Address for Correspondence
Hwan Tak Hee
Associate Professor and Senior Consultant, Division of Spinal Surgery, Department of Orthopaedic Surgery, National University of Singapore, 5 Lower Kent Ridge Road, Singapore 119074,
Email: doshht@nus.edu.sg
Abstract
Percutaneous vertebroplasty in the treatment of symptomatic vertebral compression fractures has become a popular treatment modality. The main purpose of the procedure is pain relief. Recent studies however, have cast doubt on its efficacy. An additional benefit of the procedure is possibly a partial restoration of the height of the collapsed vertebral body with potential improvement in the sagittal alignment and biomechanics of the spine.
Digital radiographs of 70 thoracolumbar osteoporotic compression fractures in 57 patients were reviewed retrospectively before and after vertebroplasty for changes in the vertebral height, wedge angle, kyphosis angle, thoracolumbar and lumbar sagittal angles.
Increases in anterior and middle heights post-vertebroplasty were statistically significant, along with improvements in the wedge angle and thoracolumbar sagittal alignment.
This study shows that percutaneous vertebroplasty effectively increases vertebral body heights resulting in improvements in the wedge angles. These improvements are achieved solely by placing patient in the prone position during the procedure. In addition, there was improvement in the thoracolumbar sagittal alignment. This finding is previously unreported and although the significance of this improvement is unclear, it may potentially result in improved biomechanics of the spine which may in turn result in reduced risk of adjacent level vertebral fractures.
J.Orthopaedics 2011;8(3)e9
Keywords:
Vertebroplasty; vertebral body height; osteoporotic compression fractures; sagittal alignment.
Introduction:
The prevalence of osteoporosis worldwide is increasing due to a combination of improved healthcare and advances in medical science resulting in increased life expectancy1. Among the many complications of osteoporosis, vertebral compression fractures (VCF) have also become more common. There is often a tendency to overlook the morbidities associated with osteoporotic VCF due to the traditionally “conservative” management of such conditions. Many VCF are asymptomatic and are only diagnosed incidentally but those that are symptomatic are often associated with significant morbidity. In addition, loss of anterior height results in wedge deformity of the affected level which is postulated to result in abnormal spinal biomechanics through altered sagittal alignment.
Percutaneous vertebroplasty was described by Gilbert2 in 1987 in the treatment of aggressive hemangiomas of the vertebral body. Subsequently, this technique was extended for use in the management of painful VCF. As such, the main indication of vertebroplasty in the treatment of VCF is that of intractable pain despite a trial of conservative management via analgesia, bed rest, gentle physiotherapy and other adjuncts e.g. acupuncture.
Percutaneous vertebroplasty involves the injection of polymethylmethacrylate (PMMA) into the affected vertebral body, often under local anaesthesia or under sedation. Partial to total relief of pain in 80 – 90% of patients is reported over the next 72 hours3,4. These results, though impressive, do not address the problem of loss of height resulting from the compression fracture. Loss of height and wedging of the affected vertebral body results in altered biomechanics of the spine and have been associated with increased risk of developing adjacent level compression fractures5. Kyphoplasty was hence developed in the hope of achieving the same excellent results as vertebroplasty with the added advantage of restoring the loss of vertebral body height6. The major drawback of this technique however, is its significantly greater cost as compared to that of vertebroplasty.
Several authors have observed mobility in vertebral compression fractures and have reported increases in vertebral height following vertebroplasty using postural reduction7-9.
This study was undertaken to investigate the immediate radiological effects of vertebroplasty with respect to the improvement in vertebral height, angles and sagittal alignment following percutaneous vertebroplasty.
Figures
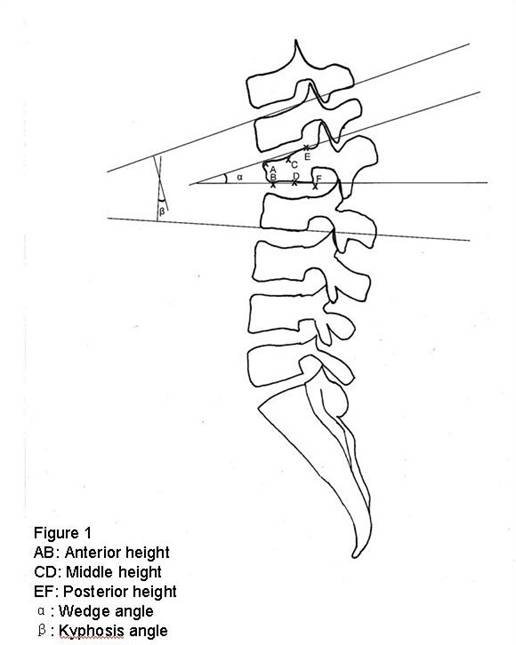
Figure 1
This shows the method of measurement carried out for determination of the wedge α and Cobb β angles on the lateral radiograph. The measurement of anterior height is taken from points AB, middle height from points CD and posterior height from points EF.
