Address for Correspondence:
Bernard C.S. LEE
Department of Orthopaedic Surgery
Alexandra Hospital (Jurong Health Services)
378 Alexandra Road
Singapore 159964
Phone: +65 97219583,
Email: bernardleecs@gmail.co
Abstract:
We describe a novel way of treating secondary osteonecrosis (ON) of the femoral head and condyles with cell-therapy. This method is simple, has low morbidity and does not affect the local anatomy in a manner that might complicate subsequent surgery. Three patients (four hips) with femoral head ON and two patients (three knees) with femoral condyle ON were treated with core decompression and debridement of the osteonecrotic area and grafting with HEALOS FX Injectable Bone Graft Replacement. The patients were assessed pre-operatively and at 12 months to compare pain (Visual Acuity Scale), function (WOMAC score), and radiological progression (Aglietti and FICAT). All the knees and all but one hip with osteonecrosis showed improved pain and function scores at 12 months, with the exception having an intra-operative complication. Patients with stage 3 osteonecrosis progressed to stage 4 radiologically at 12 months. Our early results demonstrate that this technique may prove a viable option in the treatment of early secondary osteonecrosis of the femoral head and condyles.
J.Orthopaedics 2011;8(4)e15
Keywords:
Osteonecrosis; Cell therapy; hip; knee; bone graft
Introduction:
Secondary osteonecrosis (ON) has been associated with conditions such as chronic corticosteroid use, alcohol abuse and systemic lupus erythematosus. The lesions are commonly bilateral and multifocal, often affecting the femoral head as well as the femoral condyles. ON of the femoral head is a painful disorder that often progresses to femoral head collapse and secondary osteoarthritis requiring total hip replacement. Likewise ON of the femoral condyles gives rise to painful destruction of the articular surface with resultant osteoarthritis of the knees.
Early treatment of femoral head ON traditionally involves core decompression but results have been mixed. Whilst most patients have early pain relief, many patients often progress to femoral head collapse and secondary osteoarthritis. Mont’s review of the literature showed a clinical success rate of only 53% with core decompression alone.1
The search for a treatment option that would prevent disease progression has led to the combined use of core decompression and vascularized fibular grafting in an attempt to provide living bone to replace the necrotic bone. This, however, has significant donor site morbidity and often alters the local anatomy of the recipient site, thus complicating future surgery should the need arise. Subsequently, interest has shifted towards the use of autologous bone marrow grafting and the use of mesenchymal stem cells to further improve the clinical results and prevent progression of the disease.2,3
We previously reported the use of Cell Therapy with the Cellect DBM system (DePuy Spine Inc.) in the treatment of ON of the femoral condyles in 3 patients, with encouraging results.4 This system utilized a bone marrow aspiration and concentration technique on a scaffold of demineralized bone matrix and allograft cancellous croutons. At 2 years, all 3 patients had no complications and excellent results with near-normal function and activity levels.
In this study, we used the HEALOS Fx Injectable Bone Graft Replacement (DePuy Spine Inc.) in the treatment of both ON of the femoral head and condyles.
Material and Methods :
This is a preliminary review of the short-term results (12 months) of 3 patients (4 hips) with secondary ON of the femoral head and 2 patients (3 knees) with secondary ON of the femoral condyles that was treated with core decompression and osteoprogenitor cell therapy using grafting with the HEALOS Fx system. All the patients had preoperative magnetic resonance imaging (MRI) of the affected joints for confirmation and assessment of the disease severity.Autologous Bone Marrow Harvesting and Graft Preparation Bone marrow was harvested from the iliac crest via a small stab incision just posterior to the anterior superior iliac spine, using the supplied 3-hole aspiration needle. A total of 10ml of marrow was aspirated from multiple sites in the ilia crest. Only 2 to 4ml of marrow was aspirated from each site so as to avoid the dilution with peripheral blood, as was shown by Muschler et al.5
The bone marrow aspirate is then syringe-pumped into a graft mixing and delivery device to concentrate the bone graft and produce a moldable, injectable matrix comprising osteoprogenitor cells on a scaffold of cross-linked Type-1 collagen fibers that are hydoxyapatite coated. This matrix provides a 3-dimensional mineralized structure with a composition similar to human bone that favours osteoprogenitor cell attachment and bone ingrowth. Core decompression and autologous bone graft transplantation For the femoral condyles, a direct medial and lateral approach was used under image intensifier guidance. Necrotic bone material was curetted and irrigated from the femoral condyles via a cortical window. The defect was then packed with the prepared graft material. The patients were postoperatively instructed for toe-touch weight-bearing for 6 weeks, followed by full weight-bearing thereafter.
