Abstract:
Background: The purpose of this study was to compare the effectiveness of patient controlled intravenous narcotic analgesia (PCA) and epidural catheter pain control in the management of post-operative pain in pediatric Legg-Calve-Perthes (LCP) patients. We had two hypothesis; 1.) The Epidural and PCA have similar pain relief throughout hospitalizations, and 2.) The epidural increases both hospital inpatient charges and length of stay.
Methods: We conducted a computerized medical records search aimed at identifying all LCP patients treated surgically between July 1, 2007 and June 30, 2009. We identified 27 pelvic containment procedure (PC) patients (either innominate osteotomy or shelf arthroplasty) and 19 medial soft tissue release patients (MR). A retrospective chart review was completed to confirm: diagnosis of LCP, age, procedure performed, type of pain management, average pain score, type of pain scale, length of stay (LOS), charge of stay (COS), the use of adjunct therapy, and the utilization of epidural versus PCA.
Results: Twenty eight patients with LCP underwent a total of 46 surgical procedures (19 MR, 27 CP). Of this group of children 12 utilized a PCA, and 34 utilized an epidural for pain management during their in-patient admission. The EPI group had lower pain scores than the PCA group during utilization.
When the group was evaluated as a whole, LOS showed no significant difference between the patients using an Epi versus a PCA for pain control. However the length of time in hours that the Epi was used was significantly longer than the PCA (83.8 vs. 53.8 hours).
For those patients who had undergone a MR, there was no significant difference in LOS (in hours), COS, age, or length of time utilizing the pain control method for those patients who were administered an epidural vs. those patients administered a PCA.
For the PC group EPI patients demonstrated a greater length of stay (96.8 vs. 66 hours, p=0.0272) versus PCA patients, while no significant differences were identified regarding COS.
When the MR and PC patients were compared individually for each pain control measure (EPI vs. PCA), adjunct therapy was utilized (P-value of 0.02) more often when the patient underwent PC and utilized the EPI. Pain control with an EPI was better overall despite the variable use of pain scales.
Conclusions:
Epidural use increased the length of utilization of the pain control measure and increased the use of adjunct therapy within the PC group. MR patients showed no significant difference in length of stay, charge of stay, or length of pain control type. The EPI group had lower pain scores than the PCA group with only in the PC patients. EPI increased the length of utilization, COS, LOS, and use of adjunctive therapy in the PC group.
Level of Evidence: Level lII
J.Orthopaedics 2011;8(1)e5
Introduction:
Legg-Calve-Perthes disease (LCP) represents an idiopathic avascular necrosis of the femoral head that occurs in the pediatric population. It is the most common hip disease that develops in children. A variable amount of the femoral head may be involved, with greater amounts of involvement and collapse generally resulting in a proportional amount of secondary hip deformity. Deformity of the hip can cause pain and poor function of the hip1. This disease occurs between the ages of 2-12 years, and most commonly in males2.
In the past, surgical treatment of LCP was rather rare. The most common surgical procedures that these children undergo at our institution are either medial soft tissue release (MR) as seen in Figure 1-A or pelvic containment procedures (PC), further broken down into either innominate osteotomy, shelf arthroplasty, and/or a combination of the two. The two most common methods of postoperative pain control for these patients are patient controlled intravenous narcotic analgesia (PCA) and epidural catheter (EPI) pain control. The purpose of this study was to compare the effectiveness of PCA and EPI in the management of post-operative pain in pediatric LCP patients.
FIGURE 1 Radiographic appearance of the surgical procedures
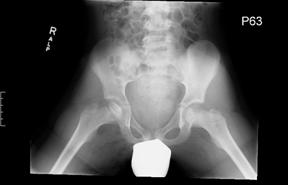
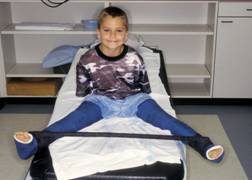
FIGURE 1-A Medial Release and Petrie Casting
Materials & Methods
Following IRB approval, an intrafacility surgical billing database utilized in the division of Pediatric Orthopaedic Surgery at Cincinnati Children’s Hospital Medical Center (CCHMC), was used to identify patients who underwent either MR or PC surgery for LCP between July 1, 2007 and June 30, 2009. A retrospective chart review of each patient was completed to obtain the following: verification of diagnosis of LCP, age at the time of surgery, procedure performed, type of pain management, duration of use of pain control method, average pain score during hospitalization, adjunct therapy, type of pain scale, length of stay, and charge of stay. The radiology imaging system at CCHMC also known as PACS was utilized to view images of each patient before and after surgery. All information was entered into an Excel spreadsheet. Statistical analysis consisted of the two-sample student’s T-Test for parametric data, and the Wilcoxon signed rank test for nonparametric data. Probability values (p-values) of less than or equal to 0.05 were considered to be significant.
