Address for Correspondence
Ahmed Elbardouni.
Department of Orthopaedic Surgery, Ibn Sina Hospital, Souissi, Rabat, PB10105, Morocco.
E-mail address: bardounia@menara.ma
Abstract
We report a case of a 70-year-old woman with carpal tunnel syndrome associated with the presence of a palmaris profundus muscle within the tunnel. During surgical carpal tunnel decompression; a well-developed anomalous tendon was found, it passed through the carpal tunnel, compressing the median nerve, and inserting to the deep surface of the palmar aponeurosis. The muscle belly originated from the ventral epimysium of pollicis longus muscle within the distal third of the forearm anterior compartment.
J.Orthopaedics 2011;8(3)e4
Keywords:
carpal tunnel syndrome; palmaris profundus muscle ; median nerve.
Introduction:
Carpal tunnel syndrome (CTS) is the most common entrapment neuropathy affecting the upper extremity, it represents 90% of entrapment neuropathies; most often idiopathic, CTS is due to thickening of the flexor tenosynovium and only 1.3% of the CTS that require surgical release are due to anomalous muscles [1]. The carpal tunnel is a narrow passageway at the anterior aspect of the wrist and allows the flessor tendons and the median nerve reaching the hand. Its dorsal floor consists of the carpal bones, and the roof of the tunnel is formed by the inextensible flexor retinaculum that continues in the midportion of the palm as the palmar aponeurosis. The narrowest point of the carpal canal corresponded to the hook of the hamate bone. To approach carpal tunnel, surgeon must know its anatomy variations and understand the relationships between its contents and its neurovascular structures [1]. The origin of the normal palmaris longus muscle (PLM) is the medial epicondyle of the humerus, it is located deep to the antebrachial fascia, and it is running downwards and outwards. It is muscular up to the forearm’s middle and tendinous below, and its tendon is running superficial to the flexor retinaculum and inserting into the proximal end of the palmar aponeurosis [2].
The palmaris profundus is a rare anomalous muscle that was described originally by Frohse and Frankel in 1908 as cited by Reimann et al. [2] and rarely has it been implicated in the carpal tunnel syndrome [3]. Reimann et al. [2] found only one palmaris profundus muscle in anatomical study of 1600 cadaver extremities, and because the palmaris longus muscle was absent the first one was considered as an anatomical variant of the second.
Case presentation
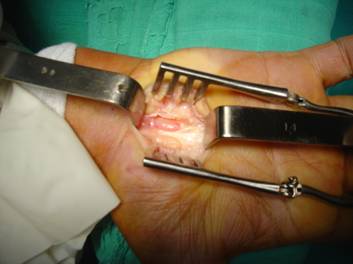
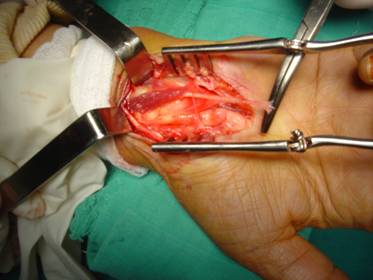
A 70-year-old right-handed woman was referred to us with a 1 year history of pain, numbness, tingling in the distribution area of the median nerve. Pain and paraesthesia radiated to the forearm and symptoms were worse at night and awoke patient from sleep; to relieve the symptoms, the patient flicked her wrist. The diurnal pain was activity related. At the clinical examination, Phalen’s maneuver and Tinel’s sign were positive. No swelling was noted, neither thenar muscle atrophy. The right median nerve at the wrist showed an increased conduction delay. Initial treatment consisted of nonsteroidal anti-inflammatory medication and corticosteroid injections into the carpal tunnels without any result. X-rays of the hand and wrist showed no bony abnormalities or soft tissue calcifications. She was operated on under axillary anesthesia with forearm tourniquet. The carpal tunnel was explored through the standard incision along the ring finger axis between the thenar and hypothena eminences, extending from Kaplan’s cardinal line to the distal wrist crease. When the transverse carpal ligament was divided, an aberrant tendon independent of the palmaris longus tendon was found beneath the flexor retinaculum enclosing and compressing the median nerve (Fig.1), and attaching to the deep surface of the palmar aponeurosis. The median nerve was compressed by the transverse carpal ligament too.The incision was extended up the distal forearm for approximately four centimeters, after the retraction of the palmaris longus tendon laterally, an accessory muscle belly was found under the antebrachial fascia. The aberrant muscle belly originated from the lower third of the forearm from the ventral epimysium of the pollicis longus muscle (Fig.2), deep to palmaris longus and flexor carpi radialis muscles. The aberrant muscle showed an independent well-formed belly with interconnection to the median nerve that gave its innervation. A gentle pull on this muscle did not produce any corresponding movement in the hand. The tendon followed the radial margin superficial to the median nerve and traversed the carpal tunnel and crossed over the median nerve from radial to ulnar side. The palmaris longus tendon, flexor digitorum superficialis tendons, and flexor carpi radialis tendon were normal. The anomalous muscle had been resected. Pain and paraesthesiae disappeared postoperatively. At 4 years after surgery, the patient was free of pain and there was no functional loss of the hand or forearm.