For the femoral heads, a cortical window was obtained in the lateral aspect of the base of the greater trochanter, and a guide wire was placed in the necrotic area under image intensifier guidance. Necrotic bone was then removed with a 10mm or 12 mm bone-tunnel reamer. The graft was then injected via a syringe into the defect where it molds to the walls of the bone tunnel. Patients were not allowed to weight-bear postoperatively for 6 weeks.
The patients were reviewed at 12 months to compare pre-operative and post-operative pain (Visual Acuity Scale, VAS), function (WOMAC score), and radiological progression (Aglietti and FICAT).
Results :
The patients’ demographics are shown in Table 1. All of the patients have been on treatment with long-term steroids.
Osteonecrosis of the knee
There were improvements in the mean Knee Society Score and Knee Society Function Score as outlined in Table 2. In addition, the mean VAS score improved from 6.3 pre-operatively to 0.7 after 12 months of follow-up. Radiological progression of the osteonecrosis was evaluated using the 5-point staging system suggested by Aglietti.6 Two knees with stage 3 ON continued to have medial femoral condyle collapse to stage 4 on follow up, whilst the third knee with Stage 3 ON of the posterior condyle also progressed to stage 4.
Osteonecrosis of the hip
Following decompression and autologous bone marrow grafting on the femoral head, the visual acuity score (VAS) for pain as well as WOMAC hip scores showed marked improvement in 3 hips.(Table 3) One patient had failure of treatment due to a surgical complication that will be discussed subsequently.
Radiological assessment was done using the FICAT system. Of the three successfully treated hips, all had FICAT Stage 2 ON. There was no radiological progression in two joints, and in the third there was progression to Stage 3. Pain and function scores in the latter hip however, showed marked improvement on follow-up.
The third patient who was treated for hip ON continued to progress from Stage 3 ON to Stage 4 with further collapse of the femoral head and subluxation of the hip joint. During the surgical procedure, there was perforation of the subchondral bone during the reaming process, which is known to be a cause of early collapse of the femoral head. While she had initial improvement of pain (VAS from 8 to 2) and function immediately after the procedure, she subsequently developed worsening symptoms (VAS 2 to 8, and WOMAC 51.6 to 36.7) on follow-up due to progressing osteoarthritis.
Discussion :
The current understanding of the pathophysiology of ON suggests that a decreased concentration of mesenchymal stem cells, and hence a decrease in the number of osteoblastic cells, results in decreased bone reparative function. Indeed, ON has been shown to be associated with low MSC levels, especially in patients on long-term corticosteroid therapy or alcohol abuse.7,8 Glucocorticoids are believed to inhibit osteoblastogenesis and promote apoptosis of osteoblasts and osteocytes.9,10
ON is also believed to arise from ischaemia resulting from fat emboli, microvascular tamponade of femoral head blood vessels by marrow fat, retrograde embolization of marrow fat, and intravascular coagulation. This affects the capillaries providing the precursor cells needed for bone healing. ON has thus been deemed a vascular as well as bone disease.11
Subsequent techniques in treating ON have thus been based on treating the pathophysiology. Autologous bone-marrow transplantation was first reported in treating osteonecrosis of the humeral head in a patient with sickle-cell disease in 1997.12 Since then, multiple laboratory and clinical studies have suggested that autologous bone marrow transplantation increases the local concentration of MSCs and hence promote bone healing in these areas of osteonecrosis. Stem cells have also been shown to promote angiogenesis, thus facilitating the healing process. Early studies suggested incorporation of the cells into the walls of these new vessels. Current studies however suggest that the mechanism of action of angiogenesis is more likely paracrine in nature with the release of various cytokines and growth factors.13
Several studies have already shown favorable results with autologous bone-marrow transplantation in arresting osteonecrosis of the femoral head.2,3,14,15,16,17 Many of these studies also showed better results in early disease, with preexisting, preoperative collapse of the femoral head usually resulting in further progression of disease. In addition, there has also been a positive correlation between the transplantation of a higher concentration of MSCs with better clinical outcomes.2,14 Hernigou et al also found a similar relationship when applying autologous bone-marrow grafting in tibial non-unions.18,19
