fusion was done as the trabeculae
crossing intervertebral space and graft incorporation
posteriorly.
Observation And Results: 19 patients had single level
PLIF, 2 patients had double level PLIF. 14 patients had double
segment fusion posteriorly. Functional score was better in all
cases but more so in lysis without listhesis. There were no
relation between sex and rate of fusion. At 16 months average
follow up, 10 patients had graft incorporation posteriorly and 3
patients had trabeculae crossing the intervertebral disk
space. Fusion was faster at L5-S1 level. The commonest
functional spinal unit affected was L5-S1.
Discussion: LSI is a concern both for patients and
surgeons, even today. Accurate preoperative identification of
each component of the problem which produces a particular
symptom should be addressed individually for a complete relief.
The instability starts as a sclerosis of the end plates and then
proceeds on to the anterior and posterior complexes, finally
resulting in global instability, which makes the patient
symptomatic. It is the surgeons duty to intervene at any of
these stages so that, this cascade of process can be arrested at
any stage.
Conclusion:
Maintaining the disk height by a posterior instrumentation with
distraction prevents reduction of the disk height and thereby
maintaining the size of intervertebral foramen. This will help
in reducing the radicular symptoms.
J.Orthopaedics 2005;2(1)e3
Introduction
The primary concern of the
Lumbar Segmental Instability (LSI) is radicular pain and pain
due to instability. The radicular pain can be addressed to a
little extent by foraminotomy. But, there is narrowing of the
intervertebral foramen, which results partly from narrowing of
the disc space, which reduces the size of the foramen. Jacking
of the disk space and maintaining the disc height, increases the
size of the intervertebral foramen indirectly. This can be
achieved by posterior distraction, instrumentation, which can be
combined with PLIF and postero lateral fusion. There is a
controversy regarding the subsequent degeneration of the
adjacent motion segments(7). In this method, adjacent motion
segments may also be included in the fusion mass. A prospective
study was performed to determine the clinical outcome of the LSI
treated with posterior discectemy, PLIF and posterolateral
fusion with instrumentation. Laminar hooks were used in all
cases universally. No pedicular screws were used in any case.
The abnormal motion segements were usually included in the
fusion mass(5). But this predisposes to excessive stress in
the adjacent motion segments. Abnormal motion segments adjacent
to the segments which is fused are subjected to excessive stress
which results in increased disc degeneration(6). And this will
lead to symptoms like radiculopathy, discogenic pain, spinal
canal stenosis and facet joint induced pain. The aim of the
study to understand the functional outcome regarding the
improvement of symptoms and understand whether fusion could be
attained anteriorly and posteriorly. The technique of jacking
up of the disc space, to maintain the disc height and indirectly
enlarging the neural foramen and its clinical outcome regarding
radiculopathy was specifically looked for.
Patients and
method
Between July 2001 to August
2004, twenty-one patients who had PLIF with posterior
instrumentation and posterolateral fusion were followed up. All
cases were done by a single surgeon at a premier teaching
institute in south India (Calicut Medical College). Patients
between the ages of 22 to 58 were selected irrespective of
sex. All cases with Lumbar segmental instability were
selected. Posttraumatic and cases with infection and neoplasm
were excluded. The clinical test for Lumbar segmental
instability was a criteria for inclusion. The radiological
criteria for LSI were more than 4 mm saggital translation and
more than 10-degree saggital rotation angle. Cases with
spondylolysis without listhesis , spondylolistheses, post
operative LSI with progressive scoliosis, recurrent disk
prolapse at the same level. Persistent radicular and non-radicular
pain, in whom the clinical and radiological criteria of
instability was present were included. Adjacent functional
spinal units were looked for instability and radiculopathy.
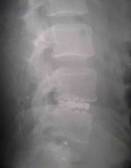
Figure-1
The surgical technique was
disk excision, posterior instrumentation with laminar hooks with
distraction and jacking of the disk height along with PLIF at
abnormal functional spinal units with facet joints and inter
transverse fusion. Expandable stand-alone cages were used
wherever possible. Standing AP, Lat, flexion-extension
lateral, and rotation lateral views were taken pre
operatively. In the lateral X ray, neutral flexion and
extension were measured for AP translation, disk height and
saggital rotation angle at the abnormal functional spinal
units. LSI due to degeneration was classified according to
University of California at Los Angeles grading scale. Grade I
No disc degeneration; Grade II Mild, Grade III Moderate,
Grade IV Severe. Grade III and IV were only included in this
study. The radiological involvement of the intervertebral disk
were assessed with Saraste Classification (Table 1) (8).
|
Stage I A |
Normal disk height
without dehydration |
|
Stage I B |
Normal disk height
with dehydration |
|
Stage II |
Disk height decreased
by less than 50% |
|
Stage III |
Disk height decreased
at least by 50% |
|
Stage IV |
Disk height
obliterated |
Table-1
Stages II, III and IV were
included in this study. The variables like age, sex, pre op
degree of LSI were compared with the post op results.
Diagnostic variables were assessed with functional outcome.
Pre op functional evaluation was done with visual analogue scale
and Oswestry score.