F(1)
F(2)
Consent
The patient was informed that data concerning the case would be submitted for publication, and she consented.
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
Both the authors have a major contribution in this case report. Both were involved in the pre operative planning, surgery, post operative management as well as in the preparation of this manuscript.
Discussion
al third lateral to flexor digitorum superficialis and deep to pronator teres [2]. The belly can arise from the lower third of the ventral epimysium of the flexor digitorum superficialis common tendon [4], from the dorsal epimysium of the palmaris longus muscle belly [5] , or like our case from the ventral epimysium of pollicis longus muscle [6]. Our anomalous belly muscle is bordered anteriorly by the tendons of the palmaris longus and the flexor carpi radialis, laterally by the brachioradialis and the radial artery, posteriorly by the flexor pollicis longus and medially by the flexor digitorum superficialis. Its tendon passed through the carpal tunnel and crossed the median nerve from radial to ulnar side. The insertion of the palmaris profundus is also variable and the tendon may be attached like our case onto the deep aspect of the palmar aponeurosis [5], the deep surface of the flexor retinaculum or both [4,6]. The musculus comitans nervi mediani may be fleshy proximally or fleshy distally (reversed palmaris profundus) [4]; the muscle appears to mimic palmaris longus in its form and variations [5]. Our patient presented a palmaris profundus that was different from accessory PLM because it had a different origin and it was enclosed in the same fascial sheath with the median nerve. It was named “musculus comitans nervi mediani” because of its intimate association with the median nerve [4]. The coexistence of anomalies of nerve and palmaris profundus muscle has been reported; the palmaris profundus could be associated with a high division of the median nerve [7], or enclosed by an unusual loop of the median nerve [6]. Consequently, it is important to be familiar with the variations in the branching, the course of the median nerve particularly the thenar motor branch, in order to achieve a complete neurolysis and also to avoid inadvertent damage to the nerve [1]. A well developed median nerve artery was also reported [4]. The palmaris longus muscle could be present [6, 8] as in our patient or absent [2]. The palmaris profundus could interfere with the median nerve causing carpal tunnel syndrom [5, 7-10], and rarely bilateral carpal tunnel syndrome were reported [7, 9]. PPM could be the cause of failed carpal tunnel release [7].
The diagnosis of carpal tunnel syndrome is essentially based on the patient’s history, clinical findings, and nerve conduction studies. In the clinical study, most of the patients with symptomatic anomalous muscles like palmaris profundus presented a carpal tunnel-like syndrome. The pain and paresthesias are effort-related and aggravate during hand movements high level activity [11]. Sometimes, a pseudomass could be palpated in the volar forearm [6], and this soft mass becomes hard with active muscular contraction [12].Electromyography and nerve conduction velocity studies can usually delineate peripheral nerve dysfunction. A sensory latency longer than 3.5 ms or a motor latency longer than 4.5 ms commonly is considered abnormal [13].
Routinely, imagery is not necessary before the treatment of the carpal tunnel syndrome. But sometimes, MRI can be helpful in cases of carpal tunnel syndrome with unusual or atypical manifestations, or in the presence of a Pseudomass of the forearm that is homogeneous and isointense to adjacent muscles on all MR images [14].