Several randomized trials have also been conducted to determine if cell therapy results in better outcomes when compared to core decompression alone. Ganji et al delivered autologous bone marrow graft into the necrotic bone of a femoral head with ON and found significantly improved VAS (p=0.021) and WOMAC hip scores (p=0.013) in the bone marrow grafting group compared to the core decompression group.2 The former group had fewer patients progressing to collapse of the femoral head (1/10 patients vs 5/8 patients). Chang et al showed significantly smaller bone necrosis volumes at 12 months in patients randomized to core decompression and autologous MSC transplantation compared to those receiving core decompression alone.20 Their randomized study of only 8 patients also had significantly improved VAS and Harris scores in the MSC transplantation group.
In the currently published literature, the bone marrow graft was been obtained by centrifuging out the mononuclear components of the bone marrow aspirate. This was done to concentrate bone-derived mesenchymal stem cells. This was then injected into the necrotic area via a small trephine. Several authors have also tried to use different scaffolds to deliver the MSCs in an environment that promotes cellular signaling and bone healing. Techniques also vary from injecting the bone marrow through a small trephine into the necrotic bone, to removing the necrotic bone and replacing the defect with a biological strut or alternative material. Regardless they are all similar in that they use marrow-derived mesenchymal stem cells and apply it in conjunction with one of the many described biological scaffolds.21
Kawate et al cultured autologous bone marrow in vitro on beta-tricalcium phosphate ceramics and transplanted these along with a free vascularized fibula graft into 3 patients with preexisting femoral head collapse.22 2 patients had post-procedure progression of the femoral head collapse, but 2 had radiological features of bone repair on follow-up. While there was evidence of bone healing, they also concluded that such a procedure was not beneficial in patients with preoperative collapse of the femoral head.
Yamasaki et al likewise found improved outcomes in patients treated with bone-marrow-derived mononuclear cells with interconnected porous calcium hydroxyapatite (IP-CHA) compared with patients treated with cell free IP-CHA, in terms of reduction of in the size of the osteonecrotic lesion as well as prevention of further collapse of the femoral head.23
In an earlier study, we used autologous bone marrow with decalcified bone matrix (DBM) and allograft cancellous bone croutons following decompression of the femoral condyles in secondary ON with good results.4 Ji et al subsequently reported treating 103 hips with early femoral head necrosis with core decompression and bMSCs and DBM.24 At 2 years follow-up, there was a mean improvement in the Harris’ scores from 47.3 to 74.0 with good to excellent results in 75.7%. They too found better clinical outcomes in early disease.
In this study, we used the HEALOS FX Injectable Bone Graft Replacement (DePuy Spine Inc). This comprises a biomimetic matrix constructed of cross-linked, Type-1 collagen fibers that is circumferentially coated with a non-sintered layer of hydroxyapatite that is hydrated and implanted with autologous bone marrow. This gives an osteoconductive, 3-dimensional mineralized structure with a composition similar to human bone that has a favorable environment for osteoprogenitor cell attachment and bone ingrowth. Once placed in vivo, the moldable matrix then remodels into new bone throughout the graft site, not solely by creeping substitution, as is the case with many other biological scaffolds. The system also allows for a 3 to 4 fold increase in osteoprogenitor cell concentration in the graft matrix. We also ensured that only 2 to 4 ml of marrow from each aspiration site as it has been shown that drawing more than this amount can result in significant dilution with peripheral blood.5
Our early follow-up results show marked improvement in symptoms and a delay in progression in patients with early disease. One failure of treatment from a technical complication resulted in a patient with existing stage 3 ON of the hip that progressed to stage 4, resulting increase in pain and disability. Similar to previous studies, this technique shows improvement in early disease and may not be as beneficial in patients with existing articular collapse.