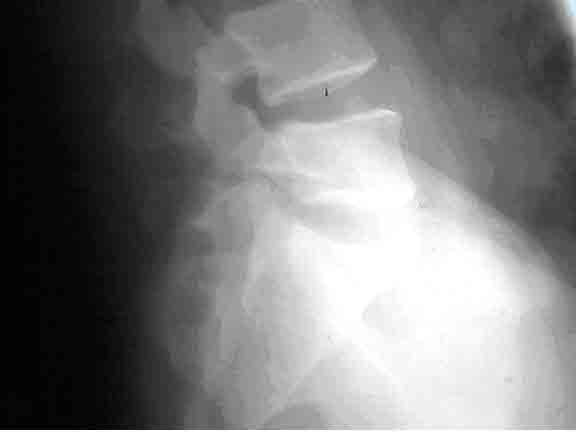
Figure-2
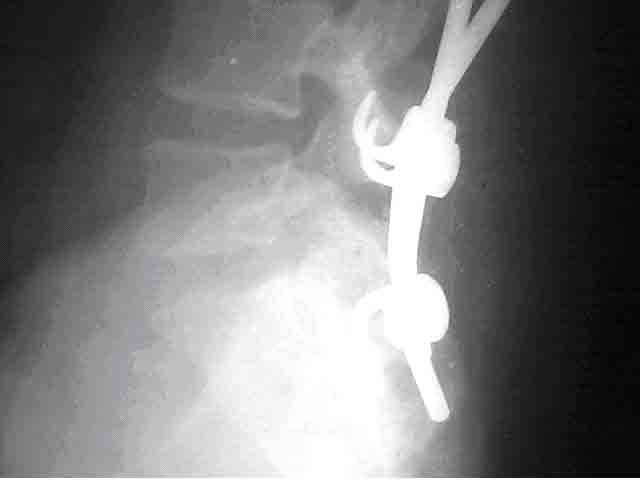
Figure-3
The patients were regularly followed up with
clinical and radiological assessment and persistence of symptoms
work status functional status, pain medication, neurological
status was documented. Fusion was assessed radiologically as
trabeculae crossing intervertebral disk and graft incorporation
posteriorly.
Results
The study group included 21
patients with 12 females and 9 males. The average age was 40
(Range 22-58). The average duration of follow up was 16 months
(ranging from 4 months to 28 months). All cases were operated
PLIF with minced Iliac crest graft, Posterior instrumentation
with posterolateral fusion, except in one case treated with
expandable cage, PLIF and no posterior instrumentation along
with posterolateral fusion with floating intertransverse bone
graft. 2 patients had double level PLIF. Posterolateral fusion
was done in 2 levels in 14 cases, 3 levels in 6 cases and 4
levels in 2 cases. Single level PLIF was done in 19
cases. The instrumentation extended 4 segments in 2 cases, 3
segments in 6 cases, 2 segments in 14 cases. Single level
posterior instrumentation was not done in any cases. The
condition of the adjacent spinal units were abnormal cephalad
single level 14 patients, caudad and cephalad one each in 6
cases, abnormal caudad 1 and cephalad 2 cases. Number segments
to be included in the fusion mass depended on the pre operative
assessment. The clinical tests for segmental instability were
positive in all cases. Sagital translation was 5 mm in 3 cases,
8 mm in 12 cases and 10 mm in 6 cases and 11 mm in 1 case.
Saggital rotation angle was 12 degrees in 3 cases, 14 degrees in
13 cases, 15 degrees in 6 cases. Average disk height was 7 mm
pre operatively. Average disk height post operatively was 13
mm.
|
Spondylolysis without
listhesis |
12 |
|
Spondylolisthesis |
6 |
|
Post Operative LSI |
1 |
|
Progressive scoliosis
with LSI |
1 |
|
Persistent radicular
pain |
1 |
Table-2
Duration of time needed for
fusion 16 months in 10 cases of fusions attained posteriorly, 3
patients in the same duration developed interbody fusion.
Laminar hooks and rods were used in all cases. Expandable cage
in one case, cross-links were used in all cases. Routine
posterior decompression, foraminotomy, posterolateral fusion
were done in all cases. Radiologically trabeculae crossing the
intervertebral disk were seen in 3 cases and graft incorporation
posteriorly was seen in 10 cases. Average pre op VAS (visual
analogue scale) 80% , post operative VAS 30%. Pre op Oswestry
scope 35, and post op 85. No significant correlation between
the age and fusion were obtained. (P = >0.35) There was no
relation between the sex and fusion. There was a relation
between diagnosis and fusion fusion was better with
Spondylolysis without listhesis. P=<0.01). functional outcome
was better in cases of Lysis without listhesis (n=12). VAS pre
op 90% and post op VAS 20%. Oswestry Pre op 30 and post op
95. Functional assessment for spondylolistheses VAS 75% pre
op, 35% postop. Oswestry pre op 40, post op 80. Oswestry and
VAS were improved in the cases were adjacent functional spinal
units were included in the fusion mass. Commonest functional
spinal unit affected was L1 (14 cases) and in L4-5 in seven
cases.