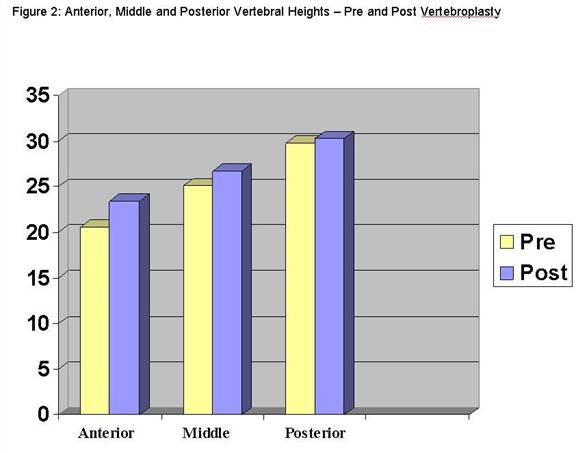
Figure 2
This shows the pre treatment and post treatment vertebral heights clearly demonstrating increases in post treatment vertebral heights most markedly in the anterior and middle columns.
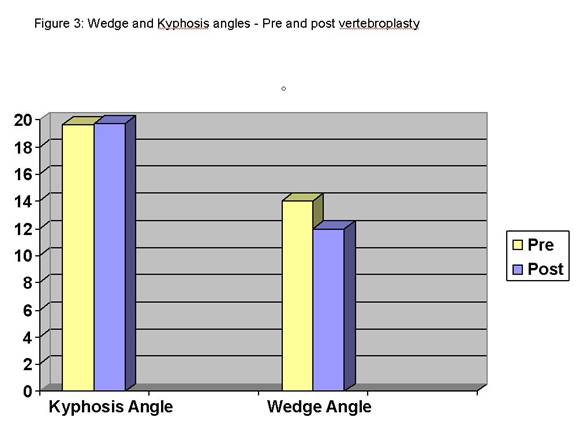
Figure 3
This shows the pre treatment and post treatment vertebral wedge and kyphosis angles demonstrating a statistically non-significant increase in kyphosis angle, but a significant improvement in the wedge angle.
Patients and Methods
Vertebroplasty for 70 osteoporotic compression fractures in 57 consecutive patients (47 females and 10 males) were carried out between the periods of Jan 2005 to Dec 2006. Age of patients ranged from 57 to 96 years with an average of 78 years. The main indication for the procedure was pain not improved despite conservative treatment, together with radiographic evidence of either an acute compression fracture or pseudoarthrosis. Duration of symptoms (ranging from 1 week to 10 months) was not considered an important consideration in the decision for or against surgery.
All patients underwent magnetic resonance imaging (MRI) of the spine prior to vertebroplasty to ensure accurate identification of the involved level especially in cases where more than a single level of osteoporotic compression fracture existed. Vertebroplasty was performed on acute fractures only, as evidenced by MRI changes of increased signal intensity of the vertebral body on T2 and short tau inversion recovery (STIR) sequences.
All pre-operative radiographs were taken in the erect position and were performed within 2 weeks of vertebroplasty while all post-operative radiographs were also taken in the erect position and done within 3 days of the procedure. Only osteoporotic compression fractures occurring in the thoracolumbar region of T10 to L3 were included in this study. Any compression fractures occurring as a result of other pathological conditions besides osteoporosis (e.g. tumors) were excluded. Compression fractures occurring as a result of blood dyscrasias were also excluded based on routine screening blood investigations which include a complete blood count, erythrocyte sedimentation rate and C-reactive protein.
Digital radiographs for these cases were reviewed by 2 independent investigators pre and post vertebroplasty. All radiographs and measurements were made using the Centricity (version 2.1, 2004 GE Medical Systems) digital radiography software.