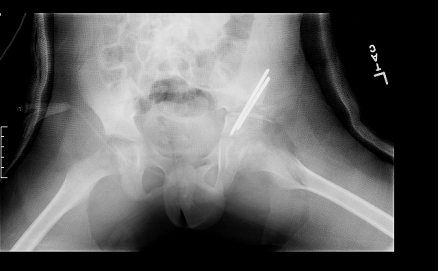
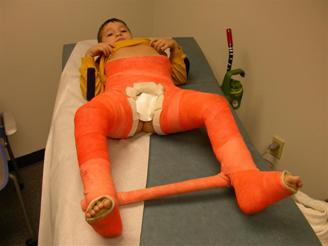
FIGURE 1-B Salter Osteotomy with Shelf Augmentation
Results
There were 28 patients who underwent 46 procedures during 46 distinct hospital admissions. MR patients had an average age of 6.85 years with a range from 5.35-9.78years, and PC patients had an average age of 7.49 years, with a range from 5.04-9.96 years. Of those patients 32.1% were females (9 girls) and 67.9% were males (19 boys). The right and left side were affected nearly equally (52.2% right and 43.5% left) and patients who were affected bilaterally accounting for 4%. Of the 28 patients, 19 underwent a medial release; of those 19 patients 4 utilized a PCA, and 15 utilized an epidural. Eighteen patients proceeded with a PC, to total 27 containment procedures for this study. Of the PC, patients 8 utilized a PCA, and 19 utilized an EPI for pain control. Of the 18 patients who had both procedures at CCHMC, 3 utilized the PCA for both surgeries, and 12 patients utilized the EPI for both surgeries. Additionally, one patient who was placed on an EPI for the first surgery, began an EPI for 7.6 hours, after the second surgery and a PCA was ordered in addition to the EPI for 27.5 hours. The PCA was then continued for 22.6 hours after the discontinuation of the epidural. Another patient utilized a PCA for the first surgery, was ordered an EPI for the second surgery, but was placed on a PCA for undocumented reasons within 2 hours of the initial order. Nine patients used an EPI only. One EPI patient altered their pain control method to a PCA for the second surgery. A total of 5 patients utilized a PCA only. One EPI patient was placed on a PCA after the EPI was discontinued for twenty-four hours.
Two-Sample Student’s T-Test Results: When medial release was compared to containment procedure the statistically significant levels showed that the charge of stay (COS) was greater for containment procedure with a p-value of <0.0001, and length of stay (LOS) was also greater in the containment procedure than medial release as the p-value was 0.0008.
When the LOS (p = 0.0272) was evaluated for the containment procedure, no significant difference was noted in patients with PCA vs. Epi. When Epi and PCA were compared, they also demonstrated no significant differences regarding age, or COS. A statistically significant difference was noted both for LOS (p = 0.0272) and duration of in-patient specialized pain control (p-value 0.0120). Subgroup analysis of the medial release patients (i.e. PCA vs. Epi) revealed no significant differences with respect to age, COS, LOS, or duration of in-patient specialized pain control. When each group was observed for adjunct therapy it was noted that only in the PC group, was there an increase in total number of medications delivered in addition to the EPI.
One patient utilized both pain control measures that allowed additional information to be contributed to the outcomes. The patient was a 9.9 year old male who underwent a containment procedure who was placed on a PCA for 7.5 hours, then had an epidural in addition to the PCA for 22.6 hours, the patient then remained on an epidural for 4.9 hours after the discontinuation of the PCA prior to discharge.
During the process of gathering information, it was noted that patients who were placed on an epidural, had pain scores which were initially very low, usually between 0-3 prior to the order to discontinue the epidural. The patients who were placed on the PCA, had higher pain scores during the hospitalization period prior to the discontinuation of the PCA.