Our study has many limitations in terms of the number of patients treated, the absence of a control group and the relatively short follow-up. However these results may form the basis of subsequent study protocols to evaluate the long-term results compared to core decompression alone, or other means of delivering MSCs. Certainly the moldable matrix may promote bone healing in an area cleared of necrotic bone as the MSCs are retained within it.
The advantages of this technique are that 1) there is minimal donor morbidity, 2) the injectable, moldable form of this graft allows reliable introduction of the graft into the site of interest via a small minimally invasive technique, and 3) it does not preclude the patient from further surgery by avoiding alteration of the local anatomy.
Despite the exciting new frontier of cell-based therapy in the treatment of secondary osteonecrosis, there is still a need to 1) further understand the function and cellular triggers of MSCs, 2) optimize MSC harvesting and expansion, and 3) determine the best means to deliver and retain MSCs into the necrotic area with reliable and high local concentrations.25
In conclusion, our early results suggest that the use of autologous bone-marrow with the HEALOS FX injectable bone graft replacement improves patient outcomes in terms of pain, function and disease progression in early osteonecrosis. Further randomized studies with longer follow-up are required to better understand what might be an effective way of treating secondary osteonecrosis.
Table 1. Patient data
|
Age |
Diagnosis |
Area of ON |
Patient 1 |
20 |
Acute lymphocytic leukemia |
Bilateral knee ON |
Patient 2 |
32 |
SLE |
Left knee and hip ON |
Patient 3 |
33 |
SLE |
Left hip ON |
Patient 4 |
45 |
SLE |
Bilateral hip ON |
Table 2. Comparison of knee function scores from this study with those from our previous study4
|
Mean Knee Society Score |
Mean Knee Society Function Score |
Pre-op |
Post-op |
Pre-op |
Post-op |
Lee et al 2009 |
56 |
97* |
53 |
87* |
Present study |
53 |
95# |
63.3 |
93.3# |
* at 2 year follow-up
# at 1 year follow-up
Table 3. Outcome of treatment of osteonecrosis of the hip
|
Number
of Hips, n |
Mean VAS Score |
Mean WOMAC |
Pre-op |
1 year post-op |
Pre-op |
1 year post-op |
Treatment success |
3 |
7.3 |
0.7 |
66.7 |
97.4 |
Treatment failure |
1 |
8 |
8 |
51.6 |
36.7 |
|
No of Patients |
No of Hips |
Disease
Stage |
Study Type |
Bone marrow Delivery |
Follow-up duration (mean) |
Results |
Failures |
Hernigou,
2002 |
116 |
189 |
I-IV |
Cohort
CD + BMGT |
3mm Trephine |
5-10 years (7) |
|
9/145 (6.2%) with no collapse preoperatively progressed to THR
25/44 (56.8%) with pre op collapse had THR |
Ganji,
2004 |
13 |
18 |
I-II |
RCT
CD vs CD and BMGT |
3mm Trephine |
2 years |
Pain (p=0.021)
WOMAC
(p=0.013) |
5/8 (62.5%) CD progressed
vs 1/10(10%) CD+ BMGT |
Yan, 2006 |
28 |
44 |
I-IV |
Cohort
CD + BMGT |
Trephine |
2 years |
Harris (5886) |
|
Kawate,
2006 |
3 |
3 |
III |
Cohort
MSC in -TPC + vascularized fibular graft |
MSC in -TPC |
27-48 months (34) |
Evidence of bone healing |
Progression in 2/3 (67%) |
Ji,
2008 |
87 |
103 |
I-III |
Cohort CD+ MSC+DBM |
MSC+DBM |
2 years |
Harris (47.3-74)
75.7% Good-excellent results |
|
Hernigou,
2009 |
342 |
534 |
I-II |
Cohort
CD+BMGT |
3mm trephine |
8-18 years (12) |
ON Volume (26cm3-12cm3) |
94/534 (17.6%) progressed |
Wang,
2010 |
45 |
59 |
I-III |
Cohort
CD+BMGT |
Trephine |
12-40 months (27.6) |
Harris (71-83) |
7/59 (11.9%) had THR |
Yoshioka,
2010 |
6 |
9 |
I-III |
CD + BMGT |
6mm trephine |
3 years |
Harris (68-89)
VAS (67-17) |
1/9(11.1%) THR |
Chang,
2010 |
8 |
16 |
I-III |
RCT
CD vs CD+ BMGT |
Trephine |
12-42 months (23.5) |
VAS
Harris
Necrotic area |
Nil |
Yamasaki,
2010 |
30 |
39 |
I-II |
Comparative
IP-CHA vs BMG+IPCHA |
BMG + IPCHA |
12-48 months (29) |
Necrotic area |
3/30 (10%) collapse (BMG+IPCHA)
6/9 (67%) collapse (IPCHA) |
Table 4. Summary of existing studies on bone marrow graft transplantation.