Vertebroplasty technique
All cases were done under local anaesthesia with sedation provided by an anaesthetist. The patient was positioned in the prone position on a radiolucent table (Jackson table, Orthopaedics Systems, Inc) with pillows positioned under the patient to ensure comfort during the procedure.
Under guidance using an image intensifier, two 11 Gauge Spineplex needles (Stryker Corp., Kalamazoo, Michigan) were inserted via a bilateral transpedicular approach and advanced till the tip was approximately between the anterior and middle thirds of the vertebral body. Up to 10mls of radio-opaque contrast was injected and any signs of leakage checked with the image intensifier. If any leak was detected, the needle was repositioned and again checked for the presence of leakage. In the absence of leakage of contrast, PMMA loaded in 1ml syringes was injected into alternate needles while filling was checked regularly under image intensification. Between 2 to 7 mls of PMMA was used in each vertebral body depending on the degree of collapse, amount of filling and size of vertebral body. Injection of PMMA was stopped when either filling was observed to reach the posterior fourth of the vertebral body or if significant leakage was observed. The patients were kept in the prone position for 20 minutes since commencement of mixing of cement, after which they were allowed to turn supine. The patients were instructed to rest in bed on the day of the procedure and allowed to ambulate on the first post operative day. The patients were allowed to return home on the first post-operative day.
Measurement (Figure 1)
The lateral radiographs of all patients were analyzed using the Centricity (version 2.1, 2004 GE Medical Systems) digital radiography software. The anterior, central and posterior heights were measured using a magnified image to the nearest 0.1mm. The Cobb angles, wedge angles, and sagittal alignment of the thoracolumbar and lumbar regions (defined by convention as T10 to L2 and L1 to S1 respectively) were also measured to the nearest 0.1 degrees.
Analysis
Analysis of the data was carried out using the paired Students t-test with the help of a statistician. Statistical significance was taken as p value of less than 0.05.
Results
Of the patients analyzed, 48 had single level VCF, 6 had double level VCF, 2 had triple level VCF and only one had 4 level VCF.
The most commonly affected level is the T12 vertebrae with 23 cases. Twenty cases involved the L1 vertebrae, 11 cases involved the L3 vertebrae, 9 cases involved the L2 vertebrae, 4 cases involved the T11 vertebrae and only 3 cases involved the T10 vertebrae.
There were statistically significant increases in anterior (p<0.001) and middle heights (p<0.001). Of the 70 vertebral bodies which underwent vertebroplasty, 48 had increases in anterior heights and 43 had increases in middle heights. The average increase in anterior height was 2.9mm (range -5mm to +16.7mm, SD of 4.8mm) while the average increase in middle height was 1.6mm (range -1.9mm to +14.5mm, SD of 3.6mm). (Figure 2)
Statistically significant improvements in the wedge angles and thoracolumbar saggital alignment were also measured. Wedge angles improved by an average of 4.0° (range 0.2 to 10.4°, SD of 6.4°) while thoracolumbar saggital alignment improved by an average of 2° (range of 0.2 to 9°, SD of 6.5°). (Figures 3 and 4) Of the 70 vertebral bodies which underwent vertebroplasty, 43 showed improvement in wedge angles while 41 showed improvement in sagittal angles.
The kyphosis angle increased by 0.4° (range -16.5° to +18.6°, SD of 6.3°) but this was not statistically significant (P<0.881).
Posterior heights generally increased but improvements were not statistically significant. The average increase in posterior height was 0.5mm (p=0.16). The change in lumbar sagittal alignment showed a trend towards improvement by an average of 2.3°, but this was not statistically significant (p=0.74).
Discussion :
Percutaneous vertebroplasty is a well described procedure that has gained widespread acceptance. Its main application is for safe, rapid and effective relief of debilitating pain associated with acute wedge compression fractures of the vertebral body10,11. More recent studies have studied the effects of vertebroplasty on vertebral heights and many have found statistically significant increases in vertebral heights post vertebroplasty7,12,13. These improvements in vertebral heights were achieved using postural reduction with the patient placed in prone position during the procedure.
The efficacy of vertebroplasty, however, has recently been disputed by 2 randomized trials performed by independent investigators14,15. Their findings that vertebroplasty yielded no better results than sham procedures have cast doubt on the credence of the procedure.
