|
ABSTRACT
Background: Many patients come to the orthopaedic department with neglected
CTEV, residual CTEV or recurrent CTEV. They usually present after one year of age. In a elderly child, soft tissue release alone is often not suffiecient for full correction. Ina patient with previous surgical scar, it is all the more difficult. So fractional distraction with Joshi's external stabilisation system is a useful option to correct the deformity in such patients. We aimed to study the short term follow up of 41 patients with 16 bilateral cases treated with Joshi's external stabilisation system at the department of orthopaedics, medical college, Calicut; regarding the cosmetic, fuctional and anatomical outcome.
Methods: 41 patients with 16 bilateral cases in whom, Joshi's external stabilisation system was done at the department of Orthopaedics, Calicut medical college, during the period of 1994-2002; followed up for an average period of three and half years. Patients were selected irrespective of sex, but patients with non-idiopathic club foot was not included in this study. The principle of correction applied in this study was fractional distraction.
Results: 33.3% of patients in this study had undergone various surgical procedures previously including posteromedial surgical release. 66.7% had undergone, conservative treatment, which included serial casting, one child had neglected
CTEV. The severity assessed in these cases were 5 and above in 666.7% of children. Children with less severe deformity had lesser distraction period. 59.7% had excellent and good results.
Conclusion: Fractional distraction with JESS is an easy method and it is simple and easy to understand. The parents learn the distraction technique easily and were usually complaint. Adequate static period is necessary for maintaining full correction. Once the external fixator is removed , protective splints are a must to maintain the correction. The procedure is less invasive and the results are good irrespective of the severity of the deformity.
J.Orthopaedics 2004;1(1)e3
Introduction:
The basic deformity in clubfoot is a congenital subluxation of
Talocalcaneal-navicular joint. But the correction of abnormal
tarsal relationship is resisted by pathological contracture of
soft tissues. A lasting correction is obtained when the
correction is complete and reduction is maintained long enough
for the tarsal bones to remold and form a stable
articulation(1). Many one and two staged operations have been
described to correct all components of the deformity. Some
surgical procedures are piecemeal operations intended to correct
one specific component of the deformity(2). Soft tissue release
operations, though produce good results in most of the cases,
may reduce motion of the foot and ankle(3). Extensive soft
tissue release operations have resulted in over correction of
the deformity(4,5). JESS works on the principles of soft tissue
distraction, maintenance of tarsal relations and correcting all
the deformities simultaneously. As the procedure does not
include any incision and acute correction of the deformity,
dreaded skin complications, which are so common in other
modalities of treatment is less likely to occur.
Aim of the Study:
Continuous and adequate conservative treatment usually results
in satisfactory complete correction of CTEV in most of the
cases, in children of all age groups. Most failures occur from
inadequate treatment(6), negligent parents interrupting regular
continuous treatment or resistant form of clubfoot. This study
aims to find out the indications and operative feasibility at
various age groups with different grades of deformity. The study
evaluates complications and management of complications. The
study also intends to assess the final outcome of this technique
of treatment.
Patients and Methods:
A prospective study of fractional distraction using JESS
distractors for Idiopathic congenital club foot was conducted on
41 patients during the period 1994-2002. The cases broadly came
under 3 categories.
1. Rigid foot not responding to serial manipulation and casting.
2. Recurrent cases after earlier surgical failures.
3. Neglected, late presenting cases.
Non Idiopathic club foots were not included in this study. All
the cases were clinically assessed for associated anomalies
clinically and in indicated cases with X-rays of Lumbosacral
spine and X ray pelvis, to rule out spina bifida and congenital
dysplasia of Hip. The child and parents were informed about the
procedure, giving opportunity to discuss with other patients
undergoing the same treatment and with photographs. The
importance of pin track care and strict regular follow up is
stressed in the preoperative planning.
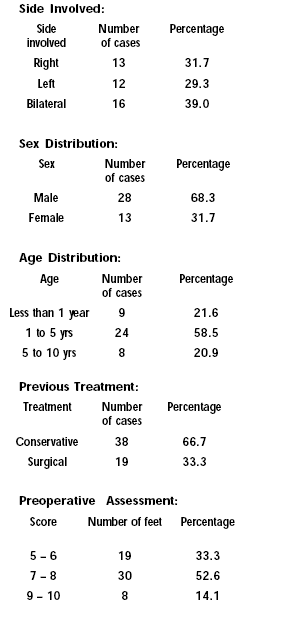
All the cases were assessed preoperatively with
1. Clinical assessment for severity of the club foot.
2. Pre operative photograph.
3. Preoperative X-ray of foot- Antero posterior and lateral
view(7,8).