Table 1: Medial Release Versus Osteotomy:
Pt# |
Sex |
Side |
Surgery |
|
Pain Control |
|
Pt# |
Sex |
Side |
Surgery |
|
Pain Control |
1.1 |
M |
L |
Med rel |
5.7 |
PCA |
|
1.2 |
M |
L |
Osteotomy |
5.8 |
PCA |
33.1 |
M |
L |
Med rel |
6.7 |
PCA |
|
11.2 |
M |
L |
Osteotomy |
9.3 |
PCA |
24.1 |
M |
R |
Med rel |
9.8 |
PCA |
|
33.2 |
M |
L |
Osteotomy |
6.8 |
PCA |
4.1 |
M |
R |
Med rel |
6.1 |
PCA |
|
34 |
M |
R |
Osteotomy |
10.3 |
PCA |
|
|
|
|
|
|
|
4.2 |
M |
R |
Osteotomy |
7.2 |
PCA |
5.1 |
M |
L |
Med rel |
7.1 |
Epi |
|
23.2 |
M |
R |
Osteotomy |
8.8 |
PCA |
13.1 |
M |
L |
Med rel |
7.2 |
Epi |
|
24.2 |
M |
R |
Osteotomy |
9.9 |
PCA |
17.1 |
M |
L |
Medial soft tess rel |
7 |
Epi |
|
25.2 |
M |
R |
Osteotomy |
8.4 |
PCA |
22.1 |
M |
L |
Med rel |
9.5 |
Epi |
|
|
|
|
|
|
|
16.1 |
F |
L |
Med rel |
6.4 |
Epi |
|
20.2 |
M |
R |
Osteotomy |
9.2 |
Epi |
20.1 |
M |
R |
Med rel |
9 |
Epi |
|
8.2 |
F |
R |
Osteotomy |
7.8 |
Epi |
9.1 |
M |
R |
Med rel |
9.3 |
Epi |
|
12.2 |
F |
R |
Osteotomy |
9.3 |
Epi |
30.1 |
M |
R |
Med rel |
6 |
Epi |
|
13.2 |
M |
L |
Osteotomy |
7.3 |
Epi |
36.1 |
M |
R |
Med rel |
5.4 |
Epi |
|
22.2 |
M |
L |
Osteotomy |
9.6 |
Epi |
37.1 |
M |
R |
Med rel |
6.5 |
Epi |
|
16.2 |
F |
L |
Osteotomy |
6.5 |
Epi |
25.1 |
M |
R |
Med rel |
8.2 |
Epi |
|
5.2 |
M |
L |
Osteotomy |
7.2 |
Epi |
8.1 |
F |
R |
Medial rel |
7.7 |
Epi |
|
6 |
M |
L |
Osteotomy |
8.5 |
Epi |
12.1 |
F |
R |
Medial rel |
9.2 |
Epi |
|
7 |
M |
L |
Osteotomy |
7.1 |
Epi |
19.1 |
F |
R |
Med rel |
7.3 |
Epi |
|
26.2 |
M |
L |
Osteotomy |
9.4 |
Epi |
27.1 |
M |
B |
Med rel |
6.2 |
Epi |
|
35 |
M |
L |
Osteotomy |
7.5 |
Epi |
|
|
|
|
|
|
|
17.2 |
M |
L |
Osteotomy |
7.2 |
Epi |
|
|
|
|
|
|
|
31.2 |
F |
L |
Osteotomy |
5.1 |
Epi |
|
|
|
|
|
|
|
19.2 |
F |
R |
Osteotomy |
7.4 |
Epi |
|
|
|
|
|
|
|
21 |
M |
R |
Osteotomy |
10 |
Epi |
|
|
|
|
|
|
|
30.2 |
M |
R |
Osteotomy |
6.1 |
Epi |
|
|
|
|
|
|
|
36.2 |
M |
R |
Osteotomy |
7.5 |
Epi |
|
|
|
|
|
|
|
37.2 |
M |
R |
Osteotomy |
6.7 |
Epi |
|
|
|
|
|
|
|
27.2 |
M |
B |
Osteotomy |
6.4 |
Epi |
Two-Sample Student’s T-Test Results:
Table 2: Length of stay (two-tailed t-test)
Variable* |
p-value |
PCA vs. EPI |
0.0666 |
Table 3: Cost of stay (two-tailed t-test)
Variable* |
p-value |
PCA vs. EPI |
0.2537 |
Table 4: EPI vs. PCA for Medial Release (two-tailed t-test)
Variable* |
p-value |
Age |
0.6250 |
COS |
0.0755 |
LOS (hours) |
0.7891 |
Len. Pain Control |
0.0506 |
Table 5: EPI vs. PCA for Osteotomy (two-tailed t-test)
Variable* |
p-value |
Age |
0.3521 |
COS |
0.1781 |
LOS (hours) |
0.0272 |
Len. Pain Control |
0.0120 |
*Statistical significance is indicated by a p-value <0.05. These items are highlighted in yellow above.