Surgery is the treatment of choice [11]. It needs release of the flexor retinaculum and resection of the anomalous muscle. In young patients, the treatment is limited to resection of the anomalous muscle without carpal tunnel release [12]. Our surgical dissection revealed that the aberrant tendon muscle exerted a median nerve compression; therefore, we released the flexor retinaculum and resected the anomalous muscle. The patient had complete resolution of symptoms at four year follow up.
Beside the palmaris profundus muscle, the most frequent others anomalous muscles implicated in the etiology of carpal tunnel syndrome include the palmaris longus muscle, the flexor digitorum superficialis and the lumbrical muscle [3, 12]. According to Reimann et al. [2], the PLM is the most variable muscle of the upper extremity, the PLM is absent (agenesis) in 12.8 % and there are many variations in the number (duplication, triplication, bifid), the origin (reversed PLM) , the muscle belly form (digastric, totally muscular) , the course, and the insertion of the tendon. When its tendon runs deep to the retinaculum and inserts into the undersurface of the palmar aponeurosis or the deep surface of the flexor retinaculum, it is difficult to distinguish it from the palmaris profundus.
The origin of the palmaris profundus muscle is variable, It most commonly arises from the lateral edge of radial proxim
Conclusion
We report a case of carpal tunnel syndrome in a patient with palmaris profundus compressing the median nerve within the carpal tunnel. Release of the carpal tunnel, decompression of the median nerve and excision of the anomalous muscle from the origin to the insertion led to complete resolution of symptoms. Palmaris profundus muscle may be confusing when entering carpal tunnel. The knowledge of this anomalous muscle is useful to orthopaedic, plastic and hand surgeons.
References
- Lindley SG, Kleinert JM: Prevalence of anatomic variations encountered in elective carpal tunnel release. J Hand Surg [Am] 2003, 28A: 849-55.
- Reimann AF, Daseler ED, Anson BJ, Beaton LE: The palmaris longus muscle and tendon. A study of 1600 extremities. Anat Rec 1944, 89: 495-505.
- De Smet L: Median and ulnar nerve compression at the wrist caused by anomalous muscles. Acta Orthop Belg 2002, 68: 431-8.
- Sahinoglu K, Cassel MD, Miyauchi R, Bergman RA : Musculus comitans nervi mediani (palmaris profundus). Ann Anat 1994, 176 : 229-32.
- Sanchez Lorenzo J, Canada M, Diaz L, Sarasua G: Compression of the median nerve by an anomalous palmaris longus tendon: a case report. J Hand Surg [Am] 1996, 21: 858-60.
- Chou HC, Jeng H, Ko TL, Pai MH, Chang CY, Wu CH: Variant palmaris profundus enclosed by an unusual loop of the median nerve . J Anat 2001, 199: 499-500.
- Jones DP: Bilateral palmaris profundus in association with bifid median nerve as a cause of failed carpal tunnel release. J Hand Surg [Am] 2006, 31: 741-3.
- Dyreby JR, Engber WD: Palmaris profundus, rare anomalous muscle. J Hand Surg [Am] 1982, 7 : 513-4.
- Stark RH: Bilateral palmaris profundus causing bilateral carpal tunnel syndrome. J Hand Surg [Am] 1992, 17: 182-3.
- Bauer JM, Trucell JJ: Palmaris profundus causing carpal tunnel syndrome. Orthopedics 1992, 15: 1348-9.
- Verdan CC : Les anomalies musculo-tendineuses et leur signification en chirurgie de la main. Rev Chir Orthop 1981, 67 : 221-30.
- Rapp E : Anomalies musculaires et syndromes canalaires du membre supérieur. Chir main 2004, 23 suppl : 188-98.
- Kilmer DD, Davis BA. Electrodiagnosis in carpal tunnel syndrome. Hand Clin. 2002, 2: 243-55.
- Schuurman AH, Van Gils AP. Reversed palmaris longus muscle on MRI: report of four cases. Eur Radiol. 2000, 10: 1242-4.
|