Our study showed statistically significant improvements in the anterior and middle vertebral heights. In addition, statistically significant improvements in the wedge angles and thoracolumbar sagittal alignment were also noted. These improvements were likely due to performance of the procedure in the prone position with pillows placed under the chest and hips to effect a gentle hyper-extension of the spine. As the fracture was still relatively recent, the prone position resulted in a partial restoration of the vertebral height. Patients were also kept in the hyper-extended position till the polymethyl-methacrylate cement (PMMA) fully hardened after the procedure. In addition, ambulation was delayed till the first post-operative day to reduce the chances of loss of height immediately post procedure. The rationale for this is based on the fact that the strength of polymethylmethacrylate continues to increase for up to 4 to 5 days, after which its strength reaches a plateau16. Keeping the patient in bed for that amount of time, however, would be impractical and counter productive as patients could encounter problems associated with protracted bed rest.
The results of our study compare favorably with other studies done by other investigators which also conclusively showed significant increases in vertebral height post vertebroplasty7-9. Teng et al7 showed significant increases in anterior, middle, posterior heights (increment of 16.7%, 14% and 7% respectively) in addition to kyphosis and wedge angles (restorations of 4.3° and 7.4° respectively) of treated vertebral bodies. Hitawashi et al8 also showed significant increases in anterior, middle and posterior heights (2.5mm, 2.7mm and 1.4mm respectively). However, the study population in Hitawashi’s paper included compression fractures that resulted from neoplastic diseases and osteoporosis. Chin et al9 studied the efficacy of postural reduction prior to vertebroplasty in 3 groups of patients categorized into duration of onset of symptoms prior to intervention (less than 4 weeks, 4-8 weeks and more than 8 weeks). He presented his data in the form of a compression ratio of the anterior height divided by the posterior height. In all 3 groups, statistically significant increases in compression ratio post vertebroplasty were noted but more interestingly, the greater increases in compression ratio were observed in more acute compression fractures. The same observation was noted for the wedge and kyphosis angles.
Our study also analyzed the sagittal alignment of the spine pre and post vertebroplasty. These are predefined by convention as L1 to S1 for the lumbar sagittal alignment and T10 to L2 for the thoracolumbar alignment. Our study showed that the thoracolumbar alignment showed significant improvement while lumbar alignment did not. The reason for this observation is unclear. Our postulation is that the lumbar motion segments are capable of greater movements, and as such may “dampen” changes in wedge angles of the treated vertebral segments. On the other hand, thoracolumbar segments being less mobile, are not able to compensate for any changes in wedge angles of the treated vertebral bodies so readily.
Pradhan et al17 analyzed the sagittal angle of spinal segments pre and post kyphoplasty and found that improvement of the angular deformity diminished as he measured the Cobb angle off increasing numbers of spanning vertebrae from the VCF. He also found that the length of spine over which sagittal alignment was improved also increased with number of treated levels. In our study, 7 patients had vertebroplasty done concurrently on 2 levels while only one had vertebroplasty done on 3 levels. A sub-analysis done on these patients revealed a trend towards improvement in the sagittal alignment of both the thoracolumbar and the lumbar alignments. However due to the small sample size, further studies using larger sample sizes are required to verify these findings.
To the best of our knowledge, no other studies have analyzed the effects of vertebroplasty on the overall sagittal alignment of the spine. In a biomechanical study, Kayanja et al18 showed that the anterior wall of the upper adjacent vertebra of a VCF experienced higher strain. This suggests that the resultant kyphotic deformity from a VCF could predispose the adjacent vertebral bodies to compression fractures. As such, our findings are especially important as the improvement in wedge angles and sagittal alignment could theoretically result in improved biomechanics of the spine, hence reducing the incidence of adjacent level VCF. If this is true, vertebroplasty should then be adopted as the standard of treatment of VCF in all patients deemed suitable to undergo the procedure. Further studies are needed to confirm this postulation.
Conclusion
Vertebroplasty has long been established as a safe and efficacious means of pain relief from osteoporotic compression fractures. 2 recent studies have cast serious doubt on the efficacy of the procedure yielding results no better than sham procedures, in terms of pain relief. The potential benefits of vertebroplasty, however go beyond just pain relief. Significant improvements in anterior and middle heights, wedge and kyphosis angles are also observed. These improvements occur simply by placing the patient in a prone position with pillows positioned under the chest and hips. This maneuver not only enhances the comfort of the patient but also causes hyper-extension and hence, reduction of the fractured vertebra.