Wilcoxon Signed Rank Sums Test Results:
Table 6: Pain Score Average IV
Variable* |
p-value |
Medial Release vs. Osteotomy |
0.6333 |
PCA vs. EPI |
0.3014 |
Petrie vs. Spica Cast |
0.6885 |
Table 7: Pain Score Average
Variable* |
p-value |
Medial Release vs. Osteotomy |
0.1160 |
PCA vs. EPI |
0.0874 |
Petrie vs. Spica Cast |
0.1089 |
Table 8: Medial Release Adjunct Therapy:
Variable |
Pain Control |
Statistical Test |
P-value |
Total Doses of meds
(scheduled muscle relaxants, muscle relaxants PRN, pain medications) |
PCA vs. Epi |
T-test |
0.0220 |
Pain Medications |
PCA vs. Epi |
Wilcoxon Signed Rank Test |
0.0841 |
Scheduled Muscle Relaxants |
PCA vs. Epi |
Wilcoxon Signed Rank Test |
0.6281 |
Muscle Relaxants |
PCA vs. Epi |
Wilcoxon Signed Rank Test |
0.4397 |
Table 9: Containment Procedure Adjunct Therapy:
Variable |
Pain Control |
Statistical Test |
P-value |
Total Doses of meds
(scheduled muscle relaxants, muscle relaxants PRN, pain medications) |
PCA vs. Epi |
Wilcoxon Signed Rank Test |
0.5548 |
Pain Medications |
PCA vs. Epi |
Wilcoxon Signed Rank Test |
0.4949 |
Scheduled Muscle Relaxants |
PCA vs. Epi |
Wilcoxon Signed Rank Test |
0.8721 |
Muscle Relaxants |
PCA vs. Epi |
Wilcoxon Signed Rank Test |
0.6974 |
Discussion
The etiology of LCP remains largely unknown and may be due, at least in part, to blood clotting abnormalities, and/or insulin like growth factor abnormalities3. Factor-V Leiden and anticardiolipin antibody abnormalities have been identified in association with LCP4. Anticoagulation therapy (not to include the very young child) that the progression of necrosis of the femoral head5. Other factors thought to contribute to the occurrence of LCP are low birth weight, increase maternal age, passive smoke exposure, and abnormal presentation at birth2. It has also been noted that second hand smoke, maternal smoking during pregnancy, and clotting abnormalities increase the likelihood of osteonecrosis in children6. In a Swedish study it was noted that exposure to maternal smoking could be related to the restriction of vasculature to the femoral head7.
The treatment objective is to return the hip joint to normal function, and minimize further destruction of the hip8. These objectives are achieved primarily by focusing on two main principles regarding the hip joints of patients with Legg-Calve-Perthes disease: (1) maintain containment of the hip, and (2) maintain range of motion.
Postoperative pain is a major concern for the patient and parent alike. Two main pain control mechanisms utilized at CCHMC are the patient controlled analgesia (PCA) and the epidural. The PCA eliminates the need for intermittent dosing by nurses and allows the patient autonomy9. Epidural pain relief allows continuous pain control during recovery, and is independent of patient’s knowledge level and prevents patient noncompliance. There are noted pain goal achievements as well as complications for both pain relief methods10.
When looking at medial release in a solitary manner statistically the epidural group and the PCA group were comparable in nature in relation to COS, LOS, age, and length of pain control method. On the other hand, when looking at the pain scores the PCA were found to have a significantly higher pain scores during the entire admission than the patients using an epidural. This did not allow the researchers to prove the first hypothesis that the epidural and PCA have comparable pain control for the medial release group.
In the containment procedure group it was noted that the patients utilizing the epidural had a longer length of utilization of the pain control method when compared in hours to those patients using the PCA. When comparing and contrasting medial release versus containment procedure the containment procedures were proven to have a longer stay with greater accrued costs. Thus proving the second hypothesis that the Epidural would increase the length of stay and the charge of stay, but only for the containment procedure group.
