|
Key words:-Expansile spinal cages
, Lumbar segmental instability , PLIF, minimally invasive
BACKGROUND
Lumbar segmental instability ( LSI) is
commonly treated with PLIF using conventional cages supported
with posterior instrumentation which requires extensive tissue
dissection and removal of lamina, ligaments and facet joints-
which are posterior stabilizing structures. It also needs dural
retraction to make way for the large cages which are introduced
through the posterior aspect. So there is increased risk of
dural laceration and neural damage. The conventional cages often
need posterior instrumentation.
There has always been a quest for minimally
invasive spinal spacers which can be used as a stand alone
implant. The new Expansile Spinal Cages (ESC) requires little
or no removal of the lamina and less of dural retraction. At the
time of insertion the cage is only 5 mm in size and at the end
of expansion it is 15 mm in size. Since it is only 5 mm at the
time of insertion most of the posterior structures are kept
intact. The fins of the system pierces the end plate and gets
anchored to the vertebral body-stabilizing them. The remaining
space is filled with bone graft minced iliac crest graft.
The whole construct acts as a stand alone cage.
INTRODUCTION
Since the existing cages require removal of
most of the posterior stabilizing structures, a cage which could
achieve PLIF with less of destabilization of the posterior
structures was sought after. The ESC is a relatively newer
surgical technique which can achieve PLIF with minimum tissue
dissection and is surgeon friendly. In this article stress is
given to describe the surgical technique of ESC by describing
it in a single patient with 12 month follow up.
Lumbar segmental instability is manifested
by progressive collapse of the disc space with reduction in size
of the intervertebral foramen, hypertrophy of the ligamentum
flavum and posterior longitudinal ligament with eventual facet
joint arthritis / instability. The final result is
spondylolysthesis or retrolysthesis. The mechanical
alterations result is discogenic and facetal induced pain
leading to compressive radiculopathy. A solution to the problem
requires reversal of these processes which includes expansion of
the disc space to increase disc height. This will indirectly
increase the size of the intervertebral foramen. In this study
Jacking up the disc space is the term used which means the
process of increasing the disc height by using expansile spinal
cage. The result is stabilization of the unstable segment in a
balanced alignment to ensure gradual intervertebral fusion.
PLIF becomes biomechanically sound with ESC
because it helps in removal of the disc, restoration of disc
height, relieves the foraminal stenosis and positions the graft
along the weight bearing axis.
Application of this technique was
introduced by Briggs 1 et al in (1944) and Cloward2 (1945). But
the result were not promising. Bagby3 et al introduced the
concept of cage support which help in neutralization of
compressive faces while providing three dimensional stability
that is essential for sound fusion. These devices have many
shortcomings
It has to be large enough to cause tension
in the annulus which is needed for stabilization. Because of the
size of the implant very often excision of the facet is needed
which reduces posterior stability. Often it has to be
supplemented with posterior instrumentation. Because of the size
of the cage heavy retraction may result in dural damage / tear
and eventual epidural fibrosis.
AIM
To highlight the surgical technique of
expansile spinal cage with presentation of a single case.
METHOD
The device is made of titanium. When
collapsed the fins are enclosed in a cylinder with a diameter
of 5 mm. Following expansion the cage in 15 mm in diameter and
25 mm in length. The final configuration is trapezoid. There
are three available sizes 9.5 / 11 , 11.5 / 13 , & 13.5 / 15.
the selection is made pre op and confirmed intra operatively. At
the end of the procedure the device self locks. The delivery
system is single use. The instrumentation system consists of
rectangular curette which can be used as a measure of the
diameter and for scratching the end plates till it bleeds. There
is a trial implant which can be used for measurement of length.
There is a special sheath with cannula for the introduction of
the graft into the disc space.
The procedure consists of routine posterior
approach with patient in the lateral decubitus position with
flavectomy, discectomy and end plate curettage which is done
until it bleeds. The space is filled with minced iliac crest
bone graft through the sheath which has a diameter of 5 mm. The
ESC is introduced into the space and expanded. Adjustment can
be made after expansion of the first fin if needed. No
drilling/tapping/ hammering or screwing is needed. The cage is
either stand- alone or with bone graft. Posterior
instrumentation is done in old facectomies.
Pre op radiographic evaluation includes
routine AP and lateral X- rays, stress X rays and MRI scans.
In the X-rays one should look for intervertebral disc height,
end plate sclerosis, subchondral cysts, lysthesis and facet
joint arthritis. In the stress views sagittal rotation angle,
sagittal translation distance are the signs of lumbar segmental
instability. Post op radiological assessment should include
measurement of disc height and positioning of the cage. The
fusion criteria should include:
►No radiolucent
gap at the device vertebral end plate interface.