4. Pre anaesthetic check up.
In preoperative clinical assessment (Caroll) the details
evaluated are(4,9):
1. Calf atrophy
2. Posterior displacement of the fibula
3. Creases- medial or posterior
4. Curved lateral border of the foot
5. Cavus
6. Fixed equinus
7. Navicular fixed to the medial malleolus
8. Os calcis fixed to the Tibia
9. Fixed forefoot supination.
Each feature scores one point when present and no point when
absent. Thus the worst foot having all the features would score
10 points and a normal as well as corrected foot would score 0
points.
Very simple routine instrumentation will suffice for the
procedure. Hand drill, T-Handle are used for introduction of
Kirschner Wires. The basic component forming the heart of the
JESS system is the link joint. Kwire drilled through the bone is
assembled to the system of connecting rod through link joint.
Link joint connect the K wire and connecting rod at right
angles. The link joint is locked in place by a recessed
hexagonal nut.
Connecting rods of various lengths of smooth rods and angled rod
are used, in younger children 3.0mm and older children 4.0mm
connecting rods are used. Z rods used to construct the Tibial
segment of frame is available in predetermined sizes to suit
various age groups. L shaped rods of 2 sizes are necessary for
metatarsal segment and calcaneal segment of the frame.
The standard JESS distraction device is used(11). It has a
threaded rod on which is mounted a static block and a
translating block. Each block has 2 holes for passage of K wire
or a connecting rod. The length of the outer border of the foot
is measured for ascertaining the length of distractor used for
the foot. The length of the leg is measured to select the size
of the Tibiocalcaneal distractor and Tibio-metatarsal connecting
rod.
The Tibial K wires are passed first. 2 K wires should be
parallel and the distance between the 2 K wires is determined by
the length of the Z rod. Metatarsal K wires are introduced using
T handle, for continuous feed back regarding the position of the
K wire in the foot. One transfixing wire is passed from the
firth to the first Metatarsal engaging fifth and first
metatarsal at the neck. No attempt is made to impale all the
metatarsals and thereby flattening the transverse arch of the
foot. 2 separate wires, one from medial and other from lateral
aspect are introduced parallel and proximal to the first wire.
These two wires engage two or three metatrsals on their
respective side at the level of the proximal shaft. Calcaneal K
wires are introduced using T handle. The position of the
posterior Tibial Artery is palpated and two transfixing K wires
are passed into the Calcaneum from the medial side taking care
not to injure the artery. These wires are perpendicular to the
long axis of the Calcaneum. The distance between the two wires
should be the distance between the holes in the blocks of
distractror to be used. The axial calcaneal wire is passed
posterior to anterior. By abducting the hip, externally rotating
the limb, the foot can be positioned to expose the heel. The
point of entry is; just distal to the insertion fo the Achilles
tendon. The wire is directed medially and distally, towards the
varus and equinus of the Calcaneum. The wire should be in the
long axis of the Calcaneum.
The connecting rods and distractors and assembled. The plantar
limbs of the L rods provide a slot for the foot plate
attachment. This plate supports the foot and toes and prevent
flexion contractures of the toes during distraction phase due to
the relatve in elasticity of the flexor tendons.
Distraction Schedule:
Calcaneo metatarsal distraction corrects forefoot adduction at
midtarsal and tarsometatarsal joints. This also realigns the
head of the Talus with the Navicular and derotates the Calcaneum.
Placement of a distractor on the lateral column of the foot will
prevent a wedge compression of the bones and cartilages if only
medial distractor is used. It will also help to unlock the tight
Calcaneo cuboid joint. This connection is static. It keeps
anterior part of the ankle joint and subtalar joints open, while
the heel equinus is being corrected.
Dorsiflexion of the ankle joint is achieved gradually after
correction of all other components of the deformity. 20-30 of
dorsiflexion is necessary to avoid recurrences and to permit
squatting.
Following the achievement of correction the foot has to be
maintained with the assembly till the soft tissues remould and
mature in the elongated position. It is generally preferred that
the period of static phase should be twice the period of
distraction. Positioning the foot in evertion for a few days
before the removal of the frame will help in reducing
recurrence. This is achieved by evertion bar.
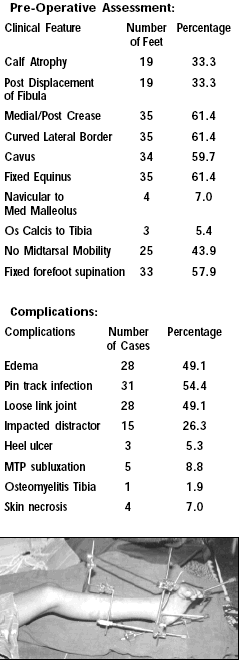
Complications:
Edema of the Leg, Flexion contracture of the toes, Loosening of
link joints, jamming of the distractors, linear skin necrosis,
heel ulcer, rocker bottom foot and under correction are the
common complications. These complications can be avoided by
closely adhering to the suggested protocol.