Legend: CD=Core decompression, BMGT=bone marrow graft transplant, -TPC=beta-triphosphate calcium ceramics, MSC= mesenchymal stem cells, DBM=decalcified bone matrix, IP-CHA= interconnected porous calcium hydroxyapatite.
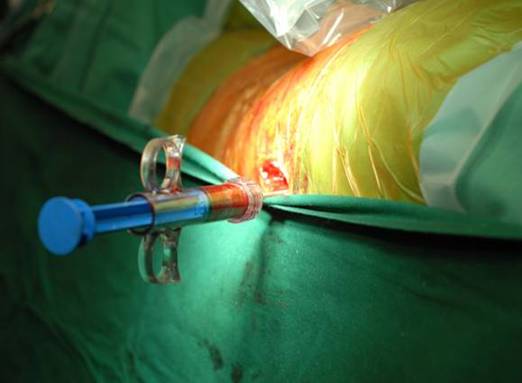
Photograph 1: Delivery syringe with autologous bone graft substitute inserted into the right hip
Reference :
- Mont MA, Carbone KK, Fairbank AC. Core decompression versus nonoperative management for osteonecrosis of the hip. Clin Orthop Relat Res. 1996 Mar;(324):169-78.
- Hernigou P, Beaujean F. Treatment of osteonecrosis with autologous bone marrow grafting. Clin Orthop Relat Res. 2002 Dec;(405):14-23.
- Ganji V, Hauzeur JP, Matos C, De Maertelaer V, Toungouz M, Lambermont M. Treatment of osteonecrosis of the femoral head with implantation of autologous bone-marrow cells. A pilot study. J Bone Joint Surg Am. 2004 Jun;86-A(6):1153-1160.
- Lee K, Goodman SB. Cell therapy for secondary osteonecrosis of the femoral condyles using the Cellect DBM System: a preliminary report. J Arthroplasty 2009;24(1):43-8.
- Muschler GF, Boehm C, Easley K. Aspiration to obtain osteoblast progenitor cells from human bone marrow: the influence of aspiration volume. J Bone Joint Surg Am 1997;79:1699.
- Aglietti P, Insall JN, Buzzi R, Deschamps G. Idiopathic osteonecrosis of the knee. Aetiology, prognosis and treatment. J Bone Joint Surg Br. 1983 Nov;65(5):588-97.
- Hernigou P,Beaujean F. Abnormalities in the bone marrow of the iliac crest in patients who have osteoecrosis secondary to corticosteroid therapy or alcohol abuse. J Bone Joint Surg Am. 1997 Jul;79(7):1047-53.
- Hernigou P, Beaujean F, Lambotte JC. Decrease in the mesenchymal stem-cell pool in the proximal femur in corticosteroid-induced osteonecrosis. J Bone Joint Surg Br. 1999 Mar;81(2):349-55.
- Calder JD, Pearse MF, Revell PA. The extent of osteocyte death in the proximal femur of patients with osteonecrosis of the femoral head. J Bone Joint Surg Br 2001;83:419–22.
- O’Brien CA, Jia D, Plotkin LI, Bellido T, Powers CC, Stewart SA et al. Glucocorticoids act directly on osteoblasts and osteocytes to induce their apoptosis and reduce bone formation and strength. Endocrinology 2004;145:1835–41.