Discussion
Lumbar segmental
Instability is a concern both for patients and surgeons even
today. Accurate pre op identification of each component of the
problem, which produces a particular symptom, should be
addressed individually for a complete relief. Instability in a
particular functional spinal unit starts as sclerosis of the end
plates with disk space narrowing, initial hypertrophy of the
ligament of flavum and PLL. Later on there is translation
listhesis, and angulations indirectly narrowing the
intervertebral foramen and compressing the root, which may
result in spinal canal stenosis, facet joint arthritis, capsular
ligament laxity of the facet joint with facetal instability
resulting in facet induced pain and discogenic pain and
claudication and neurological deficit from global spinal
instability in a particular functional spinal unit. It is the
surgeons duty to intervene at any of these stages to reverse
this cascade of processes, so that the symptoms can be
reversed. Instability should be addressed by instrumentation,
which later on should be taken over by fusion both interbody and
posterolaterally. Otherwise, the implant will fail in the long
run. Canal compromise should be addressed by decompression.
In this study, stress is given to maintain the disk height by
the technique of jacking up the disk space so that this will
indirectly increase the size of the intervertebral foramen and
decompressing the root, thus relieving the radiculopathy.
Adjacent functional spinal units are usually abnormal and should
be included in the fusion mass to avoid re operation for LSI at
the adjacent functional spinal unit. Accelerated degeneration
of the adjacent segments was described in literature(1,2,3,5).
Once a particular functional spinal unit is fused, more stress
occurs at the adjacent spinal unit, accelerating degeneration
and LSI(4).
42.9% of patients were
males, 57.1% were females. Females were commonly affected
(n=12). 90.5% patients with single level PLIF and 9.5%
patients with double level PLIF. 95.6% were treated with
posterior instrumentation, PLIF and PL fusion. 4.7% were
treated with anterior stand-alone cage and posterior floating
graft without posterior instrumentation. The common LSI was at
L5-S1 level (n=14). (66.7%). At 16 months average follow up
14.2% fusion achieved in PLIF. 47.6% fusion achieved
posterolaterally. 8 out of 10 cases of posterolateral fusion
were at L5-S1. Three out of 21 cases of fusion were at L5-S1
anteriorly. 80% of posterolateral fusion attained was at
L5-S1. 66.66% of fusion by PLIF was at L5-S1. Early fusion
was seen at L5-S1 compared to L4-5 , probably due to better
mechanical stabilization to the sacrum, which is immobile.
57.1% of the cases were spondylolysis with listhesis. 28.5%
cases were spondylolistheses. L5-S1 level (n=14) were commonly
affected 66.7%. L4-5 (n=7) was affected in 33.33% of cases.
VAS improved from 90% to 20% in Lysis without listhesis.
Distraction instrumentation helps in
maintaining the disk height results in preventing the
compression between the 2 vertebrae, which results in further
narrowing of the disk space and foraminal narrowing. The
traditional method of pedicular screws used to compress the
vertebrae together reduces the disk height that narrows the
intervertebral foramen. This could be a reason for persistent
radicular symptoms even after achieving solid fusion. The
better symptomatic results in this study may be due to either
decompression of the root or decompression of the dura but this
could also be due to a short term nature of the study and only
by a long term follow up any further conclusion could be made.
Conclusions
Maintaining the disk height by a posterior
instrumentation with distraction prevents reduction of the disk
height and thereby maintaining the size of intervertebral
foramen. This will help in reducing the radicular symptoms.
References
1)Brodsky AE. Post laminectomy and post
fusion stenosis of the lumbar spine. Clin Ortho. 1976; 115:130-9
2)Lehmann TR, Spratt KF, Tozzzi JE. Weinstein JN, Reinarz SJ,
el-Khoury GY. Colby H. Long term follow up of lower lumbar
fusion patients. Spine 1987; 12:97-104
3)Leong JC, Chun SY, Grange WI, Fang D. Long term results of
lumbar intervertebral disc prolapse. Spine. 1983;8:793-9
4)Mlyakoshi N, Abe E, Shimada Y, Okuyama K, Suzuki T, Sato K.
Outcome of one-level posterior lumbar interbody fusion for
spondylolistheses and postoperative intervertebral disc
degeneration adjacent to the fusion Spine. 2004;25:1837-42.
5)Whitecloud TS 3rd, Davis JM, Olive PM. Operative treatment of
the degenerated segment adjacent to a lumbar fusion. Spine.
1994; 19:531-6
6)Quinnell RC, Stockdale HR. Some experimental observations of
the influence of a single lumbar floating fusion on the
remaining lumbar spine. Spine. 1981;6:263-7.
7)Pope MH. Wilder DG, Matteri RE, Frymoyer JW. Experimental
measurements of vertebral motion under load. Ortho Clin North
Am. 1977; 8:155-67.
8)Saraste H, Brostrom LA, Aparisi T, et al. Radiographic
measurement of the lumbar spine. Aclinical and experimental
study in man. Spine 1985; 10:236-41.
|