►Bridging trabeculae across the
vertebral bodies.
►No evidence of mobility in the stress
X- rays.
A 42 year old patient was selected who
had IVDP at L4 -L5 level who was operated upon by another
surgeon 3 yrs back in the form of laminectomy and discectomy. 3
yrs back the patient presented to the same surgeon with acute
IVDP with pain radiating down the left leg. MRI showed
posteriolateral disc prolapse at L4 L5 level, L5 root lesion
in the form of EHL, EDL weakness. SLR at the time of first
presentation was positive at 400. sensory findings were confined
to L5 dermatome.
Following the first surgery the patients
symptoms did not improve and actually worsened.
VAS ( Visual Analog Score) at the time of
presentation to us was 90 and Oswestry disability index was
80%. The patient could not move about and could not do daily
activities.
At the time of presentation patient had
severe LBA radiating to left leg , with EHL / EDL paralysis , L5
dermatomal sensory loss. There was no sphincter involvement. SLR
was positive at 200, Bowstring test and Braggard test were
positive. Routine radiographs showed disc space height of 7mm.
There was end plate sclerosis, grade 1 listhesis and facet
joint arthritis.Stress views showed sagittal translation
distance of 4 mm and sagital rotation angle of 250 in static
lateral view.
A diagnosis of LSI was made with IVDP L4
-L5 level. Abnormal functional spinal unit was identified at L4
L5. MRI confirmed the findings of huge posterolateral disc
prolapse at L4 L5 level. The patient was treated with
re-exploration which included mobilization of dural sac from
scar tissues and discetomy at L4 L5. end plates were
curetted till they started to bleed. The disc space was filled
with minced iliac crest graft and the expansile spinal cage was
introduced into the disc space. Up to 12 mm of the rectangular
curette could be easily rotated and 11.5 / 13 mm lordotic cage
was selected and expanded in the disc space. Posterior fusion
with floating intertransverse graft was done with no posterior
instrumentation.
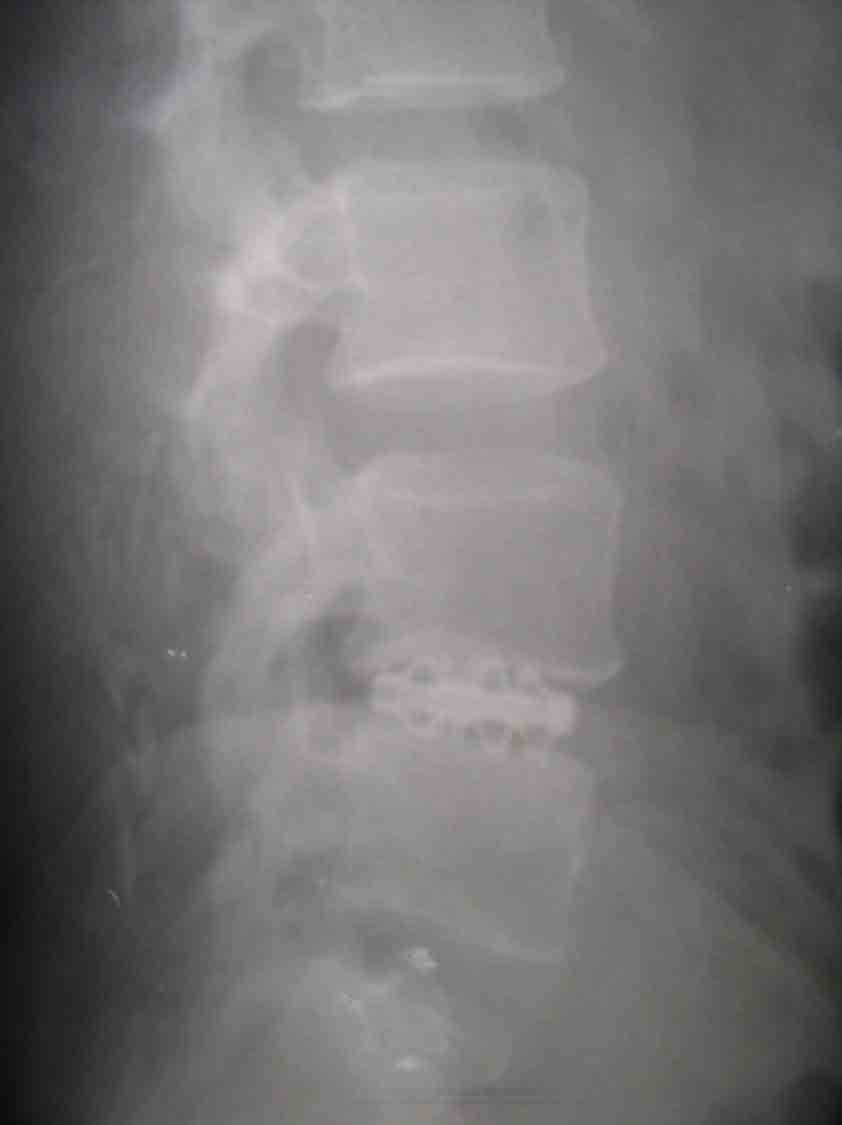
Post op the patient was mobilized with
spinal support on the 7th day. Post op X-ray showed a disc
height of 13mm, equal opening out of anterior and posterior disc
spaces, sagittal rotation angle and sagittal translation
distance returned to normal. At the latest follow of the patient
at 12 months the VAS was 10% and oswestry disability index was
20%.
