|
Abstract:
This study was conducted to know whether light handles are contaminated in the orthopaedic operation theatres, their frequency of contamination and to know whether surgeons should change their gloves every time they touch the light handle. The study was done from November 2010 to December 2010 at Blackpool Teaching hospital. The culture swabs taken from light handles during pre-operative,intra-operative and post-operative period from a single laminar flow operating theatre. A total of 40 cases were selected for study.
Most of our cases were primary hip and knee replacement.
Three culture swabs were taken for each case from light handles. . All the swabs were taken by operating team within the laminar airflow area. The swabs were cultured into blood agar /Mcconkey medium and incubated for 48 hours at 37 degree Celsius aerobically for 48 hours.
None of the swabs showed any bacterial contamination which shows light handle is not a source of intraoperative contamination .we conclude that light handle is not a source of contamination in operation theatres and hence surgeons need not change their gloves each time after handle the light handle .
J.Orthopaedics 2012;9(2)e7
Keywords:
handles;contamination;orthopaedic theatres;culture swabs,laminar flow
Introduction:
Bacterial contamination in operation theatres can be a source of infection in post-opreative patients and can have devastating effect on patient. There are publications about various sources of contamination in a clean air operation theatre. The contamination which occurs at tip of suction and skin blades has been well recorded.
There is a major controversy regarding light handle contamination. One study2 shows 14% contamination and other study1 shows 0% contamination rate.
The operation theatre light by its massive size can obstruct laminar air flow and can create eddies of current and can cause bacteria in air to get deposited around the light handles and that in turn can cause contamination of the surgeons gloves when they handle the light handles during operation and is a potential source of post operative infection.
Our aim in this study is to assess the frequency of contamination of light handle, identify organism, and formulate the pathway for contamination and suggest change in current practise of changing the gloves every time surgeon manipulates light handle.
Patients and methods
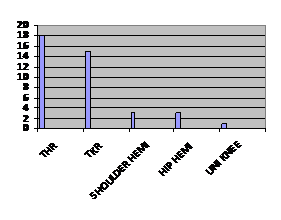
A total of 40 cases were selected for study during a period from November 2010 January 2010. All of our cases were primary hip and knee replacement. Other cases included shoulder hemiarthroplasties and hip hemiarthroplasties.. There were 18 cases of THR, 15 of TKR, 3 shoulder hemiarthroplasty and one case of unicompartmental knee replacement.
The cases were done by five operating surgeons, which included 3 consultants and 2 staff grade doctors. In 19 cases consultants were the primary operating surgeon and rest of the cases staff grades were the primary surgeon which in most of the cases were done under the supervision of a consultant. All the procedures were done in an ultra clean air theatre with vertical laminar airflow. A body suit exhaust system was not used in any operation. The surgeons and staff wore impermeable gowns for all the cases. All the patients received prophylactic antibiotics preoperatively at time of induction.Thirtysix patients received Flucloxacillin and Gentamycin and 2 patients who had Penicillin allergy received Cefuroxime.
The duration of procedure and number of times the light handle was manipulated for each case was recorded.
Three culture swabs were taken for each case from the light handles. We only took swabs from the body of the light handle as this is the only area which comes with direct contact with the surgeons/assistants gloves. The first swab was taken immediately after the light handle was attached. The second swab was taken intraoperatively and the final swab was taken at the end of the operation. Surgeons did not change their gloves after handling the light handles.
All the swabs were taken by the operating team within the laminar airflow are, put in a closed container and transported to microbiology lab. The swabs were cultured into blood agar /mcconkey medium and incubated for 48 hours at 37 degree Celsius aerobically for 48 hours.
Results
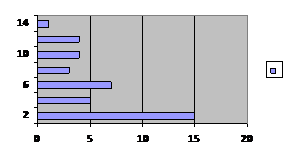
The male female ratio included in study was 1.4:1, 23 males and 17 females. The average age of patient included in study was 71.2 with a range from 38-96 yrs.The average duration of procedure was 1.21 hours and median of 1.3 hours. .the range was from .50 minutes -1hr 30 minutes.The average number of times the light handle was manipulated was 5.5 times with a range of 1-14 times and a median of 2.
Graph showing frequency of light handles being manipulated in x-axis and number of cases in x axis
It was noted that preoperative antibiotic was given to all patients as per hospital protocol. None of the swabs taken preoperatively and intraoperatively showed bacterial contamination. . None of the primary joint replacements developed any contamination. The patients in the study were followed up for 3 months postoperatively and there is no evidence of infection and their fractures are healing. Our study results show that there is no contamination of light handles in any of the cases.
Discussion
The introduction of ultraclean air operating theatre had reduced prevalence of postoperative infection from 9% to 1%3.in 1972 Charnley concluded that clean air was most important factor but not the sole reason for reduction in prevalence of infection .Subsequent studies have shown that prophylactic antibiotic was most single effective measure in reduction in prevalence of infection3,7 .
Some of the recent studies show that laminar airflow does not confer any advantages over conventional operating suit 8 .
N.Daviss2 study showed a high rate of light handle contamination around 14.5% followed by suctiontipnd other operative equipments. A further study of suction tip contamination4 has confirmed this high rate. But controversy exists on light handle contamination as another study by J R Huessin1 who studied only 15 cases showed that he had 0% contamination.
Our study found that there was no risk of contamination from the light handle. There is no need for changing the gloves every time we handle the light handle .The study suggests that light handle may not be a good surface for bacterial adhesion and therefore very low risk of surgical contamination while handling it.
Reference:
- Use of light handles in the laminar flow operating theatre--is it a cause of bacterial concern?--. R. Hussein, R. N. Villar, A. J. Gray, and M. Farrington- Ann R Coll Surg Engl. 2001 September; 83(5): 353354
- Intraoperative bacterial contamination inoperations for joint replacement-N. Davis, A. Curry, A. K. Gambhir, H. Panigrahi, C. R. C. Walker,E. G. L. Wilkins, M. A. Worsley, P. R. Kay -J Bone Joint Surg [Br] 1999;81-B:886-9.
- Effect of ultraclean air in operating rooms on deep sepsis in the joint after total hip or knee replacement ,a randomised study
- -O M Lidwell,E J Lowbury,W Whyte,R Blowers,S J Stanley,D Lowe-British medical journal,volume285,3 july1982
- Suction during orthopaedic surgery ,how safe is suction tip?- Panagiotis GIVISSIS, Dimitrios KARATAGLIS, Petros ANTONARAKOS,Panagiotis D. SYMEONIDIS, Anastasios CHRISTODOULOU- Acta Orthop. Belg., 2008, 74, 531-533
- Postoperative infection in total prosthetic replacement arthroplasty of hip joint-Charnley J,Efthekar NBr J Surg Engl 1993;75;254-6.
- Hanley JA, Lippman-Hand A. If nothing goes wrong, is everything alright? JAMA 1983; 259: 17435.
|