- Ganji V, Hauzeur JP. Treating osteonecrosis with autologous bone marrow cells. Skeletal Radiol. 2010 Mar;39(3):209-11.
- Hernigou P, Bernaudin F, Reinert P, Kuentz M, Vernant KP: Bone-marrow transplantation in sickle-cell disease. Effect on osteonecrosis: a case report with a four-year follow-up. J, Bone Joing Surg. Am. (1997);79(11):1726-1730.
- Kinnaird T, Stabile E, Burnett MS Lee CW, Barr S, Fuchs S et al: Marrow-derived stromal cells express genes encoding a broad spectrum of arteriogenic cytokines and promote in vitro and in vivo arteriogenesis through paracrine mechanisms. Circ. Res. (2004);94(5):678-685.
- Hernigou P, Poignard A, Zilber S, Rouard H. Cell therapy of hip osteonecrosis with autologous bone marrow grafting. Indian J Orthop. 2009 Jan;43(1):40-5.
- Wang BL, Sun W, Shi ZC, Zhang NF, Yue DB, Guo WS et al. Treatment of nontraumatic osteonecrosis of the femoral head with the implantation of core decompression and concentrated autologous bone marrow containing mononuclear cells. Arch Aorthop Trauma Surg. 2010 Jul;130(7):859-65.
- Yan ZQ, Chen YS, Li WJ, Yang Y, Huo JZ, Chen ZR, et al. Treatment of osteonecrosis of the femoral head by percutaneous decompression and autologous bone marrow mononuclear cell infusion. Chin K Traumatol. 2006 Feb;9(1):3-7.
- Yoshioka T, Mishima H, Akaogi H, Sakai S, Li M, Ochial N. Concentrated autologous bone marrow aspirate transplantation treatment for corticosteroid-induced osteonecrosis of the femoral head in systemic lupus erythematosus. Int Orthop. 2010 May 29.
- Hernigou P, Poignard A, Beaujean F, Rouard H. Percutaneous autologous bone-marrow grafting for nonunions: influence of the number and concentration of progenitor cells. J Bone Joint Surg Am 2005;87:1430–7.
- Hernigou P, Poignard A, Manicom O, Mathieu G, Rouard H. The use of percutaneous autologous bone marrow transplantation in nonunion and avascular necrosis of bone. J Bone Joint Surg Br 2005;87:896–902.
- Chang T, Tang K, Tao X, Cao H, Li H, Chen Q et al. Treatment of early avascular necrosis of femoral head by core decompression combined with autologous bone marrow mesenchymal stem cells transplantation. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2010 Jun;24(6):739-43.
- Lee K, Chan CK, Patil N, Goodman SB. Cell Therapy for bone regeneration—bench to bedside. J Biomed Mater Res B Appl Biomater. 2009 Apr;89(1):252-63.
- Kawate K, Yajima H, Ohgushi H, Kotobuki N, Sugimoto K, Ohmura T et al. Tissue-engineered approach for the treatment of steroid-induced osteonecrosis of the femoral head: transplantation of autologous mesenchymal stem cells cultured with beta-tricalcium phosphate ceramics and free vascularized fibula. Artif Organs. 2006 Dec;30(12):960-2.
- Yamasaki T, Yasunaga Y, Ishikawa M, Hamaki T, Ochi M. Bone-marrow mononuclear cells with a porous hydroxyapatite scaffold for the treatment of osteonecrosis of the femoral head: a preliminary study. J Bone Joint Surg Br. 2010 Mar;92(3):337-41.
- Ji WF, Ding WH, Ma ZC, Li Jm Tong PJ. Three-tunnels core decompression with implantation of bone marrow stromal cells (bMSCs and decalcified bone matrix (DBM) for the treatment of early femoral head necrosis. Zhongguo Gu Shang. 2008 Oct;21(10):776-8.
- Ganji V, Hauzeur JP. Cellular-based therapy for osteonecrosis. Orthop Clin North Am. 2009 Apr;40(2):213-21. Review
|