Early radiological fusion was in the form
of trabecular crossing the vertebral end plates and there was no
radiolucent gap between the endplates and cage. Improvement of
VAS was by 70% and of oswestry disability index was
by 60%.
DISCUSSION
PLIF is commonly advocated as a method of
treating mechanical low back pain including LSI. 70-80 % fusion
rates and patient satisfaction are reported in
literature5,7,8,9. 75 90% return to work is also reported.
Expansile spinal cages have the potential to achieve similar
results which less invasive techniques. The biomechanical
properties of ESC were designed to provide immediate mechanical
fixation in all planes. The constraints of flexion and lateral
bending are mediated by the annulus. This is attained by
distraction of the disc space by the ESC. This only involves
Jacking up mechanism. The stability in the axial plane is
credited to the limited invasiveness of the surgical procedure
which makes it possible to preserve the main stabilizers in the
axial plane- namely the facet joints and the annulus
fibrosus4,10. Our main concerns were in regard to the
penetration of the end plates by the fins and the possibility of
implant migration. The subsidence in this patient was 0.22mm.
This did not jeopardize the stability of the ESC. The
engagement of the fins into the vertebral end plates provided an
element of resistance against migration. The quality of the bone
really determines the anchorage of the fins into the endplates.
So the results may be poor in patients with osteoporosis, this
patient did not have osteoporosis.
Any stabilizing construct is bound to fail
if fusion does not occur. In our patient fusion was established
at 12 months in plain X- rays. The results of ESC may be better
because of relatively small implant end plate contact area,
this will leave a large area free so that the bone graft is in
contact with the bone; enabling bone to bone contiguity without
having to depend upon bone growth into and through the implant
as in the case of conventional cages. It is important to do
meticulous curettage of nucleus pulposus so that it may promote
fusion . Installation of the cage is equally important.
In this patient radiolucencies at the
implant end plate interface were not there which means that
fusion is already occurring. Stress views did not demonstrate
any instability. The length of the implant and its contouring
may preclude radiological assessment of fusion. It is to be
stressed that the merit of the ESC is the relative freedom from
complication encountered with traditional cages. Although PLIF
is an accepted surgical option its record of complications are
very high. PLIF with conventional cages is reported to have
major complication in 45 % and re-operation in 25-45% of
patients.
CONCLUSION
ESC may be an option in the future as the
complications conventionally seen with conventional cages are
absent with ESC.
REFERENCES
1. Briggs H,Milligan P.R Chip fusion of the
low back following exploration of the spinal canal JBJS
1944;26:125-130.
2. Cloward RB. New treatment for ruptured
intervertebral disc.Presented at annual meeting of Hawaai
territorial medical association may 1945.
3. Bagby GW Arthrodesis by the distraction
compression method using a stainless steel implant Orthopaedics
1988:11:931-934.
4. Albumi K ,Panjabi MM.Kramer K et al.
Biomechanical evaluation of lumbar spinal stability after
graded facetectomies Spine 1990:15:1142-1147.
5. Brantigan JW, Steffee AD,Lewis ML et al.
Lumbar interbody fusion using the Brantigan I/F cage for PLIF
and the variable pedicle screw placement system Spine
2000:25:1437-1446.
6. Jun BY. PLIF with restoration of lamina
and facet fusion Spine 2000:25:917-922.
7. Agazzi S,Reverdin A,May D PLIF with
cages: an independent review of 71 cases: J neurosurgery 1999
91:186-192.
8. LEE CK,Vessa P,Lee JK . Chronic
disabling LBP syndrome caused by internal disc derangements.The
results of disc excision and PLIF Spine 1995,20:356-361.
9. Schechter NA,France MP,Lee CK . Painful
internal disc derangement of the lumbar spine:discographic
diagnosis and treatment by PLIF Orhthopaedics 1991:14:447-451.
10. Krismer M,Haid C, Rabl W.the
contribution of annulus fibres to torque resistance Spine
1996:21:2551-2557.
|