 |
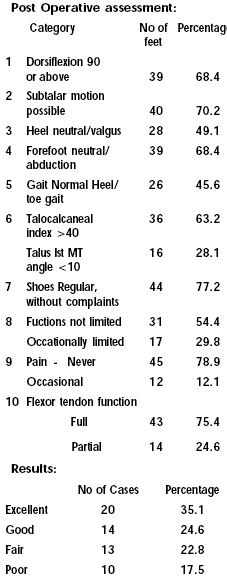
Post
Operative Assesssment(10): |
 |
| |
Discussion:
This prospective study of treatment of idiopathic club foot with
jess distractor was done in 41 patients, of which 16 children
had bilateral deformity. 33.3% of the children in this study
group had undergone various surgical treatment including
Tendoachillis lengthening, posterior release and posteromedial
release. Other 66.7% children had undergone only conservative
treatment. One child aged 9 years had not undergone any
treatment before. Severity assessment (Caroll) in these cases
were 5 and above. 66.7% of the children were above score 7.
Irrespective of severity and age group all the children have
undergone the same protocol of surgery and post operative
management. Children with less severe deformity needed lesser
period of distraction, where as moderate deformity of scores
needed longer time of distraction.
54.4% of the children developed pin tract infection. In one case
there were radiological changes of osteolmyelitis in Tibia and
Calcaneum which was treated with parentral antibiotics and
achieved healed status. Edema of the leg was also a major
problem. 49.1% of children had obvious edma. Edema in most of
the cases subsided with elevation of the limb. In the cases of
moderate edema, the distraction is delayed for a few days until
the edema is subsided. Those cases which had edema showed
increased incidence of pin tract infection.
We have discarded using foot plate after initial 4 cases. All of
them developed severed pain at the heel and tip of the toes. One
of them developed a pressure ulcer over the heel. Flexion
deformity of the toes occurred in most of the cases, but
responded to passive stretching by the parents. Loosening of
link joints are seen in 49.1% of the cases.
Skin necrosis was seen in 4 cases , reversing the distraction
for a few days solved the problem. This was developed due to
intial correction tried to achieve at the time of application of
the apparatus. Initial correction was tried in this case due to
difficulty in alaigning the distractor in the rigid club foot
due to sever deformity. We have not used swivel distractors
sofar, which would be a better option in these cases.
Assessement of results showed excellent and good results in
59.7% of cases, Functional, cosmetic and radiological criteria
were used for assessment.
Though all the children had achieved full correction clinically
at the time of removal of the apparatus, the difference was in
the static period. We could not maintain static period of double
the time of distraction in most of the cases due to pin track
infection and non-compliance from the parents.
We could not find any correlation between the severity of the
clubfoot and end result, but strong correlation was present in
children who strictly follow the distraction static phase
protocol and the final outcome.
Conclusion:
Functonal distraction using JESS apparatus is an easy method,
which does not require any sophisticated instrumentation or
image intensification. Parents learn the distraction technique
easily and comply with the procedure. Pin tracks should be cared
meticulously. Adequate period of static phase is necessary
before removal of the appartus. Strict post operative management
and follow up is mandatory.
As the procedure does not involve any open surgery, chances of
scaring and skin complication are very unlikely. Surgical
feasibility and tolerance to fixator is same for all age groups.
Distraction system gives good results irrespective of the
severity of the deformity.
The assessment of results reveals that many acceptable results
still leave much to be desired, this stimulate us to elevate our
goals and strive to attain the ideal of a near normal foot.
Reference:
1. Blek. E E: Congenital club foot Pathomechanics,
radiographic analysis and results of surgical treatment,
clinical orthopaedics and related research No 125 June 1977
2. Tachdijian M O. Peadiatric Orthopaedics 2nd Edition, W. B
Saunders company, 2428-2557, 1990.
3. Vincent J Turco : Clubfoot Churchill
Livingston
4. Caroll N. C. Mc Murtky R and Leete S.F: The pathoanatomy of
congenital clubfoot, Orthopedic clinics of North America 9:2255.
5. Evans D. Relapsed clubfoot, JBJS 43 B 1961
6. Mc Kay DW: New concepts of and approach to club foot teatment,
Principles and morbid anatomy J Peadiatric Orthopaedics,
2:347 1982
7. Huggo Adams Keim, Gordon W Ritchie: Weight bearing
roentgenograms in the evaluation of foot deformities. CORR No 70
May June 1970
8. Milton E Ashby: Roentgenographic assessment of soft tissue
medial release operations in club foot deformity, CORR No 90 Jan
Feb 1973
9. Grill F and Franke J: The Ilizarov distractor for the
correction of relapsed or neglecvted clubfoot. JBJS 69 B
593, 1987.
10. Dan Atar, Wellace B Lehman, Alfred D Grant, Allen
Strongwater: Functional rating system for evaluating the results
of club foot surgery Orthopedic Review Vol I No. 2 1991
11. Joshi BB, Laud NS, Warrier SS : Operative manual of
treatment of CTEV by JESS
|