In addition to improvements in the wedge angle of each treated vertebra, some improvement of the sagittal alignment was also observed in the thoracolumbar region. This improvement in the thoracolumbar sagittal alignment may theoretically reduce the incidence of new compression fractures occurring in the same patient. Further studies are required to establish if this is indeed true.
Reference :
- E M C Lau. Osteoporosis: Implications in Asia. Ann Acad Med Singapore January 2002, Vol. 31 No.1
- Galibert P, Deramond H. Note préliminaire sur le traitement des angiomes vertébraux par vertébroplastie acrylique percutanée. Neurochirurgie 1987; 33: 166–7.
- Deramond H, Depriester C, Galibert P, Le Gars D: Percutaneous vertebroplasty with polymethylmethacrylate: Technique, indications and results. Raiol Clin North Am 36:533-546, 1998
- Amar AP, Larsen DW, Esnaashari N, Albuquerque FC, Lavine SD, Teitelbaum GP: Percutaneous transpedicular polymethylmethacrylate vertebroplasty for the treatment of spinal compression fractures. Neurosurgery 49:1105-1114, 2001
- Heaney RP. The natural history of vertebral osteoporosis: Is low bone mass an epiphenomenon? Bone 1992; 13 (suppl 2): 23–6.
- Lieberman IH, Dudeney S, Reinhardt MK, Bell G. Initial outcome and efficacy of "kyphoplasty" in the treatment of painful osteoporotic vertebral compression fractures. Spine. 2001 Jul 15;26(14):1631-8
- Teng MMH, Wei CJ, Wei LC, Luo CB, Lirng JF, Chang FC, Liu CL, Chang CY. Kyphosis Correction and Height Restoration Effects of Percutaneous Vertebroplasty. AJNR Am J Neuroradiol24:1893–1900, October 2003
- Hiwatashi A, Moritani T, Numaguchi Y, Westesson PL. Increase in vertebral body. AJNR Am J Neuroradiol. 2003 Feb;24(2):185-9.
- Chin DK, Kim YS, Cho YE, Shin JJ. Efficacy of postural reduction in osteoporotic vertebral compression fractures followed by percutaneous vertebroplasty. Neurosurgery. 2006 Apr;58(4):695-700; discussion 695-700.
- Amar AP, Larsen DW, Esnaashari N, Albuquerque FC, Lavine SD, Teitelbaum GP: Percutaneous transpedicular polymethylmethacrylate vertebroplasty for the treatment of spinal compression fractures. Neurosurgery 49:1105–1114, 2001.
- Jensen ME, Evans AJ, Mathis JM, Kallmes DF, Cloft HJ, Dion JE: Percutaneous polymethylmethacrylate vertebroplasty in the treatment of osteoplastic vertebral body compression fractures: Technical aspects. AJNR Am J Neuroradiol 18:1897–1904, 1997.
- Hiwatashi, A, Moritani, T, et. al., Increase in vertebral body height after vertebroplasty, AJNR Am J Neuroradiol 23:185-189, February 2003
- Hiwatashi A, Sidhu R, Lee RK, deGuzman RR, Piekut DT, Westesson PL. Kyphoplasty versus vertebroplasty to increase vertebral body height: a cadaveric study. Radiology. 2005 Dec;237(3):1115-9.
- Buchbinder, Rachelle, et al. "A Randomized Trial of Vertebroplasty for Painful Osteoporotic Vertebral Fractures." The New England Journal of Medicine.August 6, 2009, Volume 361:557-568, Number 6
- Kallmes, David F., et al. "A Randomized Trial of Vertebroplasty for Osteoporotic Spinal Fractures." The New England Journal of Medicine.August 6, 2009, Volume 361:569-579, Number 6
- SS Haas, GM Brauer and G Dickson. A characterization of polymethylmethacrylate bone cement. J Bone Joint Surg Am. 1975;57:380-391.
- Pradhan BB, Bae HW, Kropf MA, Patel VV, Delamarter RB. Kyphoplasty reduction of osteoporotic vertebral compression fractures: Correction of local kyphosis versus overall sagittal alignment. Spine. 2006;31:435-41.
- Kayanja MM, Ferrara LA, Lieberman IH (2004) Distribution of anterior cortical shear strain after a thoracic wedge compression fracture. Spine J 4(1):76–87
|