The current research must be interpreted within the context of the study design. This was a small retrospective cohort study that could have been influenced by multiple forms of bias. Another weakness of the paper relates to the fact that while standardized pain control methods were used, there was no standardization regarding utilization of various in-patient pain scales.
The pain scale for medial release was noted to be assigned 60% of the time to children that were not in the assigned age for the scale. The pain scale for containment procedures was noted to be varied in 62.8%. Pain scale distribution for patient assessment was distributed as: CHEOPS alone 3, CHEOPS then OUCHER 1, FLACC 27, FLACC then VAS 2, OUCHER alone 2, OUCHER then CHEOPS 1, OUCHER then FLACC 3, VAS alone 12, and VAS then FLACC 4. The VAS scale was utilized per the criteria 94.74% and disproportionately 5.3%, FLACC was considered undeterminable of usage in 100% due to the lack of justification for usage, CHEOPS was used per stated criteria 80% of the time and leaving 20% undeterminable, and OUCHER was utilized per criteria 57.1 and undeterminable 42.9% of the time. Pain control method usage was noted as Epi 62.5%, and PCA 21.4%.
In conclusion, our first hypothesis that both pain control measures were equal was unable to be supported. The study did allow to prove the second hypothesis that the epidural increases the length of stay and adjunct therapy usage in the postoperative containment procedure population. When each type of medication use was reviewed, 1.) scheduled muscle relaxants, 2.) as needed muscle relaxants, and 3.) narcotic pain medications, there were no explanations for delivering the medications. No direct correlation was found in relation to the pain score and the delivery time. This information opens up the opportunity to standardize the pain scale usage, and guidelines for the use of pain control method. Finally our retrospective cohort study has left us with what we feel are TWO important take home points; the pain scale is used interchangeably, and the pain control in the pediatric LCP is non-standardized
Abbreviations:
CCHMC- Cincinnati Children’s Hospital Medical Center
CHEOPS- Children’s Hospital of Eastern Ontario Pain scale
COS- Charge of stay
Epi- Epidural
FLACC- Faces legs arms cry Consulability
LCP- Legg-Calve-Perthes Disease
LOS- Length of stay
PCA- Patient controlled analgesia
VAS- Visual analog scale
MR- Medial Release
PC- Containment Procedure
ACKNOWLEDGMENTS
The authors wish to acknowledge the research assistance of Cassie Kirby, BA and statistical support of William C. Lippert, MPH.
References
1.Beer, Y., et al., Long-term results of proximal femoral osteotomy in Legg-Calve-Perthes disease. J Pediatr Orthop, 2008. 28 (8): p. 819-24.
2.Roy, D.R., Current concepts in Legg-Calve-Perthes disease. Pediatr Ann, 1999. 28(12): p. 748-52.
3. Wall, E.J., Legg-Calve-Perthes' disease. Curr Opin Pediatr, 1999. 11(1): p. 76-9.
4.Balasa, V.V., et al., Legg-Calve-Perthes disease and thrombophilia. J Bone Joint Surg Am, 2004. 86-A(12): p. 2642-7.
5. Gruppo, R., et al., Legg-Perthes disease in three siblings, two heterozygous and one homozygous for the factor V Leiden mutation. J Pediatr, 1998. 132(5): p. 885-8.
6. Glueck, C.J., et al., Secondhand smoke, hypofibrinolysis, and Legg-Perthes disease. Clin Orthop Relat Res, 1998(352): p. 159-67.
7. Bahmanyar, S., et al., Maternal smoking during pregnancy, other prenatal and perinatal factors, and the risk of Legg-Calve-Perthes disease. Pediatrics, 2008. 122(2): p. e459-64.
8. Myers, G.J., K. Mathur, and J. O'Hara, Valgus osteotomy: a solution for late presentation of hinge abduction in Legg-Calve-Perthes disease. J Pediatr Orthop, 2008. 28(2): p. 169-72.
9. Viscusi, E.R., Emerging treatment modalities: balancing efficacy and safety. Am J Health Syst Pharm, 2007. 64(6 Suppl 4): p. S6-S11.
10. Momeni, M., M. Crucitti, and M. De Kock, Patient-controlled analgesia in the management of postoperative pain. Drugs, 2006. 66(18): p. 2321-37. |






